Kidney Disease Linked To Dementia
The chances of losing one’s mental faculties with age are increased in older adults with chronic kidney disease, according to two research reports in the August issue of American Journal of Kidney Diseases, the official journal of the National Kidney Foundation.
The good news is that there are medications that decrease albuminuria or protein in the urine, one of the earliest signs of kidney disease, and therefore may prevent or delay cognitive decline.
Abnormalities in the capillaries, which are the smallest blood vessels in the body, are found in the brains of people who die of dementia. Similar capillary findings are observed in kidneys of people with albuminuria, leading scientists to predict that albuminuria and vascular disease of the brain may go hand in hand.
“Persistent albuminuria means that the kidney has some damage and is starting to spill some albumin — a kind of protein — into the urine,” said Dr. Kerry Willis, Senior Vice President for Scientific Activities, National Kidney Foundation. The most common causes of albuminuria are diabetes and high blood pressure.
As part of the Cardiovascular Health Cognition Study, more than 2000 people over the age of 65 years underwent testing of their memory and thinking skills, and they gave urine samples to measure levels of albumin.
These findings imply that “albuminuria increases the likelihood that dementia is present or will develop,” Dr. Barzilay and his associates write.
Cognitive Impairment In Albuminuria
Studies that assess the association between CKD and cognition mostly use creatinine or eGFR as a marker of kidney function. Fewer studies assessed the relationship between cognition and albuminuria. Albuminuria is the excessive loss of protein in urine, and a marker of kidney damage, amongst other underlying conditions that include cumulative vascular damage related to hypertension, diabetes, and inflammation . It is known to be an early indicator of CKD .
Prevalence of albuminuria increases with kidney impairment it is estimated that 24% of individuals with CKD stage 3 have albuminuria . Individuals with albuminuria have an increased risk of further accelerated eGFR loss when compared to controls . Higher levels of albuminuria have been associated with increased mortality and cognitive impairment in older adults . Studies have explored whether albuminuria and cognition are associated at the cross-sectional and longitudinal level however, concordance among eGFR, albumuninuria, and cognitive impairment is not as clear and results at both cross-sectional levels and longitudinally are mixed.
T Scores For Individual Tests: Ckd Versus Hd
In order to compare groups, T scores for each neuropsychological test were calculated and reported . HD subjects scored significantly lower than CKD subjects on 3 of 5 measures of attention and processing speed and all measures of language. CKD subjects scored significantly lower than HD subjects on one test of executive function. There was no significant difference between the groups for measures of memory. When the T scores were adjusted for hypertension, diabetes, hyperlipidemia, CAD, CHF, PAD, PO4, Ca × PO4, PTHi and TSH, significant differences between the groups remained . For the HD group, time since the last dialysis was not significantly associated with performance on the cognitive tests.
Table 4
Cognitive function scores and prevalence of impairment by group
Recommended Reading: What Shampoos Cause Alzheimer’s Disease And Cancer
Acute Kidney Failure In Elderly: Causes And Symptoms
Written byDevon AndrePublished onSeptember 12, 2016
Acute kidney failure is the inability of the kidneys to filter waste from the blood. If the kidney lose their filtering ability, the waste accumulates in the blood and its levels become dangerously high, disrupting the bloods own chemical balance.
Acute kidney failure can develop rapidly. It is commonly seen in persons who are already hospitalized, specifically those who are critically ill or in intensive care.
Acute kidney failure can be a fatal condition, but it can be reversible, too.
Here we will outline the causes and symptoms of acute kidney failure.
The Provision Of Services For Eskd

Clinicians suggested that where there was a lack of assisted APD, frail patients were more likely to receive CKM.
Those patients would have been for non-dialysis care in many senses because haemodialysis would have been too distressful.
While underprovision in one modality was felt to discourage referrals, clinicians felt that good local services actively encouraged referral for that pathway.
Because we have got an active conservative management programme my colleagues feel you know although the patient is elderly we can still offer them something. You feel that you can do something proactive.
However, a nurse expressed concerns that patients may feel pressured into accepting a specific dialysis modality solely because of availability.
Because there is an option to use assisted APD, theres a chance and a risk that it would be used inappropriatelyto just attach someone to a machine because the opportunity is there, I dont feel is appropriate.
You May Like: Does Andrea Mitchell Have Dementia
Failing Kidneys Could Bring Higher Dementia Risk
FRIDAY, May 7, 2021 — Chronic kidney disease may carry an increased risk of dementia, according to a Swedish study.
In people with chronic kidney disease, the bean-shaped organs gradually lose their ability to filter waste from the blood and eliminate fluids.
“Even a mild reduction in kidney function has been linked to an increased risk of cardiovascular disease and infections, and there is growing evidence of a relationship between the kidneys and the brain,” said study author Dr. Hong Xu, a postdoctoral researcher at the Karolinska Institute in Stockholm.
For the study, her team analyzed health data from nearly 330,000 older people in Stockholm. None had dementia or had undergone kidney transplants or dialysis when the study began.
During an average five-year follow-up, 6% were diagnosed with dementia. As kidney function decreased, the rate of dementia increased, the researchers found.
Rates of dementia were more than four times higher among those with a kidney filtration rate below 30 mL per minute, compared to those with a normal filtration rate of 90 to 104 mL per minute, according to the study authors.
After adjusting for other dementia risk factors , the researchers concluded that compared to people with normal kidney function, people with filtration rates of 30 to 59 mL per minute had a 71% higher dementia risk. People with filtration rates below 30 mL had a 162% higher risk.
Xu noted that the risk of dementia, as with chronic kidney disease, increases with age.
Women Face A More Significant Risk Than Men
We have discussed the relationship between sex and Alzheimers in the past. You can access this article here: Sex Differences Between Men and Women Are Believed to Impact Alzheimers Risk.
As stated in the article, of the approximately 5.7 million Americans living with Alzheimers, two-thirds are women. There are many potential variables that may help explain this phenomenon, including hormonal and genetic factors.
While studying older adults receiving dialysis, it was found that once again, women are affected more significantly than men. Based on their findings, the 10-year risk of developing dementia following dialysis treatment was 21 percent in men and 25 percent in women. In comparison, end-stage kidney disease tends to be more common in men although researchers are not sure why.
Once dialysis patients develop dementia, researchers found that the mortality rate doubles. In relation to this two-fold mortality risk, these effects were apparent regardless of sex, race, age, or the presence of other disease conditions.
It is important to note that these recent findings do not indicate that it is the dialysis treatment itself that is causing a higher risk of dementia and Alzheimers disease.
Read Also: Dementia Neurotransmitter
Disorders Of The Heart And Lungs
The heart and lungs provide the brain with oxygen and nutrients that are necessary for proper functioning. Age is often accompanied by vascular disease that interferes with cardiac output or lung disease that interferes with the delivery of oxygen to the brain. These underlying diseases can cause MaND as well as whats commonly known as vascular dementia . They can also affect alertness, memory, and executive function..
Causes And Risk Factors
Acute hepatic encephalopathy results from acute hepatic failure with severe brain swelling which varies according to the aetiology of liver disease, with patients with hepatitis B or non-A, non-B hepatitis having the highest incidence of this complication.
PSE frequently results from a precipitating factor, such as dietary protein overload, constipation or gastrointestinal bleeding. Other conditions are hypoglycaemia, hypoxia, or the use of sedative drugs, particulary benzodiazepines, may also precipitate PSE in cirrhosis patients.
The pathophysiology of uremic encephalopathy is complex and is considered a multifactorial process, and may initially reflect a neurotransmitter deficit. There is evidence that parathyroid hormone plays a role , since, in uremic patients, both the EEG abnormalities and the neuropsychiatric symptoms are improved by either parathyroidectomy or medical suppression of PTH . The mechanism whereby parathyroid hormone disturbs CNS function is unknown but could relate to facilitation of Ca2+ entry into the cell and consequent cell death.
Also Check: What Color Ribbon Is Alzheimer’s
Problems With Vision And Hearing
Sensory limitations, too, can create a picture like cognitive impairment that worsens as the affected person becomes increasingly isolated as a result of hearing or vision problems. Recent research has emphasized that there is a relationship between hearing loss and the risk for development of cognitive impairment.
Cognitive Impairment And Dementia
Cognitive impairment is defined as a new deficit in two or more areas of cognitive function. In milder forms, cognitive impairment may not interfere with daily functioning. In contrast, dementia is characterised by persistent cognitive decline and behavioural disturbance that is severe enough to interfere with independence and daily functioning. CKD is an independent risk factor for progressive cognitive impairment and dementia. Dementia presents an important clinical complication as it can result in poor health literacy, medical adherence and is a powerful predictor of mortality in dialysis patients., While cognitive impairment is recognised as a common complication of CKD, it remains poorly identified. The reported prevalence of cognitive impairment in dialysis is estimated at between 30% and 60% while less than 5% of patients have clinically documented histories of cognitive impairment.
Evidence suggests that both the prevalence and progression of cognitive impairment are inversely associated with the level of kidney function. Several large population-based studies have demonstrated an increased risk of cognitive decline in the presence of moderate CKD including an 11% increased prevalence of cognitive impairment per 10mL/min/1.73m2 decrease in eGFR.
Diagnosis and management
Acute manifestations of altered mental status
Don’t Miss: Dementia Paranoia Accusations
Patients On Kidney Dialysis Have A Higher Risk Of Dementia
There is no denying the importance of dialysis for patients living with potentially fatal kidney diseases. Being a life-saving treatment, this intervention allows patients to better manage their illnesses.
As stated by the National Kidney Foundation, nearly 500,000 Americans currently rely on this treatment to survive. However, researchers are now concerned that this treatment may also increase the risk of dementia in older adults. This is particularly true for women and minorities.
Neuropsychiatric Disorders In Chronic Kidney Disease

- 1Interdisciplinary Laboratory of Medical Investigation, Faculty of Medicine, UFMG, Belo Horizonte, Brazil
- 2Laboratory of Neurobiology, Department of Morphology, Institute of Biological Sciences, UFMG, Houston, Brazil
- 3Neuropsychiatry Program, Department of Psychiatry and Behavioral Sciences, McGovern Medical School, University of Texas Health Science Center at Houston, Houston, TX, United States
Also Check: What Is The Color For Dementia
Baseline Characteristics Of Esrd And Non
A total of 99,158 ESRD patients and 927,142 non-ESRD subjects were finally enrolled for analysis . Table summarizes the differences in the demographic data between the ESRD and non-ESRD groups. The mean age of the ESRD group was greater than that of the non-ESRD group . Male subjects slightly dominated in the non-ESRD group, and the proportion of men and that of women were nearly identical in the ESRD group. In addition, ESRD patients were more likely to have the concomitant comorbidities than those non-ESRD individuals.
What You Can Do For Your Loved One
Besides managing symptoms, as a family caregiver you can help by communicating what end-of-life kidney failure signs you are seeing to the patients doctor and the hospice care team. Additionally, as a loved one, you can help the patient get their affairs in order. And finally, if it hasnt been done already, by contacting a hospice services provider as soon as possible.
Don’t Miss: What Is The Difference Between Dementia And Senility
Data Synthesis And Analysis
Random-effects meta-analysis was used to generate pooled odds ratios and their 95% confidence intervals . Tests were 2-sided at an level of 0.05. Estimates from crude as well as most fully adjusted models available were used. Heterogeneity among studies was assessed using the I2 statistic. Possible publication bias was assessed by funnel plots and the Egger test. Separate meta-analyses were only conducted for different levels of eGFR and albuminuria. All analyses were done with Stata 13.1 .
Ace Inhibitors And Angiotensin Receptor Blockers And Beta
ACE inhibitors and angiotensin receptor blockers have been shown to improve cognitive function in both hypertension and HF. Beta-blockers worsen dizziness and hypotension in HF which is a theoretical risk for worsening cognitive function in fragile elderly HF patients. Sacubitril/valsartan in the PARADIGM-HF trial, whilst reducing mortality and morbidity was associated with more hypotension compared to patients randomized to enalapril, and there is an as yet unresolved concern about its potential to promoting Alzheimers disease via inhibition of NEP degradation of -amyloid and the potential accumulation of A in the brain. However, analyses of PARADIGM did not find any increased risk of dementia or Alzheimers.,
Devices used to treat HF such as left ventricular assist devices carry an increased risk of embolic stroke, bleeding, and thrombotic complications. Changes in systemic immune state, platelet function, and acquired von Willebrand syndrome may potentially lead to cerebral infarction and haemorrhage. Other devices such as Veno-arterial extracorporeal membrane oxygenation are similarly thought to lead to an increased risk of thrombosis, bleeding, and neurologic events.
Don’t Miss: Does Meredith Have Alzheimer’s
How Hospice Can Help With End
Besides providing help in recognizing the signs of end-of-life kidney failure, hospice can help the family caregiver in managing their own needs. The team at Crossroads Hospice & Palliative Care includes nurses, volunteers, aides, social workers, and doctors who provide many different services, from personal care like grooming and bathing, to help with managing the patients medication.
If you would like to learn more about how Crossroads can help, we recommend you contact us now by selecting one of the Get Help options from the blue help center bar at the top of this page.
Associations Between The Rate Of Egfr Decline And The Risk Of Dementia
There were 205,622 participants who had at least 2 eGFR measurements within the first year of data collection. These individuals were included in the analysis of eGFR change in regard to dementia risk. The median number of plasma creatinine measurements per individual used to calculate the eGFR slope was 3 , ranging from 2 to 17. During a mean subsequent follow-up of 4.5 years, there were 11,175 cases of all-cause dementia, 4,692 cases of Alzheimer dementia, and 2,495 cases of vascular dementia. The mean eGFR slope was 1.17 mL/min/y .
In multivariable-adjusted analyses, a steeper eGFR decline was associated with a higher risk of all-cause dementia , with statistically significant associations for declines > 2 mL/min/y . Similar associations, but stronger in magnitude, were also observed between the rate of eGFR decline and the risk of vascular dementia. Less clear association was observed for Alzheimer dementia .
Hazard ratios for all-cause dementia risk by the rate of kidney function decline using linear splines. Model adjusted for baseline eGFR, sex, chronic smoking, alcohol abuse, diagnosed obesity, comorbid conditions , and medications . Knots were set at 3, 1, 0, and 1 mL/min/y. Data were reported as HRs and 95% confidence intervals . Percentage of participants across eGFR slope values.
You May Like: Alzheimer Awareness Ribbon Color
Monitoring Cognitive Function In Heart Failure
Multiple validated questionnaires exist to screen for, and to an extent, grade cognitive impairment. These include the Mini-Mental Status Examination and the Montreal Cognitive Assessment . Mildest on the spectrum of cognitive decline syndromes is mild cognitive impairment . It is advisable to screen for cognitive impairment, as it is similarly for depression when a patient is admitted with acute HF. Screening and review should also be regularly performed in the outpatient review setting, although primary care can often pick up earlier milder changes, perhaps being reported by carers and family members. The MMSE has been used to screen for cognitive deficits, but it is not very sensitive in detecting MCI. The MoCA has been said to be more sensitive to subtle changes. These screening tools can be helpful in differentiating acute from chronic cognitive decline in HF. The questionnaires detect clinical cognitive decline, whereas the pathophysiological antecedents may be there months or years earlier. For example, cerebral atrophy, white matter hyperintensities, loss of grey matter, and silent cerebral infarcts are frequent imaging findings in HF patients with and without cognitive dysfunction.,
How Does Kidney Disease Impact The Brain
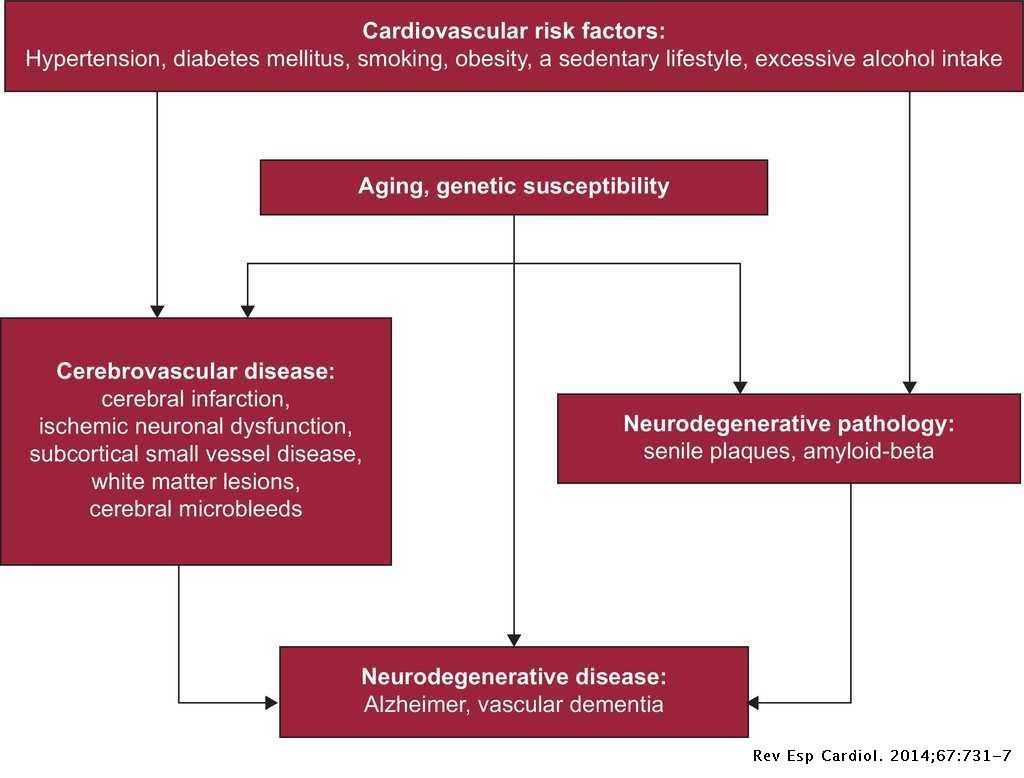
Numerous studies have suggested theres a connection between ESRD and cognitive impairment. Some researchers even suggest that some element of kidney failureor the dialysis treatments that combat itcould be responsible for cognitive decline and dementia. However, its important to note that this cognitive impairment isnt limited to patients with ESRD. There have been signs in patients in all stages of chronic kidney disease.
Kidney disease presents a number of factors that could potentially impact brain function, such as high blood pressure. High blood pressure is both a cause and a symptom of CKD, and is also known to cause a variety of neurological problems. This can be attributed to its risk of blocking blood from accessing the brain. Kidney disease can also lead to a high creatinine level in the blood, or a buildup of other toxins, such as Cystatin-C, which can affect brain function as well.
Finally, kidney disease increases ones risk of developing a urinary tract infection , which is associated with acute instances of confusion and delirious behavior in older adults. These symptoms can look very similar to dementia.
You May Like: Does Meredith Grey Have Alzheimer’s