Brain Changes Evident In Scans Before Memory Cognitive Decline
- Date:
- Washington University School of Medicine
- Summary:
- Doctors may one day be able to gauge a patient’s risk of dementia with an MRI scan, according to a new study. Using a new technique for analyzing MRI data, researchers were able to predict who would experience cognitive decline with 89 percent accuracy.
One day, MRI brain scans may help predict whether older people will develop dementia, new research suggests.
In a small study, MRI brain scans predicted with 89 percent accuracy who would go on to develop dementia within three years, according to research at Washington University School of Medicine in St. Louis and the University of California San Francisco.
The findings, presented Sunday, Nov. 25 at the Radiological Society of North America meeting in Chicago, suggest that doctors may one day be able to use widely available tests to tell people their risk of developing dementia before symptoms arise.
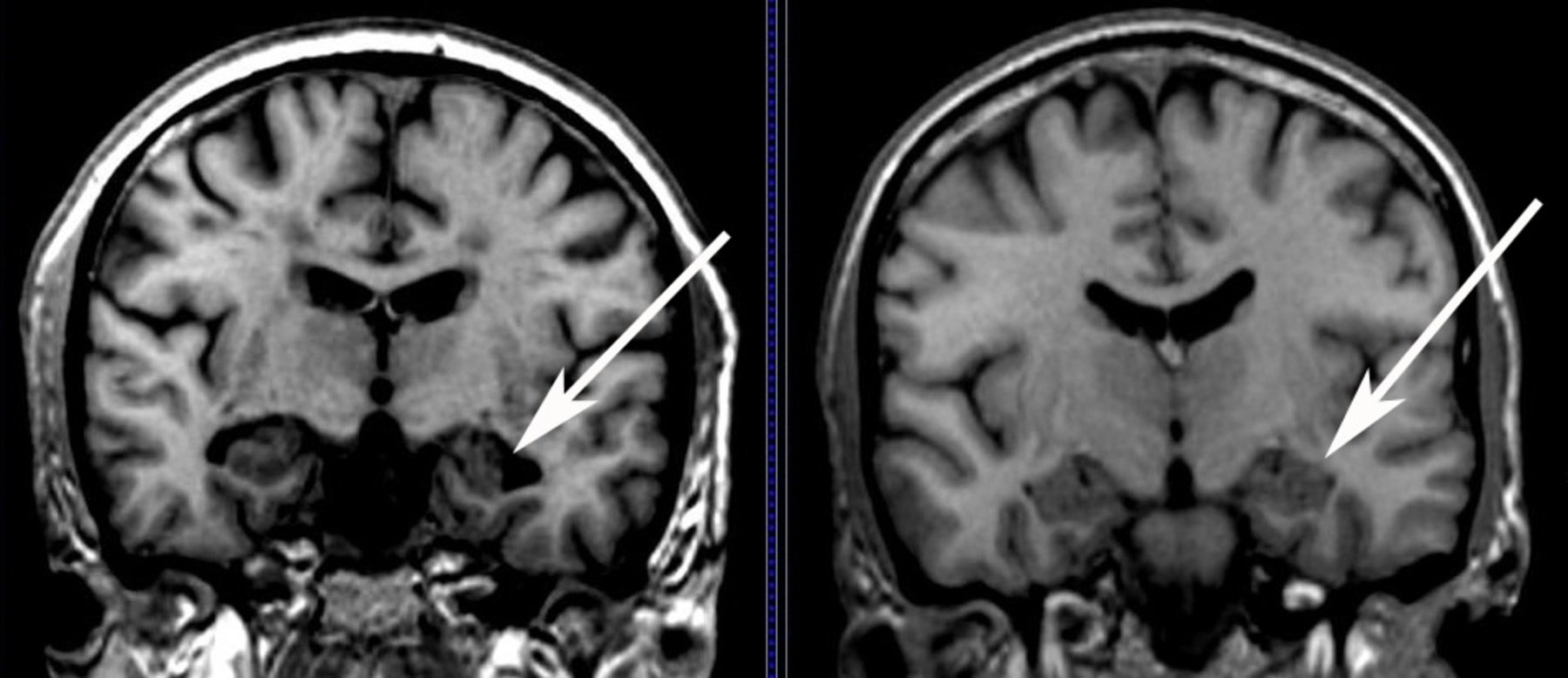
“Right now it’s hard to say whether an older person with normal cognition or mild cognitive impairment is likely to develop dementia,” said lead author Cyrus A. Raji, MD, PhD, an assistant professor of radiology at Washington University’s Mallinckrodt Institute of Radiology. “We showed that a single MRI scan can predict dementia on average 2.6 years before memory loss is clinically detectable, which could help doctors advise and care for their patients.”
Story Source:
Cite This Page:
Frederik Barkhof Marieke Hazewinkel Maja Binnewijzend And Robin Smithuis
Alzheimer Centre and Image Analysis Centre, Vrije Universiteit Medical Center, Amsterdam and the Rijnland Hospital, Leiderdorp, The Netherlands
Publicationdate 2012-01-09
This review is based on a presentation given by Frederik Barkhof at the Neuroradiology teaching course for the Dutch Radiology Society and was adapted for the Radiology Assistant by Robin Smithuis.First publication: 1-3-2007.Updated version: 9-1-2012.This presentation will focus on the role of MRI in the diagnosis of dementia and related diseases.We will discuss the following subjects:
- Systematic assessment of MR in dementia
- MR protocol for dementia
- Typical findings in the most common dementia syndromes
- Alzheimer’s disease
Utility Of Fdg Pet In The Study Of Ad
The Pattern of FDG Hypometabolism Is an Endophenotype of AD
A substantial body of work over many years has identified a FDG-PET endophenotype of AD that is, a characteristic or signature ensemble of limbic and association regions that are typically hypometabolic in clinically established AD patients . The anatomy of the AD signature includes posterior midline cortices of the parietal and posterior cingulate gyri, the inferior parietal lobule, posterolateral portions of the temporal lobe, as well as the hippocampus and medial temporal cortices. Metabolic deficits in AD gradually worsen throughout the course of the disease. Bilateral asymmetry is common at early stages, more advanced disease usually involves prefrontal association areas, and in due course even primary cortices may be affected. Interestingly, the regions initially hypometabolic in AD are anatomically and functionally interconnected and form part of the large-scale distributed brain network known as the default mode network . We now know in addition that these regions are highly vulnerable to amyloid- deposition .
FDG Hypometabolism Is Related to Other AD Biomarkers and to Genes
FDG PET Is a Valid AD Biomarker
Don’t Miss: What Is The Difference Between Dementia And Senility
Experiment : Prediction Of Smci Vs Cad
The change in performances on the RAVLT-Im and ADAS13 tests are illustrated in Fig.;. Note the age-related decline in both the sMCI and the cAD subgroups, with the most severe impairments shown within the cAD group.
Figure; illustrates age-related tissue loss in the brain, with an almost linear shrinkage of the hippocampus volumes and a non-linear increase in the volume of the lateral ventricle . Overall, the most extensive losses are found among subjects in the cAD subgroup.
Inclusion of the cognitive trajectory features in the ensemble model gave \ for the accuracy, precision, recall and the \ scores. These scores changed to \, \, \ and \, respectively, when the longitudinal MRI features were added. The confusion matrices in Fig.; show a misclassification rate of \ for the subjects in both the cAD and the sMCI group when only the cognitive features were included, with a reduction to \ for the cAD subgroup and an increase to \ in the sMCI subgroup when the MRI features were added.
Figure 4
The trajectories for performances on the RAVLT-Im test and the ADAS13 test , with age at testing on the x-axis. The thick black curve is the cohort regression line, and thin grey lines are random effects for each subject. Severity of impairment is reflected by a lower score on the RAVLT test and a higher score on the ADAS13.
Would Mri Or Ct Show Dementia Ar Alzheimers
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Also Check: Does Smelling Farts Help Prevent Dementia
Current Practice In Diagnosing Dementia
The remainder of this information will provide an overview of the diagnosis process and a guide to what happens after diagnosis.;
It is important to remember that there is no definitive test for diagnosing Alzheimers disease or any of the other common causes of dementia. Findings from a variety of sources and tests must be pooled before a diagnosis can be made, and the process can be complex and time consuming. Even then, uncertainty may still remain, and the diagnosis is often conveyed as possible or probable. Despite this uncertainty, a diagnosis is accurate around 90% of the time.;
People with significant memory loss without other symptoms of dementia, such as behaviour or personality changes, may be classified as having a Mild Cognitive Impairment . MCI is a relatively new concept and more research is needed to understand the relation between MCI and later development of dementia. However, MCI does not necessarily lead to dementia and regular monitoring of memory and thinking skills is recommended in individuals with this diagnosis.;;
Basics Of Fdg Pet As Applied To Ad
Brain FDG PET primarily indicates synaptic activity. Because the brain relies almost exclusively on glucose as its source of energy, the glucose analog FDG is a suitable indicator of brain metabolism and, when labeled with Fluorine-18 is conveniently detected with PET. The brains energy budget is overwhelmingly devoted to the maintenance of intrinsic, resting activity, which in cortex is largely maintained by glutamaturgic synaptic signaling . FDG uptake strongly correlates at autopsy with levels of the synaptic vesicle protein synaptophysin . Hence, FDG PET is widely accepted to be a valid biomarker of overall brain metabolism to which ionic gradient maintenance for synaptic activity is the principal contributor . In this context, a single, specific AD-related alteration in FDG metabolism has not been identified and therefore the FDG-PET abnormalities described below are assumed to be the net result of some combination of processes putatively involved in the pathogenesis of AD including, but not limited to, expression of specific genes, mitochondrial dysfunction, oxidative stress, deranged plasticity, excitotoxicity, glial activation and inflammation, synapse loss, and cell death.
You May Like: Did Margaret Thatcher Have Dementia
Fazekas Scale For Wm Lesions
On MR, white matter hyperintensities and lacunes – both of which are frequently observed in the elderly – are generally viewed as evidence of small vessel disease.
The Fazekas-scale provides an overall impression of the presence of WMH in the entire brain. It is best scored on transverse FLAIR or T2-weighted images.
Score:
- Fazekas 0: None or a single punctate WMH lesion
- Fazekas 1: Multiple punctate lesions
- Fazekas 2: Beginning confluency of lesions
- Fazekas 3: Large confluent lesions
The Fazekas scale for WM lesions predicts future disability in elderly.
Fazekas 1 is considered normal in the elderly. Fazekas 2 and 3 are pathologic, but may be seen in normally functioning individuals. They are however, at high risk for disability.
In 600 normally functioning elderly people the Fazekas score predicted disability within one year .In the Fazekas 3 group 25% was disabled within one year . Three year follow-up shows that severe white matter changes independently and strongly predict rapid global functional decline .
Caps and bands
Alternatives To A Head Scan
Arguably, a head CT scan is the most effective way to diagnose Alzheimers, but there are other options. There are a few cognitive tests that you can download, print, and take at home. Then, you bring these tests to your doctor to score. For instance, the SAGE test from the Ohio State University Wexner Medical Center is one option.
Unfortunately, an autopsy is the only way to conclusively diagnose Alzheimers disease. To get a quality diagnosis before death, you may need to combine several cognitive functioning tests. For example, a head CT test along with an assessment by your primary care doctor may be ideal.
Don’t Miss: What Is The Color For Dementia
Basics Of Functional Mri As Applied To Ad
Functional MRI is being increasingly used to probe the functional integrity of brain networks supporting memory and other cognitive domains in aging and early AD. fMRI is a noninvasive imaging technique which provides an indirect measure of neuronal activity, inferred from measuring changes in blood oxygen leveldependent MR signal . Whereas fluoro-deoxy-d-glucose -PET is thought to be primarily a measure of synaptic activity, BOLD fMRI is considered to reflect the integrated synaptic activity of neurons via MRI signal changes because of changes in blood flow, blood volume, and the blood oxyhemoglobin/deoxyhemoglobin ratio . fMRI can be acquired during cognitive tasks, typically comparing one condition to a control condition , or during the resting state to investigate the functional connectivity within specific brain networks. Fc-MRI techniques examine the correlation between the intrinsic oscillations or time course of BOLD signal between brain regions , and have clearly documented the organization of the brain into multiple large-scale brain networks . Both task-related and resting fMRI techniques have the potential to detect early brain dysfunction related to AD, and to monitor therapeutic response over relatively short time periods; however, the use of fMRI in aging, MCI, and AD populations thus far has been limited to a relatively small number of research groups.
Basics Of Structural Mri As Applied To Ad
MRI utilizes the fact that protons have angular momentum which is polarized in a magnetic field. This means that a pulse of radiofrequency can alter the energy state of protons and, when the pulse is turned off, the protons will, on returning to their energy stage, emit a radiofrequency signal. By a combination of different gradients and pulses, sequences can be designed to be sensitive to different tissue characteristics. In broad terms structural MRI in AD can be divided into assessing atrophy and changes in tissue characteristics which cause signal alterations on certain sequences such as white matter hyperintensities on T2-weighted MRI as a result of vascular damage. A number of MR sequences that are sensitive to microstructural change have shown alterations in AD. These sequences are already important research tools; however, they have not yet found a place in routine clinical practice in AD and they will not be considered further here.
Also Check: Dementia Neurotransmitter
Early Diagnosis Of Alzheimer’s Disease And Mild Cognitive Impairment
The typical reductions of hippocampal volume in MCI with an average Mini-Mental State Exam score of 25 are 10% to 15% and in AD with an average MMSE score of 20 are 20% to 25% . Measuring these significant reductions in the medial temporal lobe can be extremely useful for early diagnosis of AD and MCI. At present, diagnostic criteria for AD are based on the criteria in the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition , which are based primarily on clinical and psychometric assessment and do not use quantitative atrophy information available in sMRI scans. However, there is a proposal to add reliable biomarkers to the diagnostic criteria . One of the suggested features is the volume loss of medial temporal structures since measures of sMRI atrophy have accuracies of 70% to 90% in AD and 50% to 70% in amnestic MCI in distinguishing them from age-matched controls . All of the above-mentioned cross-sectional methods, except 3a, can be used as diagnostic metrics for AD and MCI.
Structural Magnetic Resonance Imaging And Pib
Although there are several amyloid imaging PET tracers based on 11C and 18F, the tracer most studied in the field of AD is PIB , which we discuss here. PIB-PET scans measure the deposition of A in the brain . Since the invention of PIB, there has been significant interest in investigating the effect of A plaques as measured by PIB on cognition and sMRI. In this section, we will discuss studies that have investigated both PIB and sMRI in the same group of subjects. These studies are summarized in Table . In CN, baseline PIB was not associated with longitudinal sMRI changes in the preceding years but was strongly related to brain atrophy and future cognitive decline . The majority of studies have found a correlation between baseline sMRI and PIB measures . In addition, serial PIB and sMRI studies have found that longitudinal changes are much more pronounced on sMRI and that longitudinal change in PIB is minimal . All of this evidence has led to our understanding that A deposition measured by PIB is an upstream process whereas neurodegeneration is a downstream process that is probably initiated by A deposition and is more closely related to cognitive decline .
Table 3 Summary of combined magnetic resonance imaging and Pittsburgh compound B studies in Alzheimer’s disease
Don’t Miss: What Is The Difference Between Dementia And Senility
Can A Ct Scan Show Dementia
After extensive research, we look into the commonly-asked-question of whether or not can a CT scan show dementia.
It IS POSSIBLE to detect the condition by watching for telltale signs in loved ones or yourself.
The cause of action, in this case, is to visit a physician right away so that they can perform brain imaging procedures TO DETECT the progressive neurologic disorder.
That begs the question, can a CT scan show dementia?
Limitations Of Structural Mri In Ad
Structural MRI lacks molecular specificity. It cannot directly detect the histopathological hallmarks of AD and as such it is downstream from the molecular pathology. Cerebral atrophy is a nonspecific result of neuronal damage and, whereas certain patterns of loss are characteristic of different diseases, they are not entirely specific. Atrophy patterns overlap with other diseases and unusual forms of AD have atypical patterns of atrophy too. In more severely affected individuals and those with claustrophobia, MRI may not be tolerated whereas a rapid CT scan may be more feasible. In terms of measuring progression, volume changes on MRI may be produced by factors other than the progression of neuronal loss and as such assessment of disease modification may be obscured, at least in the short term, by such spurious effects. As the name implies, structural MRI cannot assess function; this is provided with increasing sophistication by functional MRI and PET.
Overall the availability, ease of use, and multiple applications of structural MRI in AD mean it will play a central role in research and practice for some years to come. Increasingly, the other modalities described in this article will address the weaknesses of MRI.
Recommended Reading: What Is The Difference Between Dementia And Senility
Cerebral Autosomal Dominant Arteriopathy With Subcortical Infarcts And Leukoencehalopathy
CADASIL is another hereditary disease which may present with a progressive cognitive dysfunction.Other presenting symptoms include migraines, stroke-like episodes and behavioral disturbances. It affects the small vessels of the brain.Confluent white matter hyperintesities in the frontal and especially anterior temporal lobes in combination with infarcts and microbleeds are seen on imaging.
The FLAIR images show classic findings in CADASIL – confluent white matter hyperintensities with lacunar infarcts and involvement of the anterior temporal lobes.
Traumatic brain injury
How Is Alzheimer’s Disease Diagnosed And Evaluated
No single test can determine whether a person has Alzheimer’s disease. A diagnosis is made by determining the presence of certain symptoms and ruling out other causes of dementia. This involves a careful medical evaluation, including a thorough medical history, mental status testing, a physical and neurological exam, blood tests and brain imaging exams, including:
Don’t Miss: Sandyside Senior Living
Early Warning Signs And Diagnosis
Alzheimers Disease can be caught in the early stageswhen the best treatments are availableby watching for telltale warning signs. If you recognize the warning signs in yourself or a loved one, make an appointment to see your physician right away. Brain imaging technology can diagnose Alzheimers early, improving the opportunities for symptom management.
Signs You May Need A Scan
If you have a family history of Alzheimers or dementia, you may want to get tested proactively so that you can determine if you have this condition. In other situations, you may want to get tested if you have any of the following symptoms:
- Memory loss
- Issues with depth perception
- Delusions or hallucinations
Many people believe that some memory loss is inevitable with aging, but this is simply not true. If you or your loved one is experiencing chronic or progressive memory loss or memory loss combined with the above symptoms, it may be a sign of Alzheimers.
Also Check: Does Alzheimer’s Run In Families
Extracting Information From Structural Magnetic Resonance Imaging
Given the large amount of data present in a three-dimensional sMRI scan, several different methods are employed to condense atrophy information in each patient’s scan or assess atrophy over multiple scans of the same individual. The pattern of neurodegeneration seen using sMRI is similar to the progression of neurofibrillary pathology as described by Braak and Braak . The disease usually begins and is ultimately most severe in the medial temporal lobe, particularly the entorhinal cortex and hippocampus. Later , the disease spreads to the basal temporal lobe and paralimbic cortical areas such as the posterior cingulate gyrus and precuneus. The onset of dementia is due to the spread of degenerative atrophy to multimodal association neocortices. Basal forebrain and the dorsal pontomesencephalic areas are also involved. However, unusual variants that do not follow this particular pattern are increasingly recognized. Furthermore, other limbic lobe structures such as posterior cingulate seem to be involved early and consistently in AD. Figure shows typical MRI scans in cognitively normal subjects and in patients with MCI or AD. As can been seen in the figure, there is increasing medial temporal atrophy in MCI and AD when compared with CN. Here, we present a brief survey of methods to extract or visualize this information from 3D sMRI scans of cross-sectional and longitudinal studies.
Figure 2