The Effects Of Alzheimer’s On The Brain
Heather Mercer is native to Northwest Ohio and graduated from Loma Linda University with two doctorate degrees . She is currently a professor at Owens Community College, as well as a fact-checker for Verywell Health. She has gained experience in a variety of settings, ranging from corporate wellness and preventive medicine, to mental health, chronic disease, and end-of-life care.
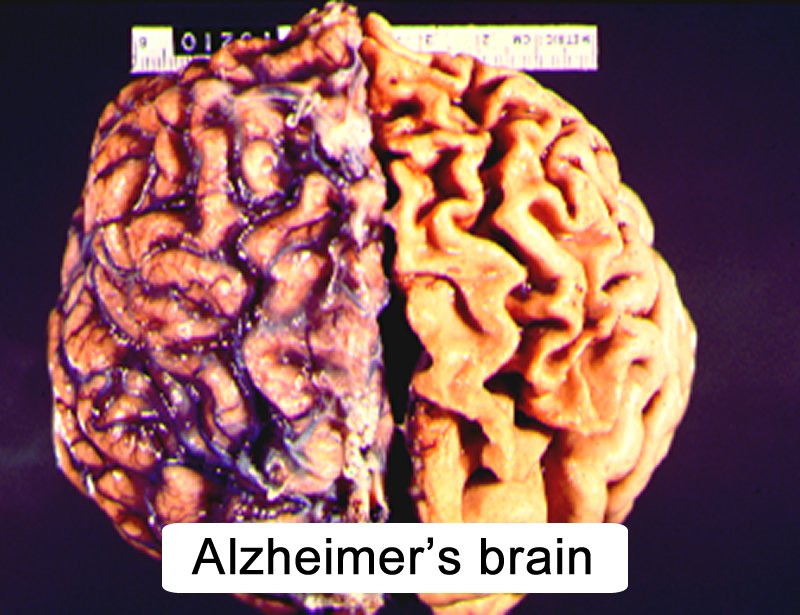
Alzheimer’s disease is a degenerative disease of the brain. Understanding how the anatomy of the Alzheimer’s brain differs from a normal brain gives us insight. It can help us cope better with the changes that happen to our loved ones as a result of this debilitating disease.
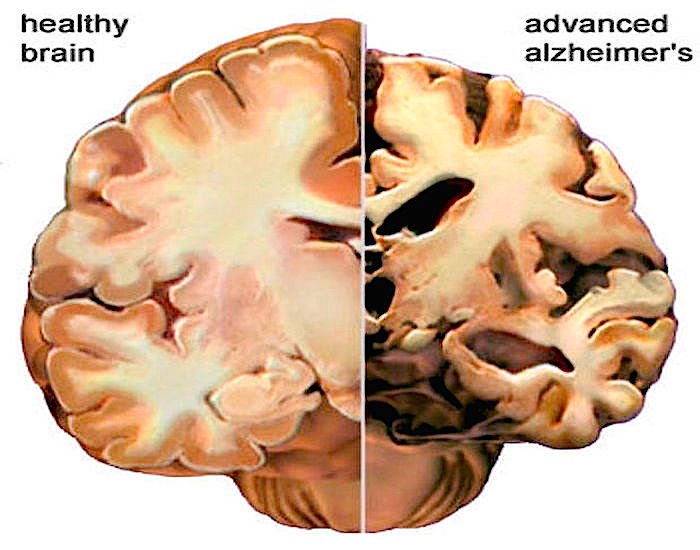
In Alzheimer’s disease, the appearance of the Alzheimer’s affected brain is very different to a normal brain. The cerebral cortex atrophies. That means that this area of the brain shrinks and this shrinkage is dramatically different from the cerebral cortex of a normal brain. The cerebral cortex is the outer surface of the brain. It is responsible for all intellectual functioning. There are two major changes that can be observed in the brain using magnetic resonance imaging :
- The amount of brain substance in the folds of the brain is decreased
- The spaces in the folds of the brain are grossly enlarged.
Alternatives To A Head Ct Scan
Head CT scans may be the most effective way to diagnose Alzheimers disease. But if you prefer another method, magnetic resonance imaging of the head shows your doctor if you have mild cognitive impairment or brain shrinkage. Cognitive tests are available online to download, print and bring to a doctors office for a score. One option is the SAGE test from the Ohio State University Wexner Medical Center.
To get the most accurate diagnosis, your doctor may recommend combining tests and scans. For example, you can have a head MRI along with an assessment by your primary care doctor.
Facing the idea that you or a loved one might have Alzheimers disease is difficult. Its important though to not delay important imaging scans. Learn more about how CT scans help you and how to prepare for an upcoming appointment.
Key Points About Early
-
Alzheimer disease commonly affects older people, but early-onset Alzheimer disease can affect people in their 30s or 40s.
-
It affects memory, thinking, and behavior.
-
Although there is no known cure, early diagnosis and treatment can lead to better quality of life.
-
Stay healthy with a good diet and regular exercise.
-
Avoid alcohol and other substances that may affect memory, thinking, and behavior.
Read Also: Alzheimers Awareness Symbol
How Does Alzheimers Disease Affect The Brain
The brain typically shrinks to some degree in healthy aging but, surprisingly, does not lose neurons in large numbers. In Alzheimers disease, however, damage is widespread, as many neurons stop functioning, lose connections with other neurons, and die. Alzheimers disrupts processes vital to neurons and their networks, including communication, metabolism, and repair.
At first, Alzheimers disease typically destroys neurons and their connections in parts of the brain involved in memory, including the entorhinal cortex and hippocampus. It later affects areas in the cerebral cortex responsible for language, reasoning, and social behavior. Eventually, many other areas of the brain are damaged. Over time, a person with Alzheimers gradually loses his or her ability to live and function independently. Ultimately, the disease is fatal.
Early Warning Signs And Diagnosis
Alzheimers Disease can be caught in the early stageswhen the best treatments are availableby watching for telltale warning signs. If you recognize the warning signs in yourself or a loved one, make an appointment to see your physician right away. Brain imaging technology can diagnose Alzheimers early, improving the opportunities for symptom management.
Recommended Reading: Bob Knight Health
Consolidated Results And Study Design
There were increased markers of oxidative stress in the cortex and cerebellum of COVID-19 tissue. Kynurenic acid, a marker of inflammation, was increased in COVID-19 cortex and cerebellum brain lysates compared to controls, is in accordance with recent studies showing a positive correlation between kynurenic acid and cytokines and chemokine levels in COVID-19 patients.-
To determine whether SARS-CoV-2 infection also increases tissue TGF-β activity, we measured SMAD3 phosphorylation, a downstream signal of TGF-β, in control and COVID-19 tissue lysates. Phosphorylated SMAD3 levels were increased in COVID-19 cortex and cerebellum brain lysates compared to controls, indicating that SARS-CoV-2 infection increased TGF-β signaling in these tissues. Interestingly, brain tissues from COVID-19 patients exhibited activation of the TGF-β pathway, despite the absence of the detectable virus in these tissues. These results suggest that the TGF-β pathway is activated systemically by SARS-CoV-2, resulting in its upregulation in the brain, as well as other organs. In addition to oxidative stress, COVID-19 brain tissues also demonstrated increased PKA and calmodulin-dependent protein kinase II association domain activity, most likely associated with increased adrenergic stimulation. Both PKA and CaMKII phosphorylation of tau have been reported in tauopathies.,
Functional Signs Of Dementia
Functional imaging of the brain can include a functional MRI, a positron emission tomography , or a single photon emission computed tomography scan. This kind of imaging serves as a complement to structural imaging, focusing on the underlying brain chemistry and activity rather than its physical composition.
SPECT and PET are similar kinds of scans, and in most cases of degenerative dementia, can showcase bilateral, biparietal, and bitemporal hyperperfusion. Some ligand compounds can reveal the impaired integrity of presynaptic dopamine transporters, present both in degenerative dementias and Parkinson’s disease.
The external signs of dementia can often be mistaken for those of another condition, but neural imaging can analyze the internal signs of the disease and help draw a firmer conclusion about a patient’s specific condition, and the progression of that condition.
0662
Also Check: Where Does Bobby Knight Live
Key Biological Processes In The Brain
Most neurons have three basic parts: a cell body, multiple dendrites, and an axon.
- The cell body contains the nucleus, which houses the genetic blueprint that directs and regulates the cells activities.
- Dendrites are branch-like structures that extend from the cell body and collect information from other neurons.
- The axon is a cable-like structure at the end of the cell body opposite the dendrites and transmits messages to other neurons.
The function and survival of neurons depend on several key biological processes:
Neurons are a major player in the central nervous system, but other cell types are also key to healthy brain function. In fact, glial cells are by far the most numerous cells in the brain, outnumbering neurons by about 10 to 1. These cells, which come in various formssuch as microglia, astrocytes, and oligodendrocytessurround and support the function and healthy of neurons. For example, microglia protect neurons from physical and chemical damage and are responsible for clearing foreign substances and cellular debris from the brain. To carry out these functions, glial cells often collaborate with blood vessels in the brain. Together, glial and blood vessel cells regulate the delicate balance within the brain to ensure that it functions at its best.
Brain Scans Spot Alzheimers Changes Years Before Symptoms
Study: People With Brain Shrinkage in Key Areas Are More Likely to Develop Memory Loss, Other Alzheimerâs Symptoms
Dec. 21, 2011 — Researchers say they can see telltale brain shrinkage years before a person develops memory loss or other symptoms of Alzheimerâs disease.
The new finding may one day allow doctors to detect and treat patients earlier and perhaps keep them functional for longer.
Researchers at Massachusetts General Hospital and the University of Pennsylvania used magnetic resonance imaging scans to measure the thickness of the brainâs outer layer in 159 people who were free of memory problems.
Previous studies have linked Alzheimerâs disease with characteristic shrinkage in nine different regions of the brainâs gray matter, or cerebral cortex. Doctors call this the âAlzheimerâs signature.â
Researchers say the brain shrinks as it loses nerve cells, or neurons. They arenât entirely sure what causes the nerve cells to die. One theory is that the cells die after they become choked by excess amounts of two kinds of protein — beta amyloid and tau.
âThe neurons degenerating over time are really what we think causes the shrinkage,â says researcher Brad Dickerson, MD, an associate professor of neurology at Harvard Medical School and director of the frontotemporal disorders unit at Massachusetts General Hospital. âAnd that shrinkage in their size is something you can measure with an MRI scan.â
Read Also: Bobby Knight Dementia
Dementia Symptoms And Areas Of The Brain
Knowing how different types of dementia affect the brain helps explain why someone with dementia might behave in a certain way.
Dementia and the brain
Until recently, seeing changes in the brain relied on studying the brain after the person had died. But modern brain scans may show areas of reduced activity or loss of brain tissue while the person is alive. Doctors can study these brain scans while also looking at the symptoms that the person is experiencing.
The most common types of dementia each start with shrinkage of brain tissue that may be restricted to certain parts of the brain.
What Happens To The Brain In Alzheimer’s Disease
The healthy human brain contains tens of billions of neuronsspecialized cells that process and transmit information via electrical and chemical signals. They send messages between different parts of the brain, and from the brain to the muscles and organs of the body. Alzheimers disease disrupts this communication among neurons, resulting in loss of function and cell death.
Also Check: Bob Knight Alzheimer’s
Stage : Normal Outward Behavior
Alzheimerâs disease usually starts silently, with brain changes that begin years before anyone notices a problem. When your loved one is in this early phase, they won’t have any symptoms that you can spot. Only a PET scan, an imaging test that shows how the brain is working, can reveal whether they have Alzheimer’s.
As they move into the next six stages, your friend or relative with Alzheimer’s will see more and more changes in their thinking and reasoning.
What To Do If You’re Concerned
Remember that these visual signs are only one aspect of the person, and they may be related to other conditions. Additionally, some people with dementia initially demonstrate very few of these visual clues, causing much surprise when they’re diagnosed with dementia because “they look so healthy.”
If you’re worried that someone has dementia, review these 10 warning signs of dementia and make an appointment with the physician for an evaluation. While this may be an anxiety-provoking step to take, a doctor’s assessment can also help by identifying reversible causes of confusion or by identifying dementia and beginning treatment as early as possible.
Recommended Reading: Dementia Awareness Ribbon Color
What Does It Mean When What Looks Like Alzheimers Isnt Alzheimers
Shutterstock
For a definitive Alzheimers diagnosis, doctors still need to see the neuropathological changes neurofibrillary tau tangles and beta-amyloid plaques in the brains of patients after biopsy or autopsy. But in recent years, one pathology finding has left doctors and researchers puzzled: The brains of some patients who had clearly had dementia, and showed the symptoms associated with Alzheimers disease, were clear of the tell-tale signs of the disease. Instead of tangles and amyloid plaques, jumbled messes of another protein, TDP-43, crowded their brains. In a consensus paper published in spring 2019, a group of researchers named this phenomenon limbic-predominant age-related TDP-43 encephalopathy , describing it as a distinct disease that mimics some features of Alzheimers.
What does it mean when what looks like Alzheimers isnt, in fact, Alzheimers?
Dementia More Complex than Previously Thought
This paper is part of an evolving appreciation of the complexities that underlie dementia, says Peter Nelson, professor at the Sanders-Brown Center on Aging at the University of Kentucky and first author of the consensus paper.
New Name, New Interest
What Does it Mean for Dementia Research?
Structural Signs Of Dementia
Structural imaging of the brain consists of computed tomography and the popularly known magnetic resonance imaging scans. This kind of imaging focuses on the morphology as well as the structural details of the brain’s composition. It is a very physical kind of scan, searching for solid, visible signs of degeneration or abnormalities.
Degenerative dementia causes a number of visible physical signs in the brain in some patients, but is not always easy to detect. CT scans can usually observe some atrophy of the brain’s medial temporal lobe, but the CT scans’ lack of sensitivity can occasionally be problematic. MRI scans, of much higher resolution, can capture atrophy of the hippocampus in nearly 90 percent of all cases of Alzheimer’s disease.
Read Also: Ribbon For Alzheimer’s
Vascular Contributions To Alzheimers Disease
People with dementia seldom have only Alzheimers-related changes in their brains. Any number of vascular issuesproblems that affect blood vessels, such as beta-amyloid deposits in brain arteries, atherosclerosis , and mini-strokesmay also be at play.
Vascular problems may lead to reduced blood flow and oxygen to the brain, as well as a breakdown of the blood-brain barrier, which usually protects the brain from harmful agents while allowing in glucose and other necessary factors. In a person with Alzheimers, a faulty blood-brain barrier prevents glucose from reaching the brain and prevents the clearing away of toxic beta-amyloid and tau proteins. This results in inflammation, which adds to vascular problems in the brain. Because it appears that Alzheimers is both a cause and consequence of vascular problems in the brain, researchers are seeking interventions to disrupt this complicated and destructive cycle.
The Dementia Brain Tour
The brain is incredibly complex and this section of our site contains a lot of information about how the brain is thought to function. For more about how the brain works and the effects of dementia, see our set of videos below.
Think this page could be useful to someone? Share it:
- Page last reviewed:
You May Like: What’s The Difference Between Dementia And Alzheimer’s And Senility
Neuroimaging: Visualising The Brain
Neuroimaging describes a range of tools which are used to visualise the living brain, including computerised tomography scans, magnetic resonance imaging , single photon emission computerised tomography and positron emission tomography .
Researchers are working on new ways of using neuroimaging tools to diagnose Alzheimer’s disease and other types of dementia.
Positron Emission Tomography
In 2004, researchers successfully viewed beta-amyloid plaque deposits in the living human brain. The study used Pittsburgh Compound-B , a substance which binds to amyloid and can be visualised with PET scanning. The results demonstrated that people with Alzheimer’s disease displayed more amyloid deposits in certain brain areas compared to people without the condition. More recent research has shown that PiB-PET can also detect the early brain changes of Alzheimer’s disease before symptoms become apparent.
While PiB has proved quite effective, its widespread clinical use may be limited by the need for specialised equipment to produce PiB at the site of the PET scanner. Researchers are currently developing and testing other compounds that bind to beta-amyloid and may overcome the limitations of PiB.
Magnetic Resonance Imaging
MRI is able to image the structure of the brain, which changes in dementia, to a very high resolution.
Tangles And Cell Death
In normal brain tissue, a protein called tau stabilizes microtubules. Microtubules are key parts of cell structure.
In a diseased brain, protein strands, or threads, become tangled. As a result, the brain system of transporting cell nutrients along parallel structures which can be compared to railroad tracks falls apart.
Without these critical nutrients, brain cells die.
Memory and thinking depend on the transmission of signals across 100 billion neurons in the brain.
AD interferes with this cell signal transmission. It also affects the activity of brain chemicals called neurotransmitters.
The scrambled chemistry produces flawed signaling, so the brains messages are lost. This impacts the ability to learn, remember, and communicate.
Microglia are a type of cell that initiate immune responses in the brain and spinal cord. When AD is present, microglia interpret the beta-amyloid plaque as cell injury.
The microglia go into overdrive, stimulating inflammation that further damages brain cells.
Some AD research focuses on how this inflammatory response can be reduced or controlled.
You May Like: How Long Does A Person Live After Being Diagnosed With Alzheimer’s
Can Mri Diagnose Dementia
Can MRI Diagnose Dementia?
Can MRI diagnose dementia? The answer is complicated. It can definitely help in the diagnosis.
In Radiology, patients pose this question often. Can MRI show if I have dementia? In fact, we scan patients every day with a diagnosis of dementia, memory loss, Alzheimers, and confusion, among a variety of other neurological disorders.
The truth is that MRI is NOT the test to formally diagnose dementia. But to understand how MRI fits into the diagnosis process of a patient with suspected dementia, one must first understand how dementia is defined.
Dementia is a general term for neurocognitive deficiencies that impair or interfere with living a normal life due to memory deficits, decision making issues, or difficulty thinking clearly. Alzheimers disease is the most common and well known rendition of dementia, but there are other forms of the disease as well.
As we age, the capacity to remember, think sharply, or complete tasks independently inherently decreases. In fact, one could argue that we all show signs of dementia as we enter our golden years. This process is natural and considered a normal part of aging.
The term dementia starts to bubble up when an individual exhibits neurological deficits that cause them to stand out from their peers. This is usually noticed by people who know the individual best and can judge their cognitive decline, and see how it affects their daily lives.
Normal Pressure Hydrocephalus
Stroke
Stages Of Alzheimers Disease
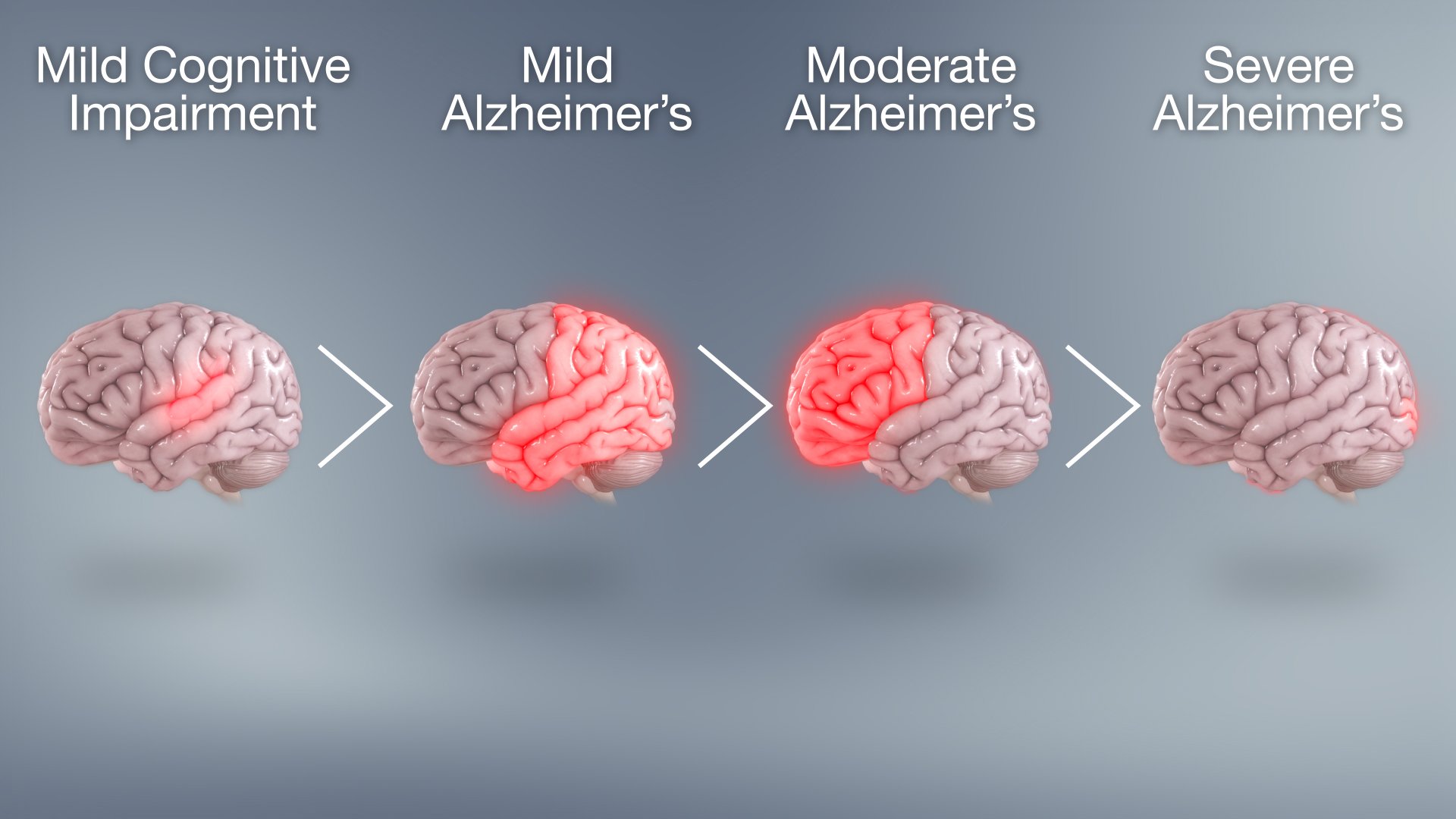
These stages include:
1. Early Stage Alzheimers
The earliest stages of Alzheimers may begin 20 years or more before diagnosis. At this point, plaques and tangles begin to form in parts of the brain that impact learning, memory, planning and thinking. Medical tests cannot yet detect Alzheimers in its earliest stages.
2. Mild to Moderate Alzheimers
As Alzheimers progresses to moderate stages, more plaques and tangles develop in areas of the brain important to memory, planning and thinking, and spread to areas that affect speech. These changes cause noticeable confusion and communication problems that can impact an individuals personal or work life. Often, Alzheimers is diagnosed in this stage.
Mild to moderate Alzheimers stages can last from two to 10 years. During this time period, individuals may struggle to recognize family members and friends. They may also experience behavior and personality changes.
3. Late Stage Alzheimers
The most severe stage of Alzheimers can last from one to five years. Most of the brains outer layer, which scientists have mapped to memory, movement, thinking and other functions, has been permanently damaged.
Widespread cell death causes the brain to shrink. At this point, individuals no longer recognize family and friends. They also lose their ability to care for themselves and communicate.
Don’t Miss: Alzheimer’s And Neurotransmitters