Pandemic Sparks New Discussions About Disparity
In 2020, the COVID-19 pandemic and social justice movements sparked new conversations about endemic and long-standing health and health care disparities faced by people of color, especially when it comes to access, discrimination and trust in the health care system., People of color were disproportionately affected by the environmental, societal and economic impact of the pandemic facing greater risk of losing a job or income, being more likely to be frontline workers with greater risk of exposure to the SARS-CoV-2 virus that causes COVID-19, and having a higher likelihood of housing uncertainty and food insecurity due to the pandemic.- The effects of these social, economic and environmental factors, known as social determinants of health, can put a population’s current and future health in jeopardy. For example, they have created stark contrasts in COVID-19 infection rates and outcomes. Black, Native American and Hispanic communities have seen COVID-19 cases, hospitalizations and deaths at rates greater than Whites, and these events far exceed their share of the U.S. population.-
Amyloid Hypothesis Versus Tau Hypothesis
A central but controversial issue in the pathogenesis of AD is the relationship between amyloid deposition and NFT formation. Evidence shows that abnormal amyloid metabolism plays a key pathogenic role. At high concentrations, the fibrillar form of Ab has been shown to be neurotoxic to cultured neurons.
Cultured cortical and hippocampal neurons treated with Ab protein exhibit changes characteristic of apoptosis , including nuclear chromatin condensation, plasma membrane blebbing, and internucleosomal DNA fragmentation. The fibrillar form of Ab has also been shown to alter the phosphorylation state of tau protein.
The identification of several point mutations within the APP gene in some patients with early-onset familial AD and the development of transgenic mice exhibiting cognitive changes and SPs also incriminate Ab in AD. The apolipoprotein E E4 allele, which has been linked with significantly increased risk for developing AD, may promote inability to suppress production of amyloid, increased production of amyloid, or impaired clearance of amyloid with collection outside of the neuron.
Autopsies have shown that patients with 1 or 2 copies of the APOE E4 allele tend to have more amyloid. Additional evidence comes from recent experimental data supporting the role of presenilins in Ab metabolism, as well as findings of abnormal production of Ab protein in presenilin-mutation familial Alzheimer disease.
Differences Between Women And Men In The Prevalence And Risk Of Alzheimer’s And Other Dementias
More women than men have Alzheimer’s or other dementias. Almost two-thirds of Americans with Alzheimer’s are women. Of the 6.2 million people age 65 and older with Alzheimer’s in the United States, 3.8 million are women and 2.4 million are men. This represents 12% of women and 9% of men age 65 and older in the United States.
The prevailing reason that there are more women living with Alzheimer’s or other dementias than men is most likely the fact that women live longer than men on average, and older age is the greatest risk factor for Alzheimer’s.- However, when it comes to differences in the actual risk of developing Alzheimer’s or other dementias for men and women of the same age , findings have been mixed. Most studies of incidence in the United States have found no significant difference between men and women in the proportion who develop Alzheimer’s or other dementias at any given age., , – Some European studies have reported a higher incidence among women at older ages,, and one study from the United Kingdom reported higher incidence for men. Differences in the risk of dementia between men and women may therefore depend on age and/or geographic region.,
Read Also: Alzheimer’s Disease Ribbon Color
Living With Alzheimer’s Disease
Alzheimer’s disease affects more than six million Americans and can be devastating for those who live with the disease and their loved ones. Explore the resources in this guide to find the support, tips and care services that can help you and your family during every stage of the disease.
Alzheimer’s disease is a form of dementia that affects more than six million Americans. Scientists don’t know the exact cause, although many researchers suspect that it occurs due to a combination of age-related changes in the brain, lifestyle factors, environmental variations and genetic factors.
Because Alzheimer’s disease gets worse over time, early detection is important. The sooner you recognize the symptoms, the sooner your loved one can get the support they need. This guide provides an overview of Alzheimer’s disease and offers tips to help caregivers understand how they can help their loved ones.
Memory loss is one of the most common signs of Alzheimer’s disease. Occasional forgetfulness isn’t usually a problem, but if your loved one asks the same question multiple times, can’t remember important events, forgets information they just learned or has to take notes to remember important information, they could have memory loss caused by Alzheimer’s disease or another form of dementia.
The brain changes that occur in Alzheimer’s disease may also make your loved one forget where they are or forget how they got from one place to another.
- Difficulty solving problems
Early Signs And Symptoms Of Alzheimers Disease
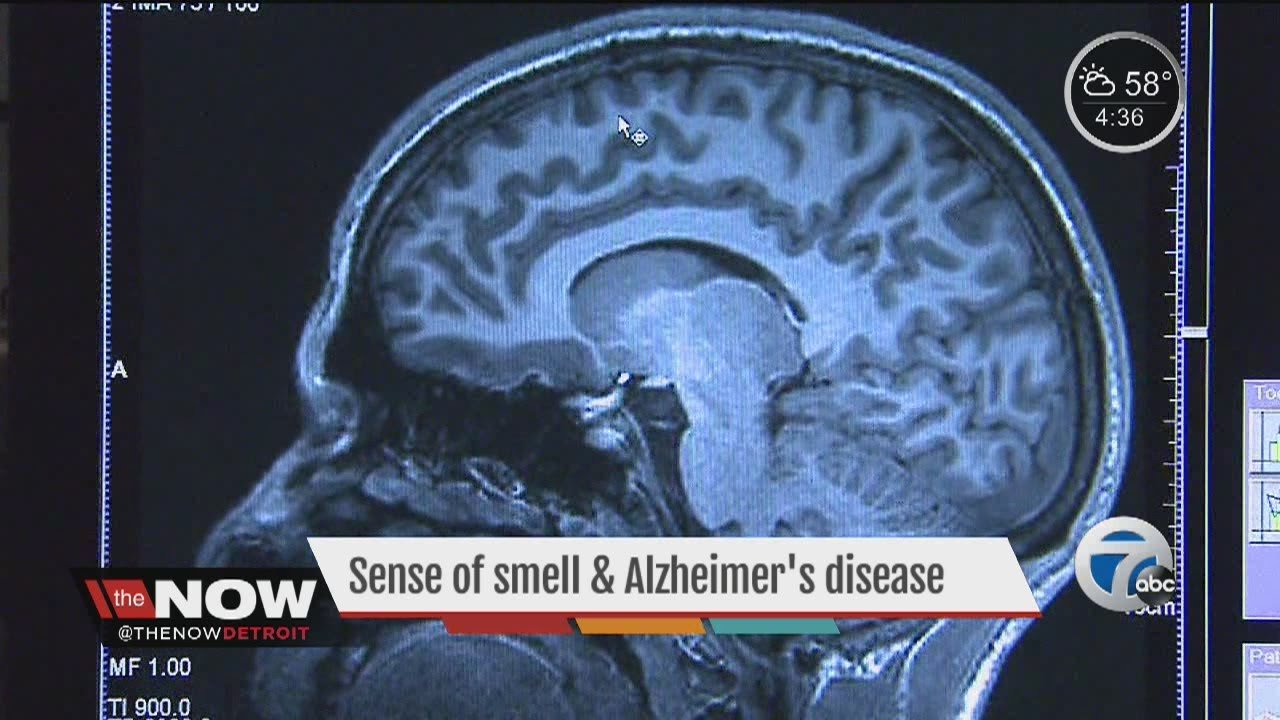
For most people who develop Alzheimers, it tends to be changes in memory that are detected first. You may notice the decline yourself or have it pointed out to you by family or friends. But the disease is about more than just memory changes. Alzheimers also presents itself as problems with language, judgment, and abstract thinking.
The early warning signs of Alzheimers disease include:
You May Like: At What Age Alzheimer’s Start
Treatments For Individual Symptoms
People with moderate Alzheimers and other dementias can suffer from a host of other symptoms, ranging from depression and anxiety to sleep issues and aggressiveness. But because many of the meds used to treat these symptoms can cause more problems, doctors try to avoid them unless the issue is so severe that all sorts of behavior-modifying tactics arent working any more. These drugs include:
-
Anti-anxiety drugsto treat agitation. These should be used sparingly as they can cause dizziness, sleepiness and up the chances of a fall. Drugs include Xanax , Ativan , and Valium .
-
Anti-depressantsfor irritability, general anxiety, or depression. These are generally safe to take but talk to your doctor. Medications include Prozac , Zoloft , and Celexa .
-
Anti-psychoticsfor extreme aggression, hallucinations, and delusions. This type of med can increase the risk of stroke in older folks with dementia, so its a medication of last resort. Drugs include Abilify and Seroquel .
Early In Alzheimer Disease
Symptoms develop gradually, so for a while, many people continue to enjoy much of what they enjoyed before developing Alzheimer disease.
Symptoms usually begin subtly. People whose disease develops while they are still employed may not do as well in their jobs. In people who are retired and not very active, the changes may not be as noticeable.
The first and most noticeable symptom may be
-
Forgetting recent events because forming new memories is difficult
-
Sometimes changes in personality
Early in the disease, people become less able to use good judgment and think abstractly. Speech patterns may change slightly. People may use simpler words, a general word or many words rather than a specific word, or use words incorrectly. They may be unable to find the right word.
People with Alzheimer disease have difficulty interpreting visual and audio cues. Thus, they may become disoriented and confused. Such disorientation may make driving a car difficult. They may get lost on their way to the store. People may be able to function socially but may behave unusually. For example, they may forget the name of a recent visitor, and their emotions may change unpredictably and rapidly.
Many people with Alzheimer disease often have insomnia. They have trouble falling or staying asleep. Some people become confused about day and night.
At some point, psychotic behavior develops in many people with Alzheimer disease.
Don’t Miss: Does Alzheimer’s Cause Dementia
Neurofibrillary Tangles And Senile Plaques
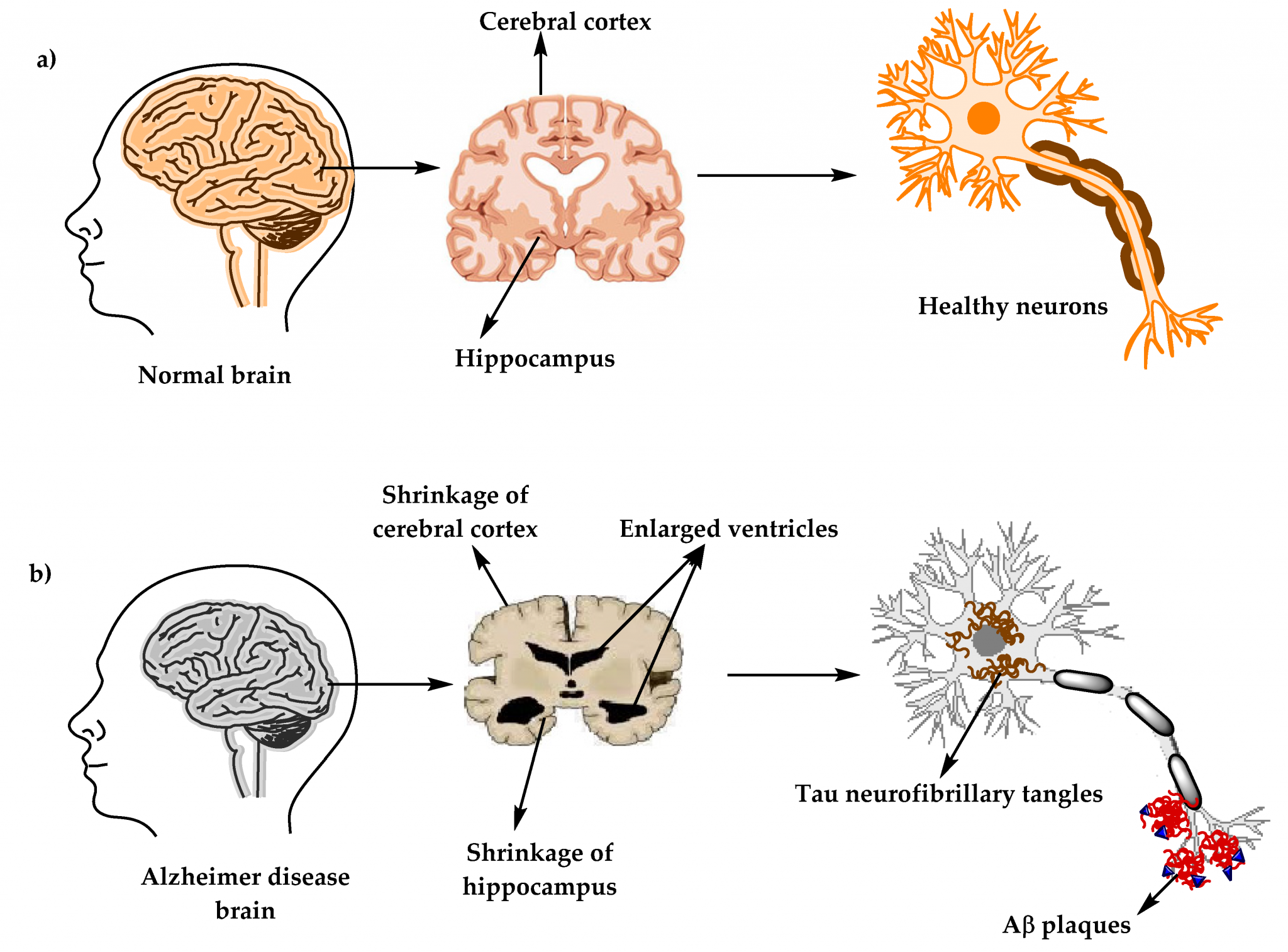
Plaques are dense, mostly insoluble deposits of protein and cellular material outside and around the neurons. Plaques are made of beta-amyloid , a protein fragment snipped from a larger protein called amyloid precursor protein . These fragments clump together and are mixed with other molecules, neurons, and non-nerve cells .
In AD, plaques develop in the hippocampus, a structure deep in the brain that helps to encode memories, and in other areas of the cerebral cortex that are used in thinking and making decisions. Plaques may begin to develop as early as the fifth decade of life. Whether Ab plaques themselves cause AD or whether they are a by-product of the AD process is still unknown. It is known that changes in APP structure can cause a rare, inherited form of AD.
Tangles are insoluble twisted fibers that build up inside the nerve cell. Although many older people develop some plaques and tangles, the brains of people with AD have them to a greater extent, especially in certain regions of the brain that are important in memory. There are likely to be significant age-related differences in the extent to which the presence of plaques and tangles are indicative of the presence of dementia.
SPs also accumulate primarily in association cortices and in the hippocampus. Plaques and tangles have relatively discrete and stereotypical patterns of laminar distribution in the cerebral cortex, which indicate predominant involvement of corticocortical connections.
Coping With A Diagnosis
A diagnosis of Alzheimers disease is the last thing anyone wants to hear. While it is undoubtedly a life-altering experience that will take both you and your family time to come to terms with, it doesnt mean that your life is over. Once you have a diagnosis and know what youre facing, you can start to take steps to slow the progression of the disease and ensure youre able to live your life as fully as possible for as long as possible.
Its important to give yourself time to process the myriad of emotions youre likely experiencing. Allowing yourself to feel even unpleasant emotions will allow the shock and distress of your diagnosis to eventually pass, and enable you to see a way forward. Its also important to reach out to others at this difficult time. The love and support of friends and loved ones can make a huge difference to your mood and outlook.
Similarly, pursuing activities that bring you meaning and joy can help bolster your sense of purposewhether thats engaging in favorite hobbies and interests, traveling, volunteering, or building your legacy by writing your memoirs or spending more time with your family.
You May Like: Karen Vieth Edgar Knight
Use And Costs Of Health Care And Long
Among Medicare beneficiaries with Alzheimer’s or other dementias, Blacks had the highest Medicare payments per person per year, while Whites had the lowest payments . The largest difference in payments was for hospital care, with Blacks incurring 1.7 times as much in hospital care costs as Whites .
| Race/Ethnicity | Total Medicare Payments Per Person | Hospital Care |
|---|---|---|
| 2,904 |
- Created from unpublished data from the National 5% Sample Medicare Fee-for-Service Beneficiaries for 2014.
In a study of Medicaid beneficiaries with a diagnosis of Alzheimer’s dementia that included both Medicaid and Medicare claims data, researchers found significant differences in the costs of care by race/ethnicity. These results demonstrated that Blacks had significantly higher costs of care than Whites or Hispanics, primarily due to more inpatient care and more comorbidities. These differences may be attributable to later-stage diagnosis, which may lead to higher levels of disability while receiving care delays in accessing timely primary care lack of care coordination duplication of services across providers or inequities in access to care. However, more research is needed to understand the reasons for this health care disparity.
Causes And Risk Factors
Despite its prevalence and the amount of research into the disease, theres still much about Alzheimers that remains unclear. For a long time, scientists looking for the causes of Alzheimers focused mainly on the buildup of proteins in the brainamyloid that accumulates in plaques and tau that forms tangleswhich degenerate nerve connections and gradually destroy memory and thinking.
However, new evidence suggests that many other factors may also play a role in the development of the disease, such as inflammation, immunity impairment, exposure to toxins, and changes in the way the brain handles glucose. Since women experience Alzheimers at significantly higher rates than men, its possible hormonal changes could also contribute to the disease.
With the exception of early-onset Alzheimers, the disease is most likely triggered by a combination of advancing age and genetic, environmental, and lifestyle factors.
Also Check: Alzheimer’s Color Ribbon
Where Can I Find Alzheimers Disease Communities
If youre looking for a support system, its likely that you or someone very dear to you has been diagnosed with Alzheimers disease. Or maybe youre just in the suspecting stage and want to gauge how others have navigated this very confusing and overwhelming time. Theres no one who can quite understand it and guide you like the caregivers who have been thereand those who are still in it, every day. If youre new to this world, these are the people and organizations to follow and join ranks with, so that you never quite feel alone.
A Long Road Back From Covid
Meanwhile, people like Cassandra Hernandez, the nurse, are simply trying to get better. More than a year after getting sick, she says, her brain is still foggy.
“We were at dinner and I forgot how to use a fork,” she says. “It was embarrassing.”
Even so, Hernandez says she’s improving slowly.
“Before this I was working on my master’s,” she says. “Now I can do basic math, addition and subtraction, I can read at a fifth-grade level. I’m still working hard every day.”
Hernandez has been working with Dr. Monica Verduzco-Gutierrez, chair of the department of physical medicine and rehabilitation at UT Health and director of the COVID-19 recovery clinic.
Verduzco-Gutierrez says her practice used to revolve around people recovering from strokes and traumatic brain injuries. Now she spends some days seeing only patients recovering from COVID-19.
The most common complaint is fatigue, Verduzco-Gutierrez says. But these patients also frequently experience migraine headaches, forgetfulness, dizziness and balance issues, she says.
Some of these patients may never recover fully, Verduzco-Gutierrez says. But she’s hopeful for Hernandez.
“She’s made so much improvement and I would love for her to go back to nursing,” Verduzco-Gutierrez says. “But again, we don’t know what happens with this disease.”
Also Check: How To Get A Person With Dementia To Shower
Emotion And Behavior Treatments
The emotional and behavioral changes linked with Alzheimers disease can be challenging to manage. People may increasingly experience irritability, anxiety, depression, restlessness, sleep problems, and other difficulties.
Treating the underlying causes of these changes can be helpful. Some may be side effects of medications, discomfort from other medical conditions, or problems with hearing or vision.
Identifying what triggered these behaviors and avoiding or changing these things can help people deal with the changes. Triggers may include changing environments, new caregivers, or being asked to bathe or change clothes.
It is often possible to change the environment to resolve obstacles and boost the persons comfort, security, and peace of mind.
The Alzheimers Association offer a list of helpful coping tips for caregivers.
In some cases, a doctor may recommend medications for these symptoms, such as:
- antidepressants, for low mood
develops due to the death of brain cells. It is a neurodegenerative condition, which means that the brain cell death happens over time.
In a person with Alzheimers, the brain tissue has fewer and fewer nerve cells and connections, and tiny deposits, known as plaques and tangles, build up on the nerve tissue.
Plaques develop between the dying brain cells. They are made from a protein known as beta-amyloid. The tangles, meanwhile, occur within the nerve cells. They are made from another protein, called tau.
- aging
The Brain And Body Connection
Though the cause of Alzheimerâs is not known, doctors think the symptoms of the disease are caused by a buildup of harmful proteins in your brain called amyloid and tau. These proteins form large clumps, called tangles and plaques. They get in the way of normal brain function and kill healthy cells.
The damage usually starts in the area of your brain that forms memories. People with early-stage Alzheimer’s disease often have trouble remembering things. As the disease gets worse, the plaques and clusters also appear in the parts of the brain in charge of bodily behaviors.
Everyday activities like walking, eating, going to the bathroom, and talking become harder.
The effects of the disease will differ for each person as it gets worse. The pace can be slow. Some people live up to 20 years after a diagnosis. The average life expectancy, though, is 4 to 8 years.
You May Like: Bobby Knight Health Update