Stage : Moderate Dementia
Patients in stage 5 need some assistance in order to carry out their daily lives. The main sign for stage 5 dementia is the inability to remember major details such as the name of a close family member or a home address. Patients may become disoriented about the time and place, have trouble making decisions, and forget basic information about themselves, such as a telephone number or address.
While moderate dementia can interfere with basic functioning, patients at this stage do not need assistance with basic functions such as using the bathroom or eating. Patients also still have the ability to remember their own names and generally the names of spouses and children.
Facts About Alzheimer Disease
Alzheimer disease is becoming more common as the general population gets older and lives longer. Alzheimer disease usually affects people older than 65. A small number of people have early-onset Alzheimer disease, which starts when they are in their 30s or 40s.
People live for an average of 8 years after their symptoms appear. But the disease can progress quickly in some people and slowly in others. Some people live as long as 20 years with the disease.
No one knows what causes Alzheimer disease. Genes, environment, lifestyle, and overall health may all play a role.
Stages As A Modification To The 3
Now, one possible way to salvage the three-stage view would be to start referring to grades within each stage. So, instead of speaking about âmiddle stage, ,â you might talk instead of âearly-middle stageâ or âlate-middle stage.â So, for instance: My dad, sitting and smiling, but unable to talk or care for himself was in âearly-late stage.â But my dad lying there, unable to swallow food or water was in âlate-late stage.â Or something like this.
But by this time, a person might reasonably ask: do we really have a three-stage view anymore? If you are going to add qualifiers to every stage, why not just carve out a few more stages?
I am not entirely clear on the history, here, but presumably, the seven-stage view was an outgrowth of this kind of reasoning process.
Even here, though, variations abound. Just as with the three-stage view, the seven-stage system has its variants as well. My research suggests that when a seven-entry catalog is used, it generally represents the stages as follows.
The Standard, Seven-Stage View of Alzheimerâs
This articulation of the stages was apparently devised by academics Barry Reisberg and Emile Franssen and seems to be preferred by authority sites such as Alzheimers.net. Additionally, it is repeated, or reproduced on a website called CaregiverHomes.
You May Like: Difference Between Dementia And Senility
Stage : Second Last Stage Middle Vascular Dementia
Individuals in this severe stage begin to lose memory and usually recollect things happened and things they did in their past. They become more delusional and even cannot remember close friends and family members names. Some bodily changes also turn up including incontinence, difficulty with muscle and motor functions and difficulty with controlling bladder flow. They need assistance to do daily activities and finish tasks. These signs and symptoms are enough to diagnose middle vascular dementia.
Weight loss: Almost all of the people with vascular dementia lose weight in the later stages of this disorder, although sometimes some people eat so much and put on weight. In fact, weight loss can affect their immune system, making the people fight infections more difficultly. It can also increase the possibility of falling. Ensure that they consume enough food and water. They can need encouragement with drinking and eating. Besides, problems with swallowing and chewing are common as their muscles no longer work properly.
Problems with continence: Many people cannot control their bladder and bowels. This can occur most or all of the time.
This is also a stage one on the list of vascular dementia stages that people should not miss out but consider changing their lifestyles to prevent themselves from getting this disorder.
The Stages Of Alzheimers Disease
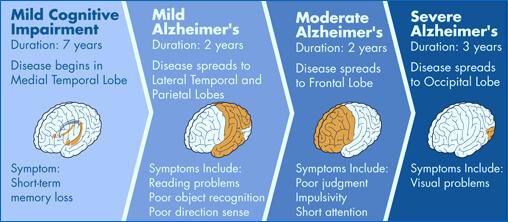
The only certainty when diagnosed with Alzheimer’s disease is that a seniors condition will progressively worsen. The national Alzheimers Association has developed a very useful staging system to use as a frame of reference when coping with AD.
Alzheimer’s disease constantly keeps doctors, family members and caregivers on their toes. It is instinctive for humans to want a roadmap or some sort of guide to help get us through a journey or a difficult situation. We strive to know what lies ahead to help ensure that we are adequately prepared. Following a serious medical diagnosis like Alzheimers disease , it is only natural to explore the subject with some research. What can we expect and when can we expect it?
Keep in mind that the following staging system is not foolproof, but it can give caregivers a general idea of where their aging loved one falls along the Alzheimers disease spectrum. Seniors with Alzheimers are not guaranteed to follow these stages in a direct line. No matter how much we would like to know exactly what stage someone is in and what symptoms will develop next, we cannot. No two Alzheimers patients are exactly the same. To make matters even more complex, a patients symptoms often vary from day to day. Today, a loved one may seem like they are in stage five, and tomorrow their behaviors and symptoms may align more closely with stage four or stage six.
Also Check: Alzheimer’s Paranoia Medication
A Word About Progression
Alzheimers typically progresses slowly and transitions from mild to severe symptoms. The rate of progression varies widely between people. People with Alzheimers live an average of 4 to 8 years after their diagnosis, but some people live more than 20 years.
The risk of progressing to a higher stage increases with age. For example, in a
Changes In Middle Stage
Cognitive Changes in Middle Stage
During middle stage, language abilities take a major hit. Reasoning processes become more muddled.
Other cognitive changes dovetail with personality changes, about which read more further on.
Daily-Living Changes in Middle Stage
The suffererâs abilities to perform the ADLs also declines sharply through middle stage. The affected individual may bathe infrequently and inadequately, for instance. And the person may begin to behave erratically and unreliably in the bathroom.
To illustrate, my dad would sometimes confuse various paper products â facial tissues, paper towels, toilet paper, etc. â with potentially messy results that I will leave to readersâ imaginations.
The capability of dressing oneself may or may not remain. In some cases, the mechanical ability to put on clothes is present, but â because of decreased awareness, judgment, and so on â a person loses the good sense to choose appropriate garments for the occasion or for the weather.
Sleeping may also begin to go haywire. My dad would often be awake late into the night, and he would frequently nap at odd times during the day. Some of this might be treatable with sleep aids or coffee.
Memory Changes in Middle Stage
As the Alzheimerâs worsens, sufferers begin to have difficulty remembering personal information â address, social-security number, telephone number, and so on. They will also tend to have trouble recalling newly acquired information and recent events.
Also Check: Aphasia And Alzheimer’s
Stage : Mild Cognitive Impairment
Persons at this stage manifest deficits which are subtle, but which are noted by persons who are closely associated with the person with mild cognitive impairment. The subtle deficits may become manifest in diverse ways. For example, a person with mild cognitive impairment may noticeably repeat queries. The capacity to perform executive functions also becomes compromised. Commonly, for persons who are still working in complex occupational settings, job performance may decline. For those required to master new job skills, such as a computer or other machinery, decrements in these capacities may become evident.
MCI persons who are not employed, but who plan complex social events, such as dinner parties, may manifest declines in their ability to organize such events. This may be an early stage of Alzheimers, however, it is important for the person to seek medical help as soon as possible, to determine if a broad variety of medical conditions may be causing or contributing to the persons difficulties. Blood tests and an MRI of the brain should be obtained to assist in determining if the individual has MCI due to Alzheimers and whether there are other causes or contributing conditions to the persons cognitive decline.
Some MCI persons may manifest concentration deficits. Many persons with these symptoms begin to experience anxiety, which may be overtly evident.
What Causes Alzheimers Disease
In recent years, scientists have made tremendous progress in better understanding Alzheimers and the momentum continues to grow. Still, scientists dont yet fully understand what causes Alzheimers disease in most people. In people with early-onset Alzheimers, a genetic mutation may be the cause. Late-onset Alzheimers arises from a complex series of brain changes that may occur over decades. The causes probably include a combination of genetic, environmental, and lifestyle factors. The importance of any one of these factors in increasing or decreasing the risk of developing Alzheimers may differ from person to person.
Read Also: Aphasia In Alzheimer’s
The Basics Of Alzheimers Disease
Scientists are conducting studies to learn more about plaques, tangles, and other biological features of Alzheimers disease. Advances in brain imaging techniques allow researchers to see the development and spread of abnormal amyloid and tau proteins in the living brain, as well as changes in brain structure and function. Scientists are also exploring the very earliest steps in the disease process by studying changes in the brain and body fluids that can be detected years before Alzheimers symptoms appear. Findings from these studies will help in understanding the causes of Alzheimers and make diagnosis easier.
One of the great mysteries of Alzheimers disease is why it largely affects older adults. Research on normal brain aging is exploring this question. For example, scientists are learning how age-related changes in the brain may harm neurons and affect other types of brain cells to contribute to Alzheimers damage. These age-related changes include atrophy of certain parts of the brain, inflammation, blood vessel damage, production of unstable molecules called free radicals, and mitochondrial dysfunction .
Sixth Dementia Stage: Severe Decline
The sixth stage of dementia is the second to last stage where patients may require constant supervision as well as around the clock or 24/7 medical care. If a person cannot receive proper care at home at this point, it is best to look for assisted living centers near you or nursing homes which also specializes in taking care of patients who have dementia . Symptoms that people usually showcase in the 6th stage of dementia include:
- Unawareness or confusion of surroundings and environment
- Wandering
- Need for assistance with day to day activities like bathing, dressing, toileting, eating and incontinence
- Potential behavioral problems as well as personality changes
- Inability to recall most details about their history
- Failure to recognize faces apart from very close relatives and friends
- Loss of bladder and bowel control
- Loss of willpower
You May Like: What Are Complications Of Alzheimer Disease That Cause Death
Managing Alzheimer’s Disease Behavior
Common behavioral symptoms of Alzheimers include sleeplessness, wandering, agitation, anxiety, and aggression. Scientists are learning why these symptoms occur and are studying new treatments drug and nondrug to manage them. Research has shown that treating behavioral symptoms can make people with Alzheimers more comfortable and makes things easier for caregivers.
Stage : Mid Stage Semi Severe Vascular Dementia
Another one on the list of the vascular dementia stages that I would like to reveal in this article today and want you and my other readers to know if you are considering whether they get this disorder or not.
Loss of mobility: Many people gradually lose the ability of walking and performing everyday tasks. One of the first signs is that they walk unsteadily. They can also seem slower, bump into things and fall objects. Some people even become confined to a chair or bed. People who are caring for people with vascular dementia should ask for an advice from a community nurse or a therapist to aid mobility.
Memory loss: This symptom is very severe in the stages of vascular dementia. Patients may not be able to recognize other people who are close to them and even their own reflection. Also, they may not be able to find their way home around familiar surroundings or identify objects they use every day. However, occasionally, they may experience sudden flashes of recognition. They may believe that they are in a time from their past and may look for something or somebody from that time. For those around them, it may be helpful to try talking with them about the past. Even when they have severe memory loss, they still can appreciate or respond to music, touch and scent. Thus, continue to talk to them, even when they cannot respond.
Also Check: Atypical Alzheimer’s Disease
The 3 Stages Of Alzheimer’s: What To Expect And What To Do
If you or a loved one has recently been diagnosed with Alzheimers disease, you are likely experiencing many different emotions including shock, fear, sadness, and worry. Knowing what to expect and how to plan ahead can provide a sense of control and important peace of mind. Alzheimers disease has three stages: early , middle , and late . Here is what to expect and what to do during each of them.
Three Stages As Losses Of Psychological Powers
The ancient Greek philosopher Aristotle wrote a book that has come to us better known by its Latin title, De Anima , meaning âOn the Soul.â In fact, the Greek word for âsoulâ was psyche . The word persists in our day in our science of psychology â which, to an ancient, would designate the âstudy of the soul.â
But, just as the science of psychology does not attribute religious or supernatural qualities to the psyche, so too in this work does Aristotle assume a more or less âneutralâ definition of âsoul.â Stemming back to at least to Plato, psyche basically just meant âlife force.â And that minimalistic definition will suffice for what follows.
Aristotle recognized three levels of life force, pertaining to plants, animals in general, and human animals in particular. He distinguished them in virtue of what have come to be called âpowersâ of the soul.
So, at the level of plant life, Aristotle thought, there was a ânutritiveâ or âvegetativeâ soul. This life force was evident in virtue of a plantâs ability to grow, ânutrifyâ itself â by drawing upon soil, sunlight, and water â and to reproduce.
A bit higher up are the animals, enjoying an âanimalâ or âsensitiveâ soul. This life force has all the nutrifying and reproductive abilities of a plant alongside certain locomotive and appetitive powers that allow animals to move from place to place and to experience sensations.
3-Stage âAristotelianâ View
Also Check: Smelling Farts Dementia
What To Do Next After Learning What Stage Of Alzheimer’s Disease Your Loved One Is In
As mentioned, learning about the stage of Alzheimers disease that a loved one is experiencing helps provide perspective and context. This knowledge makes it easier to have conversations with doctors about the patients condition and how to approach future treatment options. Understanding the later stages of the disease also helps when planning for lifestyle changes, new equipment, and other items that may be needed. One of the other major benefits in understanding the overall progression of Alzheimers disease is preparing for future living arrangements, such a memory care community, that could become a preferred option during later stages of the disease. Because the cost of dementia care is high, families should begin planning as soon as possible following a diagnosis.
Stage : Moderately Severe Dementia
When the patient begins to forget the names of their children, spouse, or primary caregivers, they are most likely entering stage 6 of dementia and will need full time care. In the sixth stage, patients are generally unaware of their surroundings, cannot recall recent events, and have skewed memories of their personal past. Caregivers and loved ones should watch for:
- Delusional behavior
Read Also: How Long Does The 7th Stage Of Alzheimer’s Last
How Quickly Does Alzheimers Disease Progress
Alzheimers disease advances at widely different rates. The duration of the illness may often vary from 3 to 20 years. The areas of the brain that control memory and thinking skills are affected first, but as the disease progresses, cells die in other regions of the brain. Eventually, the person with Alzheimers will need complete care. If the individual has no other serious illness, the loss of brain function itself will cause death.
More On Activities Of Daily Living
ADLs are the things people perform every day as part of their daily routines such as eating, dressing, bathing/showering, attending to personal hygiene and grooming such as brushing his/her hair, and toileting.
Not everyone with MCI will go on to develop the third stage of Alzheimers diseaseAlzheimers dementia.
Symptoms of MCI are usually mild, involving problems in cognition. Cognition is defined as the process of thinkingcognitive abilities are the skills required to carry out any task ranging from simple to complex ones. They are the brain-based abilities required to learn, remember, problem-solve and pay attention.
Not all symptoms of MCI interfere with a persons ability to perform ADLs. These may include forgetting appointments or important events, losing things frequently, or difficulty remembering words.
Symptoms that must be present for a diagnosis of MCI include:
- Concern about a change in cognition
- Impairment of one or more cognitive functions, such as problem-solving or memory
- Ability to perform ADLs
Don’t Miss: How Fast Does Ftd Progress
The Short Answer To A Big Question
On this page we will discuss the development of an Alzheimers / dementia Life Expectancy Calculator, but lets first address the question most people ask after receiving the diagnosis of an incurable disease: How long do I have left to live? With dementia, the answer differs depending on the type. By far the most common form of dementia is Alzheimers disease, and the average life expectancy after diagnosis is 10 years. Other dementias have different life expectancies. Someone with vascular dementia lives for about five years after diagnosis. Someone who has dementia with Lewy bodies will typically live for six to twelve more years.
Average life expectancies for the most common types of dementia are as follows:
| Dementia type |