Barriers To Recognising Pain
Training for healthcare staff in recognising pain and providing adequate pain relief to patients in long-term care facilities can be limited.6,7 Pain, although highly prevalent in nursing homes, is often not documented in nursing notes 7 staff are reliant on patients self-reporting their pain.8 This is problematic for patients with dementia who may struggle to verbalise their symptoms. Lack of time to observe patients, particularly in hospital settings, can be a significant issue.8 Inadequate staff continuity can lead to isolated snapshots of what the patient is experiencing,8 rather than the full picture. Establishing a pattern of the patients pain is essential if analgesia is to be appropriately evaluated. More accurate pain assessment may come from engaging with family members or carers who know the patient well.3
Pain can be misinterpreted as behavioural disturbance. A positive association between pain and aggression or agitation has been demonstrated in several studies.3,6,7,9,10 Consequently, misidentification of pain can lead to psychotropic drugs being inappropriately prescribed.11 If pain is not successfully treated, behavioural symptoms may mask the underlying issue and exacerbate distress.
Why A New Tool Is Needed
There is evidence that the established pain assessment tools are not used in practice. An observational study of pain assessment in people with dementia in acute care found that nurses distrusted the scores obtained by pain assessment tools and preferred to use their own experience. As a consequence, they tend not to be used in everyday practice .
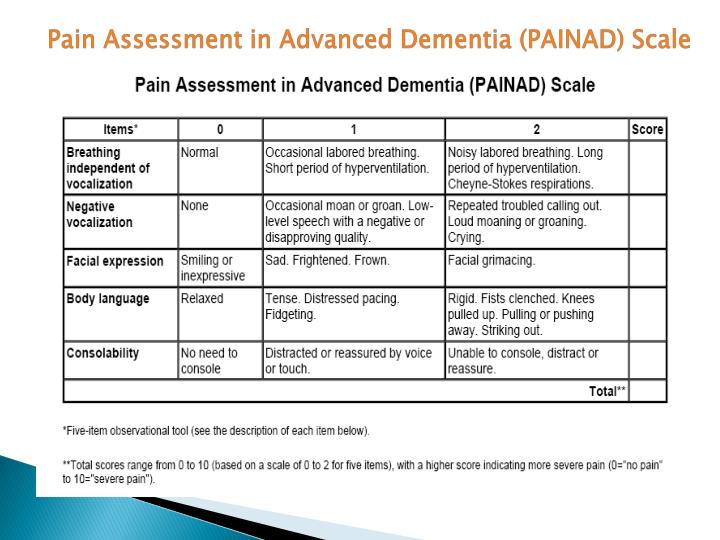
In 2012, the Abbey Pain Scale, PAINAD and CNPI were tested in acute care wards, including trauma wards, as part of a practice development project in the north west of England . The aim was to identify a pain assessment tool for people with communication problems in acute settings. The three tools were evaluated by staff after a six-week trial on their wards. All were helpful in identifying pain, but staff concluded that they all had specific issues:
- The Abbey Pain Scale was subjective and required previous knowledge of the individual
- There were issues with some PAINAD items, mainly consolability and Cheyne Stokes respiration indicating severe pain
- The CNPI did not provide clear guidance on how to interpret the scores.
Relatives and carers were involved in the project and identified behaviours that did not feature in the three tools.
Caring For Dementia Patients In Painresearcher Explores Ways That Caregivers And Health Care Professionals Can Better Assess And Treat Pain In People With Dementia
In Canada, over 430,000 dementia patients experience problems that include memory loss and the inability to communicate.
Dr. Thomas Hadjistavropoulos, a Research Chair in Aging and Health at the University of Regina, is exploring ways that caregivers and health care professionals can better assess and treat pain in people with dementia.
Because dementia patients have a hard time communicating pain, they can become agitated, said Dr. Hadjistavropoulos. As a result, health care professionals often diagnose it as a psychiatric problem and use psychotropic medications for treatment. Unfortunately, this does not lead to better care for patients. In fact, the medication can cause death among those who are frail.
With the support of CIHR funding, Dr. Hadjistavropoulos is studying nonverbal pain expressions among older patients with dementia and developing methods to assess those expressions. Rather than waiting years for his research findings to translate into widespread clinical practice, he is also trying to fast track the dissemination of this information through a social media campaign called #SeePainMoreClearly.
With this campaign, we are encouraging health care professionals to visit our SeePainMoreClearly website, and learn about how seniors with dementia communicate pain, noted Dr. Hadjistavropoulos. We are also providing an information video and hyperlinks to other websites and media stories so that family members can help identify the problem too.
- Date modified:
Read Also: What Color Ribbon Is Alzheimer’s
Impact Of Dementia On Facial Responses
Findings on the impact of dementia on facial responses to pain are surprisingly homogeneous, despite the use of different pain induction methods and the study of mixed samples of patients suffering from dementia. It has been consistently found that as pain intensity increases, facial responses intensify in patients with dementia. This clearly indicates that facial expressions in patients with dementia reliably convey pain intensity. Furthermore, the facial responses to pain in patients with dementia are the same as those in individuals without dementia.13,15,16 In terms of the strength and extent of facial responses to pain in patients with dementia, it was found that patients actually show increased facial displays of pain compared to the cognitively unimpaired.13,14 The increased facial expression of pain might suggest an intensified processing of noxious stimuli and/or a loss of inhibitory mechanisms that govern the degree to which we express pain via facial expressions. In summary, while individuals with dementia and cognitively healthy individuals express pain using the same types of facial muscle movements, individuals with dementia show more vigorous and intense responses.
Numeric Rating Scales 303133353844
Numeric rating scales are measures of pain intensity that are available in a number of ranges , with 0 representing no pain and the highest number on the scale indicating pain as bad as it could be. Participants completing an NRS are asked to choose the number that best represents the intensity of their pain. Research studies employing NRS suggest that they are appropriate for use among cognitively intact seniors as well as seniors with mild to moderate dementia., NRS have also been shown to be more reliable than VRS, particularly in patient populations with a lower educational level.
Also Check: Ribbon For Dementia
Assessment Of Neuropathic Pain
Neuropathic pain is often based on underlying diseases such as diabetic neuropathy, after stroke and amputation. Assessing this form of pain in dementia is extremely challenging. The assessment of central neuropathic pain, which is defined as pain caused by a lesion, or dysfunction of the central nervous system, is even more complex. Approximately 35% of stroke patients suffer from post-stroke central neuropathic pain. Because this deafferentiation also takes place in VaD, it has been suggested that central neuropathic pain is by far the most undertreated type of pain in patients with dementia. The assessment and treatment of this type of pain is of high clinical relevance, but it has hardly been described in the literature, most likely because it requires assessment and treatment approaches that differ from those of other types of pain. In 2004, the European Federation of Neurological Societies Panel on Neuropathic Pain published guidelines on neuropathic pain assessment that included thorough sensory bedside testing in individuals with neuropathic pain. This guidance would provide a useful basis for an assessment tool for neuropathic pain. However, as far as the authors are aware, no such instrument has been developed to date.
Potential Biases In The Overview Process
We checked further available data when readily available, such as in supplementary tables online but we did not communicate with the authors to obtain missing data. This may have introduced publication bias.
In our assessment of the reliability and validity of the tools, we did not attempt a meta-analysis we are aware that studies had been counted in various reviews and their results could have been counted more than once. However, we do not believe this to be an issue for our narrative synthesis.
Our search did not specifically target reviews reporting on the feasibility or clinical utility of the tools thus our evidence may be more limited on these aspects than it might have been otherwise.
We attempted to minimise bias in the review process by involving a review team with diverse expertise by having each review assessed independently by at least two members of the team, and the whole team of reviewers involved at every stage of the process by not excluding reviews on the basis of our assessment of their quality.
Also Check: Senile Vs Dementia
New Developments In Nonpharmacological Management
Complexities of pain in older persons with dementia necessitate a comprehensive pain management approach that encompasses more than pharmacotherapy. For years, clinical practice guidelines have recommended incorporation of nonpharmacologic approaches as part of the pain management plan for older adults, but recent concern related to opioid use for chronic pain has increased attention to the effective use of nondrug approaches. Incorporation of nondrug techniques involves careful consideration of the unique patient circumstances, patient preferences, and evidence of effectiveness and guidance for selection of these interventions in the frail older person with dementia. Although evidence is growing, the majority of evidence for nondrug pain interventions has been conducted in cognitively intact older adults because those with dementia are typically excluded from most randomized control trials . Evidence is accumulating on nondrug interventions to manage behavioral and psychological symptoms of dementia , but few studies focus specifically on pain as the outcome of interest.
The Opioid Epidemic In Dementia
While the overall use of opioids in community-dwelling elderly people increased from 2006 to 2013,42 declining trends for opioid prescribing were reported in nursing home patients with and without dementia from 2011 to 2017,40 potentially reflecting a change in prescribing practice as a result of increased attention for the prevention of opioid addiction and opioid overdose deaths associated with the opioid epidemic in the USA. Despite an apparent shift in prescribing practice, the likelihood of receiving opioid treatment remains significantly lower in people with dementia compared to people without dementia across care settings, particularly in people with severe cognitive impairment.
You May Like: Do Parkinsons And Alzheimers Go Together
Assessment Of Methodological Quality Of Included Reviews
The PRISMA guidance on systematic reviews explains how, in carrying out a systematic review, it is important to distinguish between quality and risk of bias and to focus on evaluating and reporting the latter . The authors encourage the reviewers to think ahead carefully about what risks of bias may have a bearing on the results of their systematic reviews . In our meta-review, the risk of bias may reside in each review considered for inclusion, as well as in the original studies that comprise that review. We did not access the studies to be able to accurately judge their quality or risk of bias. In terms of each review, we assessed risk of bias in terms of how the review was conducted and the criteria applied for inclusion/exclusion. Critical appraisal was carried out by two independent reviewers, using the AMSTAR systematic review critical appraisal tool . Critical appraisal and evaluation of potential bias was carried out at the time of data extraction, after screening was completed on the basis of the inclusion criteria.
Pain In Other Types Of Dementia
There have been few studies on pain in different subtypes of dementia such as VaD, FTD, or Lewy body dementia. In VaD, white matter lesions lead to several disconnections between areas of the brain in a process known as deafferentiation. This is thought to be responsible for an increase in the motivationalaffective aspects of pain. This type of pain, also called central neuropathic pain, occurs frequently in patients who have had a stroke and there is some clinical evidence that this type of deafferentiation pain might also occur in VaD.,
You May Like: Andrea Mitchell Speech Problems
Alternative Ways To Assess Pain Are Needed For Individuals With Dementia
Individuals with dementia are at particular risk of untreated pain because their ability to recognize, evaluate, and verbally communicate their pain gradually decreases across the course of dementia . As a consequence, alternative ways to assess pain that do not rely on the capacity to self-report pain are needed for this ever growing group of vulnerable individuals in order to ensure that pain can be accurately assessed in a timely fashion.
Pain assessment in dementia: self-report
Although the validity of self-report ratings of pain declines across the course of dementia, self-report might still be an appropriate method for pain assessment in the early stages of dementia, when the patient is still able to recognize and verbalize pain . However, when assessing self-report of pain in dementia, certain precautions have to be taken, such as using simple scales , repeating the question and the instructions on how to use the scale, and leaving adequate time to respond . Moreover, a more individualized approach should be used that takes into account the specific neuropsychological deficits of the individual as well as his/her cognitive recourses. This can be achieved by a short neuropsychological screening. When dementia progresses to moderate and severe stages, self-report of pain is often absent . Clinicians should be aware of this and should not interpret a lack of self-reported pain in individuals with severe cognitive impairments as an indicator of a pain-free state.
Openuse A Tested Tool To Assess Pain

A number of different resources are available to help care staff establish whether a person with dementia is in pain, especially if the person cannot tell you in words. One example is the Abbey Pain Tool . The tool asks us to look for other ways in which the person may be letting us know they are in pain, perhaps through screwing up their face or rocking back and forth.
The Abbey Pain Tool can be used by care staff and suggests six possible signs of pain in a person with dementia:
Using a tool like this can help in your assessment of the persons pain. It can guide you to the cause of the pain, its severity, when it occurs and what helps to make the pain better or worse. It will also give you evidence to show a nurse or doctor if the pain is present or gone. If the pain is still present, always inform a doctor or nurse to review the persons medication.
You May Like: What Color Ribbon Is Alzheimer’s
Overall Assessment Of The Tools
There seemed to be a general consensus among the reviewers that the current evidence on validation and clinical utility of the tools is insufficient . The overall conclusion was that there is a need for further psychometric testing of each tool. Two reviews recommended that the focus should be on studying existing scales rather than creating new ones , although one review also suggested that there may be a need to revisit the tools conceptual foundations .
Recommendations for further research and testing of the tools included the involvement of culturally diverse populations and the provision of scoring methods and guidelines for interpretation in the evaluation of the scale . Finally, a need for research emerged to link assessment with treatment algorithms .
Some of the reviews also concluded with recommendations for practice, for example: the use of at least two different pain assessment approaches at the same time in clinical practice and two different tools in research the importance of a comprehensive approach to pain assessment beyond the use of tools the need to involve social workers in regular holistic multidisciplinary pain assessment , with training in the use of the scales .
Verbal Rating Scales 323335384243
Verbal rating scales, or verbal descriptor scales, are self-report scales that require the individual to choose the descriptor that best matches his or her level of painfor example, no pain, slight pain, mild pain, moderate pain, severe pain, extreme pain, and pain as bad as it could be. Each of these descriptors corresponds to a number, often found on the back of the scale, with higher numbers corresponding to more intense descriptors of pain. Research comparing five different self-report measures, including a simple VRS, suggests that simple VRS are appropriate measures of pain intensity in cognitively intact older adults as well as in older adults with mild dementia. Moreover, research has demonstrated that the VRS ranked higher than various numeric and/or visual analogue scales for both younger and older adults in terms of scale success, internal consistency, reliability, sensitivity, and preference.
Recommended Reading: What Is Vascular Dementia Life Expectancy
Medicating For Pain Control
While non-drug approaches are important, many people will still benefit from prescribed pain medications. If you’ve ruled out other causes of behaviors , and you’ve determined that the person is likely experiencing pain, getting a prescription for pain medicine is a good idea.
Be wary of pain medications that are ordered on a PRN basis. Because the person with dementia might not be able to express their pain well, or might not be aware of a gradual increase in discomfort until she’s in a lot of pain, PRN pain medications are more likely to result in poorly controlled pain. Either the person doesn’t ask for it so she doesn’t receive it, or she gets it later than would have been ideal and her pain is beyond what’s normally controllable by the medication and dose prescribed. If at all possible, a routine order for pain medicine is preferable for the person with dementia.
Although family members may express the worry of possible addiction to pain medications, this is usually not a primary concern since drug-seeking behavior is not common in people with dementia. Additionally, many value quality of life which is likely to improve with adequate pain control.
Feasibility And Clinical Utility
The feasibility of a tool is its applicability in daily practice, including aspects such as ease of use and time to administer it, while clinical utility is the usefulness of the measure for decision making, i.e. to inform further action, such as the administration of analgesics . Data on feasibility and clinical utility of tools were very limited . Often data were not available in the reviews, or when data were available, it often pertained to a lack of data in the original studies . More specifically: feasibility data were completely absent for six tools clinical utility data were completely or substantially absent for seven tools . For four tools reviewers explicitly noted that claims of feasibility were made from the authors of the study without supporting evidence . There were also two instances of conflicting data on clinical utility and feasibility from the different reviews, possibly due to an ambiguous reference to different versions of the same tool.
Specific evaluation for feasibility appears to have been carried out only for three tools – CPAT, Mahoney Pain Scale, and Pain Assessment Scale for Use with Cognitively Impaired Adults in the first two of these cases the evaluation was done by use of questionnaires. It also appeared that users of the Abbey Pain Scale were asked for feedback in the context of the psychometric testing of the tool. In was unclear whether the ADD Protocol was also assessed for feasibility.
Recommended Reading: Dementia Ribbon Color