Could This Be You
Youre doing your best to make sure your loved one is cared for properly but
1. Some days seem to fly by without you getting anything done2. Other days go really slowly and you worry about them getting bored.3. Whatever kind of day it is, you never have a minute to yourself
Creating a simple structure to each day, could help you avoid these really common pitfalls and maybe even enjoy life a little more! And dont worry, it isnt hard and it wont take long to do.
Once Written Keep For Reference
If you have a care plan made by an organisation you should be able to have your care plan printed out on paper for you to keep at home. If somebody makes one for you and youre not given a paper copy, you can ask for one.
Your care plan may also be stored on the care organisations/providers computer or whatever filing system they may use.
You as the individual must make sure you express whats important to you and that youre happy with any decisions that are put into the plan. In some cases your needs and wants may not be possible to achieve. But unless your family, carers, health and social care workers know what you want, they cant tailor it to your wishes.
All the information provided should be kept private. It should be seen only by you and the people who give you the care or support.
By making a care plan you and other carers and support groups can look back and read the plan to see if it is working and you are receiving the best care that is possible.
You are able to change your personal care plan if you wish. If a doctor or nursing agency has written it for you, ask to see it at least once a year, This helps to make sure you are getting the best from your care plan and that any changes in your wishes are considered.
How To Create A Care Plan For A Dementia Patient
A care plan for a patient with dementia, no matter where he is living, ensures the highest quality of life for him despite this diagnosis. Since each person with dementia displays different behaviors, has specific interests and different strengths, the care plan is person centered. His dementia progresses over time. Because of this, it is more difficult to assess the dementia patients needs and preferences as time goes on. Learn all you can while the dementia person is able to communicate. The outcome of the care plan makes the dementia patients life as happy and satisfying as possible.
-
Get an accurate history about the patient with dementia. This includes current medications, strengths, weaknesses, current and past interests, former jobs, and a thorough family history.
-
Observe the dementia patient. Make note of how she reacts to her environment, especially triggers for unwanted behavior.
-
Meet with all team leaders who are responsible for every aspect of the dementia patients care. The teams include nursing, social work, therapy, activities, family members and the dementia patient, unless the meeting will upset him.
-
Together write a care plan that includes the best ways to care for this person. Include specific goals for each team and ways to accomplish these goals. Assign team members to each goal. Make sure to get everyones input.
-
Update this care plan every three months or sooner if the dementia patients condition changes.
Read Also: Alzheimer’s Awareness Ribbon
Signs And Symptoms Of Dementia
Put Your Care Plan Into Action
The purpose of having a care plan and care team in place is to promote communication and unified efforts for the welfare of both the care recipient and the caregiver. A divide and conquer approach to caregiving is far more sustainable than a sole caregiver taking on all these responsibilities. Keep in mind that a care plan is an ever-evolving tool. Professional care providers use similar organizational techniques and regularly evaluate and update each clients plan of care to ensure all their needs are being met. Finding the best solutions may take some trial and error, and your loved ones needs are likely to increase over the long term, so flexibility is key.
Even if your loved one does not currently need a care plan, beginning to put these pieces of the puzzle into place can save valuable time and help you avoid a great deal of stress later on. They dont necessarily need to share their detailed financial statements or medical records with you just yet, but asking them to put together an updated file containing this information can be incredibly helpful in the event of an emergency. This goes for medications, health information and legal documents as well. Should something happen, you will know where to access the materials you need to make care decisions quickly and confidently.
To assist you in devising a customized care plan, AgingCare has created a free guide for you and your family to use during the planning process.
You May Like: Louie Body Dementia Hereditary
Help With Legal Needs
Families who cannot afford a lawyer can still prepare documents and express their wishes in advance. Samples of basic health planning documents are available online. Area Agency on Aging officials may provide legal advice or help. Other possible sources of legal assistance and referrals include state legal aid offices, state bar associations, local nonprofit agencies, foundations, and social service agencies.
Visit the National Hospice and Palliative Care Organization for free sample documents.
For help with legal advice, contact the Eldercare Locator.
Lasting Power Of Attorney
Any one of us can give named individuals the power to make specific decisions on our behalf, if there comes a time when we are unable to make them ourselves.
This is called making a Lasting Power of Attorney . A person chosen to make the decision is called an ‘attorney’. A person may choose more than one attorney. Most often attorneys will be family members. They might also be friends, or solicitors.
Attorneys must make decisions in the person’s best interests. If you think an attorney is not doing this you should report it to the Office of the Public Guardian.
There are two types of Lasting Power of Attorney: one relates to property and affairs, the other to health and welfare.
You May Like: How Long Does The 7th Stage Of Alzheimer’s Last
How To Create A Daily Care Plan Checklist For Dementia Patients
If you are caring for someone with dementia, your role in managing their daily routine will increase as the disease progresses. A person with dementia will need a caregiver’s support to organize their daily routine. Planned activities can often reduce anxiety and improve the mood of your loved one with dementia. Whether the primary caregiver is a loving partner, a close relative, or a trained professional, creating a dementia care plan enables the individual to remain in control of their daily life. Daily care planning will help you understand what needs to be done and when.
An effective dementia care plan requires assisting individuals with their everyday tasks, knowing the medication they need, and ensuring safety and security. It is necessary to explore and examine the world from their point of view and the life they led before they developed dementia. Taking a holistic approach and knowing the person’s likes, dislikes, moods, and character establish the best ways the caregiver can assist the individual in continuing to achieve the activities of daily living, adapting the care given as needs change.
The Concept Of A Personalised Care Plan For Dementia
With dementia, its fair to say that its sometimes difficult to truly see the individual. Instead, often people see the disease. As such, they miss who this individual was in the past, who they are now, and the future they have ahead of them. Yet, we firmly believe that it is only through considering the dementia patient as an individual that we can fully care for them, helping them gain meaning and contentment in daily life.
For us, there is no one-size-fits-all approach that works when creating a care plan for the individual with dementia. There cannot be a single set of routines to apply! Instead, this person, their needs, and their past and future, need to be considered. Thats the essence of a personalised care plan.
Also Check: Alzheimer Awareness Ribbon Color
Activities For Adults With Dementia
Keeping busy stimulates the brains of elderly people with dementia while boosting a sense of usefulness and accomplishment. But they lose the ability to select satisfying activities and follow through on them so you need to initiate things to do for the person with dementia you are caring for. Too much idle time can make anyone feel lonely and unproductive, raising the risk of depression, agitation, and anger.
Statements About Future Needs And Wishes
People can say what they would like to happen if they lose capacity to make decisions in the future. This can cover care, support and treatment. These are sometimes called ‘advance statements’.
While these statements don’t need to be written down, it is best to do this. It is also important to decide the best place to keep these statements so that the right people can refer to them when needed. For example, the GP could keep a copy as could a relative or friend, and it might be attached to a care plan.
Here are some examples of statements people might make in case there is a time in the future when they can’t make these decisions:
- I would want to stay in my own home as long as possible.
- I would only want to be supported with personal care by women.
- I would want to continue to have a glass of wine with my evening meal.
- I would want to keep to a strict halal diet.
- I would want to get out as much as possible.
- I would like to carry on going to garden centres and my church.
- I would not want to share a room if I move to a care home and I would want to bring my photos and music.
- I would want any treatment that could reduce the effects of dementia.
- I would want you to involve my same-sex partner and my daughter in decisions about me.
- I would not want my father visiting me and being involved in my decisions.
- I would not a faith leader visiting me when I am dying.
Recommended Reading: What Color Is The Alzheimer’s Ribbon
Advance Decisions To Refuse Treatment
Some advance statements could be about medical treatments that a person would not want, were they to lose capacity to make decisions about these in future. These are called ‘Advance Decisions to Refuse Treatment’. They have a special status in law.
Some examples include:
- I would not want a blood transfusion because of my religion.
- I would not want any further chemotherapy for my cancer, in the event of my cancer reaching stage IV.
Like other advance statements they do not always have to be written down. If a person with dementia tells a member of the care team what treatment they would not want, it is a good idea for them to make a note in the person’s records, and share this information in best interests decision-making meetings.
Advance Decisions to Refuse Treatment must, however, be written down, signed and witnessed if the person is refusing, in advance, a treatment that might keep them alive feeding or attempts at cardio-pulmonary resuscitation). The person must also make a statement which shows they understand that the decision to refuse the treatment may put their life at risk.
People who are physically unable to sign their name can still make advance decisions to refuse life-sustaining treatment. For example, a person paralysed from the neck down can tell someone to sign on their behalf. The witness would then sign to say this had happened.
It is good practice to make sure that the person’s GP has a copy of any Advance Decisions to Refuse Treatment.
What Is A Care Plan
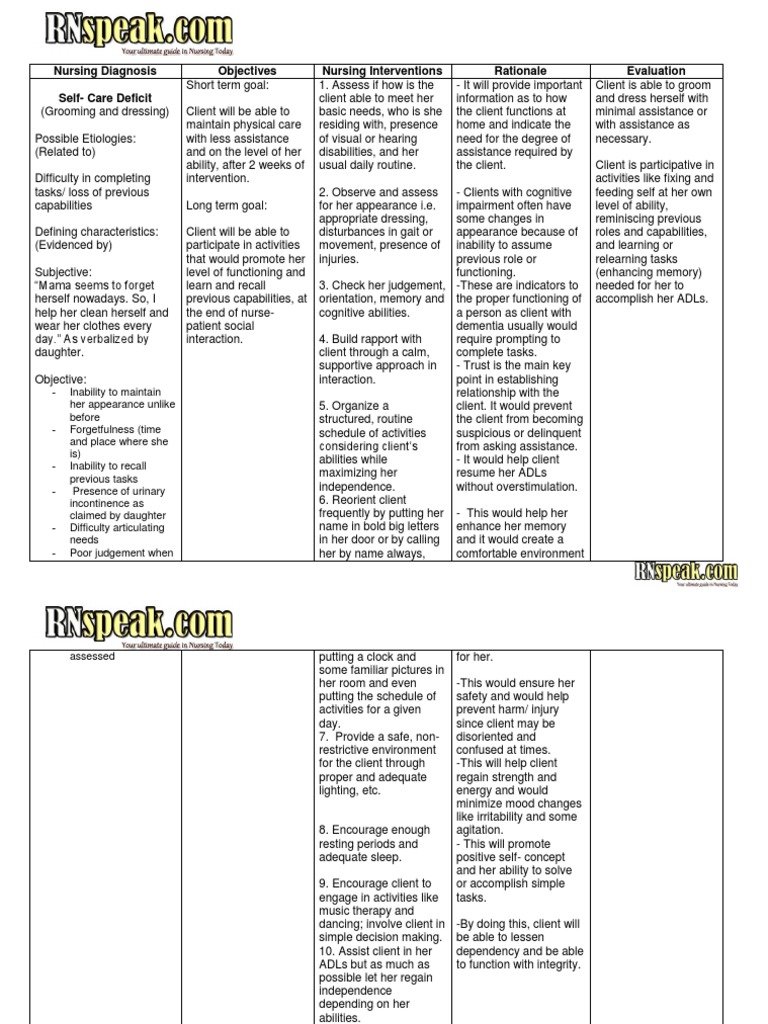
A care plan is a form pdf icon that summarizes a persons health conditions and current treatments for their care. The plan should include information about:
- Health conditions
- Emergency contacts
- Caregiver resources
You can ask the doctor of the person you care for to help you complete the care plan. At that time, you can also discuss advanced care plan options such as what follow-up care is necessary, end of life care options, and resources that are available to help make things easier for you as a caregiver. Try to update the care plan every year or if the one you care for has a change in health or medications to keep the care plan current, and remember to respect the care recipients privacy after reviewing their personal information.
You May Like: Multi Infarct Dementia Treatment
Care Plans Help Both Older Adults And Caregivers
Developing and maintaining a care plan will help you balance both your life and that of the person to whom you are providing care!
Are you a caregiver for someone with Alzheimers disease, dementia, or another chronic health condition? Caregivers are often family members or friends of a person who is in need of care. Caregivers may manage everything from medications and getting dressed in the morning to doctor appointments, social events, and meals.
Special Attention To Challenges Posed By The Covid Situation
Planning for care should also include precautions required to keep the person safe from the COVID infection and also ensuring that care remains suitable in the current constraints. The precautions and adjustments required may need frequent review based on the latest requirements and recommendations, and the implementation will depend on the stage of the persons dementia.
Precautions at home are required on an ongoing basis to protect seniors from the COVID infection, like following the advice that they stay at home and also measures like use of masks, social distancing and hand washing to protect them from infection. This is very important because COVID is more problematic for seniors with dementia and also as COVID is very infectious and can be spread even by persons who dont have any symptoms. Caregiver alertness is required continuously.
Persons in early stages of dementia may be able to understand about COVID, but may not always remember to take required precautions and may need to be reminded/ assisted for these.
When care starts including helping in daily activities, caregivers will need to be even more cautious about wearing masks and taking other precautions and also be more reassuring to the person as the person may find these changes odd and disorienting.
Also Check: Alzheimer Ribbon Color
Find Out How Much Money And Coverage Is Available For Care
Take a look at any insurance plans, long-term care plans and other dementia care financing options so you know how much money your loved one has available. If this step is overwhelming, find a professional, such as a social worker experienced in dementia care, with the expertise to guide you. In some cases, the details of coverage for dementia care could determine where your loved one will live.
Identify Care Needs And Set Goals Of Care
The next step revolves around two central questions:
- What is lacking or being overlooked in your loved ones current routine?
- What objectives would you like to help them achieve?
Based on the results of the care assessment you completed, make an ordered list of all shortcomings or concerns, placing the highest priorities at the top. Your loved ones immediate health and quality of life are of utmost importance, so if they are losing weight or not complying with their medication regimen, these problems must be dealt with first.
Even if you do not identify any flaws in their day-to-day schedule, setting goals for their wellbeing is a useful way to convey your interest in helping them thrive. For example, I want Mom to be safer in her own home, I want Dad to eat better, and I want my husband to have a higher quality of life are all excellent caregiving goals that can be achieved in numerous ways. Dont forget to include your loved ones own desires for the future when creating these objectives as well.
Read Also: What Is The Difference Between Alzheimer’s And Parkinson’s Disease
Problem : Refusing To Bathe
- Have depression
- Be embarrassed being seen naked
- Have had a previous upsetting experience
- Have fears
- Dislike being told what to do
- Build positive associations with bathing: Precede the bath with a pleasant activity and follow up with another one .
- Build pleasant associations with the bathroom, such as hanging favorite pictures there. Keep the door closed for privacy. Buy their favorite brands or scents.
- Stick to a consistent bathing routine, which becomes soothing. When you find an approach that works, try to replicate it exactly the next time.
Problem : Forgetting To Bathe
- Have memory loss that prevents them from keeping track of or caring about bathing
- Feel confusion about the sequence of steps involved
- Feel juvenile, anxious, or defensive when asked or reminded about bathing
- Stick to a consistent bathing routine. Make it the same time the person previously bathed .
- Dont remind or even mention how long its been since the last cleanup. Instead of arguing, proceed with bath preparations.
- Dont ask, Did you shower? or Would you like to shower now? Get everything ready and invite the person in: Look, your bath is ready. I know how you love your evening bath.
Also Check: Alzheimer’s Purple Ribbon