How Do Ct Scans Show Dementia
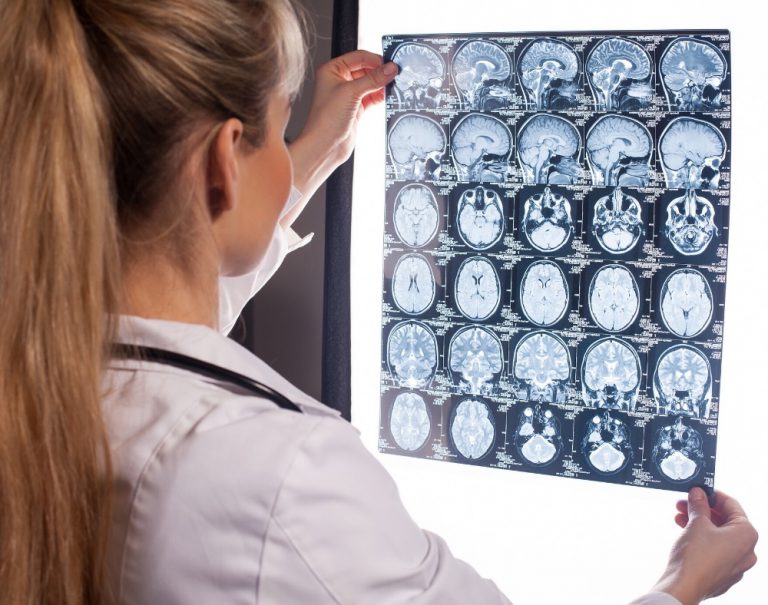
The most common types of brain scan you might encounter are magnetic resonance imaging and computed tomographic scans.
Doctors regularly recommend MRIs and CT scans when they examine someone they suspect has dementia.
CT scans detect brain structures through X-rays and the procedure can reveal evidence of ischemia, brain atrophy, and strokes.
The procedure also picks up on PROBLEMS like subdural hematomas, hydrocephalus, and changes that affect the blood vessels.
As implied, MRIs make use of focused radio waves and magnetic fields to detect the presence of hydrogen atoms within the bodys tissues.
MRIs ARE BETTER at diagnosing brain atrophy and the damage that subtle ischemia or incidents of small strokes cause to the brain.
Thus, MRI is normally the first test a person undergoes and CT second.
Ai Algorithm Can Accurately Predict Risk Diagnose Alzheimers Disease
Researchers have developed a computer algorithm based on Artificial Intelligence that can accurately predict the risk for and diagnose Alzheimers disease using a combination of brain magnetic resonance imaging , testing to measure cognitive impairment, along with data on age and gender.
The AI strategy, based on a deep learning algorithm, is a type of machine learning framework. Machine learning is an AI application that enables a computer to learn from data and improve from experience. Alzheimers disease is the primary cause of dementia worldwide. One in 10 people age 65 and older has Alzheimers dementia. It is the sixth-leading cause of death in the United States.
If computers can accurately detect debilitating conditions such as Alzheimers disease using readily available data such as a brain MRI scan, then such technologies have a wide-reaching potential, especially in resource-limited settings, explained corresponding author Vijaya B. Kolachalama, PhD, assistant professor of medicine. Not only can we accurately predict the risk of Alzheimers disease but this algorithm; can generate interpretable and intuitive visualizations of individual Alzheimers disease risk en route to accurate diagnosis, said Dr. Kolachalama.
The researchers believe their methodology can be extended to other organs in the body and develop predictive models to diagnose other degenerative diseases.
These findings appear online in the journal Brain.
Basics Of Fdg Pet As Applied To Ad
Brain FDG PET primarily indicates synaptic activity. Because the brain relies almost exclusively on glucose as its source of energy, the glucose analog FDG is a suitable indicator of brain metabolism and, when labeled with Fluorine-18 is conveniently detected with PET. The brains energy budget is overwhelmingly devoted to the maintenance of intrinsic, resting activity, which in cortex is largely maintained by glutamaturgic synaptic signaling . FDG uptake strongly correlates at autopsy with levels of the synaptic vesicle protein synaptophysin . Hence, FDG PET is widely accepted to be a valid biomarker of overall brain metabolism to which ionic gradient maintenance for synaptic activity is the principal contributor . In this context, a single, specific AD-related alteration in FDG metabolism has not been identified and therefore the FDG-PET abnormalities described below are assumed to be the net result of some combination of processes putatively involved in the pathogenesis of AD including, but not limited to, expression of specific genes, mitochondrial dysfunction, oxidative stress, deranged plasticity, excitotoxicity, glial activation and inflammation, synapse loss, and cell death.
Also Check: Does Alzheimer’s Run In Families
Utility Of Fdg Pet In The Study Of Ad
The Pattern of FDG Hypometabolism Is an Endophenotype of AD
A substantial body of work over many years has identified a FDG-PET endophenotype of AD that is, a characteristic or signature ensemble of limbic and association regions that are typically hypometabolic in clinically established AD patients . The anatomy of the AD signature includes posterior midline cortices of the parietal and posterior cingulate gyri, the inferior parietal lobule, posterolateral portions of the temporal lobe, as well as the hippocampus and medial temporal cortices. Metabolic deficits in AD gradually worsen throughout the course of the disease. Bilateral asymmetry is common at early stages, more advanced disease usually involves prefrontal association areas, and in due course even primary cortices may be affected. Interestingly, the regions initially hypometabolic in AD are anatomically and functionally interconnected and form part of the large-scale distributed brain network known as the default mode network . We now know in addition that these regions are highly vulnerable to amyloid- deposition .
FDG Hypometabolism Is Related to Other AD Biomarkers and to Genes
FDG PET Is a Valid AD Biomarker
Basics Of Structural Mri As Applied To Ad

MRI utilizes the fact that protons have angular momentum which is polarized in a magnetic field. This means that a pulse of radiofrequency can alter the energy state of protons and, when the pulse is turned off, the protons will, on returning to their energy stage, emit a radiofrequency signal. By a combination of different gradients and pulses, sequences can be designed to be sensitive to different tissue characteristics. In broad terms structural MRI in AD can be divided into assessing atrophy and changes in tissue characteristics which cause signal alterations on certain sequences such as white matter hyperintensities on T2-weighted MRI as a result of vascular damage. A number of MR sequences that are sensitive to microstructural change have shown alterations in AD. These sequences are already important research tools; however, they have not yet found a place in routine clinical practice in AD and they will not be considered further here.
You May Like: What Is The Difference Between Dementia And Senility
Signs You May Need A Scan
If you have a family history of Alzheimers or dementia, you may want to get tested proactively so that you can determine if you have this condition. In other situations, you may want to get tested if you have any of the following symptoms:
- Memory loss
- Issues with depth perception
- Delusions or hallucinations
Many people believe that some memory loss is inevitable with aging, but this is simply not true. If you or your loved one is experiencing chronic or progressive memory loss or memory loss combined with the above symptoms, it may be a sign of Alzheimers.
Mental Ability Tests To Diagnose Dementia
People with symptoms of dementia are given tests to check their mental abilities, such as memory or thinking.
These tests are known as cognitive assessments, and may be done initially by a GP.
There are several different tests. A common one used;by GPs is;the General Practitioner Assessment of Cognition .
Although;these tests cannot diagnose dementia,;they may show there are memory difficulties that need further investigation.
Most;tests involve a series of pen-and-paper tests and questions, each of which carries a score.
These tests assess a number of different mental abilities, including:
- short- and long-term memory
- language and communication skills
- awareness of time and place
It’s important to remember that test scores may be influenced by a person’s level of education.
For example, someone who cannot read or write very well may have a lower score, but they may not have dementia.
Similarly, someone with a higher level of education may achieve a higher score, but still have dementia.
You May Like: Does Meredith Grey Have Alzheimer’s
Utility Of Structural Mri In The Study Of Ad
Atrophy in AD
Progressive cerebral atrophy is a characteristic feature of neurodegeneration that can be visualized in life with MRI . The major contributors to atrophy are thought to be dendritic and neuronal losses. Studies of regional MRI volumes have shown these are closely related to neuronal counts at autopsy . The pattern of loss differs between diseases reflecting selective neuronal vulnerability and/or regional disease expression. AD is characterized by an insidious onset and inexorable progression of atrophy that is first manifest in the medial temporal lobe . The entorhinal cortex is typically the earliest site of atrophy, closely followed by the hippocampus, amygdala, and parahippocampus . Other structures within the limbic lobe such as the posterior cingulate are also affected early on. These losses then spread to involve the temporal neocortex and then all neocortical association areas usually in a symmetrical fashion. This sequence of progression of atrophy on MRI most closely fits histopathological studies that have derived stages for the spread of neurofibrillary tangles . Nonetheless, a significant minority of AD cases have atypical presentations and in these cases the pattern of atrophy accords with clinical phenotype: with language presentations particularly having left temporal atrophy and visual variants having posterior cortical atrophy.
Measuring Progression in AD with Structural MRI
Availability and Utility of Structural MRI
Limitations Of Fmri In Ad
There are multiple challenges in performing longitudinal fMRI studies in patients with neurodegenerative dementias. It is likely that fMRI will remain quite problematic in examining patients with more severe cognitive impairment, as these techniques are very sensitive to head motion. If the patients are not able to adequately perform the cognitive task, one of the major advantages of task fMRI activation studies is lost. Resting state fMRI may be more feasible in more severely impaired patients.
It is critical to complete further validation experiments. BOLD fMRI response is known to be variable across subjects, and very few studies examining the reproducibility of fMRI activation in older and cognitively impaired subjects have been published to date . Longitudinal functional imaging studies are needed to track the evolution of alterations in the fMRI activation pattern over the course of the cognitive continuum from preclinical to prodromal to clinical AD. It is also important to evaluate the contribution of structural atrophy to changes observed with functional imaging techniques in neurodegenerative diseases. Finally, longitudinal multimodality studies, including structural MRI, fMRI, and FDG-PET and PET amyloid imaging techniques, are needed to understand the relationship between these markers, and the relative value of these techniques in tracking change along the clinical continuum of AD .
Also Check: Dementia Paranoia Accusations
How A Head Ct Scan Can Detect Alzheimers Disease
A head CT scan looks at the structure of your brain. This scan can detect issues such as tumors, hemorrhages, and strokes, which can all mimic the symptoms of Alzheimers, but in addition to helping you rule out those conditions, a CT scan can also detect the loss of brain mass thats associated with Alzheimers disease.
Mri Scans As Accurate As Lumbar Punctures In Identifying Alzheimers Or Ftld
They found that by studying the structural brain patterns the density of gray matter on the MRI scans, their predictions were 75% accurate when confirming diagnosis with people who had pathology-confirmed diagnoses and those with biomarker levels retrieved from lumbar punctures this shows that the new MRI use is as accurate as lumbar puncture methods.
McMillan said:
Developing a new method for diagnosis is important because potential treatments target the underlying abnormal proteins, so we need to know which disease to treat. This could be used as a screening method and any borderline cases could follow up with the lumbar puncture or PET scan.
This method would also be helpful in clinical trials where it may be important to monitor these biomarkers repeatedly over time to determine whether a treatment was working, and it would be much less invasive than repeated lumbar punctures.
Also Check: Did Margaret Thatcher Have Dementia
How Accurate Is Magnetic Resonance Imaging For The Early Diagnosis Of Dementia Due To Alzheimer’s Disease In People With Mild Cognitive Impairment
Why is improving Alzheimer‘s disease diagnosis important?
Cognitive impairment is when people have problems remembering, learning, concentrating and making decisions. People with mild cognitive impairment generally have more memory problems than other people of their age, but these problems are not severe enough to be classified as dementia. Studies have shown that people with MCI and loss of memory are more likely to develop Alzheimer’s disease dementia than people without MCI . Currently, the only reliable way of diagnosing Alzheimer’s disease dementia is to follow people with MCI and assess cognitive changes over the years. Magnetic resonance imaging may detect changes in the brain structures that indicate the beginning of Alzheimer’s disease. Early diagnosis of MCI due to Alzheimer’s disease is important because people with MCI could benefit from early treatment to prevent or delay cognitive decline.
What was the aim of this review?
To assess the diagnostic accuracy of MRI for the early diagnosis of dementia due to Alzheimer’s disease in people with MCI.
What was studied in the review?
The volume of several brain regions was measured with MRI. Most studies measured the volume of the hippocampus, a region of the brain that is associated primarily with memory.
What are the main results in this review?
How reliable are the results of the studies?
Who do the results of this review apply to?
What are the implications of this review?
How up to date is this review?
What Is Alzheimers Disease
Alzheimers is;thought to be the result;of beta-amyloid plaques, which are thick protein deposits present in the brain, and neurofibrillary tangles abnormal structures, which form in neurons building up in the brain. This buildup causes neurons in the brain to cease working, losing connection with other neurons before dying. However, the exact cause of Alzheimers is still unknown. The condition is the most common form of dementia and can quickly progress from being mild to severe.
There are no known causes for Alzheimers since the disease is still being studied. A persons chances of developing Alzheimers tend to increase with age, but people;in their 40s and 50s;can begin showing symptoms of early-onset Alzheimers. People who have;a relative with the condition;may also be at higher risk of developing it themselves since the disease has hereditary factors.
A persons overall physical health may also be a factor in whether they develop Alzheimers disease. One study showed that people who have heart disease or other cardiovascular issues could be at a higher risk of developing Alzheimers;than those with good heart health. This is because cardiovascular issues often reduce the amount of blood the brain receives, which may increase the cognitive issues associated with Alzheimers.
Read Also: Ribbon Color For Dementia
Current Practice In Diagnosing Dementia
The remainder of this information will provide an overview of the diagnosis process and a guide to what happens after diagnosis.;
It is important to remember that there is no definitive test for diagnosing Alzheimers disease or any of the other common causes of dementia. Findings from a variety of sources and tests must be pooled before a diagnosis can be made, and the process can be complex and time consuming. Even then, uncertainty may still remain, and the diagnosis is often conveyed as possible or probable. Despite this uncertainty, a diagnosis is accurate around 90% of the time.;
People with significant memory loss without other symptoms of dementia, such as behaviour or personality changes, may be classified as having a Mild Cognitive Impairment . MCI is a relatively new concept and more research is needed to understand the relation between MCI and later development of dementia. However, MCI does not necessarily lead to dementia and regular monitoring of memory and thinking skills is recommended in individuals with this diagnosis.;;
A New Type Of Brain Scan To Detect Alzheimers Early
May 7, 2012
A new type of brain scan may help to detect Alzheimers early, using no radiation and at less cost than other techniques, researchers report. Doctors at the University of Pennsylvanias Perelman School of Medicine have developed a form of magnetic resonance imaging, or MRI, that detects brain changes that signal Alzheimers disease. The doctors have developed a modification to the technique called arterial spin labeling, or ASL-MRI. Small studies show, this may be a useful way to diagnose probable early dementia.
MRI scans are routinely used in hospitals to check for tumors and other issues, and seniors with memory problems may undergo the procedure to rule out brain tumors, strokes or other problems that may be causing the deficits. If Alzheimers is suspected, they may then undergo another scanning procedure, such as a PET scan.
The advantage of the new ASL-MRI technique is that someone could undergo brain scanning in a single session to help determine whether Alzheimers may be present. The technique looks for changes in blood flow and the uptake of blood sugar, or glucose, in the memory centers of the brain. It requires about an additional 20 minutes compared to standard MRI scans.
Studies show that the MRI method is similar in effectiveness to current PET scans that inject a radioactive dye to measure these brain changes. However, the ASL-MRI method uses no radiation and costs one-fourth as much.
Recommended Reading: Does Meredith Grey Have Alzheimer’s
Additional Tests To Treat And Manage Dementia
Once an individual is diagnosed with dementia, the next step that follows is helping them understand how the condition will affect them and how to manage it.
Several other medical assessments exist to help physicians understand how the condition affects a specific person. And also help families, as well as caregivers, figure out the best course of treatment for the individual.
Did you HEAR of the peanut butter test?
Neuropsychological Testing
Neuropsychologists and psychologists who have specialized training can also prescribe neuropsychological tests to detect dementia.
The process involves WRITTEN and ORAL tests that can take several hours to complete.
They use these methods to assess the cognitive functions of the person suspected to have dementia.
It helps them figure out if certain areas are impaired.
The tests assess aspects like vision-motor, memory, comprehension, reasoning, coordination, and writing abilities.
Physicians may administer additional tests to find out if the person in question is SUFFERING from mood problems or dementia.
Functional Assessments
Dementia is a cognitive disorder that affects the afflicted persons daily functioning in different regards.
Objective assessments can establish what a person is STILL ABLE to do versus what they can no longer do in light of the condition.
Family members are asked to fillquestionnaires that provide details about the persons daily life in terms of the activities they are able to perform.
Psychosocial evaluation
What Are The First Signs Of Lewy Body Dementia & Can An Mri Detect Lewy Body Dementia
Lewy body dementia is an advanced brain disorder. The Lewy bodies build-up in portions of the brain which regulate movement, cognition, and behaviour. This disease affects the bodys autonomic body functions, like temperature regulation, blood pressure control, bowel, and bladder function. Lewy body dementia is considered as the second most prevalent kind of progressive dementia that follows Alzheimers disease dementia.
You May Like: Senile Dementia Of Alzheimer\’s Type