Ways To Ease Sundowner Syndrome Symptoms
Mood swings, restlessness, and confusion are all potential signs that your loved one has Sun downs Syndrome, a group of symptoms seen in over 20% of patients with Alzheimers disease.
Coping with Sun Downs Syndrome symptoms can be a challenge, but there are some non-medical ways to alleviate the symptoms and give your loved one the support they need.
What Causes Sundowners Syndrome
Some studies suggest that as many as 20% of Alzheimer’s patients experience worsening confusion, agitation, and anxiety beginning in the afternoon or evening. Again, doctors do not fully understand sundowners syndrome or its causes, but some potential triggers have been identified. Research suggests that contributing factors may include the following:
- Sensory deprivation or overload
- Unmet physical needs
- Limited mobility or social isolation
- Increased stress levels
- Unfamiliar environment or unexpected change
- Disrupted circadian rhythm, sleep deprivation
Is it Sundowners Syndrome or Delirium?
When it comes to treating and managing sundowning symptoms, the first step is to confirm that it is, in fact, sundowners syndrome and not delirium. Delirium is a medical condition that results in mental confusion and changes in attention span, perception, mood, and activity level. Though delirium is a stand-alone medical condition, people with dementia are highly susceptible to it.
The best way to tell whether your loved one is suffering from delirium or sundowners syndrome is to look at the timing. Delirium sets in quickly over the course of days or weeks rather than months or years, and its associated confusion may fluctuate throughout the day instead of along a predictable late-afternoon or early-evening timeline.
What Triggers Sundown Syndrome
While the cause is unknown, researchers suggest several possible triggers:
- End-of-day activityA flurry of activity toward the end of the day may lead to anxiety and confusion.
- FatigueEnd-of-day exhaustion, or a lack of things to do late in the day, may also be a contributor.
- Low lightAs the sun goes down, the quality of available light may diminish and shadows may increase, making it more difficult for someone with poor eyesight to see. This may increase confusion and agitation.
- Internal imbalanceHormonal imbalances or possible disruptions in the internal biological clock, which regulates cognition between waking and sleeping hours, may;trigger sundowning.
- WinterIn some cases, the onset of winters shorter days amplifies sundowning.;Seasonal affective disorder, a common depression associated with shorter hours of daylight, may also exacerbate sundowning.
- Infection.;In older adults, a urinary tract infection may cause symptoms similar to those of sundowning.
Read Also: Will Meredith Get Alzheimer’s
Causes Of Sundown Syndrome
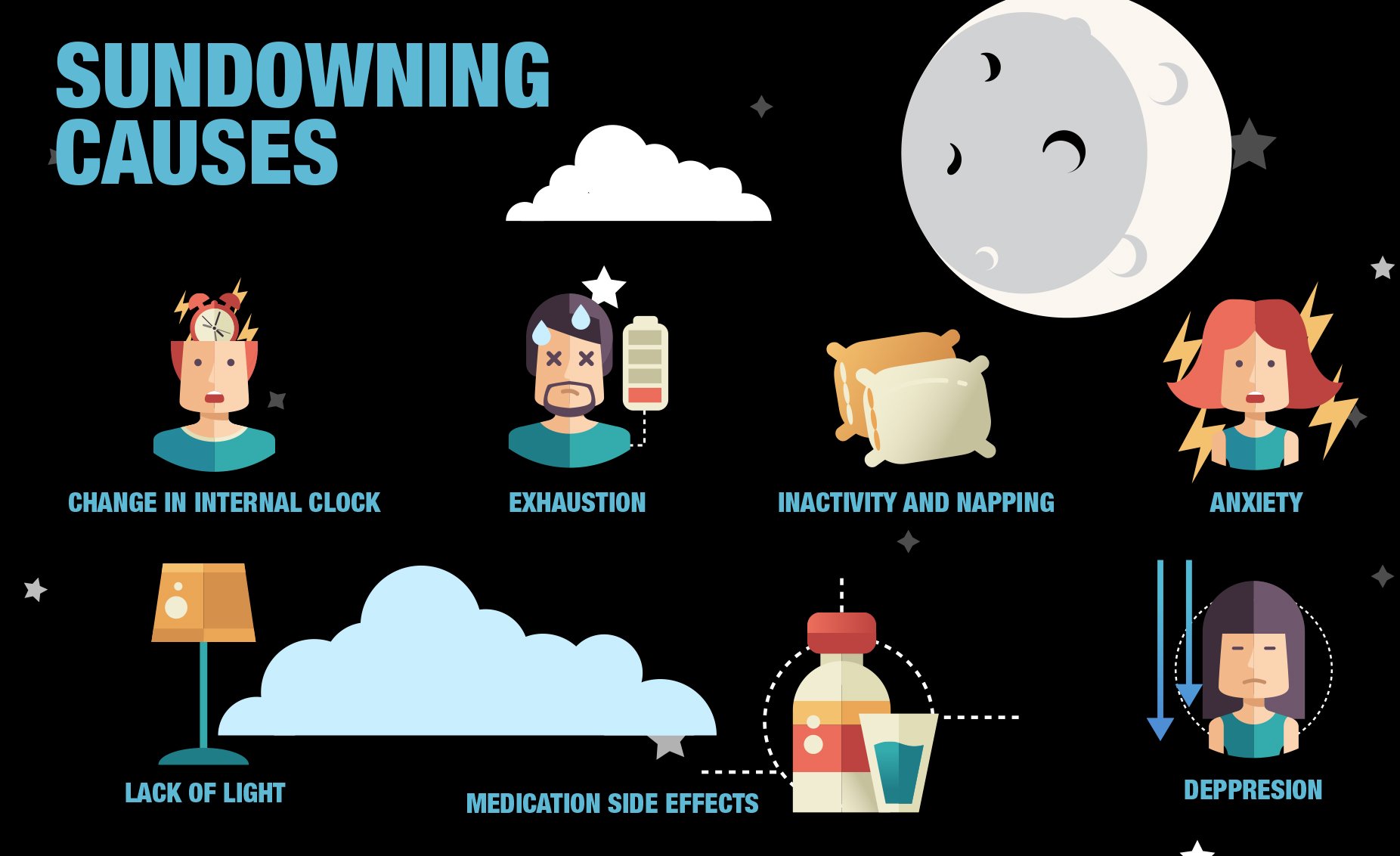
The exact cause of Sundown Syndrome is unknown and will be unique for each individual, but likely triggers of the behavior change include:
- Hunger
- A drop in blood pressure that happens after eating
- Low lighting – Patients with vision problems combined with the change in lighting that happens as the sun goes down may cause more challenges.
- Fatigue
- Caregivers become tired at the end of the day
- Flurry of activity that can happen when caregivers change over at the end of day
- Hormone changes related to internal biological clock imbalance
- Season changes – Seasonal Affective Disorder caused by less exposure to natural sunlight
At Sundown The Demons Get Riled Up
Many people enjoy the sunset. Sunsets are picturesque, and they usher in the beginning of evening after a day of labor. Families congregate in the early evening around dinner, chatting and sharing in their daytime activities. For the most part, we look forward to sunsets that transition us from our relatively hectic daytime goings-on to unwinding with family, dinner and subdued pastimes or hobbies, before eventually relaxing into sleep.
It is naturally not so for those who experience sundown syndrome. For them, sunsets and the evening hours can be associated with heightened dread and scorching anxiety, as opposed to the calm and relief many of us feel.
Sundowning syndrome throughout the day
Also Check: Dementia Ribbon Color
Other Sleep Issues In People With Dementia
Sundowning is a phenomenon in which individuals with dementia experience increased agitation later in the day and in the evening. The symptoms of sundowning include confusion, anxiety, wandering, and yelling. Sundowning can contribute to insomnia and other sleep problems when these behaviors continue into the night. Possible causes of sundowning include the circadian rhythm changes that occur in dementia, as well as fatigue, depression, and pain.
People with dementia may also talk, yell, or cry out at night if they cannot sleep. Some dementia patients have a tendency to wander away from their homes, which can be especially dangerous at night. In dementia patients with REM sleep behavior disorder, shouting, grabbing, jumping, and other behaviors are related to dream enactment during sleep.
You May Like: What Is The Color For Dementia
Tips For Preventing Sundowning
There are a number of steps that you can take to prevent sundowning. Because there are many factors that contribute to sundowning, not all of these tips will work for everyone. It is best to keep a record of what does and does not work for your relative.
Mutsai suggested the following tips for trying to prevent sundowning.
Read Also: Is Senility The Same As Dementia
Excessive Sleep In Elderly
When you are caring for an elderly person, you may get concerned when they start sleeping too much. As we age, sleep becomes lighter and we may be awakened by aching joints or the need to use a restroom.
Most seniors will usually compensate this with a nap during the day, which is quite normal. Sleeping in the day becomes an issue when the person seems to be sleeping most of the time instead of interacting with people.
If such a thing happens, you need to find out whether there are any reasons that are causing this. You may need the help of a doctor for this.
What Is Sundowner Syndrome
Sun Downs Syndrome commonly affects people with Alzheimers disease, dementia, or other cognitive impairments. If your loved one has Sun Downs Syndrome, they may show changes in their usual behaviour from late afternoon and into the early evening and night, including signs of confusion and agitation, or erratic behavior.
Because sundowning symptoms may point to a progression from early stages of Alzheimers disease to more serious deterioration of cognitive function, its important to let your loved ones doctor know about it sooner rather than later.
According to the Mayo Clinic, doctors and researchers still dont know what causes Sun Downs Syndrome, however you can easily identify the signs and symptoms of a person who has sundowning symptoms and take proactive steps to ease their symptoms
Recommended Reading: What’s The Difference Between Dementia And Alzheimer’s And Senility
What Should I Do If A Person With Dementia Is Sleeping A Lot
If the person is in the later stages;of dementia;and they have gradually started sleeping more and more, it is likely to be due to the dementia progressing.;;
However, if the excessive;sleeping has started more suddenly, or the person doesnt seem well in other ways, it may have another cause.;;
If this is the case you should speak to the GP, to rule out any infections or conditions that could be having an impact.
It may also be worth asking for a medication review with the GP or speaking to a pharmacist as medication can cause a range of side effects.;
If the person is sleeping a lot but it isnt having a negative impact on;them;it is often best to just go with it;and make sure they are comfortable.;
Also Check: Does Medicare Cover Nursing Home For Dementia
Tips For Coping With Sundowners Syndrome
As the sun begins to set, have you noticed changes in a loved ones behavior? For those living with Alzheimers disease;and other forms of dementia, its not uncommon to experience unpredictable agitation and confusion during this time of day.
Sundowners syndrome, also called sundowning or late-day confusion, is a group of symptoms that occur in someone with memory loss that can start around late afternoon and continue into the night. It can cause increased confusion, disorientation, anxiety, agitation, pacing and even wandering.
We know that most people living with dementia will experience behavioral symptoms during the course of their disease, particularly during the moderate stage of Alzheimers disease and earlier in other types of dementia, said Lori Nisson, a licensed clinical social worker and Family and Community services director at Banner Alzheimers Institute and Banner Sun Health Research Institute. They are working much harder to complete tasks and activities that used to come easily to them, so they are expending more energy and can wear out easily as the day progresses.
While there is no one explanation for its cause, factors that typically trigger changes in behavior include fatigue, disruption to the sleep cycle, boredom, restlessness or unmet needs, such as hunger, thirst or the need to use the restroom.
Recommended Reading: Difference Between Senility And Dementia
Shining A Light On Sundowning: Many Alzheimers Patients Experience Strong Mood Swings Late In The Day
Growing up, Emily German looked up to her mother as a fierce role model who effortlessly juggled family, friends and a successful career. demn
In the 1980s and ’90s, Linda Larsen German had worked her way up the corporate ladder in Manhattan, helping to grow the Liz Claiborne business into a Fortune 500 company before leaving to start her own ventures. She was a natural-born leader with a quick mind.
“She was such a tough, powerful, strong woman. That is 100 percent how I viewed her my entire life,” said Emily, 24, a software sales representative who lives in New Orleans. “It was really because of my mom’s bright personality that we caught on to her disease so quickly.”
In 2012, Emily and other family members noticed a shift in Linda’s behavior. At age 61, she began to show uncharacteristic signs of confusion, agitation and restlessness. Once Emily flew home to New York for a college winter break. She says she remembers her mother spending an hour searching for her parked car at the airport. They laughed it off at the time, but these “funny” instances became more frequent.
A year or so later, she witnessed her mother get frustrated and confused at the grocery store, snapping rudely at the cashier – something she wouldn’t ordinarily do. The shock of seeing her erratic behavior was enough to lead Emily and her father to make a doctor’s appointment for Linda.
In early 2014, at age 62, Linda was diagnosed with early-onset Alzheimer’s disease.
Creating A Safe And Comfortable Sleeping Environment

An individuals sleeping area should be as comfortable as possible.
This should include ensuring the bedroom has comfortable temperatures.
To INCREASE safety, caregivers can offer nightlights and make sure that window and door locks are secure.
Motion detectors and door sensors can alert loved ones when a person with dementia is wandering.
Read Also: Does Meredith Grey Have Alzheimer’s
Causes And Symptoms Of Sundowning
The exact cause of sundowning is still unclear, but researchers speculate there are many factors involved. Some of these factors are extreme fatigue, hunger or thirst, depression, pain, boredom, or sleep problems.
Triggers of sundowning symptoms may include less light and more shadows in the house, which can lead to confusion and fear, or trouble separating dreams from reality, which can lead to disorientation.
Symptoms of sundowning include:
- Mood swings
Tau: A Direct Driver Of Cognitive Decline
In the study, Dr. Grinberg and the team analyzed the brains of 13 deceased people who had Alzheimers disease, as well as those of seven deceased individuals who had not experienced clinical neurodegeneration. The researchers obtained these samples from UCSFs Neurodegenerative Disease Brain Bank.
The team found that, in comparison with healthy brains, those affected by Alzheimers disease had a high level of tau across three regions that are key to staying awake, namely the locus coeruleus, the lateral hypothalamic area, and the tuberomammillary nucleus. Not only this, but these regions had actually lost 75% of their neurons.
Its remarkable because its not just a single brain nucleus thats degenerating, but the whole wakefulness-promoting network, notes the studys lead author, Jun Oh.
Crucially, this means that the brain has no way to compensate because all of these functionally related cell types are being destroyed at the same time, Oh explains.
For further clarification, the researchers went on to conduct a postmortem analysis of brain samples from seven people who had progressive supranuclear palsy and corticobasal disease. These are two forms of dementia that are characterized specifically by the overaccumulation of tau protein.
In these samples, the scientists did not find the same loss of neurons in areas connected with states of wakefulness, which suggests that this destructive loss may only occur in Alzheimers disease.
Don’t Miss: Dementia Picking At Skin
Factors That Aggravate Sundowning
Because individuals with Alzheimers or other forms of dementia can become easily disoriented, they are often more susceptible to sundowning and the challenging behaviors associated with it. While the exact cause of sundowning is unknown, some factors tend to worsen symptoms. These aggravating factors can include:
- Lack of sleep, fatigue, or mental exhaustion
- Caffeine and alcohol close to bedtime
- Faded light, low light, and increased shadows that cause confusion and fear
- Upset in their circadian rhythms, confusing day and night
- Underlying health issues, such as an infection, discomfort, or pain
- Stress, depression, or boredom
Sundowning Signs And Symptoms
The medical community reminds us that the difference between a sign and a symptom is that your doctor can detect a sign, such as the very first flicker of memory loss or confusion, whereas you tell the doctor what symptoms you have experienced, for example being unsteady on your feet, or enduring frequent headaches.
The symptoms of sundowning are as follows:
- Mood swings, paranoia; delusions of being watched, a suspicious deportment
- Disorientation, insecurity, and being argumentative and demanding
- Becoming combative or aggressive, hurling insults, and occasionally lashing out at caregivers
Read Also: Does Andrea Mitchell Have Dementia
Common Sleep Problems In People With Dementia
Sleep changes are common in older adults with and without dementia. Many seniors experience changes in the quality of their sleep, the number of hours they sleep, and how much time they spend awake at night. In fact, older adults;total sleep time decreases;by about 30 minutes per decade starting in middle age.
Sleep problems are even more common in people with dementia. The type and severity of sleep disturbances may vary depending on the;cause of your loved ones dementia;and the;stage of their disease. Sleep problems associated with dementia tend to get worse as the disease progresses.
Your loved one with dementia may experience the following sleep problems:
- Difficulty maintaining or falling asleep, which can be caused by;insomnia, problems with the sleep cycle, side effects of medication, or other factors.
- Sundown syndrome, which is common in people with Alzheimers and other forms of dementia, can contribute to problems with sleep.;Sundown syndrome;refers to increased confusion, agitation, anxiety, and aggression in the evening or during the night.
- Problems with movement during sleep, such as restless legs syndrome which is characterized by an uncomfortable urge to move the legs during periods of rest or rapid eye movement sleep behavior disorder, which makes people act out their dreams.
- Breathing disorders during sleep, such as sleep apnea, which affects about;50% of people with Alzheimers.
You May Like: Ribbon Color For Dementia
Sleep Aids: Medications Melatonin And Dementia
In some cases, the doctor may prescribe medications to help your loved one sleep. However, older adults with cognitive impairment are more likely to experience side effects from sleep-inducing drugs, so those medications arent usually recommended for long-term use.
Some studies show melatonin may improve sleep in people with mild to moderate dementia. It may also help reduce agitation and confusion late in the day. Check with your loved ones doctor before starting any over-the-counter supplements or sleep aids.
Recommended Reading: What Is Vascular Dementia Life Expectancy
How Can We Support You
Sundowning delirium can be a painful, exhausting and troubling experience for caregivers. No one likes to see a loved one suffer. It is a troubling and common problem of middle-stage Alzheimers disease.
No one is sure why the transition period from light to dark is so disturbing. There are several steps you can take to reduce upsetting behavior. Keeping to a routine and encouraging good sleep patterns contribute to symptom relief.
Dont let sundowning behavior overwhelm you. Talk to others and avoid caregiver isolation.;There are many other people also experiencing the same thing.
We offer custom-tailored programs of care to assist caregivers and give them a much-needed break.;Contact us today to schedule a tour.
Responding To Sundowning As It Happens

Just as you have tools when loved ones are agitated or fixed on something at other times of the day, you have tools to help them settle down and relax when sundowning.
- Listen carefully. It can be difficult to identify the source of their fear or agitation, but keep listening and try different things to help them calm down. For instance, they may see someone in the room, but maybe it is the shadow created by the light outside the window.
- Redirect where possible. Is it almost time for dinner? Go ahead and eat. Does your loved one like to fold the laundry? Find some, even the laundry that is already folded and in the closet. Pull it out to start all over again. Towels and napkins are always useful for this activity. If it is after dinner and a good night for a walk, go out. Sometimes a TV or a radio program can be a good method to redirect and take their mind off things that are bothering them. Just be careful about the images on the screen.
- Use gentle touch to connect. Hold their hand, stroke their back, hug them. Such touch will be soothing, and may be just what they need.
References
1. Kahchiyants, N. et al . Sundown Syndrome in Persons with Dementia: An Update. Psychiatry Investigation, pp. 275-287.
Resources
Recommended Reading: What Is The Color For Dementia