How Is Dementia Treated
While there is no cure for some dementias, the progression of some types of dementia can be slowed or even reversed with treatment. Options include:
- Treating the cause of dementia when there is a treatable cause: This includes hormonal treatment for hypothyroidism, treating hydrocephalus with shunting, evacuation of subdural collections, etc.
- Cholinesterase inhibitors, a type of medication that may slow the progress of Alzheimer’s disease by helping people improve their attention and working memory.
- Medications to manage blood pressure, cholesterol, triglycerides, diabetes, and problems with blood clotting.
- Procedures to improve blood flow to the brain, such as carotid endarterectomy or Angioplasty and Vascular Stenting.
- Lifestyle modifications, such as following a healthy diet and adding an exercise regimen, quitting smoking and quitting or decreasing alcohol consumption.
The Lumbar Puncture Myth Buster
As published in Dimensions
Dr. Elaine Peskind, UW Professor of Psychiatry and former director of the UW ADRC Clinical Core, reinvented the way research lumbar punctures, or spinal taps, are done, making them safer and less painful for research participants. But urban legends and myths of pain, meningitis, and paralysis are still associated with the procedure. Dr. Peskind, who has performed more than a thousand lumbar punctures during her work at the ADRC, takes a look at a handful of these fables and reveals the truth about research lumbar punctures.
MYTH: Lumbar punctures are really painful.
The discomfort associated with a lumbar puncture seems to vary from person to person. Most people report that the only painful or uncomfortable part of the procedure is a very brief sting they experience when the local anesthetic or numbing medicine is injected. This local anesthetic is similar to the one you would receive at the dentist, and it is used to prevent pain during the lumbar puncture. As the needle for the lumbar puncture is positioned to collect spinal fluid, most people describe the feeling as a pressure sensation. In a study we did at the ADRC, we found that, overall, anxiety and pain ratings were low among the research participants who had lumbar punctures. Most people are surprised at how comfortable the procedure is, and occasionally a person will sleep through the procedure.
MYTH: If a person gets a lumbar puncture, that person will have a bad headache afterwards.
Why Early Detection Can Be Difficult
Alzheimers disease usually is not diagnosed in the early stages, even in people who visit their primary care doctors with memory complaints.
- People and their families generally underreport the symptoms.
- They may confuse them with normal signs of aging.
- The symptoms may emerge so gradually that the person affected doesnt recognize them.
- The person may be aware of some symptoms but go to great lengths to conceal them.
Recognizing symptoms early is crucial because medication to control symptoms is most effective in the early stages of the disease and early diagnosis allows the individual and his or her family members to plan for the future. If you or a loved one is experiencing any of the following symptoms, contact a physician.
Read Also: Alzheimer Ribbon Color
Are There Side Effects From Lumbar Punctures
Lumbar punctures are a standard medical procedure used for a wide range of medical purposes. It is not common to experience side effects after a well-conducted lumbar puncture. When there are side effects, these are generally limited to headaches that can last for several days. Despite this, there are some common myths and misconceptions about the procedure that prevent some people from having one done.
Volume In Brain Region Linked To Physiological Changes Characteristic Of Ad
New research has drawn a link between changes in the brains anatomy and biomarkers that are known to appear at the earliest stages of Alzheimers disease , findings that could one day provide a sensitive but non-invasive test for AD before cognitive symptoms appear.
Scientists have known for some time that one of the first signs of AD is buildup of amyloid-Beta and tau proteins in the brain. They have also known that the hippocampus atrophies and loses volume in some AD patients years before cognitive decline.
To examine the link between the two, a team of researchers from McGill University and McGill-affiliated health institutes followed 88 individuals at hereditary risk of AD, but who did not show any cognitive signs of the disease. Subjects were scanned using magnetic resonance imaging to determine brain volume and had cerebrospinal fluid extracted to test levels of amyloid-Beta and tau. These data were collected by the Centre for Studies on the Prevention of Alzheimers Disease group at the Douglas Mental Health University Institute under the leadership of Dr. John Breitner.
Biomarkers can be used to test the effectiveness of drugs in clinical trials
Their work was published in the journal Human Brain Mapping on Nov. 21, 2017. It was funded with generous support from the StoP-AD Centre.
Recommended Reading: Does Ben Carson Have Dementia
Detecting Alzheimers Gets Easier With A Simple Blood Test
New assays could reduce the need for costlier, more invasive brain scans and spinal fluid measures
When a patient complains of forgetfulness, a neurologist might not know immediately whether it results from normal aging, reduced blood flow to the brainor, more ominously, Alzheimers disease. For much of the past century, a definitive Alzheimers diagnosis could only be made during an autopsy. Brain imaging and spinal fluid tests now make it possible to spot the disease in patients even before the initial symptoms appear. But these invasive tests are expensive and generally limited to research settings that are not part of routine care for the millions of people suffering from the most common neurodegenerative disorder.
An era in which an Alzheimers diagnosis can begin in a doctors office is now arriving. Advances in technologies to detect early signs of disease from a blood sample are helping doctors to identify the memory-robbing disorder more accurately and to screen participants more quickly for trials of potential treatments for the more than five million people in the U.S. afflicted with Alzheimers.
The development of a blood-based test for Alzheimers disease is just phenomenal, says Michelle Mielke, a neuroscientist and epidemiologist at the Mayo Clinic. The field has been thinking about this for a very long time. Its really been in the last couple of years that the possibility has come to fruition.
Spinal Fluid Biomarkers Detect Neurodegeneration Alzheimer’s Disease In Living Patients
- Date:
- University of Pennsylvania School of Medicine
- Summary:
- Alzheimer’s disease and other forms of neurodegeneration can be identified using a combination of biomarkers in cerebrospinal fluid of living patients, researchers find.
Alzheimer’s disease and related diseases can still only be confirmed in deceased patients’ brains via autopsy. Even so, the development of biomarkers can give patients and their families answers during life: Alzheimer’s disease can be accurately detected via peptides and proteins in a patient’s cerebrospinal fluids , which can be collected through a lumbar puncture and tested while the patient is alive. In 2018, a new framework suggested combining three Alzheimer’s disease biomarkers in CSF — pathologic amyloid plaques , tangles , and neurodegeneration , collectively called ATN. According to recent research from the Perelman School of Medicine at the University of Pennsylvania, the ATN framework can be extended to detect another neurodegenerative condition: frontotemporal degeneration.
This study was funded by the Swedish Research Council the European Research Council, Swedish State Support for Clinical Research the Alzheimer Drug Discovery Foundation the Swedish Alzheimer Foundation, European Union Joint Program for Neurodegenerative Disorders and the Alzheimer’s Association Research Fellowship .
Explore the latest scientific research on sleep and dreams in this free online course from New Scientistâ
Story Source:
Also Check: Can Dementia Turn Into Alzheimer’s
Lumbar Punctures Can Improve The Prediction Of Alzheimer’s Disease
Measuring the concentration of proteins in cerebrospinal fluid is a promising technique to improve dementia care and quality of life in dementia patients. However, this technique is not widely applied in practice. Researchers at Maastricht UMC+ and the Alzheimer Centre Limburg conducted a study to determine whether the standard application of protein tests would benefit patients. The researchers recently published their findings in the Journal of Alzheimer’s Disease.
Alzheimer’s disease is characterised by the formation of so-called amyloid plaques in the brain. These protein accumulations disrupt brain functions and can lead to memory problems and dementia. While memory problems are often the first sign of Alzheimer’s disease, not everyone develops this symptom. Memory tests and a brain scan can be used to determine the risk of developing dementia. However, it is still relatively common for these tests to provide no definitive diagnosis. As a result, patients are unsure of where they stand, which can impact quality of life.
What Is Alzheimer’s Disease
Alzheimers disease, which is the most common form of dementia, is still today an incurable degenerative disease. Neurons in certain parts of the brain are destroyed which leads to deficits in cognitive functions, such as memory, language skills, and behavior. Clinical diagnosis can be supported by biomarkers that detect the presence or absence of the disease. This will become even more important in the future, when new treatments of Alzheimers disease will become available.
Recommended Reading: Does Coke Cause Alzheimer’s
What Are The Benefits Of An Early Diagnosis Of Dementia
There are many benefits of an early dementia diagnosis. These include:
- After a series of testing and questions, your healthcare provider can give you an accurate diagnosis based on your symptoms.
- If dementia is diagnosed early enough, you can play an active role in the decision-making process for your future.
- You may be a candidate for clinical trials.
- You can focus on things that are most important in your life.
- If diagnosed early, you will have time to get your financial, legal, and medical matters in order.
- Allows time for you and your family to understand the challenges ahead and prepare for them.
Rating Of Clinical Indications
Using the evidence summary, their clinical experience and expertise, as well as their knowledge of research outside of the scope of the evidence review, the workgroup employed a three-step, modified Delphi approach to reach consensus ratings for each of the clinical indications. Workgroup members were asked to assess the benefits and risks to patients of using LP and CSF in diagnosis in rating each indication. In each of the three rounds, members were asked to assign to each indication a rating within ranges of appropriate, uncertain, or inappropriate for use of LP for diagnosis of MCI or AD. A 9â1 rating scale was used in each of the three rounds of voting. The rating scale ranged from:
- 9 = Highly confident that the indication is appropriate
- 8 = Moderately confident that the indication is appropriate
- 7 = Only somewhat confident that the indication is appropriate
- 6 = Uncertain, but possibility that appropriate
- 5 = Uncertain
- 4 = Uncertain, but possibility that inappropriate
- 3 = Only somewhat confident that the indication is inappropriate
- 2 = Moderately confident that indication is inappropriate
- 1 = Highly confident that the indication is inappropriate
Recommended Reading: Alzheimer Vs Dementia Vs Senility
What If I Have Dementia How Is It Treated
Dementia is a progressive disease that has no cure. With proper treatment, some types of dementia can be slowed. There are different ways to help manage symptoms. These may include:
Routine Lumbar Puncture For The Early Diagnosis Of Alzheimer’s Disease Is It Safe
- 1Sección de Neurología, Hospital Álvarez-Buylla, Mieres, Spain
- 2Morfología y Biología Celular, Universidad de Oviedo, Oviedo, Spain
Diagnosing Alzheimer’s disease early is itself a controversial topicnot to be addressed here, as many believe that adequate therapeutics are not available for modifying the course of the disease. Although this may be the case today, it is perhaps due to the fact that existing therapies do not have positive results as the disease process is too far advanced. Distinguishing the cases who will progress to AD among individuals with mild cognitive impairment , would allow early administration of these currently and future available treatments. Together, this can prolong a meaningful life and also reduce the burden on caregivers as well as the cost of care, now that both the prevalence and cost of AD are rising at a rapid rate.
As a result, the use of LP for testing CSF biomarkers in the diagnosis of AD is surprisingly culturally dependent and subject to changes in fashion today. From clinicians who support its use in daily clinical practice and countries where lumbar punture is almost a routine to other territories where it is regarded as a very serious issue and used for research purposes under strict protocols only .
Recommended Reading: What Color Is Alzheimer’s Ribbon
Yes With Either A Lumbar Puncture Or Amyloid Pet Scan
This is the second post in a series on Alzheimers disease, the most common cause of memory loss and dementia. Part 1 discussed its pathology and stages.
In special circumstances a lumbar puncture can help to confirm Alzheimers disease.
Analyzing the levels of beta-amyloid and tau in the spinal fluid can help to confirm that Alzheimers is present when the disease is strongly suspected but there is something unusual, such as the individual being younger than age 65. Other things that may make the situation unusual would include early changes in movement or behavior. We dont use this test routinely both because it is not needed in the majority of individuals when the diagnosis is straightforward, and because the test provides the right answer about 85 to 90% of the time but can be inconclusive or misleading the other 10 to 15% of the time.
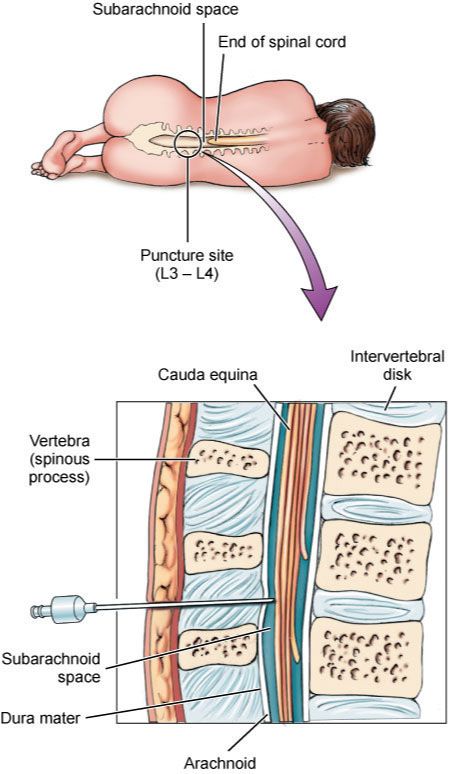
A lumbar puncturemore commonly known as a spinal tapmay sound frightening, but it is actually a very safe and simple test that is less painful for most people than having an IV placed. If your doctor suggests this test, your loved one would begin by either sitting or lying down on their side with their back to the doctor, and curling into a little ball by bringing their shoulders down and their knees up. The doctor would find the right spot, clean the area well, give them some numbing medicine , insert a very thin needle, and take a small amount of spinal fluid out.
LinkedIn Image Credit: David Pereiras/Shutterstock
References
Does Lumbar Puncture Cause Infections
There is a misconception that people can develop meningitis from a lumbar puncture. This myth may have come about because bacterial meningitis, where bacteria makes its way into the spinal canal, is diagnosed by using a lumbar puncture to collect spinal fluid for testing. There is virtually no risk of meningitis from a lumbar puncture.
Also Check: Alzheimer’s Paranoia Medication
Using Csf To Help Diagnose Dementia
An accurate diagnosis of dementia is important. It gives people the opportunity to access treatments, care and support that allows them to plan for the future while they are still able to make important decisions. It also enables people to take part in dementia research via initiatives like Join Dementia Research.
If you are worried about memory problems, the doctor will ask about your symptoms and medical history. They will ask you to do some memory and thinking tests. Other tests, like brain scans, blood tests and a lumbar puncture, may help the doctor to identify the cause of your symptoms.
There is no one diagnostic test or magic marker for the diseases that cause dementia. Putting the results of several different investigations together helps doctors to give an accurate diagnosis.
In June 2018, the guidelines for diagnosing dementia were updated by the National Institute for Health and Care Excellence to include assessment of CSF by lumbar puncture where appropriate.
In recent years, research has shown that CSF tests can be a valuable tool for the detection of hallmark proteins that are involved in diseases that cause dementia. For example, amyloid and tau protein build up in Alzheimers disease, and their levels can be measured in CSF.
Overview Of The Neuropathology Underlying Mci And Ad
At the microscopic level, the primary neuropathological features of AD include neuritic plaques and neuronal, especially synaptic, degeneration, together with other features, including cerebral amyloid angiopathy, neurofibrillary tangles, and neuropil threads , . Plaques are rounded lesions in the neuropil, primarily composed of aggregated β-amyloid . The form ending at position 42 is more prone to aggregation than shorter isoforms, of which Aβ40 is the most abundant , . Plaques exist as diffuse and neuritic plaques the latter variant consists of a central core of amyloid fibrils surrounded by dystrophic neurites , reactive astrocytes, and microglia . Tangles are detected in the neuronal cytoplasm, in the form of paired helical filaments, primarily composed of hyperphosphorylated tau protein . Intraneuronal accumulation of abnormally phosphorylated tau is believed to precede tangle formation in AD , with tau pathology spreading in a relatively consistent way from the brainstem to the transentorhinal region, hippocampal formation, and the neocortex , .
Don’t Miss: Does Prevagen Work For Dementia
A Better Test For Alzheimer’s
Along with colleagues from the Alzheimer’s Disease Neuroimaging Initiative, which paid for the research, Vanderstichele developed the protein profile and tested it on spinal fluid taken from roughly 100 older people with no evidence of memory loss, as well as 200 people with MCI and 100 with Alzheimer’s disease.
The researchers tested the samples without knowing the clinical status of the patients who supplied them.
The Alzheimer’s signature was identified in nine out of 10 samples from patients with Alzheimer’s disease and in just over two-thirds of patients with MCI. Thirty-six percent of people with no known cognitive impairment also exhibited the signature.
These results were validated in CSF samples from two other studies. In one, the protein signature indicative of Alzheimer’s was seen in 64 of 68 autopsy-confirmed cases of the disease. In another, all 57 patients with MCI followed for five years exhibited the protein profile.
It is not clear why more than a third of people without memory declines had the Alzheimer’s biomarkers. It could be that the biomarker changes occur long before symptoms of Alzheimer’s do, says neurologist John H. Growdon, MD, of Massachusetts General Hospital.
“These may be people who are able to tolerate a high burden of these toxic without developing symptoms,” he says.