Pet Imaging Of Neuroinflammation In Ad
A deposition and neurodegeneration in AD are associated with local glial response and microglial activation as an inflammatory response. 1–N-methyl-N–3-isoquinoline carboxamide is a specific ligand for the peripheral benzodiazepine binding receptor site, which is expressed on activated microglia. PET with PK11195 has been used to provide a quantitative in vivo measurement of glial activation and neuroinflammation in AD. Increased PK11195 binding was observed in patients with AD compared to healthy controls, involving the entorhinal, temporopariet al, and cingulate cortices. Moreover, cortical PK11195 binding correlated with cognition scores.
Pet Imaging Of Neuropathology In Ftld
Several types of neuropathological alterations underlie FTLD, including the presence or absence of tau and ubiquitin, while amyloid deposition is not a characteristic finding. On amyloid PET, patients with FTLD show low cortical PIB retention, with uptake values close to those seen in healthy controls, confirming the lack of amyloid deposition. For this reason, PIB is of great value in the differential diagnosis between FTLD and AD, especially in cases with atypical symptoms.
The ability of FDDNP to label NFTs suggests that this tracer could be useful in PET imaging of tauopathies, such as some cases of FTLD. Patients with FTLD show high FDDNP uptake in frontal and prefrontal regions compared to con-trols. While FTLD patients show increased tracer uptake in frontal and lateral temporal regions similar to AD patients, FDDNP uptake was lower than AD in pariet al cortex, showing a prominent frontal/temporal signal in contrast to the typical pariet al/medial temporal signal observed in AD. FDDNP could, therefore, provide a useful tool for evaluating the presence and extent of tau pathology in vivo, for differential diagnosis of FTLD from AD, and, possibly, to monitor the effect of therapies designed to prevent or slow down NFTs accumulation in both disorders.
The Mri Scan: How Can It Be Used In The Diagnosis Of Alzheimer’s
As medicine has improved in the last few decades, the role of these brain imaging studies has become more and more important in the diagnosis of the Alzheimer’s Disease and other neurological conditions. One of the key diagnostic tests is known as Magnetic resonance imaging the MRI.
In laymen’s terms, an MRI scan is an imaging study that relies on a magnetic field in order to get a good view of your internal organs. The magnetic field can actually influence the water molecules that are naturally found in your body in order to give a very refined picture of what is going on in your body. It is best to use this type of imaging for soft tissue the exact type of tissue that you will be looking at when you are investigating the brain.
An MRI scan can be a rather long examination for patients to endure and patients will need to lie as still as possible in order for doctors to get an accurate picture of the structures being investigated. During just a simple head investigation, patients may be asked to lie still for at least 30 minutes. This may sound like a simple task but the tubing in the room is rather small so many patients may not enjoy the slight claustrophobia that can easily occur. It is one of the best studies to do, though, so the accurate results are worth the slight discomfort for the patient.
Don’t Miss: Andrea Mitchell Drunk
How Does A Doctor Diagnose Dementia
The short answer to how Alzheimers disease is diagnosed in a living patient is through a series of memory and thinking tests that are administered face to face in the doctors office, brain scans, and biomarker tests.
Its important to mention that in a living patient the Alzheimers disease diagnosis is not 100% accurate. Depending on the tests performed, the accuracy can range from 80 to 95 percent in a living person. The only way to be sure that an individual has Alzheimers disease is to look at their brain following death.
Accurate mental status testing to rule out other conditions is key. There are people who have been diagnosed with Alzheimers disease but they have a different medical condition that may mimic it. There are also people who have been diagnosed with other conditions who actually have Alzheimers dementia.
We will cover the whole process from how to assess memory loss to how to get a dementia diagnosis with the highest level of accuracy possible in a living person.
Q: What Was Your Role In The Study
At the Center for Statistical Sciences we do a lot of large, multi-center studies of imaging. For example, screening studies for lung cancer and breast cancer. For the IDEAS study, I and my colleagues here at CSS were deeply involved in formulating the scientific questions of the study. A major question was how to evaluate the effectiveness of a diagnostic test when there are no therapeutic interventions for the disease itself, as it the case for Alzheimers. For somebody like me who has been thinking about diagnostic tests for a long time, it was an interesting challenge. Hence, there was a lot of brainstorming that needed to be done upfront about what is it that were going to evaluate, how might we evaluate it and how will we organize the study to evaluate it?
Recommended Reading: Alzheimer’s Aphasia
Is Alzheimers Diagnosed With A Blood Test
The other biomarker test, uses either a blood sample or, more commonly, a cerebral spinal fluid sample. The CSF sample is obtained via a spinal tap.
We look for markers of Alzheimers disease in the blood and the spinal fluid samples. These are pieces of the plaques and tangles that might be circulating in the blood or spinal fluid.
Therefore, the patient can have a thinking and memory test, and then typically the physician will add on additional tests. One could be a PET scan of the brain and the other one could be a test of either the blood or cerebral spinal fluid.
Diagnosing Alzheimers disease is a process. And its typically a combination of these three approaches: Cognitive Testing, PET biomarkers and fluid either blood or spinal biomarkers.
In all cases, personal results are compared to norms. The person is compared to other healthy people in the population that are approximately just like them. Neurologists look at the levels of all of the things that they are measuring to determine if they think its Alzheimers disease.
And thats how a diagnosis goes.
Fdg Pet Imaging In Ad
FDG PET imaging is used to measure cerebral metabolic rates of glucose , an index of brain synaptic activity and density. Several FDG PET studies have been performed to qualitatively and quantitatively estimate AD-related brain changes. These studies have consistently shown widespread metabolic deficits in the neocortical association areas, with sparing of the basal ganglia, thalamus, cerebellum, primary sensory motor cortex, and visual cortex. Specifically, the so-called AD metabolic pattern is characterized by hypometabolism in associative parietotemporal areas, posterior cingulate cortex, and precuneus, as well as medial temporal lobes, mostly entorhinal cortex and hippocampus . With advancing disease, hypometabolism extends to prefrontal cortex.
FDG PET scan of a representative patient with AD. From left to right: axial sections showing reduced tracer uptake in inferior pariet al lobules, bilaterally, where a slight asymmetry is noticeable superior temporal gyri, bilaterally, with the left hemisphere being more affected than the right bilateral medial temporal lobes and inferior temporal cortex and a coronal section showing hypometabolism of the hippocampi.
The brain hypometabolism finding in PET scans of AD patients correlates with clinical symptoms of cognitive impairment,, as well as CSF markers of AD pathology such as concentrations of phosphorylated TAU protein and A.,
Read Also: Farts And Dementia
B Epidemiology Of Alzheimer Disease
Alzheimer disease is the most common type of dementia, representing 6070% of all patients with dementia. The prevalence increases with age from approximately 35% for those under 75, 1518% for those age 7584 years, and 45% for those older than 85 years . In the US alone, an estimated 5.2 million have AD in 2008 and this may increase to 13.2 million by 2050 . Sporadic AD represents 98% of all AD cases and is likely due to a complex interaction of environmental, vascular, and genetic risk factors .
The epidemiologic data for patients at risk for late onset AD are equally daunting. In the US alone, 25 million persons are over the age of 65 . Before developing AD, many patients may transition through amnestic MCI , or memory complaints with commensurate objective neuropsychological test deficits, but without appreciable impact in general cognition or daily independent function.
Diagnosing Alzheimers: Biomarker Tests
These are tests that look at what we call biomarkers. Biomarkers are biological chemicals or changes that are known to indicate disease. In this case we look for biomarkers of Alzheimers disease.
There are two main biomarker tests: the positron emission tomography or PET scan and the body fluids test .
Recommended Reading: Neurotransmitter Alzheimers
What Are The 7 Stages Of Lewy Body Dementia
WHAT ARE THE 7 STAGES OF DEMENTIA?
- Stage One: No Cognitive Decline.
- Stage Two: Very Mild Cognitive Decline.
- Stage Three: Mild Cognitive Decline.
- Stage Four: Moderate Cognitive Decline.
- Stage Five: Moderately Severe Cognitive Decline.
- Stage Six: Severe Cognitive Decline.
- Stage Seven: Very Severe Cognitive Decline.
Pet Scans Improve Management Of Patients With Dementia
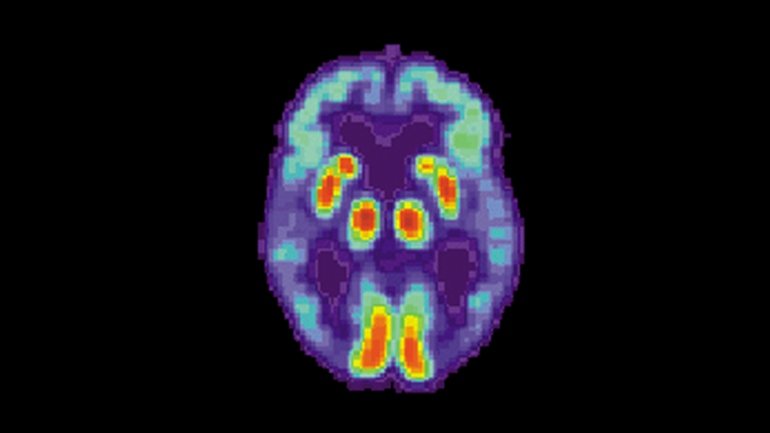
A national study has found that positron emission tomography , a form of brain imaging that detects Alzheimer’s-related “plaques,” significantly influenced clinical management of patients with mild cognitive impairment and dementia. The results of the study were recently published in JAMA.
The research team, which is part of the IDEAS study, enrolled a total of 16,000 Medicare beneficiaries. For this initial phase, the primary endpoint was how physicians altered participant’s medication prescriptions and counseling about safety and future planning. The researchers found that in MCI patients with significant amyloid deposits, physicians were twice as likely to prescribe Alzheimer’s drugs after positive PET imaging. In those with dementia, prescriptions rose from 63% pre-PET to 91% following positive amyloid imaging. A number of patients with MCI and dementia and negative amyloid imaging were taken off Alzheimer’s medications. This indicates an improvement in appropriate drug prescribing for Alzheimer’s patients.
For the secondary endpoint the scientists determined if PET imaging results caused physicians to change the patient’s diagnosis. The authors found that diagnoses changed from Alzheimer’s disease to non-Alzheimer’s in 25% of patients, and from non-Alzheimer’s to Alzheimer’s in 11% of participants. And based on imaging results, physicians were able to ensure that 93% of patients referred to Alzheimer’s trials were amyloid-positive.
Recommended Reading: What Color Ribbon Is Alzheimer’s
Q: What Are The Next Steps Of The Ideas Study
Right now were analyzing data for the second main question of the study, which is: Does the scan cut down on health care utilization? The idea here is that if somebody has an early warning from the PET scan, then can they can start planning changes in their living arrangements and behavior or somebody could monitor them more carefully. This may ultimately reduce hospitalizations and visits to the emergency room. A lot of hospitalizations and other health care utilization for dementia patients come about because they stop being able to take care of themselves people who are diabetic forget to check their blood sugar or to take heart medications, for example.
So we linked the data on people in the IDEAS study with their Medicare claims data. We now know how many times they visited the hospital and other health care utilization patterns for the year after the scan. We also went into the Medicare database and found matched controls for the participants in the study people in the same area as the original participants with similar characteristics, but who did not receive a PET scan. Were seeing if the IDEAS participants who had the amyloid PET scan had different amounts of health care utilization compared to similar Medicare beneficiaries who did not have the scan.
Q: What Are Amyloid Plaques And How Does This Method Detect Them
Amyloid plaques are deposits of protein clumps in the brain. Previous studies have shown that amyloid plaques are predictive of Alzheimers disease. However, there is controversy about whether the amyloid plaque formation causes Alzheimers. The amyloid plaque hypothesis was the basis for designing studies of drugs that attack the amyloid plaque. As of today, these drugs have failed to change patient outcomes, which calls into question the hypothesis of amyloid plaques being the causal agent. However, there is no question that amyloid plaques are predictive of Alzheimers.
In general, a PET scan is a nuclear scan. The patient is injected with an agent marked with a radioactive substance that binds to the target of interest. The three agents we used in the study show a pattern when the amyloid plaque is there. Because PET scans are somewhat fuzzy, PET is combined with a CT so you do the PET at the same time you take an x-ray computed tomography scan of the brain so you know where everything is. Previous studies have shown if this test is positive, you have an 80 to 90 percent chance of eventually getting Alzheimers.
Read Also: What Color Ribbon Is Alzheimer’s
Appropriate Use Criteria For Brain Amyloid Imaging With Pet In Ad
Criteria for appropriate clinical use are needed to avoid potential patient harm if the amyloid imaging scans are performed in inappropriate circumstances or are poorly read or if the significance of the results is not correctly applied to the clinical context.
The Society of Nuclear Medicine and Molecular Imaging and the Alzheimers Association Amyloid Imaging Taskforce have jointly developed consensus recommendations for the appropriate use of brain amyloid imaging to aid in the diagnosis of people with suspected AD. The Amyloid Imaging Taskforce concluded that amyloid imaging could potentially be helpful in the diagnosis of cognitive impairment when considered along with other clinical information and when performed according to standardized protocols by trained staff. The appropriate use of amyloid PET requires a fully comprehensive evaluation of patients undertaken by a clinician with expertise in evaluating cognitive neurodegenerative disorders.
Normal Cerebral Glucose Metabolism With Aging
Cerebral glucose metabolism patterns are similar among individuals who are age matched. The mean cerebral glucose metabolism has been found to gradually decrease with age. A study by Kuhl et al evaluating the effects of aging on the cerebral glucose metabolism of 40 normal subjects showed that the average cerebral glucose metabolic rate at age 78 years was 26% less than at age 18 years. Within the brain, the anatomical regions that show the greatest decrease in FDG uptake with aging are the bilateral superior medial frontal, motor, anterior, and middle cingulate and bilateral parietal cortices. The superior temporal pole was found to be particularly affected. The regions that show the least changes in glucose metabolism with aging are the bilateral medial temporal lobes, putamen, pallidum, lateral thalamic nuclei, right posterior cingulate cortex, precuneus, and both sides of the occipitotemporal cortex.
Don’t Miss: What Color Ribbon Is Alzheimer’s
Fdg Pet Imaging In Ftld
FDG PET studies in FTLD demonstrate the presence of metabolic impairment mainly involving frontal and anterior temporal lobes,, with milder hypometabolism of the pariet al lobes, which become more evidentas the disease advances. This pattern of predominantly frontal hypometabolism facilitates the differential diagnosis between AD and FTLD, although with some overlap, since frontal regions can be affected in AD and temporopariet al cortex in FTLD .,
Specific patterns of metabolic impairment have been associated with different subtypes of FTLD . bvFTD patients show hypometabolism of frontal lobe regions on FDG PET, specifically involving orbitofrontal, frontopolar, medial frontal, dorsolateral, and lateral inferior frontal regions, and anterior cingulate cortices., Metabolic impairments spread to temporal cortex and subcortical regions in more advanced stages of bvFTD.
FDG PET in different forms of FTLD, showing three representative cases with bvFTD , PNFA , and SD .
Patients with SD show hypometabolism of the temporal lobes, involving particularly the anterior portion ., Metabolic reductions in SD may also involve frontal midline structures, such as gyrus rectus, cingulate, orbitofrontal, and anterior medial cortices, as well as caudate nucleus, insula, and hippocampus.
B Using A Likelihood Ratio Mnemonic
Should a likelihood ratio table not be immediately available, and if one chooses not to pursue the potentially difficult calculation steps outlined below, a simpler way has been suggested, requiring the user to remember a few numbers . Positive likelihood ratios 2, 5, and 10, approximately increase the posttest probability by 15% increments individually. That is, a likelihood ratio positive of 2 increases the posttest probability by an absolute difference of 15%, 5 by 30%, and 10 by 45%. Conversely, a likelihood ratio negative of 1/2 decreases the posttest probability by an absolute difference of 15%, 1/5 by 30%, and 1/10 by 45%. Using this method considering one of the examples above, a likelihood ratio positive of 6.1 is similar to 5, which would increase a pretest probability of 50% absolutely by 30% to 80%. Similarly, a likelihood ratio negative of 0.08 is similar to 1/10 which would decrease a pretest probability of 50% absolutely by 45%, yielding a posttest probability of 5%, as estimated by the likelihood ratio tables. Overall, comparing this simplified methodology to the results above using the likelihood ratio tables, yields similar but less precise results.
Recommended Reading: Does Prevagen Help With Dementia
How Alzheimers Is Diagnosed By A Doctor
At one time, an Alzheimers diagnosis was only able to be confirmed after a person had passed away and doctors were able to perform an autopsy on the brain. Today, however, a physician can diagnose the disease with 90% accuracy while the person is still living.
It is important to note that there is no single test that can diagnose Alzheimers or dementia.
A medical evaluation will often include the following: