Medications To Maintain Mental Function In Alzheimer’s Disease
Several medications are approved by the U.S. Food and Drug Administration to treat symptoms of Alzheimers. Donepezil, rivastigmine, and galantamine are used to treat the symptoms of mild to moderate Alzheimers. Donepezil, memantine, the rivastigmine patch, and a combination medication of memantine and donepezil are used to treat moderate to severe Alzheimers symptoms. All of these drugs work by regulating neurotransmitters, the chemicals that transmit messages between neurons. They may help reduce symptoms and help with certain behavioral problems. However, these drugs dont change the underlying disease process. They are effective for some but not all people and may help only for a limited time.
The Basics Of Alzheimers Disease
Scientists are conducting studies to learn more about plaques, tangles, and other biological features of Alzheimers disease. Advances in brain imaging techniques allow researchers to see the development and spread of abnormal amyloid and tau proteins in the living brain, as well as changes in brain structure and function. Scientists are also exploring the very earliest steps in the disease process by studying changes in the brain and body fluids that can be detected years before Alzheimers symptoms appear. Findings from these studies will help in understanding the causes of Alzheimers and make diagnosis easier.
One of the great mysteries of Alzheimers disease is why it largely affects older adults. Research on normal brain aging is exploring this question. For example, scientists are learning how age-related changes in the brain may harm neurons and affect other types of brain cells to contribute to Alzheimers damage. These age-related changes include atrophy of certain parts of the brain, inflammation, blood vessel damage, production of unstable molecules called free radicals, and mitochondrial dysfunction .
Managing Alzheimer’s Disease Behavior
Common behavioral symptoms of Alzheimers include sleeplessness, wandering, agitation, anxiety, and aggression. Scientists are learning why these symptoms occur and are studying new treatments drug and nondrug to manage them. Research has shown that treating behavioral symptoms can make people with Alzheimers more comfortable and makes things easier for caregivers.
Read Also: What Are The Signs Of End Stage Dementia
Jelly Drops: An Exciting New Invention To Help Combat Dehydration In Dementia
Inspired by his grandmother, Lewis Hornby has invented bite-sized sweets known as Jelly Drops to help reduce dehydration in dementia.Alzheimers Society was delighted to partner with Lewis and the Jelly Drops team this year through our Accelerator programme. Together, we’re working on bringing their fantastic product to people living with dementia.
Current Management Of Ad

A multifactorial tailored management of AD is attempted nowadays based in the following components:
FDA-approved AD medications
The AChEIs donepezil, galantamine, rivastigmine, and the NMDA antagonist memantine are the only FDA-approved AD medications.10
AChEIs attempt at reducing the breakdown of acetylcholine levels in the brain of the patients with AD by inhibiting the responsible enzyme acetylcholinesterase in the synaptic cleft.5 Thus, AChEIs enhance central cholinergic neurotransmission and finally tend to mitigate decline in cognition at least during the first year of treatment. Further decline occurs, but even temporary discontinuation of these drugs results in rapid decline and is associated with greater risk of nursing home placement.16
Recommended Reading: Does Johnny Crawford Have Alzheimer’s
What The Results Say
The researchers found that when the amyloid-beta proteins made in the liver of the test mice combined with fats and traveled to the brain, they interfered with the proper functioning of the brains microscopic blood vessels, or capillaries.
This dysfunction in the blood-brain barrier led to the protein-fat complexes leaking from the blood into the brain, resulting in inflammation. This inflammation occurred in both the test group and the control group, but it started at a much younger age in the test group.
Unlike in the control group, this inflammation was also associated with marked degeneration in the brain cells of the mice in the test group when examined under a microscope. The scientists only rarely saw this neurodegeneration in the control mice, and it was usually at a much older age.
The team also assessed a marker of neurodegeneration and found it to be approximately two times greater in the test mice than in control mice of the same age.
So, it was unsurprising that during the test for cognitive function, the test mice performed approximately half as well as the control group at retention of learning.
These findings suggest explanations to long standing questions about the role of amyloid-beta in Alzheimers disease development.
Warren Harding, board chairman of Alzheimers WA, revealed to MNT the significance of the study results. He said:
Challenges For The Alzheimers Research Community
Even with the progress that weve made, there’s still a lot of work to do before we can find treatment and prevention strategies for the millions of people affected by Alzheimers and related dementias. These devastating diseases are highly complex conditions caused by an interplay of genetic, lifestyle, and environmental factors. They usually develop gradually changes in the brain take place over years and even decades, long before the first symptoms appear. This complexity presents challenges to the discovery and development of new drugs and other prevention and treatment approaches. Alzheimers disease does not affect all communities at the same rate, and research has found that a persons likelihood of getting Alzheimers can be affected by their sex, ethnicity, race, socioeconomic status, and other factors. These differences are called health disparities.
Researchers believe Alzheimers disease and related dementiaswill likely require multipletreatments customized to individuals.We also know that as the older adult population continues to grow aging remains the most important risk factor fordementia we will see increased numbers of people living with these diseases. Thats why thousands of researchers around the country are working on this issue.
Don’t Miss: Avalon Alzheimer’s Arlington Tx
What Causes Alzheimers Disease
In recent years, scientists have made tremendous progress in better understanding Alzheimers and the momentum continues to grow. Still, scientists dont yet fully understand what causes Alzheimers disease in most people. In people with early-onset Alzheimers, a genetic mutation may be the cause. Late-onset Alzheimers arises from a complex series of brain changes that may occur over decades. The causes probably include a combination of genetic, environmental, and lifestyle factors. The importance of any one of these factors in increasing or decreasing the risk of developing Alzheimers may differ from person to person.
What The Data Show
The late-stage development program for Aduhelm consisted of two phase 3 clinical trials. One study met the primary endpoint, showing reduction in clinical decline. The second trial did not meet the primary endpoint. In all studies in which it was evaluated, however, Aduhelm consistently and very convincingly reduced the level of amyloid plaques in the brain in a dose- and time-dependent fashion. It is expected that the reduction in amyloid plaque will result in a reduction in clinical decline.
We know that the Peripheral and Central Nervous System Drugs Advisory Committee, which convened in November 2020 to review the clinical trial data and discuss the evidence supporting the Aduhelm application, did not agree that it was reasonable to consider the clinical benefit of the one successful trial as the primary evidence supporting approval. The option of Accelerated Approval was not discussed by the Advisory Committee. As mentioned above, treatment with Aduhelm was clearly shown in all trials to substantially reduce amyloid beta plaques. This reduction in plaques is reasonably likely to result in clinical benefit. After the Advisory Committee provided its feedback, our review and deliberations continued, and we decided that the evidence presented in the Aduhelm application met the standard for Accelerated Approval. We thank the Advisory Committee for its independent review of the data and valuable advice.
You May Like: Doctors Who Deal With Dementia
Who Funds Alzheimers And Related Dementias Research
The National Institutes of Health is made up of Institutes, Centers, and Officesthat conduct and fund research into all aspects of human health. The National Institute on Aging leads NIHs efforts in clinical, behavioral, and social research in Alzheimers and related dementias through efforts aimed at finding ways to treat and ultimately prevent the disorder. NIA collaborates closely with the National Institute of Neurological Disorders and Stroke , which manages a research portfolio targeting Alzheimers disease-related dementias.While some of this research takes place in NIH laboratories, the vast majority of NIH support is provided through a competitive grants process to institutions and small businesses across the country. Other federal agencies support a range of activities focused on public health and community programs.
What Is A Professional Judgment Budget
Each year NIH submits a professional judgment budget that estimates the additional funding needed to advance NIH-supported research into the treatment and prevention of Alzheimers disease and related dementias. The report also summarizes progress and promising research opportunities. Only two other areas of biomedical research cancer and HIV/AIDS follow a similar process designed to accelerate research discovery. This approach is often referred to as a bypass budget because of its direct transmission to the President and then to Congress without modification through the traditional federal budget process.
You May Like: Caring For Alzheimer’s Parent
Love Island Star And Olympian Greg Oshea To Run London Marathon For Alzheimers Research Uk In Memory Of Grandmother
Love Island favourite and former international rugby player Greg OShea will run the TCS London Marathon in October to support the work of Alzheimers Research UK. Greg, who won the hit reality show in 2019, will be running in memory of his grandmother, Monica Ho, who passed away with dementia while he was in the
Researchers Have Identified A New Type Of Dementia
In May, an international team of researchers identified a brain disorder known as LATE. It has similar symptoms to Alzheimers disease but appears to be caused by the build up of the toxic protein TDP-43.
Our researchers were able to delve into this particular protein by studying human brain tissue through our initiative Brains for Dementia Research.
The finding will help us distinguish between different brain disorders and develop precise and personalised treatments.
Also Check: Safety For Alzheimer’s Patients
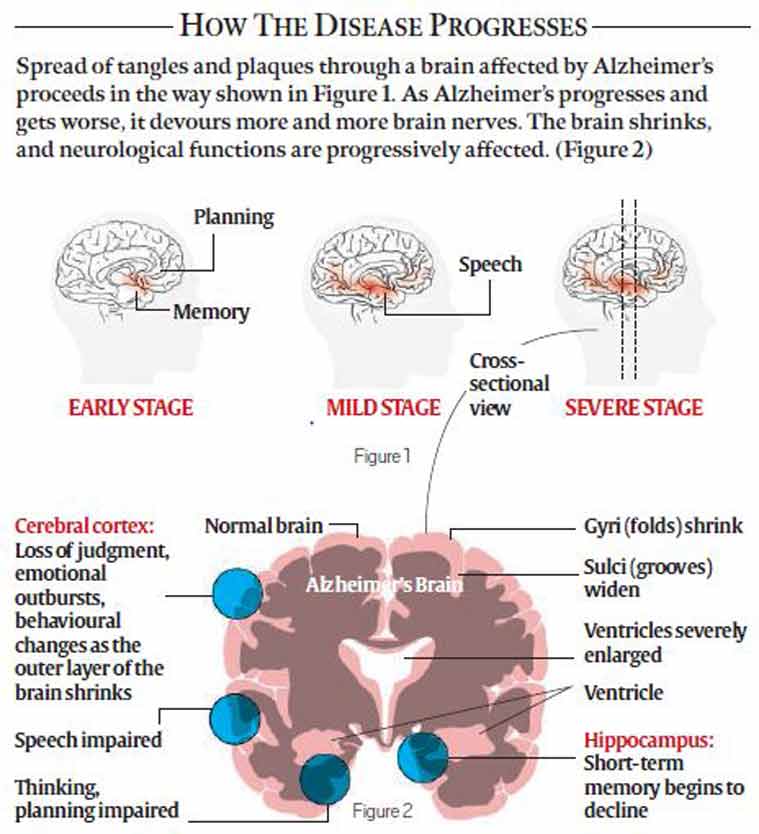
How Does Alzheimer’s Disease Affect The Brain
Scientists continue to unravel the complex brain changes involved in Alzheimers disease. Changes in the brain may begin a decade or more before symptoms appear. During this very early stage of Alzheimers, toxic changes are taking place in the brain, including abnormal buildups of proteins that form amyloid plaques and tau tangles. Previously healthy neurons stop functioning, lose connections with other neurons, and die. Many other complex brain changes are thought to play a role in Alzheimers as well.
The damage initially appears to take place in the hippocampus and the entorhinal cortex, which are parts of the brain that are essential in forming memories. As more neurons die, additional parts of the brain are affected and begin to shrink. By the final stage of Alzheimers, damage is widespread and brain tissue has shrunk significantly.
What Kinds Of Research Can You Participate In
Research involving people is called clinical research. There are two types of clinical research studies: observational studies and clinical trials.
- Observational studies are designed to collect information from people and compare that data over time. This helps them learn how different behaviors or lifestyles relate to health and disease and to understand how a disease progresses over time.
- Clinical trials are a type of research that tests new drugs, medical devices, surgical procedures, or behavior and lifestyle changes, such as exercise. Clinical trials may also test ways to detect and diagnose diseases and to better care for those living with diseases. Researchers determine if what is being tested, called an intervention, is safe and effective by comparing results in the test group to those in the control group.
The Alzheimers.gov Clinical Trials Finder includes listings for both kinds of clinical research studies.
Read Also: How To Talk To Someone With Early Dementia
Clinical Research Into Alzheimers And Related Dementias
No major advance in Alzheimers and related dementias treatment, prevention, or care will be possible without robust clinical research. Clinical research includes studies that involve people so scientists can learn more about disease progression, how behavior and lifestyle factors may affect health, and the safety and effectiveness of an intervention. Advances made through clinical research rely on the volunteers who participate in these types of studies. NIA is working on multiple initiatives to enhance recruitment and retention of diverse populations in clinical research. View some of those resources below.
NIA-funded clinical research includes both observational studies through which researchers gather important information, and clinical trials in which researchers test interventions to treat or prevent disease, improve care and caregiver support, and enhance quality of life for people living with dementia.NIA is currently funding more than 200active clinical trials.
NIA also funds more than 30 Alzheimers Disease Research Centers across the country. Scientists at these centers conduct clinical research to improve diagnosis and care for people with dementia and their families, and to find a treatment or prevention.
How Is Alzheimers Disease Treated
Alzheimers is complex, and it is therefore unlikely that any one drug or other intervention will successfully treat it in all people living with the disease.
Scientists are exploring many avenues to delay or prevent the disease as well as to treat its symptoms. In ongoing clinical trials, scientists are developing and testing several possible interventions. Under study are drug therapies aimed at a variety of disease interventions, as well as nondrug approaches such as physical activity, diet, cognitive training, and combinations of these. Just as we have many treatments for heart disease and cancer, we will likely need many options for treating Alzheimers. Precision medicine getting the right treatment to the right person at the right time will likely play a major role.
Current approaches to treating Alzheimers focus on helping people maintain mental function, treating the underlying disease process, and managing behavioral symptoms.
Recommended Reading: Does Music Help With Dementia
Signs And Symptoms Of Alzheimer’s Disease
Memory problems are typically one of the first signs of cognitive impairment related to Alzheimers. Some people with memory problems have a condition called mild cognitive impairment . With MCI, people have more memory problems than normal for their age, but their symptoms do not interfere with their everyday lives. Movement difficulties and problems with the sense of smell have also been linked to MCI. Older people with MCI are at greater risk for developing Alzheimers, but not all of them do so. Some may even revert to normal cognition.
The first symptoms of Alzheimers vary from person to person. For many, decline in nonmemory aspects of cognition, such as word-finding, vision/spatial issues, and impaired reasoning or judgment may signal the very early stages of the disease. Researchers are studying biomarkers to detect early changes in the brains of people with MCI and in cognitively normal people who may be at greater risk for Alzheimers. More research is needed before these techniques can be used broadly and routinely to diagnose Alzheimers in a health care providers office.
Assessing Alzheimer’s And Dementia Risk
Biomarkers helpful in identifying Alzheimer’s diseaseBiological measures of brain health can be useful in identifying clinical Alzheimer’s-type dementia , according to 2020 review study by the Minneapolis VA Health Care System and the University of Minnesota. Currently, the only way to confirm Alzheimer’s disease is to conduct an autopsy of the brain following death. The research team examined the efficacy of two different types testsbrief cognitive assessments and clinical biomarkersfor distinguishing Alzheimer’s disease and other causes of dementia in living people.
The researchers found cognitive assessments were highly accurate in identifying CATD, but were less accurate in distinguishing mild cognitive impairment from CATD.
The biomarker tests included amyloid PET scans, which map the build-up of amyloid protein fluorodeoxyglucose -PET scans, which map how the brain absorbs glucose and MRI testing, which detects changes in the temporal lobe of the brain, including the hippocampus. The team also assessed single-photon emission computed tomography and cerebral spinal fluid testing. The first three tests provided dementia diagnoses that were more than 90% accurate.
According to the research team, more accurate diagnoses of dementia in living patients can help direct clinical decision making on the best treatments for individuals. More accurately identifying different types of dementia can also help direct patients to clinical trials.
Also Check: How Long Does The Later Stage Of Dementia Last
Understanding The Causes And Mechanisms Of Alzheimer’s Disease
Neuroimaging InitiativeThe Alzheimer’s Disease Neuroimaging Initiative was established in 2004 to find new ways to diagnose and predict the onset of Alzheimer’s disease. VA researcher Dr. Michael Weiner is founder and principal investigator for ADNI. Weiner is affiliated with the VA-University of California Center for Imaging of Neurodegenerative Diseases located at the San Francisco VA Health Care System.
The $67 million initiativefunded by the National Institute on Aging and other partnersseeks to identify brain changes linked to Alzheimer’s disease. The funds are administered by a VA nonprofit corporation, the Northern California Institute for Research and Education . The program is coordinated by the Alzheimers Therapeutic Research Institute at the University of Southern California. ADNI is now in its third phase, in which researchers are working to validate biomarkers for Alzheimer’s disease clinical trials. ADNI-3 began in 2016 and will run through 2021.
ADNI-1 researchers found that people with Alzheimer’s disease can have high levels of a protein called beta-amyloid 42 in their brains. While dementia can result from any number of health problems, such as strokes, amyloid buildup happens only in patients with Alzheimer’s. At present, amyloid levels can be determined only through spinal taps or special diagnostic imaging.