How To Connect With The Person
Communicating with a person with late-stage Alzheimers disease can take effort and patience. Though that persons ability to respond may be limited, it is important to continue to interact:
- Continue to visit with the person even if responses are limited.
- Try to speak calmly and slowly be aware of the tone and volume of your voice.
- Consider sharing familiar stories with the person.
- Make eye contact, say the persons name and smile.
- Use other methods of communication besides speaking, such as gentle touching or massage.
- Have the person listen to music or calming nature sounds.
Learn more about how to communicate with a person who has Alzheimer’s disease.
Stage : Mild Dementia
At this stage, individuals may start to become socially withdrawn and show changes in personality and mood. Denial of symptoms as a defense mechanism is commonly seen in stage 4. Behaviors to look for include:
- Difficulty remembering things about one’s personal history
- Disorientation
- Difficulty recognizing faces and people
In stage 4 dementia, individuals have no trouble recognizing familiar faces or traveling to familiar locations. However, patients in this stage will often avoid challenging situations in order to hide symptoms or prevent stress or anxiety.
Behavioral And Cognitive Symptoms Of Dementia
Behavioral Symptoms
Michelle Niedens, L.S.C.S.W., in The Neuropsychiatric Symptoms of Alzheimers, states that 80% of individuals with dementia will experience neuropsychiatric symptoms.
Personality changes such as anxiety, depression or irritability are common in the early stages of the disease. Later, agitation, physical or verbal outbursts, pacing and restlessness are more common.
Behavioral symptoms have been identified as the most challenging and distressing for caregivers and family members. They are oftentimes the determining factor in deciding to move a family member with Alzheimers into a structured living environment.
Cognitive Symptoms
Cognitive symptoms start out mild in the early stages of Alzheimers and gradually worsen as each stage progresses. In the late stages of Alzheimers, the person with the disease is no longer able to form new memories or access old ones. Language abilities become worse until the person is no longer able to communicate. Judgment and reasoning skills continue to diminish and eventually, the person with dementia loses the ability to reason altogether.
Don’t Miss: What Percentage Of Dementia Is Alzheimer’s
How Long Will A Person With Dementia Live For
Whatever type of dementia a person has, their life expectancy is on average lower. This is why dementia is called a life-limiting condition. This can be very upsetting to think about.
However, its important to remember that, no matter how a persons dementia changes over time, there are ways to live well with the condition.
Good support can make a huge difference to the persons quality of life at all stages of dementia.
How long a person lives with dementia varies greatly from person to person. It depends on many factors, such as the ones listed on The progression and stages of dementia page.
Other factors include:
- how far dementia had progressed when the person was diagnosed
- what other serious health conditions the person with dementia has such as diabetes, cancer, or heart problems
- how old the person was when their symptoms started older people are more likely than younger people to have other health conditions that may lower their life expectancy. A person in their 90s who is diagnosed with dementia is more likely to die from other health problems before they reach the later stages than is a person diagnosed in their 70s.
Stage : Very Severe Cognitive Declinesevere Dementia
At this stage, AD persons require continuous assistance with basic activities of daily life for survival. Six consecutive functional substages can be identified over the course of this final seventh stage. Early in this stage, speech has become so circumscribed, as to be limited to approximately a half-dozen intelligible words or fewer . As this stage progresses, speech becomes even more limited to, at most, a single intelligible word . Once intelligible speech is lost, the ability to ambulate independently , is invariably lost. However, ambulatory ability may be compromised at the end of the sixth stage and in the early portion of the seventh stage by concomitant physical disability, poor care, medication side-effects or other factors. Conversely, superb care provided in the early seventh stage, and particularly in stage 7b, can postpone the onset of loss of ambulation. However, under ordinary circumstances, stage 7a has a mean duration of approximately 1 year, and stage 7b has a mean duration of approximately 1.5 years.
In persons with AD who remain alive, stage 7c lasts approximately 1 year, after which persons with AD lose the ability not only to ambulate independently but also to sit up independently , At this point in the evolution, the person will fall over when seated unless there are armrests to assist in sitting up in the chair.
Read Also: Does Diet Pop Cause Dementia
The Three Stages Of Alzheimers Disease
James M. Ellison, MD, MPH
Swank Center for Memory Care and Geriatric Consultation, ChristianaCare
- Expert Advice
Patients, families and clinicians all want to know how far Alzheimers disease has progressed and what the future is likely to hold. Learn about the symptoms associated with the three stages of the disease.
Dr. Alois Alzheimer described the disease that was later given his name more than 100 years ago, but not until 1984 did health care providers and researchers agree on a standard approach to the diagnosis of Alzheimers disease. In 1984, workgroups from the National Institutes of Health and other organizations published a set of diagnostic criteria that later became the gold standard for diagnosis.1 Their guideline emphasized that in order for a person to be diagnosed with probable Alzheimers disease, they must show difficulties in two or more areas of cognitive functioning, progressive worsening of memory, onset of symptoms between ages of 40 and 90, and no delirium or other likely cause for cognitive decline. Definite Alzheimers disease, according to their criteria, was only diagnosed after confirmation by brain biopsy or autopsy.
The International Classification of Diseases and psychiatrys Diagnostic and Statistical Manual adopted similar standards for assigning an AD diagnosis, and this approach is commonly used now throughout the world.
How Does Dementia Reduce Life Expectancy
Dementia reduces life expectancy in two ways.
First, some of the diseases that are closely linked to Alzheimers disease and vascular dementia, such as diabetes and cardiovascular disease can mean a lower life expectancy. For example, vascular dementia is closely linked to heart disease and stroke. A person with vascular dementia is at risk of dying at any stage of dementia, from one of these.
The other way that dementia reduces life expectancy is through the effects of severe disease.
These all make them much more likely to develop other medical problems that can lead to death, such as infections or cardiovascular problems .
This is why the later stage of dementia is often the shortest.
A person with dementia can also die at any stage from another condition not closely related to their dementia. Cancer and lung disease are common examples.
You May Like: What Happens To Your Brain With Alzheimer’s
How Is Alzheimers Disease Diagnosed
Doctors use several methods and tools to help determine whether a person who is having memory problems has Alzheimers disease.
To diagnose Alzheimers, doctors may:
- Ask the person and a family member or friend questions about overall health, use of prescription and over-the-counter medicines, diet, past medical problems, ability to carry out daily activities, and changes in behavior and personality.
- Conduct tests of memory, problem solving, attention, counting, and language.
- Carry out standard medical tests, such as blood and urine tests, to identify other possible causes of the problem.
- Perform brain scans, such as computed tomography , magnetic resonance imaging , or positron emission tomography , to support an Alzheimers diagnosis or to rule out other possible causes for symptoms.
These tests may be repeated to give doctors information about how the persons memory and other cognitive functions are changing over time.
People with memory and thinking concerns should talk to their doctor to find out whether their symptoms are due to Alzheimers or another cause, such as stroke, tumor, Parkinsons disease, sleep disturbances, side effects of medication, an infection, or another type of dementia. Some of these conditions may be treatable and possibly reversible.
In addition, an early diagnosis provides people with more opportunities to participate in clinical trials or other research studies testing possible new treatments for Alzheimers.
Dental Skin And Foot Problems
Dental, skin, and foot problems may take place in early and moderate stages of Alzheimer’s disease, but most often happen during late-stage Alzheimer’s disease.
Dental problems. As Alzheimer’s disease symptoms worsen, people will need help taking care of their teeth or dentures. Brushing and flossing help to maintain oral health and reduce bacteria in the mouth, which may decrease the risk of pneumonia.
Make sure the person’s teeth and teeth surfaces are gently brushed at least twice a day with fluoride toothpaste. The last brushing session should take place after the evening meal or after any medication is given at night. You may find that using a child’s size toothbrush is easier for the person.It is also best to floss once per day, if possible. If this is distressing to the person, an interdental brush, which is a small brush designed to clean between the teeth. Try to check the person’s mouth for any problems such as:
- Sores
- Food “pocketed” in the cheek or on the roof of the mouth
- Lumps
Be sure to take the person for regular dental checkups for as long as possible. Some people need medicine to calm them before they can see the dentist. Calling the dentist beforehand to discuss potential sensitivities may also be helpful.
Skin problems. Once the person stops walking or stays in one position too long, he or she may get skin or pressure sores. To prevent them, you can:
To check for pressure sores:
Read Also: What Is Life Like With Alzheimer’s
How Important Are The Stages Of Dementia
The stages of dementia are just a guide and there is nothing significant about the number three. Equally, dementia doesnt follow an exact or certain set of steps that happen in the same way for every person with dementia.
It can be difficult to tell when a persons dementia has progressed from one stage to another because:
- some symptoms may appear in a different order to the stages described in this factsheet, or not at all
- the stages may overlap the person may need help with some aspects of everyday life but manage other tasks and activities on their own
- some symptoms, particularly those linked to behaviours, may develop at one stage and then reduce or even disappear later on. Other symptoms, such as memory loss and problems with language and thinking, tend to stay and get worse with time.
It is natural to ask which stage a person is at or what might happen next. But it is more important to focus on the person in the present moment. This includes their needs and how they can live well, and how to help them with this.
For more support on living well with dementia see The dementia guide: living well after diagnosis or Caring for a person with dementia: a practical guide .
And for more information about treatment and support for the different types of dementia go to the following pages:
Scales For Rating Dementia
Rather than simply using early stage,middle-stage, and late-stage dementia as descriptors, there are scales that provide a more comprehensive description. These scales help better understand the different stages of Alzheimers disease based on how well a person thinks and functions . These scales are the Global Deterioration Scale for Assessment of Primary Degenerative Dementia, the Functional Assessment Staging Test, and the Clinical Dementia Rating.
Did You Know?
Global Deterioration Scale / Reisberg Scale
The most commonly used scale is often referred to simply as GDS, or by its more formal name, the Reisberg Scale . The GDS divides into seven stages based on the amount of cognitive decline. This test is most relevant for people who have Alzheimers disease because some other types of dementia do not always include memory loss.
Someone in stages 1-3 does not typically exhibit enough symptoms for a dementia diagnosis. By the time a diagnosis has been made, a dementia patient is typically in stage 4 or beyond. Stage 4 is considered early dementia, stages 5 and 6 are considered middle dementia, and stage 7 is considered late dementia.
| Global Deterioration Scale / Reisberg Scale |
| Diagnosis |
Clinical Dementia Rating
| Clinical Dementia Rating Scale |
| Stage |
| Average duration is 1 year to 2.5 years. |
Also Check: How Do Anti Dementia Drugs Work
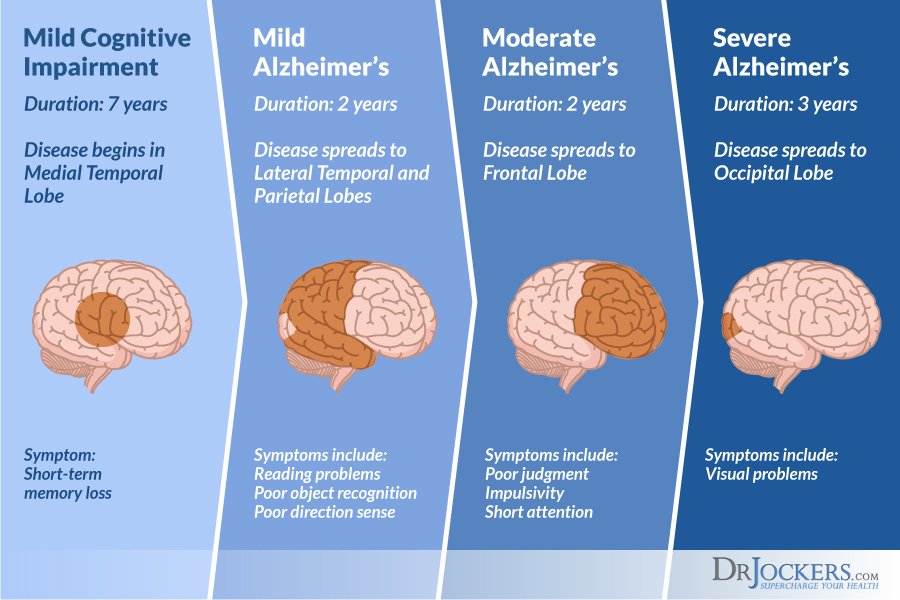
Alzheimers Progression: Mild Moderate And Severe Stages
Alzheimers is a progressive disease that damages neurons in the brain, affecting a persons ability to remember, reason, judge, use language, and otherwise meet the demands of daily life.
While there are treatments that can help sharpen the mind for a short while and make behavioral symptoms more manageable, there is currently no cure.
In a typical case, Alzheimers first destroys neurons and their connections in parts of the brain that retain memories, including the entorhinal cortex and hippocampus.
Later the disease causes damage to regions in the cerebral cortex that control language, reasoning, and social behavior. Eventually many other parts of the brain are affected.
Ultimately the disease is fatal. On average people with Alzheimers live for four to eight years after diagnosis, although some can live as long as 20 years depending on other factors.
More than one-half of all Alzheimers-related deaths are caused by respiratory system diseases, such as pneumonia, an infection that can develop when swallowing issues result in food and liquid entering the lungs.
Every person with Alzheimers will experience the disease in a different way. Some retain their cognitive abilities for longer than expected, while others move more quickly through the various stages.
Among the factors that influence the speed of progression are age, overall health, emotional resilience, medication regimen, and network of support.
The Progression And Stages Of Dementia
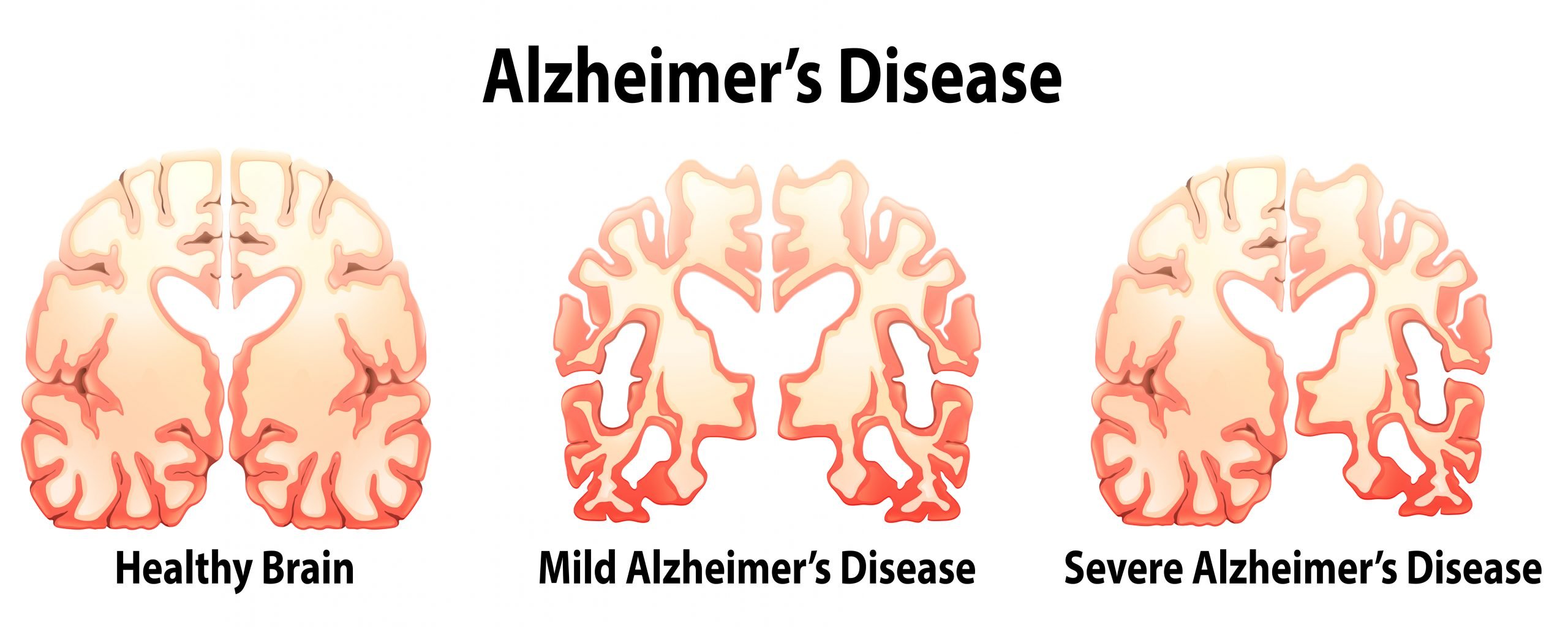
Dementia is progressive. This means symptoms may be relatively mild at first but they get worse with time. Dementia affects everyone differently, however it can be helpful to think of dementia progressing in ‘three stages’.
The progression and stages of dementia
Read Also: Who Gets Alzheimer’s The Most
Second Dementia Stage: Very Mild Decline
Older adults at the second stage of dementia may begin to notice that they are experiencing some minor memory issues. It is common for people at this stage to forget where they put things in the house. Memory lapses can also be seen when a person forgets the names that were at one time familiar. The memory loss patients experience during the second stage of dementia cannot be clearly distinguished from the ordinary age-related memory loss. It is to say that an individual may still do well when they go through memory tests.
It is also possible that physicians and loved ones may not be in a position to detect the disease at this stage. Studies reveal that almost half of the 65 and older generation report minor forgetfulness. It is also important to understand that the subtle changes could have nothing to do with dementia, but they might just be regular changes that come about as a person becomes older.
However, if a person has dementia, it may be severe enough to interfere with a persons ability to live independently or complete their daily chores. Life may go on normally at this point apart from occasional cases of slight memory loss.
Stages Of Alzheimer Disease
The stages of Alzheimer disease usually follow a progressive pattern. But each person moves through the disease stages in his or her own way. Knowing these stages helps healthcare providers and family members make decisions about how to care for someone who has Alzheimer disease.
Preclinical stage. Changes in the brain begin years before a person shows any signs of the disease. This time period is called preclinical Alzheimer disease and it can last for years.
Mild, early stage. Symptoms at this stage include mild forgetfulness. This may seem like the mild forgetfulness that often comes with aging. But it may also include problems with concentration.
A person may still live independently at this stage, but may have problems:
-
Remembering a name
-
Staying organized
-
Managing money
The person may be aware of memory lapses and their friends, family or neighbors may also notice these difficulties.
Moderate, middle stage. This is typically the longest stage, usually lasting many years. At this stage, symptoms include:
-
Increasing trouble remembering events
-
Problems learning new things
-
Trouble with planning complicated events, like a dinner
-
Trouble remembering their own name, but not details about their own life, such as address and phone number
-
Problems with reading, writing, and working with numbers
As the disease progresses, the person may:
Physical changes may occur as well. Some people have sleep problems. Wandering away from home is often a concern.
You May Like: How To Tell The Difference Between Alzheimer’s And Dementia
Changes In Mood Emotions And Perceptions
Changes in mood remain in the later stages of dementia. Depression and apathy are particularly common.
Delusions and hallucinations are most common in the late stage of dementia. They are not always distressing but they can explain some changes in behaviour because the persons perception of reality is altered.
People with later stage dementia often respond more to senses than words. They may like listening to songs or enjoy textures. For example, they may like the feel of different types of material.
Stage : Decreased Or Inability To Control Bodily Functions
As Alzheimer’s progresses, it destroys brain cells. This can lead to severe mental and physical impairment. Your loved one may start to have problems with their body shutting down. This happens when their mind can no longer process, communicate, or delegate tasks effectively.1
Your loved one’s needs will increase a lot now. They will need help walking, sitting, and even swallowing. Because they are not as mobile, they can get infections more easily. At this point, your loved one will need full-time care.1
Read Also: How Quickly Does Dementia Progress