Narrative Analysis And Synthesis
We aim to apply a narrative synthesis, guided by several techniques.
Included studies will organised into groups/clusters, a common technique in narrative synthesis and a useful way of aiding the process of description and analysis and looking for patterns within and across these groups. Groups are refined as the synthesis develops.
We aim to develop a theoretical model of how, why and for whom early palliative care is relevant, while identifying a list of facilitators and barriers to its implementation reported. We additionally aim to report on a timeline/diagram with elements of definitions/conceptualisations of palliative care early in the disease trajectory and how those changed across time .
General Aim And Research Questions
We aim to conduct a scoping review of the literature in order to systematically map the research done in palliative care early in the disease trajectory of people living with mild and moderate dementia, as well as to identify any existing gaps in knowledge, current scientific debates and conceptualisations. Early palliative care in this study is defined as âin the early stages of the disease trajectory of dementiaâ, starting from diagnosis. Hence, not focused on people living with advanced, end-stage, terminal stages of dementia. Palliative care in this review is conceptualised as defined by the WHO, that is related to one, more or all of its domains and can be provided by any type of generalist or specialist healthcare provider. Generalist palliative care most often being provided by generalist healthcare professionals and/or providers not specialised in palliative care. Specialist palliative care intended to be provided by professionals that work solely in the field of palliative care and whose main activity is devoted to dealing with complex problems requiring specialist palliative care skills and competencies.
Guiding research questionsâamong others that we may derive from the review dataâinclude:
How is âearlyâ, âtimelyâ, âearlierâ palliative care defined, in relation to dementia?
What are current debates in the scientific literature? What are pros and cons?
How Might Dementia Affect People Towards The End Of Life
Dementia is progressive, which means it gets worse over time. In the last year of life, its likely to have a big impact on the persons abilities including memory, communication and everyday activities. The speed at which someone will get worse will depend on the type of dementia they have and who they are as an individual.
The symptoms of later stage dementia include the following:
A person with later stage dementia often deteriorates slowly over many months. They gradually become more frail, and will need more help with everyday activities such as eating, dressing, washing and using the toilet. People may experience weight loss, as swallowing and chewing become more difficult.
A person with later-stage dementia may also have symptoms that suggest they are close to death, but continue to live with these symptoms for many months. This can make it difficult for the person and their family to plan for the end of life. It also makes it difficult for those supporting them professionally.
For more information on supporting someone with later stage dementia see Alzheimers Society factsheet, The later stages of dementia .
Recommended Reading: Difference Between Senility And Dementia
Dementia Is A Terminal Illness Study
In the first study to rigorously describe the clinical course of advanced dementia, a leading cause of death among Americans, researchers in the US concluded that dementia is a terminal illness and is insufficiently recognized as such, resulting in many patients not receiving the palliative care that aims to improve the comfort of the terminally ill.
The study was the work of lead author Dr Susan L Mitchell and colleagues and is published online in the 15 October issue of the New England Journal of Medicine, NEJM. Mitchell a senior scientist at the Institute for Aging Research of Hebrew SeniorLife, an affiliate of Harvard Medical School in Boston, Massachusetts, where she is also Associate Professor of Medicine.
Today there are more than 5 million Americans living with dementia, and this number is expected to treble over the next 40 years, with worldwide numbers rising to more than 35 million by 2050, according to a recent study by Alzheimers Disease International.
People with dementia, of which the most common form is Alzheimers disease, have trouble with daily living: they suffer from memory loss, find it difficult to communicate, their personality changes, and they cant reason or make decisions.
Mitchell told the press that:
They hope their findings stress the need to improve the quality of end of life care in nursing homes to relieve the suffering of patients with advanced dementia and improve communication with their family members.
Planning For The End Of Life
It is important for people with dementia to make their wishes known regarding any future care and medical treatment throughout their illness but particularly around care towards the end of their life when they may be unable to express those wishes.
If they dont feel ready to think about the future at this time, getting to know the persons values, wishes and beliefs more generally can help in the future when decisions need to be made on their behalf. As a long-term carer, you are likely to have spent years developing vital knowledge and caring strategies to help you meet the unique needs of the person you care for. Your awareness and sensitivity to the, often, subtle changes in your relative’s behaviour, facial expression and body language that can indicate pain or distress make you ideally placed to help paid carers provide appropriate care.
You May Like: Does Bobby Knight Have Dementia
What Can You Do
Although there is no effective treatment or proven prevention for Alzheimers and related dementias, in general, leading a healthy lifestyle may help address risk factors that have been associated with these diseases.
Researchers cannot say for certain whether making the above lifestyle changes will protect against dementia, but these changes are good for your health and are all part of making healthy choices as you age.
Special Prerequisites Of Palliative Care In Advanced Dementia
Originally, palliative care emerged in the UK for cancer patients in response to insufficient care for the terminally ill. Eventually conditions other than cancer were acknowledged as being in need of palliative care. Independent of specific diagnosis palliative care should be provided for people with life-threatening disease and their families âthrough the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritualâ to maintain or improve quality of life . Parallel to the development of palliative care dementia care developed separately both based on the same values for enhancing care of people with dementia and improving quality of life . Notably lessons learned from palliative care for people with cancer cannot simply be transferred to palliative care for people with dementia.
As dementia progresses people experience reduced or lost verbal communication abilities with a consequent impact on care. Despite restrictions in verbal communication people with advanced dementia can use other means of nonverbal communication such as body tension or minimal movements, turning their head away, frequency of breath and paralinguistic signals are all means of communication to express their current wishes or needs . Agreement or rejection reactions in a situation can be observed, although interpretation of nonverbal communication varies between health professionals .
Don’t Miss: Dementia Awareness Ribbon
Complex Interventions In Advanced Dementia
As people with advanced dementia suffer complex symptoms and still have numerous and complex physical, psychosocial and spiritual needs they are in need of multidisciplinary health care. By comparison with early stages of the disease there is less knowledge about needs in advanced dementia . Physical needs are related to adequate symptom relief and basic care needs. It is complex to meet the numerous and differentiated psychosocial needs comparable to people in moderate state of dementia, e.g., need of enhancing personhood, communicating and being in contact with others, participating in everyday life or feeling save and familiar . Unmet social needs for activity contributed to discomfort and behavioral symptoms . Needs being important in mild or moderate stage of the disease, e.g., financial needs and cognitive strategies for coping with disease are less direct needs at least for the people with advanced dementia themselves.
Databases And Search Strategy
We will search the following key international databases: MEDLINE , The Cochrane Library, CINAHL, PsycINFO, EMBASE and Web of Science . No grey literature and texts that are not peer-reviewed are included because we are mainly highlighting scientific debates. The full search strategy is presented in and was built by an experienced medical librarian , taking into account two validated palliative care literature searches. In a final search phase, relevant literature reviews and key reports will be handsearched to identify articles missed by the search strategy. Ifâbefore submission of final resultsâthe search was conducted more than a year ago, we will update our search. We included studies reported in English, with a publication date between January 1, 2009 and the date of search. One author downloaded all retrieved records, compiled them by using reference manager , and removed duplicate records. A first search was conducted on 5 November 2019 an updated search was performed on 5 February 2021.
Inclusion and exclusion criteria study selection
Also Check: Vascular Cognitive Impairment Life Expectancy
What Do We Know About Reducing Risk For Dementia
The number of older Americans is rising, so the number of people with dementia is predicted to increase. However, some studies have shown that incidence rates of dementia meaning new cases in a population over a certain period of time have decreased in some locations, including in the United States. Based on observational studies, factors such as healthy lifestyle behaviors and higher levels of education may be contributing to such a decline. But the cause and effect is uncertain, and such factors need to be tested in a clinical trial to prove whether they can prevent dementia.
A review of published research evaluated the evidence from clinical trials on behavior and lifestyle changes to prevent or delay Alzheimers or age-related cognitive decline. The review found encouraging but inconclusive evidence for three types of behavioral changes : physical activity, blood pressure control, and cognitive training. The findings mean that interventions in these areas are promising enough that researchers should keep studying them to learn more. Researchers continue to explore these and other interventions to determine whether and in what amounts or forms they might prevent dementia.
Watch a video below that highlights conclusions and recommendations from the research review.
Check Their Advance Care Plan
You should find out if the person has an advance care plan. This document may record their preferences about the care theyd like to receive, including what they want to happen, what they dont want to happen and who they want to speak on their behalf. It may include an advance statement or an advance decision. We have information on planning ahead for patients and their families, which you might find useful.
Recommended Reading: Alzheimer’s Aphasia
End Of Life Care At Home
You may not need to move away from home to receive care, as end of life and hospice care can be provided at home. To find out what’s available locally, ask your GP.
Your GP can arrange for community nurses to provide nursing care at home.
You may also need specialist care from community palliative care nurses, who can also provide practical and emotional support for you and those caring for you.
Social services may also provide services and equipment to help you remain at home.
The Later Stage Of Dementia
People with later-stage dementia will eventually need full-time care and support with daily living and personal care, such as eating, washing and dressing. Whatever kind of dementia a person has, their life expectancy is on average lower.
The progression and stages of dementia
Dementia is a life-limiting condition and there is information about later-stage dementia and life expectancy on this page. Some people may find this upsetting and difficult to think about.
For more general information about the different stages of dementia, see The progression and stages of dementia page.
By the later stage of dementia, the condition will have a severe impact on most aspects of a persons life. The person will eventually need full-time care and support with daily living and personal care, such as eating, washing and dressing. This support can be provided by care at home but is more often given in a care home setting.
Symptoms of all kinds are likely to cause the person considerable difficulties in this stage, but altered perception and physical problems are often the most noticeable. By the late stage, the symptoms of all types of dementia become very similar.
The later stage of dementia tends to be the shortest. On average it lasts about one to two years.
Are you supporting a person with later-stage dementia?
Get practical advice and tips on supporting a person with later-stage dementia.
Don’t Miss: Did Ronald Reagan Have Alzheimer In Office
Where To Deliver Palliative Care For Dementia Patients
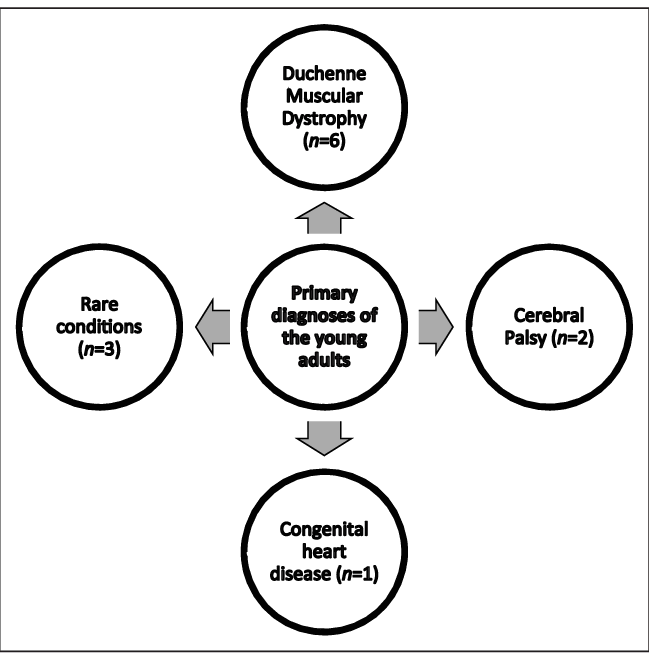
It is commonly stated that patients with dementia lack access to palliative care in hospice settings less than 1% of patients in inpatient hospices have dementia as their primary diagnosis.2
Current hospice provision in the UK would be inadequate to care for these patients in the terminal phase indeed, it could be argued that moving a patient with severe cognitive impairment to a new unfamiliar environment with unfamiliar staff is likely to have a deleterious effect on quality of life and likely to increase agitation, disorientation and distress.
Hospice care may, however, be appropriate for some casesfor example, those individuals requiring complex symptom control or where there is a lack of support available, such as those living alone with no close relative. Access to specialised palliative care should be based on need and not age or diagnosis. However, as many specialised palliative care services are often partially funded by charitable cancer organisations, a review of funding will be needed. Palliative care specialists have expressed the need for their involvement in nonmalignant disease for some time.29
A more practical approach is therefore delivering hospice quality palliative care to dementia patients in their usual place of residence, and there are a number of developing strategies to facilitate thisfor example, the Liverpool care pathway for the end of life, and the Gold Standards Framework.
Support For People With Dementia And Carers
UCL covid-19 decision aid – a tool to support carers of people living with dementia to make difficult decisions during covid-19
Alzheimers Society end of life care information for patients and families
Alzheimers Society information and fact sheets on all aspects of dementia including what is dementia, types of dementia and living well with dementia
Alzheimer Scotland specialist services for patients and carers
Dementia UK expert one-on-one advice and support to families living with dementia via Admiral Nurses
Recommended Reading: Ribbon Color For Alzheimer’s
Physical Difficulties In The Later Stages Of Dementia
The physical changes of late-stage dementia are partly why the person is likely to need much more support with daily living. At this stage they may:
- walk more slowly, with a shuffle and less steadily eventually they may spend more time in a chair or in bed
- be at increased risk of falls
- need a lot of help with eating and so lose weight
- have difficulty swallowing
- be incontinent losing control of their bladder and bowels.
The persons reduced mobility, in particular, raises their chances of blood clots and infections. These can be very serious or even fatal so it is vital that the person is supported to be as mobile as they can.
How To Deliver Palliative Care To Dementia Patients
Guidelines and care pathways
There is evidence that the use and audit of multidisciplinary guidelines improve the palliation of symptoms in dementia patients.31 The Liverpool care pathway for the end of life32 facilitates delivery of holistic palliative care in a variety of settings and it is being widely adopted in hospitals, hospices and in the community. Its use is endorsed by the proposed National Institute for Health and Clinical Excellence guidelines on dementia which includes a section on palliative care issues .
Table 2NICE guidelines on dementia: key palliative care components1
NICE, National Institute for Health and Clinical Excellence.
Equally, the guidelines also endorse the use of the Gold Standards Framework, a programme developed primarily for use in primary care based on the 7 C’s: communication, coordination, control of symptoms, continuity, continued learning, carer support, and care of the dying.26 The emphasis on anticipatory care and the transfer and communication of information to outofhours services are particularly important.
Both of these strategies are also recommendations of other key government directives in the UK including the Department of Health Guide to end of life care in care homes document and the NICE guidance on supportive and palliative care .
Symptom management
Read Also: Alzheimer’s Disease Color Ribbon
How Does Dementia Reduce Life Expectancy
Dementia reduces life expectancy in two ways.
First, some of the diseases that are closely linked to Alzheimers disease and vascular dementia, such as diabetes and cardiovascular disease can mean a lower life expectancy. For example, vascular dementia is closely linked to heart disease and stroke. A person with vascular dementia is at risk of dying at any stage of dementia, from one of these.
The other way that dementia reduces life expectancy is through the effects of severe disease.
These all make them much more likely to develop other medical problems that can lead to death, such as infections or cardiovascular problems .
This is why the later stage of dementia is often the shortest.
A person with dementia can also die at any stage from another condition not closely related to their dementia. Cancer and lung disease are common examples.