What Causes Combative Behavior In Alzheimers
Combativeness can be caused by many factors including physical discomfort, environmental factors and poor communication. If the person you are caring for is exhibiting combativeness, consider the following:
Physical Discomfort
- Is the person tired because of inadequate rest or sleep?
- Are medications causing side effects?
- Is the person unable to let you know he or she is experiencing pain?
Environmental Factors
- Is the person over stimulated by loud noises, an overactive environment or physical clutter?
- Does the person feel lost or abandoned?
Poor Communication
- Are you asking too many questions or making too many statements at once?
- Are your instructions simple and easy to understand?
- Is the person picking up on your own stress and irritability?
- Are you being negative or critical?
Treatments How To Stop Skin Picking
You may have tried to stop skin picking on your own many times, but failed. Perhaps you try to conceal your condition by picking only areas that you can cover with clothing. You spend considerable amounts of time in isolation engaging in compulsive picking sessions. You cannot get past the intense urges and anxiety associated with the disorder without professional help. Effective treatment for skin picking is available:
You may also find it helpful to join a support group that focuses on helping people refrain from picking at their skin. The International OCD Foundation has an online search tool you can use to locate a support group in your area. If you’d rather participate in an online support group, they include an online and phone support group listing as well.
Quick tips to stop skin picking:
These tips on how to stop picking at skin can help you with your disorder after you’ve gotten help from a professional. Employ these tips in addition to any medication or CBT therapy tools you’ve learned.
Treating Compulsive Nose Picking
The following treatment approaches may be helpful for people whose nose picking is a nervous or compulsive habit:
- mindfulness meditation, which can help reduce the stress and anxiety that can promote compulsive behaviors
- habit reversal training, which helps people become aware of and interrupt their habitual behaviors
- cognitive behavioral therapy, which helps people identify negative thinking and behavior patterns and develop more adaptive responses
Like adults, children may pick their nose to remove uncomfortable or irritating boogers. They may also pick their nose out of boredom or as a way of exploring their bodies.
Young children also may not have internalized societys disapproval of nose picking.
It is not necessary to make a child feel ashamed or bad about themselves for picking their nose. However, the following tips can help discourage a child from nose picking:
- Provide gentle yet firm reminders that it is not OK for a person to pick their nose in public.
- Encourage children to blow their nose into a tissue, instead of picking the nose.
- Tell children to wash their hands after seeing them pick their nose.
- Use methods to keep the childs nasal passages moist.
Don’t Miss: Can Bpd Lead To Dementia
Apply Turmeric On The Affected Area
Tumeric is a natural anti-inflammatory and anti-coagulant that can be found in your nearest grocery store. To heal picked skin fast, form a paste of turmeric and water, and apply on the affected area of your loved one. Apply on areas with the most number of skin picking cuts and wounds.
Before you go ahead with this, I have to warn you that turmeric has a bright yellow color and it can form stains on your loved ones clothes or the bedding.
Kindly, cover the entire bed or chair with a plastic sheet.
Numerous studies have proved the effectiveness of this natural herb. Tumeric contains a curcuminoid known as Curcumin. This is what gives it a natural yellow color.;
According to a study by the University of Sydney, Curcumin works as an anti-inflammatory, anti-oxidant, anti-carcinogenic, anti-mutagenic, anticoagulant, and the anti-infective agent when applied on picked skin.
You Compulsively Pick At Your Fingers
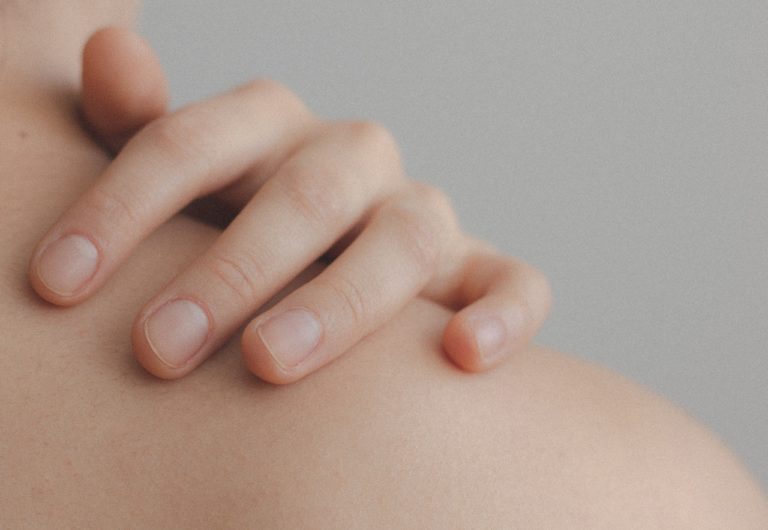
Picked nails, scabs on thumbs and fingers, bleeding, and lacerations around cuticles are a telltale sign of skin picking disorder.
It is not uncommon for people with excoriation disorder to target their fingernails and cuticles as a site for picking, says GinaMarie Guarino, Licensed Mental Health Counselor , a therapist with a history of working with people who are in treatment for excoriation disorder.
Fingernails and cuticles tend to be a prime location, Guarino says, as the skin can sometimes flake, and nails can split, making them easy to pick at. It is also a location that can be picked subtly, without too many people noticing the act of picking.
Don’t Miss: How To Prevent Alzheimer’s And Parkinson’s
How Do I Know If I Have Dermatillomania
If you have the occasional urge to pick at a scab, it doesnt always mean you have dermatillomania. However, if you find that you want to stop picking at scabs but seem unable to do so, you may be experiencing this disorder.
The next time you find yourself picking at a scab, try to take a moment to assess how youre feeling. Do you feel stressed, anxious, or on edge? How do you feel while youre picking at the scab? What about afterward?
It might be helpful to keep track of these feelings and urges on paper. If you find that your picking is usually triggered by some kind of stress or brings on a sense of relief, you may have dermatillomania.
There are some things you can try on your own to break the habit of picking at your scabs. Most of these focus on keeping your hands and mind busy.
The next timed you feel the urge to pick or find yourself unconsciously picking, try:
- popping bubble wrap
- going for a quick walk around the block
- meditating
- using fidget cubes or spinners
- squeezing a stress ball
- talking to a close friend or family member about what youre feeling in that moment
There are also things you can do to reduce the temptation to pick, such as:
- making a conscious effort to protect your skin from minor cuts and scabs whenever possible
- throwing away tweezers or other tools you might use to pick at scabs
- placing lotion on scabs to relieve itching
- placing bandage over the scab
- wearing clothing that covers the scab
Compulsive Skin Picking In The Elderly
Caring for an elderly loved one comes with many challenges. One of the greatest emotional hurdles faced by caregivers is feeling powerless when faced with a problem they dont know how to address. A question that often comes up in the AgingCare.com Support Groups is about compulsive skin picking. A number of caregivers have expressed concern about the tendency for their loved one to repetitively pick or scratch their skin to the extent that it causes damage and even injury. Thinning skin and decreased healing capabilities exacerbate the problem, as there is greater risk for the development of open wounds and infection.
Also Check: When Did Alzheimer’s Become A Diagnosis
Tips For Preparing For Emergencies
- Keep a list of emergency phone numbers of the local police and fire departments, hospitals, and poison control as well as the Safe Return 24/7 incident line 1-800-572-1122
- Keep a list of physicians phone numbers and current medications
- Keep copies of legal documents
- Check fire extinguishers and smoke alarms, and conduct fire drills regularly
How Can I Recognise When A Person With Dementia Is Experiencing Difficulties With Their Perception
It can be difficult to know when a person with a diagnosis of dementia is experiencing perceptual difficulties or hallucinations. Signs that this might be happening include:
- saying or doing things that suggest they see or hear things that you cant
- bumping into things or frequent trips and falls, as though they are struggling to see the objects around them
- not recognising where they are
- displaying changes in behaviour that may indicate fear or distress
- becoming more socially isolated
- reacting to, or looking startled by, things that you cant see
- muttering under their breath, or speaking as if in answer to something you cannot hear
- plucking or picking at their skin as if they itch
Recommended Reading: How To Deal With Someone With Dementia
How Is Childhood Alzheimers Diagnosed
It can take years to be diagnosed with one of the medical conditions associated with the term childhood Alzheimers. These diseases are very rare, so a child may be diagnosed with other, more common conditions first.
Its important to take your child to regular wellness checkups so that their developmental progress can be monitored, and any delays can be identified as early as possible.
For example, since the early symptoms often affect learning and motor skills, children are sometimes incorrectly diagnosed with learning disabilities, autism, or other developmental disorders.
However, unlike more common conditions, children with NPC or MPS III will develop more symptoms over time as their conditions worsen.
Eventually, theyll develop symptoms that cant be explained by their previous diagnosis. This often prompts parents to seek out a new, correct diagnosis.
Children with these conditions often need genetic testing before they get a diagnosis. They might need to visit specialists before there are answers about their condition. Fortunately, testing is getting easier.
Children suspected of having NPC or MPS III used to need biopsies to confirm the condition. Recent developments have allowed for a diagnosis with a standard blood test.
What Is Wandering In Dementia
Persons with dementia have varied movement patterns and trying to identify what qualifies as;wandering can be difficult for a caregiver as well as for professionals. Many people with dementia do not fit the textbook definition of wandering, To move about without a definite destination or purpose. In fact, persons with dementia may have a definite purpose for their actions.
The working definition that best describes wandering is, aimless or purposeful motor activity that causes a social problem such as getting lost, leaving a safe environment or intruding in inappropriate places.
Read Also: How To Keep Dementia Patients In Bed At Night
How Is Childhood Alzheimers Treated
Theres no cure for either type of childhood Alzheimers, and there have been no proven treatments.
Since there are no treatments for this disease itself, a plan of care will likely focus on the symptoms and making sure the child has the highest possible quality of life.
For example, if a child is having trouble swallowing due to childhood Alzheimers, they might benefit from a special diet of food that has been chopped up or pureed for for easier swallowing.
Other professionals, such as physical and occupational therapists, can help with balance, motor skills, and muscle weakness. Speech therapists can help teach them to safely swallow foods and liquids.
Wandering Outdoors With Alzheimer’s

About 125,000 affected adults wander away from their Alzheimer’s caregivers every year, with potentially serious consequences to senior health. One way to combat this is to put special sensor alarms on doors and windows or make doors harder to open with childproof knobs. Also invest in an ID bracelet, GPS-tracked phone, or a Project Lifesaver device, which can track a wanderer. Consider creating a securely fenced-in area around the home where your loved one can safely enjoy the outdoors, a boon for senior health.
You May Like: Can Diet Soda Cause Dementia
What Are The Signs Of Skin Picking Disorder
It’s hard to say exactly when skin picking changes from a mild, nervous habit to a serious problem that needs treatment. It may help to ask the following questions:
- Does picking at your skin take up a lot of time during the day?
- Do you have noticeable scars from skin picking?
- Do you feel upset when you think about how much you pick your skin?
- Does picking at your skin get in the way of your social or professional life? For example, do you avoid the beach or the gym because people might see your scars? Or do you spend a lot of time covering up sores before work or social events?
Sleeplessness And Sundowning In Alzheimers Patients
Sleeping problems experienced by individuals with Alzheimers and caregiver exhaustion are two of the most common reasons people with Alzheimers are eventually placed in nursing homes. Some studies indicate that as many as 20 percent of persons with Alzheimers will, at some point, experience periods of increased confusion, anxiety, agitation and disorientation beginning at dusk and continuing throughout the night.
While experts are not certain how or why these behaviors occur, many attribute them to late-day;confusion, or sundowning, caused by the following factors:
- End-of-day exhaustion
- An upset in the internal body clock, causing a biological mix-up between day and night
- Reduced lighting and increased shadows
- Disorientation due to the inability to separate dreams from reality when sleeping
- Less need for sleep, which is common among older adults
To learn more about sundowning, read Caring for Alzheimers Patients with Sundowning Symptoms.
Tips for reducing evening agitation and nighttime sleeplessness
Nighttime restlessness doesnt last forever. It typically peaks in the middle stages, then diminishes as the disease progresses. In the meantime, caregivers should make sure their home is safe and secure, especially if the person with Alzheimers wanders. Restrict access to certain rooms or levels by closing and locking doors, and install tall safety gates between rooms. Door sensors and motion detectors can be used to alert family members when a person is wandering.
Don’t Miss: Why Does Uti Cause Dementia In Elderly
List Of Strategies For Skin
;At one of The TLC Foundation for Body-Focused Repetitive Behaviors’ events, I was lucky to be a part of a small group of skin-pickers who met daily with Charlie Mansueto,;PhD, Suzanne Mouton-Odum,;PhD, and Sherrie Vavrichek, LCSW. We reviewed the Comprehensive Model for Behavioral Management of BFRBs . As we discussed strategies for interrupting and preventing skin-picking behaviors, I made a list of strategies I’m using, and strategies I could use.
At one of The TLC Foundation for Body-Focused Repetitive Behaviors’ events, I was lucky to be a part of a small group of skin-pickers who met daily with Charlie Mansueto, PhD, Suzanne Mouton-Odum, PhD, and Sherrie Vavrichek, LCSW. We reviewed the Comprehensive Model for Behavioral Management of BFRBs . As we discussed strategies for interrupting and preventing skin-picking behaviors, I made a list of strategies I’m using, and strategies I could use.The COMB model has 5 categories , so my notes are divided into sections:
SensoryMotorPlace / environment
Writing this out has been really fun! It’s also powerful to notice that I’ve incorporated nearly 50 practices into my daily routine. I’m really making this a priority, and it’s good to notice that it’s working! My picking is dramatically reduced from 3 years ago, when I was doing only 2 or 3 of the strategies.
SENSORY Strategies I’m Using
SENSORY Strategies I could try
COGNITIVE Strategies I’m Using
These are things I say to myself, to help prevent and resist urges:
Practical Tips On Preventing Perceptual Difficulties And Hallucinations
Ways to avoid visual misperceptions and hallucinations
- Take the person for regular eyesight tests
- If they wear glasses, make sure theyre clean
- Cover mirrors or turn them around to face the wall. People with dementia can misinterpret reflections as other people in the house
- Move other objects that could be mistaken for a person; for example, coat stands, dressing gowns or coats hung on doors
- Prevent reflections from windows with blinds or curtains
- Avoid busy patterns on carpets or tiles, and, if possible, try to avoid changes in the levels of the floor, such as from thick carpet to bare floor, which might be difficult for a person with dementia to see
- Make sure rooms are well lit
- Use contrasting colours to help the person with dementia; for instance, bright, block colour plates help food stand out; brightly coloured towels are easier to see against the wall; a vivid coloured toilet seat is easier to see against the backdrop of the bathroom
Ways to avoid auditory misperceptions and hallucinations
- Take the person for regular hearing tests
- If they wear a hearing aid, make sure its cleaned and maintained, and the battery is checked regularly
- Speak slowly and calmly to the person
- Face them when speaking
- Turn off background noise such as the TV and radio when speaking to them
Ways to avoid taste misperceptions and hallucinations
Ways to avoid sense of touch misperceptions and hallucinations
Ways to avoid sense of smell misperceptions and hallucinations
You May Like: How Quickly Does Dementia Come On
Itscommon But It Takes A Toll
If you have this problem,youre not alone, but its likely that you;spend more time alone;ifyou have SPD. If youre like many sufferers, you may have visible sores andeven scars from skin-picking behavior.
So you have a secret. And keeping that secret can lead you to isolate yourself from others. This can increase;depression;and;anxiety, which creates a vicious cycle by triggering the urge to pick, Dr. Darling says.
Most people who sufferfrom the disorder do not talk about it, and they rarely seek medical carebecause healthcare providers and loved ones often tell them to just stop,she says. They are very good at hiding the disorder because of shame andembarrassment.
Whats most important is theunderstanding that, with time and effort, it is possible to overcome thebehavior. For anyone who thinks they have SPD, Dr. Darling offers these tips:
Agitation In Alzheimer’s Patients
Many times, Alzheimer’s caregivers are faced with their loved one’s inexplicable, intractable agitation, a common Alzheimer’s symptom. Knowing their history might provide clues. For example, a woman who once eagerly anticipated her husband’s arrival home from work each day might calm down if you talk to her about how good it felt for him to arrive and reassure her that her husband will be home soon. If he is deceased, there’s no reason to mention that, Rubinstein says.
You May Like: Can Infections Cause Alzheimer’s Disease