Stage : Moderate Decline
During this period, the problems in thinking and reasoning that you noticed in stage 3 get more obvious, and new issues appear. Your friend or family member might:
- Forget details about themselves
- Have trouble putting the right date and amount on a check
- Forget what month or season it is
- Have trouble cooking meals or even ordering from a menu
- Struggle to use the telephone
- Not understand what is said to them
- Struggle to do tasks with multiple steps like cleaning the house.
You can help with everyday chores and their safety. Make sure they aren’t driving anymore, and that no one tries to take advantage of them financially.
Care Options For Seniors With Alzheimers Disease
As a family caregiver for someone who has Alzheimers, you should know that even the most dedicated families often need to enlist outside memory care help, especially during the latter stages of the disease. Two of the best options for memory care services are in-home care and residential care in a specialized memory care community.
In-Home Care
In-home memory care, often called home care or home health care, can be used to support your loved one while also giving you and your family a much-needed break from your caregiving duties.
In-home care services are provided on a one-on-one basis. A home care provider who specializes in working with individuals who have Alzheimers disease can be hired on an hourly or live-in basis. These professionals can help with activities of daily living, such as bathing, dressing and grooming, that your loved one might not want a family member helping them with.
Home care providers can also assist with light housekeeping and laundry, meal prep and in some cases, pet care. This type of care may be ideal if youre looking for someone who can supervise your loved one while you attend to your own health and well-being or on a respite basis.
Memory Care Communities
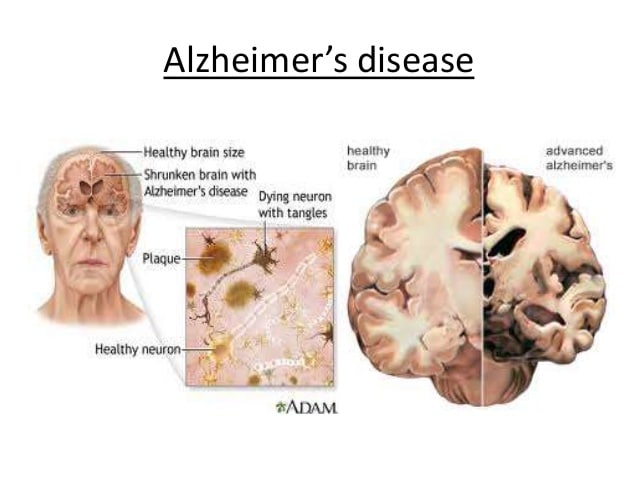
Brain Changes Associated With Alzheimer’s Disease
A healthy adult brain has about 100 billion neurons, each with long, branching extensions. These extensions enable individual neurons to form connections with other neurons. At such connections, called synapses, information flows in tiny bursts of chemicals that are released by one neuron and detected by another neuron. The brain contains about 100 trillion synapses. They allow signals to travel rapidly through the brain’s neuronal circuits, creating the cellular basis of memories, thoughts, sensations, emotions, movements and skills.
The accumulation of the protein fragment beta-amyloid outside neurons and the accumulation of an abnormal form of the protein tau inside neurons are two of several brain changes associated with Alzheimer’s.
Plaques and smaller accumulations of beta-amyloid called oligomers may contribute to the damage and death of neurons by interfering with neuron-to-neuron communication at synapses. Tau tangles block the transport of nutrients and other essential molecules inside neurons. Although the complete sequence of events is unclear, beta-amyloid may begin accumulating before abnormal tau, and increasing beta-amyloid accumulation is associated with subsequent increases in tau.,
Read Also: Can Cause Sores Rashes Dementia Or Blindness
Chronic Diseases And Cognitive Decline A Public Health Issue
People are living longer and by 2030 about one in five Americans will be aged 65 years and older.1 Although increased longevity brings with it many benefits, not all adults necessarily experience good health and well-being as they age.24 Older adults are at a significant risk of having multiple chronic diseases, also known as comorbidities or multi-morbidities, and associated functional impairment.58 Functional impairment refers to limitations in the ability to carry out day-to-day household activities and chores or experiencing interference in engaging in activities outside of the home.3,10 As they continue to age, many older adults live with a growing number of complex health issues that adversely affect their day-to-day functioning and overall quality of life.9 For some people and groups of older adults, these concerns are further compounded by the presence of memory issues.
Subjective cognitive decline is the self-reported experience of worsening or more frequent confusion or memory loss within the past year.2,3 It is a form of cognitive impairment and one of the earliest noticeable symptoms of more severe memory disorders such as Alzheimers disease and related dementias.3,11
SCD can have detrimental implications for living with and managing chronic diseases, or performing everyday activities like cooking or cleaning.3 When cognition is impaired, it can have a profound impact on an individuals overall health and well-being.
This brief examines the following topics:
Use And Costs Of Long
An estimated 70% of older adults with Alzheimer’s or other dementias live in the community, compared with 98% of older adults without Alzheimer’s or other dementias. Of those with dementia who live in the community, 74% live with someone and the remaining 26% live alone. As their disease progresses, people with Alzheimer’s or other dementias generally receive more care from family members and other unpaid caregivers. Many people with dementia also receive paid services at home in adult day centers, assisted living facilities or nursing homes or in more than one of these settings at different times during the often long course of the disease. Medicaid is the only public program that covers the long nursing home stays that most people with dementia require in the late stages of their illnesses.
6.3.1 Use of long-term care services by setting
Long-term care services provided at home and in the community
Transitions between care settings
6.3.2 Costs of long-term care services
Affordability of long-term care services
Long-term care insurance
Medicaid costs
| State |
|---|
You May Like: What Color Ribbon Is Alzheimer’s
Stage : Normal Outward Behavior
Alzheimerâs disease usually starts silently, with brain changes that begin years before anyone notices a problem. When your loved one is in this early phase, they won’t have any symptoms that you can spot. Only a PET scan, an imaging test that shows how the brain is working, can reveal whether they have Alzheimer’s.
As they move into the next six stages, your friend or relative with Alzheimer’s will see more and more changes in their thinking and reasoning.
Epidemiology Risk Factors Genetics And Neuropathology
Alzheimers Dement.
- Guerchet M.M.
- et al.
Alzheimers Dement.
- Armstrong M.J.
- et al.
Neurology.Neurology.
Alzheimers Dement.
| Modifiable | Nonmodifiable |
|---|---|
Dementia prevention, intervention, and care.Lancet.2017 390: 2673-2734 |
Alzheimer disease in the United States estimated using the 2010 census.Neurology.2013 80: 1778-1783
Lifetime risk of dementia and Alzheimer’s disease. The impact of mortality on risk estimates in the Framingham Study.Neurology.1997 49: 1498-1504)Family history Race Down syndromeApolipoprotein -4 allele carriers Cerebral amyloidosis |
Acta Neuropathol.J Neural Transm.Ann Neurol.Alzheimers Dement.Neurology.Lancet.
Neuropathol Appl Neurobiol.Neurodegener Dis.Neurology.
Nat Genet.
- Strittmatter W.J.
- et al.
Science.Ann N Y Acad Sci.Nat Rev Neurosci.Arch Neurol.
Arch Neurol.J Neurochem.Nature.Sci Am.Science.Science.Nat Rev Neurosci.
You May Like: What Color Ribbon Is Alzheimer’s
Demographic Characteristics Of Adults By Subjective Cognitive Decline And Chronic Diseasea Status
| With Subjective Cognitive Decline | |
|---|---|
| 45.5 | 54.2 |
Across all demographic characteristics except for non-Hispanic Asian and Pacific Islanders, a higher proportion of those with SCD reported having at least one chronic disease than those without SCD.
Age: The prevalence of having at least one chronic disease was lower among adults aged 4564 years than those aged 65 years and older.
Sex: Of adults aged 45 years and older with SCD, women had a higher prevalence of having at least one chronic disease compared with men .
Race and ethnicity: Across all races, except for non-Hispanic Asians and Pacific Islanders, those with SCD had a higher prevalence of having one or more chronic diseases than those without SCD.
Education: Among both adults with and without SCD, those with at least a college degree have a lower prevalence of having at least one chronic disease compared with those with less than a college degree.
Living status: Among adults with SCD, those who live alone reported a higher prevalence of having at least one chronic disease compared with those who do not live alone .
Causes Of Cognitive Decline In Heart Failure
Stroke in patients with heart failure
Impaired cerebral perfusion
Cerebrovascular autoregulation both globally and regionally in response to functional activity and local oxygen demands is impaired in HF. This vascular variability is locally controlled by pericytes, perivascular cells with contractile capacity at the capillary level. The resulting hypoperfusion seen with both acute and chronic HF may cause or worsen cognitive decline in HF.
Recommended Reading: What Color Ribbon Is For Dementia
Early Onset Alzheimers Disease
Although age is the main risk factor for Alzheimers disease, this is not just a condition that affects older adults.
According to the Alzheimers Association, early onset Alzheimers disease affects around 200,000 U.S. adults under the age of 65 years. Many people with this condition are in their 40s or 50s.
In many cases, doctors do not know why younger people develop this condition. Several rare genes can cause the condition. When there is a genetic cause, it is known as familial Alzheimers disease.
Causes For Chronic Lower Back Pain
Acute Versus Chronic Pain Treatment In Alzheimer S Disease Chronic Shoulder Pain Physical Therapy Google Scholar Strongest Pain Relief Without Prescription, Journal Articles Improving Pain Relief With Oral Analgesics After Knee Replacment Lady Gaga Turns To Gyrotonic Workout To Soothe Chronic Muscle Pain Chronic Chest Pain At Rest Comes And Goes.
St Louis Neuropathy Pain Relief Topical Pain Relief Remedies For Skin. Back Pain Relief Applicator Pain Relief Ear Drops Over The Counter Real Relief From Back Pain Teresa Carr. Kelly Mcgonigal Yoga Pain Relief Odorless Topical Pain Relief.
Recommended Reading: Alzheimer Awareness Ribbon
Microglial Activation Aggravates Ad Via Tau Pathology
Neurofibrillary tangles in the brain of AD patients increase in parallel with colocalized expression of microglial pro-inflammatory activation and tau kinases . Hyperphosphorylated tau, misfolded tau, and truncated tau co-occurs with microglia proliferation and increased expression of inflammatory genes such as Aif1 , Ptgs2 , IL-1, IL-6, and Tnf- in the LC . These findings suggest that activated microglia may participate in driving tau pathology in AD.
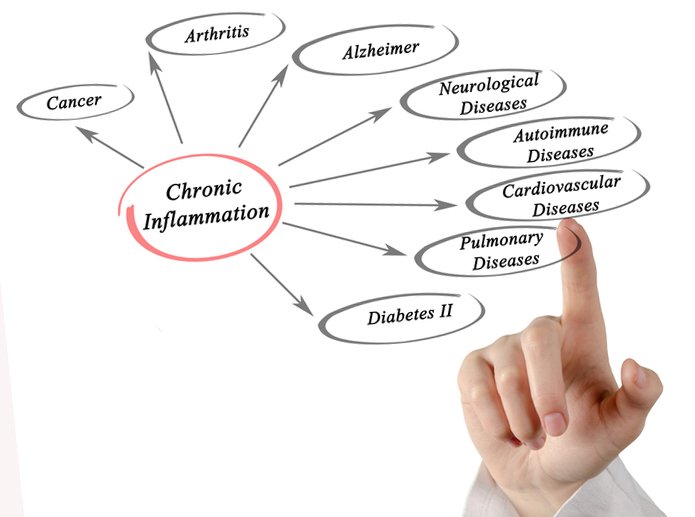
Inflammation Acute Vs Chronic
The immune system operating via the lymphatic and circulatory systems acts as the defender of the body. It keeps out what needs to be kept out, fights when it needs to fight and protects by cleaning up and disposing of dead or damaged cells.
A key component of a healthy immune system is inflammation. Inflammation is triggered immediately when it detects damage in the cells or tissues as a result of injury or the presence of pathogens or other toxins. Acute inflammation is the initial phase of the inflammation process. It is the first line of defense against disease. It is the time period when function is impaired. The area may be swollen, hot, red and painful. It is the 911 call to the immune system that danger is present and the system must be activated to neutralize the threat. Acute inflammation is short lived and is a positive, protective, healing and renewing mechanism.
Chronic inflammation on the other hand is not beneficial. Chronic inflammation is not a friend to the body nor is it short lived. It is a sign that things are getting out of control and instead of attacking invaders the body is attacking itself. Chronic inflammation drains the immune system as it continues to prompt the immune system to send white blood cells to attack healthy tissue and organs setting up a chronic inflammatory process.
Chronic inflammation may be caused by:
Symptoms / signs of chronic inflammation include:
You May Like: Dementia Ribbon
Chronic Pain May Aggravate Ad Neuropathogenesis Through Lc
Chronic pain and AD brains not only display abnormal LC structure and function but also dynamic changes in NE turnover in LC-projecting areas . Although the shifts of NE content may not perfectly overlap in all brain areas in these two disease states, LC-NE pathological changes in select regions could be one of the initiators that leads to a final common outcome: pro-inflammatory activation of microglia and neuronal dysfunction.
Signs And Symptoms Of Alzheimer’s Disease
Memory problems are typically one of the first signs of cognitive impairment related to Alzheimers. Some people with memory problems have a condition called mild cognitive impairment . With MCI, people have more memory problems than normal for their age, but their symptoms do not interfere with their everyday lives. Movement difficulties and problems with the sense of smell have also been linked to MCI. Older people with MCI are at greater risk for developing Alzheimers, but not all of them do so. Some may even revert to normal cognition.
The first symptoms of Alzheimers vary from person to person. For many, decline in nonmemory aspects of cognition, such as word-finding, vision/spatial issues, and impaired reasoning or judgment may signal the very early stages of the disease. Researchers are studying biomarkers to detect early changes in the brains of people with MCI and in cognitively normal people who may be at greater risk for Alzheimers. More research is needed before these techniques can be used broadly and routinely to diagnose Alzheimers in a health care providers office.
Also Check: Did Reagan Have Alzheimers
Ace Inhibitors And Angiotensin Receptor Blockers And Beta
ACE inhibitors and angiotensin receptor blockers have been shown to improve cognitive function in both hypertension and HF. Beta-blockers worsen dizziness and hypotension in HF which is a theoretical risk for worsening cognitive function in fragile elderly HF patients. Sacubitril/valsartan in the PARADIGM-HF trial, whilst reducing mortality and morbidity was associated with more hypotension compared to patients randomized to enalapril, and there is an as yet unresolved concern about its potential to promoting Alzheimers disease via inhibition of NEP degradation of -amyloid and the potential accumulation of A in the brain. However, analyses of PARADIGM did not find any increased risk of dementia or Alzheimers.,
Devices used to treat HF such as left ventricular assist devices carry an increased risk of embolic stroke, bleeding, and thrombotic complications. Changes in systemic immune state, platelet function, and acquired von Willebrand syndrome may potentially lead to cerebral infarction and haemorrhage. Other devices such as Veno-arterial extracorporeal membrane oxygenation are similarly thought to lead to an increased risk of thrombosis, bleeding, and neurologic events.
What Are The Most Common Types Of Dementia
- Alzheimers disease. This is the most common cause of dementia, accounting for 60 to 80 percent of cases. It is caused by specific changes in the brain. The trademark symptom is trouble remembering recent events, such as a conversation that occurred minutes or hours ago, while difficulty remembering more distant memories occurs later in the disease. Other concerns like difficulty with walking or talking or personality changes also come later. Family history is the most important risk factor. Having a first-degree relative with Alzheimers disease increases the risk of developing it by 10 to 30 percent.
- Vascular dementia. About 10 percent of dementia cases are linked to strokes or other issues with blood flow to the brain. Diabetes, high blood pressure and high cholesterol are also risk factors. Symptoms vary depending on the area and size of the brain impacted. The disease progresses in a step-wise fashion, meaning symptoms will suddenly get worse as the individual gets more strokes or mini-strokes.
- Lewy body dementia. In addition to more typical symptoms like memory loss, people with this form of dementia may have movement or balance problems like stiffness or trembling. Many people also experience changes in alertness including daytime sleepiness, confusion or staring spells. They may also have trouble sleeping at night or may experience visual hallucinations .
Don’t Miss: Smelling Farts Dementia
Discussing Chronic Diseases And Subjective Cognitive Decline
Figure 7: Adults aged 45 years and older with one or more chronic diseases and subjective cognitive decline who reported discussing their subjective cognitive decline with a health care professional
d.Limited Sample size refers to the low number of telephone participants included in the BRFSS study which reduces quality of study results.
Have you or anyone else discussed your confusion or memory loss with a health care professional?
Although nearly half of adults aged 45 and older with more than one chronic disease and subjective cognitive decline reported discussing their subjective cognitive decline with a health care professional, adults without chronic diseases were less likely to discuss symptoms of SCD with a health care professional.
The disparity between those with and without chronic diseases who discussed symptoms of SCD with a health care professional appears greater among middle-aged than older adults. Among adults aged 4564, 54.2% of those with at least one chronic disease reported discussing symptoms of SCD with a health care professional while only 30.8% of those with no chronic diseases reported discussing SCD with a health care professional. Among adults aged 65 years and older, 41.0% of those with one or more chronic disease discussed SCD while 32.3% of those with no chronic diseases discussed SCD.
- People with SCD are more likely to have multiple co-morbid chronic diseases which can complicatemanagement.
Risk Factors For Alzheimer’s Dementia
The vast majority of people who develop Alzheimer’s dementia are age 65 or older. This is called late-onset Alzheimer’s. Experts believe that Alzheimer’s, like other common chronic diseases, develops as a result of multiple factors rather than a single cause. Exceptions are cases of Alzheimer’s related to uncommon genetic changes that increase risk.
2.7.1 Age, genetics and family history
The greatest risk factors for late-onset Alzheimer’s are older age,, genetics, and having a family history of Alzheimer’s.-
Age
Age is the greatest of these three risk factors. As noted in the Prevalence section, the percentage of people with Alzheimer’s dementia increases dramatically with age: 3% of people age 65-74, 17% of people age 75-84 and 32% of people age 85 or older have Alzheimer’s dementia. It is important to note that Alzheimer’s dementia is not a normal part of aging, and older age alone is not sufficient to cause Alzheimer’s dementia.
Genetics
| APOE Pair |
|---|
- One in 10 people age 65 and older has Alzheimer’s dementia.,,
- The percentage of people with Alzheimer’s dementia increases with age: 3% of people age 65-74, 17% of people age 75-84, and 32% of people age 85 and older have Alzheimer’s dementia. People younger than 65 can also develop Alzheimer’s dementia, but it is much less common and prevalence is uncertain.
3.1.1 Underdiagnosis of Alzheimer’s and other dementias in the primary care setting
3.1.2 Prevalence of subjective cognitive decline
Don’t Miss: What’s The Difference Between Dementia And Alzheimer’s And Senility