Atypical Form Of Alzheimers Disease May Be Present In A More Widespread Number Of Patients Mayo Clinic Says
JACKSONVILLE, Fla. Neuroscientists at Mayo Clinic in Florida have defined a subtype of Alzheimers disease that they say is neither well recognized nor treated appropriately.
The variant, called hippocampal sparing AD, made up 11 percent of the 1,821 AD-confirmed brains examined by Mayo Clinic researchers suggesting this subtype is relatively widespread in the general population. The Alzheimers Association estimates that 5.2 million Americans are living with AD. And with nearly half of hippocampal sparing AD patients being misdiagnosed, this could mean that well over 600,000 Americans make up this AD variant, researchers say.
In an oral presentation at the annual meeting of the American Academy of Neurology in Philadelphia, scientists say hippocampal sparing AD often produces symptoms that are substantially different from the most commonly known form of AD, which affects the hippocampus, the center of memory.
The patients, mostly male, are afflicted at a much younger age, and their symptoms can be bizarre behavioral problems such as frequent and sometimes profane angry outbursts, feelings that their limbs do not belong to them and are controlled by an alien unidentifiable force, or visual disturbances in the absence of eye problems, researchers say.
They also decline at a much faster rate than do patients with the most common form of AD.
A Case Of Atypical Early
CASE PRESENTATION
Mrs. P, a 54-year-old Caucasian female, was seen by her primary care provider five years ago with a complaint of memory problems. She noted episodes of forgetfulness from as early as age 46. Mrs. Ps husband had noted changes in both her personality and memory. He reported out-of-character use of profanity and a gradual onset of apathy. She had progressively become less attentive to daily routines at home. Mrs. P complained of episodes where she had forgotten the route home, and reported difficulty remembering steps in routine tasks she had performed repeatedly for years.
Further evaluation revealed a maternal family history of early-onset dementia. The patients mother was diagnosed with Alzheimers disease and was placed in long-term care at an early age. Mrs. P initially attributed her changes in mood and cognition to menopause in her early 40s. Her medical history was significant for degenerative changes of the spine and mitral valve prolapse. Mrs. P denied any history of psychiatric hospitalizations, psychiatric treatments, head injury, or substance abuse. She has been married for 38 years. She completed nine years of school and never worked outside the home. She has one adult son and two grandchildren. Mrs. Ps husband is disabled and relies upon her as his primary caregiver.
DISCUSSION
OUTCOME OF THE CASE PATIENT
The authors report no relevant financial relationships.
References
What Is Alzheimers Disease
This information comes to us from Alzheimers Society, the UKs leading dementia support and research charity for people living with dementia, their families, and care partners. And also one of my favorite sites to find news and information on Alzheimers disease and other dementias.
Listen to the audio version of What is Alzheimers disease?
Alzheimers disease is the most common cause of dementia. The word dementia describes a set of symptoms that can include memory loss and difficulties with thinking, problem-solving or language. These symptoms occur when the brain is damaged by certain diseases, including Alzheimers disease. This factsheet describes the symptoms of Alzheimers disease, how it is diagnosed, and the factors that can put someone at risk of developing it. It also describes the treatments and support that are currently available.
Alzheimers is a progressive disease. This means that gradually, over time, more parts of the brain are damaged. As this happens, more symptoms develop. They also become more severe.
You May Like: Does Meredith Grey Have Alzheimer’s
The Four Atypical Parkinsonism Disorders
This section compares the four atypical parkinsonism disorders:
These diseases are frequently mistaken for each other and for Parkinsons Disease, Alzheimers Disease, stroke, and other neurological conditions. To some extent, we address the questions If its not Alzheimers Disease, what is it? and If its not Parkinsons Disease, what is it?
Excellent organizations focus on each of these atypical parkinsonism disorders. We list these organizations on our pages dedicated to each disorder. Brain Support Network casts a wider net, describing and comparing the four disorders and their subtypes.
Given our extensive experience with brain donation, we know that the diagnostic accuracy of these disorders is low. We know the diagnosis before the brain is delivered for autopsy and we learn the definitive diagnosis by the neuropathologist after autopsy. Accuracy hovers around 50%, even for diagnoses delivered by expert neurologists.
These disorders are rare, difficult to diagnose, and moving targets as new subtypes are described. One of BSNs missions is to sketch the landscape so that laypeople can have meaningful discussions with medical providers and can serve as effective advocates.
What Are Atypical Parkinsonian Disorders
Atypical Parkinsonian disorders are progressive diseases that present with some of the signs and symptoms of Parkinsons disease, but that generally do not respond well to drug treatment with levodopa. They are associated with abnormal protein buildup within brain cells.
The term refers to several conditions, each affecting particular parts of the brain and showing a characteristic course:
- Dementia with Lewy bodies, characterized by an abnormal accumulation of alpha-synuclein protein in brain cells
- Progressive supranuclear palsy, involving tau protein buildup affecting the frontal lobes, brainstem, cerebellum and substantia nigra
- Multiple system atrophy, another synucleinopathy that affects the autonomic nervous system , substantia nigra and at times the cerebellum
- Corticobasal syndrome, a rare tauopathy that typically affects one side of the body more than the other and makes it difficult for patients to see and navigate through space
Don’t Miss: Does Medicare Cover Nursing Home Care For Dementia
Dementia With Lewy Bodies
Dementia with Lewy bodies causes hallucinations and dementia, as well as tremor, slowness, and stiffness. Doctors dont know the root cause of LBD, but they think its probably a mix of genetics, environment, and aging.
DLB results from clumping of proteins in the brain called Lewy bodies. Lewy bodies also form in PD, though they arent used in the diagnosis of either condition.
Some of their symptoms are similar, however, which can make it hard to distinguish between PD and DLB. The main difference is that dementia and hallucinations begin early in DLB, whereas movement problems predominate in early PD.
The first sign of DLB is often REM sleep behavior disorder. It can begin years before other symptoms of DLB. People with this disorder act out their dreams. They move and talk while dreaming instead of lying still.
DLB and a related condition, Parkinsons disease dementia, share similar symptoms and result from clumps of the same protein, alpha-synuclein, in brain cells. Because the symptoms of both diseases relate so closely to those of PD, the three conditions are often collectively called Lewy body disorders.
Lewy body dementia is the second most common form of dementia, after Alzheimers disease. Symptoms include:
- hallucinations and delusions
- eyelid movement issues and vision problems
- lack of motivation and other behavioral changes
Symptoms Of Atypical Parkinsonism
PD symptoms vary from person to person. Some people have a tremor, usually on one side of the body. Others with PD have muscle freezing or balance difficulties. You might have PD symptoms that are mild for years. Someone else may have symptoms that worsen quickly.
Atypical Parkinsonian syndromes each have their own set of symptoms:
- VP: Gait and balance problems are common symptoms. Dementia, incontinence, and palsy also develop.
- LBD: Thinking and memory decline. Hallucinations, delusions, and difficulty staying alert are also symptoms.
- MSA: Walking and balance problems are common with this condition. You may also have symptoms related to autonomic dysfunction. This is when the autonomic nervous system doesnt function as it should. The ANS controls automatic bodily functions like breathing, digestion, and circulation. These symptoms might include:
- incontinence
- a sudden drop in blood pressure when you stand up
You May Like: What Is The Color For Dementia
How Is Age Related To Pca
People with PCA may often go to see an eye doctor first, thinking that their difficulties are due to a problem with their eyes and that they may need new glasses. Visual impairment commonly develops as people get older, and in most cases, a decline in vision is due to this natural aging process. In people with PCA, the visual problems are not due to problems with their eyes. Rather, the shrinking brain can no longer interpret and process the information received from the persons healthy eyes.
What Are The Symptoms Of Atypical Parkinsonian Disorders
Like classic Parkinsons disease, atypical Parkinsonian disorders cause muscle stiffness, tremor, and problems with walking/balance and fine motor coordination.
Patients with atypical Parkinsonism often have some degree of difficulty speaking or swallowing, and drooling can be a problem. Psychiatric disturbances such as agitation, anxiety or depression may also be part of the clinical picture.
Dementia with Lewy bodies can cause changes in attention or alertness over hours or days, often with long periods of sleep during the day. Visual hallucinations typically of small animals or children, or moving shadows in the periphery of the visual field are common in DLB. DLB is second only to Alzheimers disease as a cause of dementia in the elderly, and it most commonly affects patients in their 60s.
Patients with progressive supranuclear palsy may have difficulties with eye movements, particularly when looking downward, and with balance when descending stairs, for instance. Backward falls are common and may occur during the early course of the disease. PSP is not usually associated with tremor, unlike Parkinsons disease.
Parkinson’s Disease and Movement Disorders Center
Don’t Miss: Alzheimer Vs Dementia Vs Senility
Who Gets Alzheimers Disease
Most people who develop Alzheimers disease do so after the age of 65, but people under this age can also develop it. This is called early-onset Alzheimers disease, a type of young-onset dementia. In the UK there are over 40,000 people under the age of 65 with dementia.
Developing Alzheimers disease is linked to a combination of factors, explained in more detail below. Some of these risk factors can be controlled, but others cannot. For more information see factsheet 450, Am I at risk of developing dementia?
What Causes Alzheimers Disease
The exact cause of Alzheimer’s disease is not known.
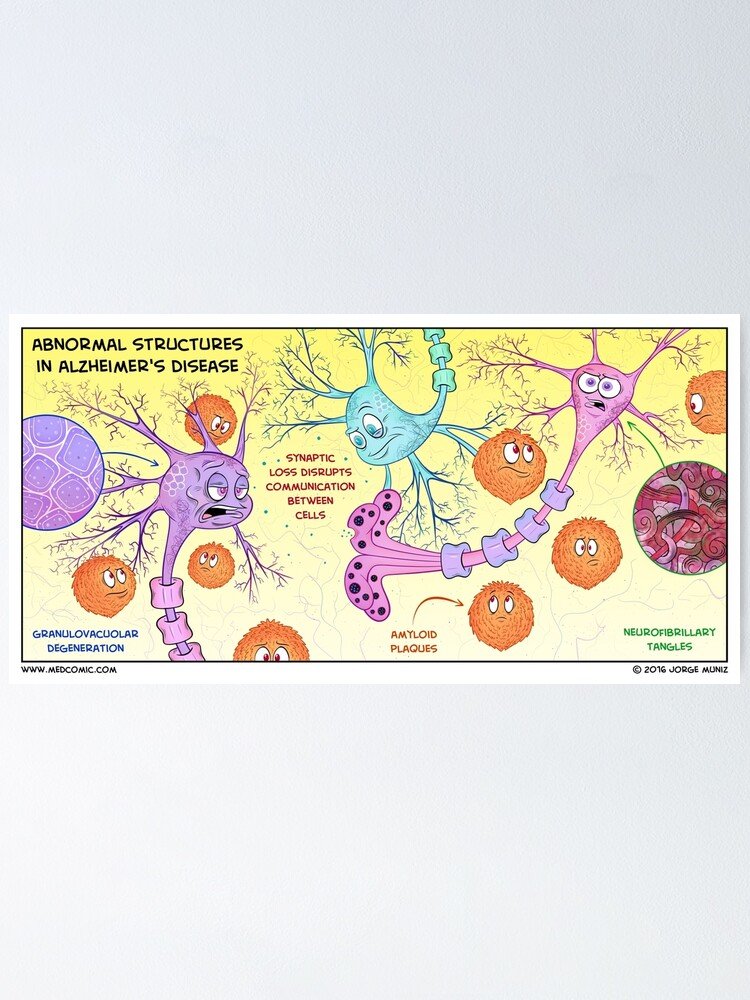
We know that the process begins with parts of the brain shrinking . This affects the function and structure of certain areas of the brain. What we dont know is what causes this process to start. As well as the amyloid plaques and neurofibrillary tangles that scientists have found in the brains of people with Alzheimer’s disease, there are also imbalances in a chemical called acetylcholine.
It’s also not uncommon to have some vascular damage in the brain with Alzheimers. All of this reduces the effectiveness of the healthy neurons and gradually destroys them. The first areas of the brain that are affected are the ones that are responsible for memories, but eventually, the damage spreads to other areas of the brain.
Read Also: Senility Vs Dementia
Comparing Disorders And Subtypes
The following table provides a brief summary of the differences among atypical parkinsonism disorders. Most exhibit parkinsonism symptoms some exhibit dementia symptoms each is identified by specific mis-folded proteins visible in the brain upon autopsy.
Atypical parkinsonism disorders are difficult to diagnose because there is no chemical test of blood or tissue, there is no imaging test, and the various disorders have similar symptoms and even share symptoms with non-parkinsonism disorders.
When a Board-certified neurologist delivers a diagnosis for any of the four atypical [arkinsonism disorders, the probability that the diagnosis is incorrect is approximately 50%. The only way to definitively diagnose an atypical parkinsonism disorder is by postmortem microscopic analysis of brain tissue.
| Atypical Parkinsonism Disorder |
|---|
Causes Of Atypical Parkinsonism
Atypical Parkinsonism disorders each have their own causes.
Scientists still dont know why people develop PD or atypical Parkinsonism. PD and some Parkinsonism conditions may have a genetic component. Research also suggests that exposure to some environmental toxins may be to blame.
Read on to learn about the various Parkinsonism conditions.
Recommended Reading: Did Margaret Thatcher Have Dementia
What Are The Most Common Symptoms For Alzheimers Disease
There are some common symptoms of Alzheimers disease, but it is important to remember that everyone is unique. Two people with Alzheimers are unlikely to experience the condition in exactly the same way.
For most people with Alzheimers, the earliest symptoms are memory lapses. In particular, they may have difficulty recalling recent events and learning new information. These symptoms occur because the early damage in Alzheimers is usually to a part of the brain called the hippocampus, which has a central role in day-to-day memory. Memory for life events that happened a long time ago is often unaffected in the early stages of the disease.
Memory loss due to Alzheimers disease increasingly interferes with daily life as the condition progresses. The person may:
- lose items around the house
- struggle to find the right word in a conversation or forget someones name
- forget about recent conversations or events
- get lost in a familiar place or on a familiar journey
- forget appointments or anniversaries.
Although memory difficulties are usually the earliest symptoms of Alzheimers, someone with the disease will also have or go on to develop problems with other aspects of thinking, reasoning, perception or communication.
They might have difficulties with:
A person in the earlier stages of Alzheimers will often have changes in their mood. They may become anxious, irritable or depressed. Many people become withdrawn and lose interest in activities and hobbies.
Pd Vs Atypical Parkinsonism
Symptoms of PD come on gradually as neurons in a part of the brain called the substantia nigra begin to die.
Doctors arent sure exactly what causes the cells to die. Theyve linked it to a misfolding of certain proteins in the brain. This could set off a reaction among other proteins, which start to form clumps and damage the brain. Over time, this leads to the loss of muscle control and dementia that characterize Parkinsons.
Symptoms of PD and atypical Parkinsonism are often similar. For this reason, Parkinsonism is sometimes initially misdiagnosed as PD. This is why testing and imaging are so important in making an accurate diagnosis.
Researchers are working on ways to take images inside the living human brain of proteins associated with PD and Parkinsonism. Live brain imaging of these proteins would greatly boost doctors ability to diagnose and monitor these disorders.
One main difference between the two conditions is that atypical Parkinsonism symptoms tend to come on earlier than they do in typical PD. Symptoms such as falling, dementia, and hallucinations occur earlier in atypical Parkinsonism disorders.
PD symptoms often appear first on one side of the body. With atypical Parkinsonism, signs are often present on both sides at the beginning.
Another key difference between PD and atypical Parkinsonism is whats happening in the brain.
Read Also: What Shampoos Cause Alzheimer’s Disease And Cancer
The Difference Between Alzheimers Disease And Primary Progressive Aphasia
Kimberly Williams-Paisley learns the difference between Alzheimers disease and primary progressive aphasia after her mothers diagnosis with PPA. The two situations share many similarities, and it can be hard for the general public to understand how they differ.
Well outline these differences in this latest installment of our online book club speaking about Kimberly Williams-Paisleys book, Where the Light Gets In. She writes about her mothers experience with primary progressive aphasia.
Frontal Variant Alzheimers Disease
For about 1 in 50 people who have Alzheimers disease, the condition affects the frontal lobes of their brain during the earlier stages something that wouldnt happen until much later in most typical cases. When this happens, the condition is known as frontal variant Alzheimers disease . For more information on the different lobes of the brain and their functions, see The brain and dementia.The damage to the frontal lobes can cause:
- behavioural symptoms or
- problems with a type of thinking known as executive function .
However, most people who have fvAD will show some of both types of symptoms.A person who has fvAD is likely to show changes in their personality and behaviour. They may:
A person who has fvAD is also likely to have symptoms related to executive function and may:
- struggle with tasks which follow a series of steps for example making a cup of tea
- find it hard to think about more than one piece of information at a time when making a decision
- be easily distracted and find it hard to concentrate
- sometimes fixate on a specific thought or on something in the room
- copy other peoples behaviour.
Also Check: Senile Dementia Of The Alzheimer Type
More Atypical Than Atypical Alzheimers Disease Phenotypes: A Treviso Dementia Registry Case Report
Article type: Research Article
Authors: Gallucci, Maurizioa b * | Mazzarolo, Anna Paolaa | Focella, Luciaa | Berlin, Elisaa | Fiore, Vittorioc | Di Paola, Francescod | Bendini, Matteod | Zanusso, Gianluigie | Fenoglio, Chiaraf | Galimberti, Danielaf g | Bonanni, Laurah
Affiliations: Cognitive Impairment Center, Local Health Authority n.2 Marca Trevigiana, Treviso, Italy | Associazione Alzheimer Treviso Onlus, Treviso, Italy | Nuclear Medicine Unit, Local Health Authority n.2 Marca Trevigiana, Treviso, Italy | Neuroradiology Unit, Local Health Authority n.2 Marca Trevigiana, Treviso, Italy | Department of Neuroscience, Biomedicine and Movement, University of Verona, Verona, Italy | University of Milan, Dino Ferrari Center, Milan, Italy | Fondazione IRCCS Ca Granda, Ospedale Policlinico, Neurodegenerative Disease Unit, Milan, Italy | Department of Neuroscience Imaging and Clinical Sciences and CESI, University G DAnnunzio of Chieti-Pescara, Chieti, Italy
Correspondence: Correspondence to: Maurizio Gallucci, MD, Cognitive Impairment Center, Local Health Authority n.2 Marca Trevigiana, Treviso, Italy. E-mail: . ORCID ID: https://orcid.org/0000-0001-6329-319
Keywords: Alzheimers disease, frontal variant, magnetic resonance, neurodegenerative diseases, PET scan, posterior cortical atrophy, TREDEM
DOI: 10.3233/ADR-210009
Journal: Journal of Alzheimer’s Disease Reports, vol. 5, no. 1, pp. 365-374, 2021
Abstract