Assessment Of Mr In Dementia
* Lewi = Dementia with Lewi bodies
An MR-study of a patient suspected of having dementia must be assessed in a standardized way.First of all, treatable diseases like subdural hematomas, tumors and hydrocephalus need to be excluded.
Next we should look for signs of specific dementias such as:
- Alzheimer’s disease : medial temporal lobe atrophy and parietal atrophy.
- Frontotemporal Lobar Degeneration : frontal lobe atrophy and atrophy of the temporal pole.
- Vascular Dementia : global atrophy, diffuse white matter lesions, lacunes and ‘strategic infarcts’ .
- Dementia with Lewy bodies : in contrast to other forms of dementia usually no specific abnormalities.
So when we study the MR images we should score in a systematic way for global atrophy, focal atrophy and for vascular disease .
When we study the MR images we must systematically score for global atrophy, focal atrophy and for vascular disease . This standardized assessment of the MR findings in a patient suspected of having a cognitive disorder includes:
The central sulcus is more posteriorly on more cranial images.
Planning For The Future
Planning early makes it easier for someone with younger onset dementia to manage their financial, legal and medical affairs now and in the future.
If you have been diagnosed with younger onset dementia, it is important to make important decisions while you still can and while you are legally competent to sign any documents.
Things to think about include:
- your living arrangements into the future
- who can have access to your financial accounts
- having joint signatures on all financial accounts
- arranging when and how you will access your finances
- talking to a financial adviser
- sorting out superannuation, health and income insurance
- writing or updating your will
If you have been diagnosed with dementia, its important to nominate a trusted person to manage your affairs in the future. You can do this through an Enduring Power of Attorney .
A financial EPA enables a nominated person to look after your financial affairs if you become unable to do so. A medical EPA covers only medical decisions. The laws regarding EPAs vary between states and territories, so it’s important to seek legal advice before the agreement is completed, or if you are moving interstate.
Some states also have medical guardianship . This allows someone to choose a person to make medical decisions for them. For more information on guardianship and administrators, visit the My Aged Care website.
What Are The Symptoms Of Younger Onset Dementia
The symptoms of dementia are similar no matter what age they start. They include:
- memory loss that interferes with daily life
- confusion
- withdrawing from friends and family
- losing the ability to think clearly or make judgements
- language problems
- changes to behaviour
Many conditions can produce symptoms that are similar to dementia, such as vitamin and hormone deficiencies, depression, medication, infections and brain tumours.
Recommended Reading: Does Meredith Get Alzheimer’s
Neuropsychiatric Manifestations Of Covid
Manifestations such as insomnia, anxiety, post-traumatic stress symptoms , psychosis and mood disorders have been described in several reports . A study that retrieved data from a global health collaborative platform that included medical records of 40,469 COVID-19 positive cases, mostly from the United States , found that 22.5% had neurological and/or psychiatric manifestations, being anxiety and related disorders the most prevalent .
Table 1. Neuropsychiatric manifestations of COVID-19.
Critically ill patients with COVID-19 who require Intensive Care Unit admission are also at most at risk of developing delirium, which is further exacerbated by the frequent need for high doses of sedation, elderly age and the presence of multiple comorbidities . In an observational study in France, 40 out of 58 COVID-19 patients attended in the ICU showed agitation and 26 of them confusional state . Brain imaging found bilateral frontotemporal hypoperfusion in eleven patients and larger leptomeningeal spaces in eight of them .
There is also evidence of prevalent depressive symptoms in those already recovered from COVID-19 . A study of 126 COVID-19 survivors in convalescence from Shenzhen, China, showed that self-reported anxiety and depression were common after discharge from hospital and moreover, depressive symptoms were associated with immune systemic suppression, based on increased white blood cells and inflammatory factors measures .
Frederik Barkhof Marieke Hazewinkel Maja Binnewijzend And Robin Smithuis

Alzheimer Centre and Image Analysis Centre, Vrije Universiteit Medical Center, Amsterdam and the Rijnland Hospital, Leiderdorp, The Netherlands
Publicationdate 2012-01-09
This review is based on a presentation given by Frederik Barkhof at the Neuroradiology teaching course for the Dutch Radiology Society and was adapted for the Radiology Assistant by Robin Smithuis.First publication: 1-3-2007.Updated version: 9-1-2012.This presentation will focus on the role of MRI in the diagnosis of dementia and related diseases.We will discuss the following subjects:
- Systematic assessment of MR in dementia
- MR protocol for dementia
- Typical findings in the most common dementia syndromes
- Alzheimer’s disease
You May Like: Dementia Ribbon Colour
Abbreviated Mental Test Score
The Abbreviated Mental Test Score is a 10-item scale derived from a longer scale introduced previously . Any clinician can use this, and it takes only 34 min. It assesses orientation, registration, recall and concentration, and scores of 6 or below have been shown to screen effectively for dementia, though as with many brief screens, low positive predictive values mean a second-stage assessment is always necessary . Its brevity and ease of use have made it popular as a screening test in primary and secondary care nonspecialist settings.
Resistance To Visiting A Doctor
Some people may be resistant to the idea of visiting a doctor. In some cases, people do not realise, or else deny, there is anything wrong with them. This can be due to the brain changes of dementia that interfere with the ability to recognise or appreciate one’s memory problems. Others, with retained insight, may be afraid of having their fears confirmed.
Dealing with resistance to visiting the doctor
One of the most effective ways to overcome this problem is to find a physical reason for a visit to the doctor, preferably a check-up for a symptom that the person is willing to acknowledge, such as headaches or failing eyesight. Perhaps suggest an examination of the heart, a test for blood pressure or diabetes, or a review of long term medication. Another way is to suggest that it is time for you BOTH to have a physical check up. Any expressed anxiety by the person is an excellent opportunity to suggest a visit to the doctor. Be sure to provide a lot of reassurance. Calm, caring attitude at this time can help overcome the person’s very real worries and fears.
If the person will not visit the doctor:
- Talk with other carers who may have had to deal with similar situations
- Contact the Aged Care Assessment Team
You May Like: Margaret Thatcher Dementia
Tentative Research Criteria Upon Which To Test And Validate Explanatory Models
As outlined above, the interplay between chronic pain and associated neuropsychiatric symptoms is complex and only poorly understood so far. Recently, it was suggested that at an individual level, the complex interplay of pain, aging and dementia is modulated by predispositions as well as lifelong and current biopsychosocial factors . However, research focusing on the social dimensions of pain in dementia is sparse. Thus, the biopsychosocial model seems a promising framework that awaits further empirical evidence.
In the following, we propose a conceptual framework illustrating how to translate clinical issues to relevant research questions. As depicted in Fig. 2 , relevant research questions need to be addressed empirically to generate new explanatory models . Consequently, these new explanatory models might help to develop alternative diagnostic and treatment approaches which in turn need to be validated. Finally , findings of the latter validation should be fed into a so-called application loop targeted at evaluating and, if needed, modifying previous explanatory models. Ideally, an empirically validated and adapted explanatory model can be used as a clinical guide to reliably identify perceived pain and associated neuropsychiatric symptoms in non-communicating patients with dementia .
What Happens After A Diagnosis Of Younger Onset Dementia
A diagnosis of younger onset dementia can come as a shock. The person affected, and their family and friends may all feel angry or sad. They might not believe it. There can be a huge sense of loss. These feelings are normal.
But help and support is available, and it is better to get it earlier than later.
Younger people with dementia need to think about several issues.
Also Check: Dementia Ribbon Color
Interview With The Patient
Although subjects with dementia may be handicapped in their communication and social skills, it is essential to have an individual assessment with them. Whenever possible, it is desirable that patients are encouraged to express their own concerns in answer to open questions before proceeding to a more systematic approach to specific symptoms. Patients free descriptions are least prone to be influenced by the interviewer and/or caregiver and can provide crucial information about emotional states underlying behaviors.
What Are The Risk Factors For Dementia
The risk factors for developing dementia include age and family history. Age and a family history of dementia are non-modifiable risk factors. Abnormal genes which are associated with Alzheimer’s disease have been identified, but are only rarely involved in the development of Alzheimer’s disease. Conditions such as high blood pressure, high cholesterol, or diabetes increase the risks of developing either Alzheimer’s disease or multi-infarct dementia. Some medications can lead to memory problems which look like dementia.
Also Check: What Is The Difference Between Dementia And Senility
What Is The Treatment For Dementia
Treatment options for Alzheimer’s disease and other dementia are limited. While there are medications available to try to improve the symptoms of Alzheimer’s disease, the effect of these medications is limited. Physical exercise has been shown to be of some benefit in helping to maintain cognition. Staying engaged and participating in social events may also be of some help. To date, no treatment which can reverse the process of Alzheimer’s disease has been identified.
What Is Dementia Symptoms Types And Diagnosis
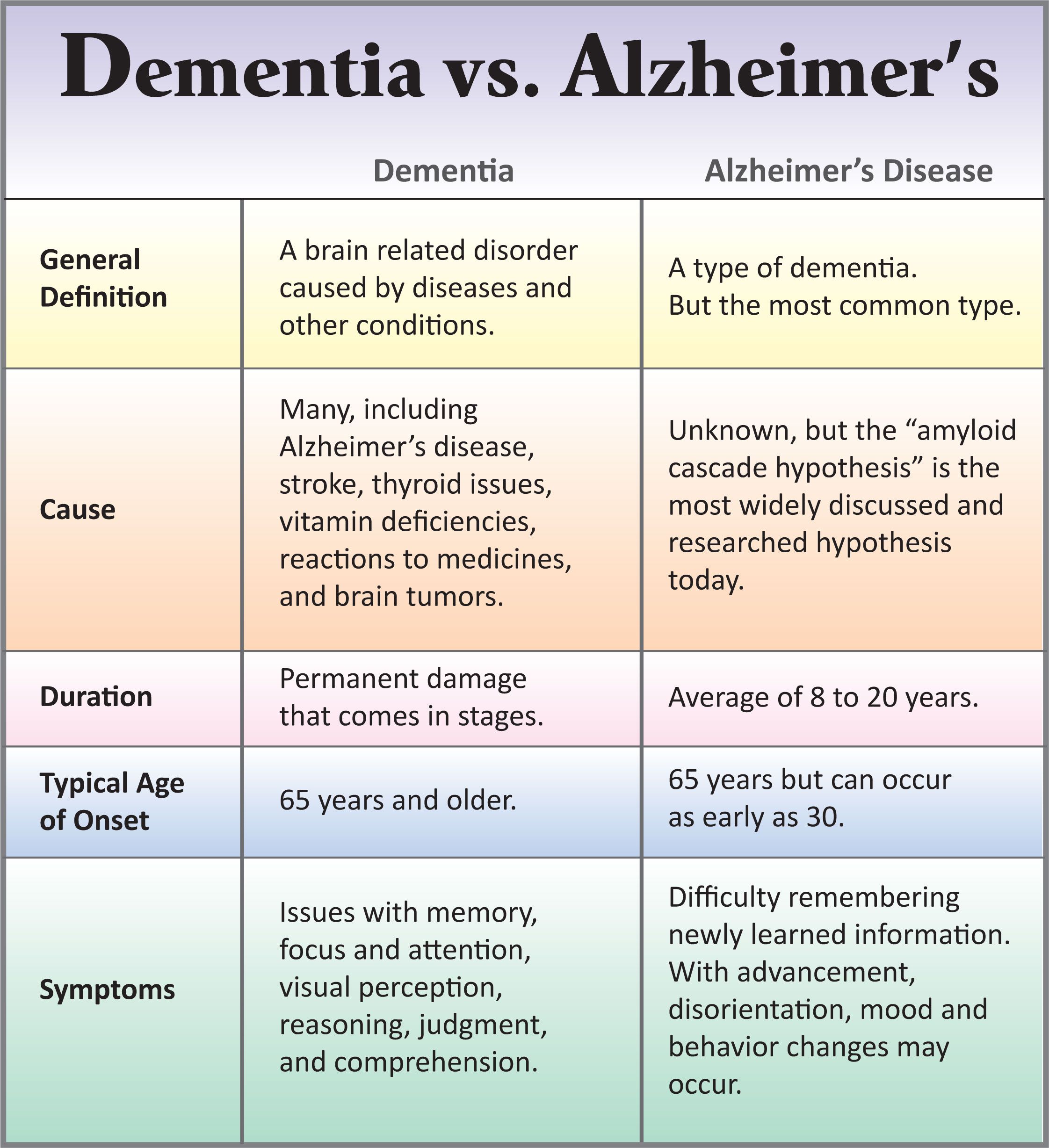
Dementia is the loss of cognitive functioning thinking, remembering, and reasoning to such an extent that it interferes with a person’s daily life and activities. Some people with dementia cannot control their emotions, and their personalities may change. Dementia ranges in severity from the mildest stage, when it is just beginning to affect a person’s functioning, to the most severe stage, when the person must depend completely on others for basic activities of living.
Dementia is more common as people grow older but it is not a normal part of aging. Many people live into their 90s and beyond without any signs of dementia.
There are several different forms of dementia, including Alzheimers disease. A persons symptoms can vary depending on the type.
Read Also: Does Meredith Grey Have Alzheimer’s
What Causes Younger Onset Dementia
Many different types of dementia can affect younger people. Each type has its own symptoms and is caused by a specific type of change in the brain. Some causes of early onset dementia are:
- Alzheimers disease
- problems with blood flow to the brain
- deterioration to the front part of the brain
- chronic overuse of alcohol over many years
What Causes Dementia
The causes of Alzheimers and related dementias can vary, depending on the types of brain changes that may be taking place. While research has found that some changes in the brain are linked to certain forms of dementia, in most cases, the underlying causes are unknown. Rare genetic mutations may cause dementia in a relatively small number of people.
Although there is no proven prevention, in general, leading a healthy lifestyle may help reduce risk factors that have been associated with these diseases.
Also Check: Parkinsons And Alzheimers Together
Where To Get Help
- Your local community health centre
- National Dementia Helpline Dementia Australia Tel. 1800 100 500
- Aged Care Assessment Services Tel. 1300 135 090
- My Aged Care 1800 200 422
- Cognitive Dementia and Memory Service clinics Tel. 1300 135 090
- Carers Victoria Tel. 1800 242 636
- Commonwealth Carelink and Respite Centres Australian Government Tel. 1800 052 222
- Dementia Behaviour Management Advisory Service Tel. 1800 699 799 for 24-hour telephone advice for carers and care workers
Aphasia In Alzheimers Disease
Alzheimer’s disease can cause aphasia, which is a decline in language function due to brain disease. Alzheimer’s disease is progressive dementia that causes impaired memory, judgment, and general cognitive functioning.
Aphasia in Alzheimer’s disease often begins with word-finding problems, such as difficulty choosing or recalling the right word. It can progress to affect your ability to express yourself, and it can involve comprehension too.
You May Like: What Color Represents Alzheimer’s
Getting Help Early Will Make A Difference
The earlier help is found, the better the family and person with the condition will be able to manage and cope. It is important to:
- plan ahead while the person can still legally sign documents, get enduring powers of attorney to manage financial affairs, medical decisions and guardianship
- get information find out about dementia and what lies ahead, so that you will be informed and have more sense of control
- seek support many people find it helpful to talk through what a diagnosis of dementia means and how they can make adjustments
- organise practical help organise help in the home, respite care, day trips and stays at day centres, which can all make a positive difference.
Cultural And Linguistic Considerations
Treatment occurs in the language used by the person with dementia, either by a bilingual SLP or through the use of trained interpreters, when necessary. See ASHA’s Practice Portal page on Bilingual Service Delivery.
Cultural influences and familial expectations may affect treatment decisions .
Cultural values, views of the aging process, and religious and spiritual beliefs relative to cognitive decline may influence a family’s decisions about therapeutic services. For example, families may not seek help, or they may delay seeking help until symptoms are beyond early or mild stages . Families may fear the stigma of dementia, and this can also affect decisions about seeking help .
Dementia can have a significant impact on individuals in the LGBTQ community. For example, transgender individuals with dementia may experience periods of confusion about medical issues related to their natal gender , or about self-care and other daily tasks related to external gender changes . Dementia may also make it challenging for LGBTQ individuals to manage disclosurethey may lose some ability to determine whom they share this information with .
Older LGBTQ individuals with dementia often experience a loss of identity, as a lack of cultural competence can lead to discrimination on the basis of age, sexuality and the stigma associated with dementia . Care facilities should be sensitive to the needs of older LGBTQ patients and provide them with accommodations consistent with their expression .
Also Check: What Color Ribbon Is Alzheimer’s
Ethics Approval And Consent To Participate
NHS Research Ethics Committee approval was obtained both in England and Scotland . The process to recruit patients was informed by the Mental Capacity Act 2005 and the Adults with Incapacity Act 2000 it included written consent by patients or agreement from a carer consultee, patients capacity assessment to consent, consultation with staff and assent of carers. Interviewees gave their written consent and were informed of the audio-recording. The NHS trusts participating in this study reviewed the study and granted access to the researchers, in compliance with local requirements for data collection.
Generic Measures Of Quality Of Life
EuroQol
The EuroQol measure is a short, freely available generic measure of health-related quality of life. It can be simply administered to patients or carers in the form of a very brief self-completed questionnaire. There are two core components to the instrument: a description of the respondents own health using a health state classification system with five dimensions, and a rating on a visual analogue thermometer scale. It takes 2 min to complete. Like many quality of life instruments, carer and proxy ratings diverge widely, many patients with dementia cannot fill out the instrument, and the chief use of EuroQoL in dementia is as a health utility measure for measuring the economic impact of interventions in trials.
Short Form-36
The Short Form-36 and its shorter descendant the SF-12 are examples of generic measures of quality of life which use recall over particular periods of time and are used to estimate health burden in large populations. These instruments have been shown to have high rates of noncompletion among frail older people and especially among those with moderate to severe dementia. They may have limited use for carers of people with dementia, but probably cannot routinely be used in practice with patients.
Read Also: What Is The Difference Between Dementia And Senility
Referral To A Specialist
You may be referred to a specialist service for further assessments. This might be a memory assessment service, memory clinic or other specialist service within a community mental health team. These services are set up especially to assess people with memory problems. They have teams of different types of health professionals who can look at your case in more detail.
Normally it will be the GP that refers you to a specialist centre for further assessment, if they think this is necessary. If you feel that a referral would be helpful, but the GP has not yet suggested it, you can ask them to refer you.
Sometimes people choose not to carry on with any further assessments – for example if they choose not to find out if they have dementia. If this is the case, you can tell the GP that you do not want to be assessed any further. A specialist will have more knowledge and experience of assessing dementia than a GP. They will also have more time allocated for appointments and access to more specialised investigations such as brain scans and in-depth mental testing. Once you have been referred, you should not have to wait longer than 4-6 weeks to see a specialist.
The GP will make the referral to a consultant with special expertise in a particular area of medicine. Who they refer you to may depend on your age and symptoms, and the kind of consultant available in your area. The main types are explained below.