Frontotemporal Dementia Versus Psychiatric Disorders
When behavioral symptoms predominate, people with FTD who become ill in mid-life may be confused with patients who have late life depression. When the onset is in younger persons, the FTD may be confused with schizophrenia or bipolar disorder. Repetitive compulsive behaviors are very common in bvFTD, and some patients may initially be given the diagnosis of obsessive-compulsive disorder. Since the history and exam of a person with a psychiatric disorder and a person with FTD may look very similar, neuropsychological testing and a brain image may help clarify the picture. MRI can help rule out other diseases and support a diagnosis of FTD.
What Is Frontotemporal Dementia
Frontotemporal dementia , a common cause of dementia, is a group of disorders that occur when nerve cells in the frontal and temporal lobes of the brain are lost. This causes the lobes to shrink. FTD can affect behavior, personality, language, and movement.
These disorders are among the most common dementias that strike at younger ages. Symptoms typically start between the ages of 40 and 65, but FTD can strike young adults and those who are older. FTD affects men and women equally.
The most common types of FTD are:
- Frontal variant. This form of FTD affects behavior and personality.
- Primary progressive aphasia. Aphasia means difficulty communicating. This form has two subtypes:
- Progressive nonfluent aphasia, which affects the ability to speak.
- Semantic dementia, which affects the ability to use and understand language.
A less common form of FTD affects movement, causing symptoms similar to Parkinson disease or amyotrophic lateral sclerosis .
What Causes Frontal Lobe Dementia/frontotemporal Dementia
Scientists dont know what causes the majority of cases of frontal lobe dementia. However, abnormal accumulations of proteins, either tau or TDP-43, have been found during autopsy in the brains of people who suffered from frontal lobe dementia.
Furthermore, a number of genes linked to the abnormal production of these proteins have been identified and are responsible for the disease in the 15 to 40 percent of people who suffer from a hereditary form of it.
Also Check: Does Meredith Grey Get Alzheimers
You May Like: Dementia Ribbon Colors
Managing Behavior Changes In Ftd
Behavior changes associated with bvFTD can upset and frustrate family members and other caregivers. Understanding changes in personality and behavior and knowing how to respond can reduce frustration and help provide the best care for a person with FTD.
Managing behavioral symptoms can involve several approaches. Here are some strategies to consider:
- Try to accept rather than challenge someone with behavioral symptoms. Arguing or reasoning will not help, because they cannot control their behaviors or see that they are unusual or upsetting to others. Instead, be as sensitive as possible and understand that its the illness talking.
- Take a timeout when frustrated take deep breaths, count to 10, or leave the room for a few minutes.
- To deal with apathy, limit choices and offer specific choices. Open-ended questions, such as What do you want to do today? are more difficult to answer than specific ones, such as Do you want to go to the park or for a walk?.
- Maintain a regular schedule, reduce distractions, and modify the environment to reduce confusion and improve the persons sleep.
- If compulsive eating is an issue, consider supervising eating, limiting food choices, locking cabinets and the refrigerator, and distracting the person with other activities.
To ensure the safety of a person and his or her family, caregivers may have to take on new responsibilities or arrange care that was not needed before.
What Are The Prognosis And Options For Treatment
FTD worsens over time and impairs the individuals ability to live and function independently. Although there is no cure for FTD, there are medications that can help control the behavioral symptoms of the disorder. With an accurate diagnosis, unnecessary medications can be removed that might otherwise worsen the disease symptoms.
You May Like: What Color Represents Dementia
Recommended Reading: Does Diet Coke Cause Alzheimer’s
The Future Of Ftd Treatment
Researchers are continuing to explore the biological changes in the body, including genetic mutations and proteins, that lead to FTD and identify and test possible new drugs and other treatments. They are also developing better ways to track disease progression, so that treatments, when they become available, can be directed to the right people. Clinical trials and studies are underway to advance these efforts. People with FTD and healthy people may be able to participate. To find out more, talk to your health care provider or visit the Alzheimers.gov Clinical Trials Finder.
Why Is Ftd Hard To Diagnose
Frontotemporal dementia is much less common than other types of dementia and often has different early symptoms. This means FTD can be hard for doctors to diagnose as they may not recognise its symptoms as dementia.
Most changes in behaviour or personality caused by FTD may not be very obvious at first. These kinds of symptoms for example, risk-taking, loss of social or sexual inhibitions, or obsessive behaviour can sometimes look more like the person is going through a difficult or emotionally-challenging time.
Also, if the person is under 65, doctors may not expect to see dementia in someone so young.
Even if changes in behaviour are understood as medical symptoms, they may be mistaken for depression, schizophrenia or obsessive-compulsive disorder. Problems with language or movement may also be misdiagnosed.
If a person is showing some of the symptoms mentioned in this factsheet, they may want to ask their doctor to explore FTD as a possible diagnosis especially if they have family members with the condition.
Don’t Miss: What Color Ribbon Is For Alzheimer Disease
The Aftd Helpline: A Vital Source Of Support And Information
The FTD journey can be filled with many questions. Having a place to turn to for answers and reliable help is important.
The AFTD HelpLine is available for anyone looking for information, resources, and support related to FTD. Trained members of AFTDs staff are available to answer calls and emails with available research and the most current resources. HelpLine staff ensure that each inquiry receives an individualized, supportive, and timely response.
Whether its a question about managing symptoms, accessing local resources and services, or updates on FTD research initiatives, the AFTD HelpLine is available to assist with your inquiries.
If you have a question about living with FTD or caring for a loved one who is diagnosed, please contact our HelpLine by phone at or via email at .
For more information on the HelpLine and the additional AFTD support services, visit our Resources page here.
Stay Informed
Sign up now and stay on top of the latest with our newsletter, event alerts, and more
Recommended Reading: Does Bob Knight Have Dementia
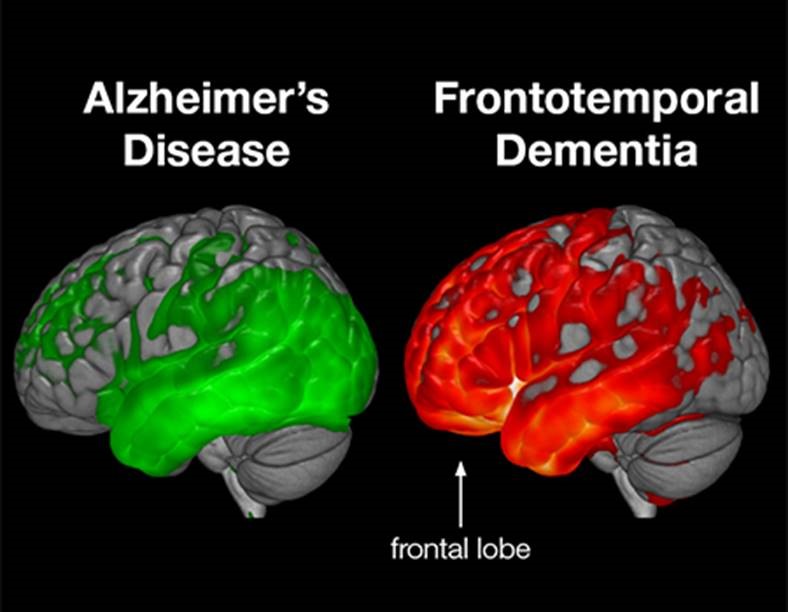
Differences Between Ftd And Other Dementias
FTD differs markedly in several ways when compared to other dementias, especially Alzheimerâs disease:
- FTD is characterized by cerebral atrophy in the frontal and anterior temporal lobes of the brain, while Alzheimerâs affects the hippocampal, posterior temporal, and parietal regions.
- The neurofibrillary tangles, senile plaques, and Lewy bodies present in the brains of Alzheimerâs and other dementia patients are absent.
- Alzheimerâs patients experience severe memory loss. While FTD patients exhibit memory disturbances, they remain oriented to time and place and recall information about the present and past.
- FTD patients, even in late stages of the disease, retain visuo-spatial orientation, and they negotiate and locate their surroundings accurately.
- Intellectual failure in FTD is distinctly different from that of Alzheimerâs patients. Results of intelligence tests are normal in those with FTD until the point in the disease when disinterest results in lower scores.
- Life expectancy is slightly longer for FTD.
You May Like: Alzheimer’s Disease Ribbon Color
Outlook For Frontotemporal Dementia
How quickly frontotemporal dementia gets worse varies from person to person and is very difficult to predict.
People with the condition can become socially isolated as the illness progresses. They may not want to spend time in the company of others, or may behave in rude or insulting ways.
Home-based help will usually be needed at some stage, and some people will eventually need care in a nursing home.
The average survival time after symptoms start is around 8 to 10 years. But this is highly variable and some people live much longer than this.
If you or a loved one has been diagnosed with dementia, remember you’re not alone. The NHS and social services, as well as voluntary organisations and specialist support groups, can provide advice and support for you and your family.
Core Ad Csf Biomarkers: A142 A142/a140 Ratio T
The currently most used panel to assess pathological markers of neurodegenerative brain disease is a combination of amyloid- of 42 amino acids , total tau protein , and hyperphosphorylated tau in CSF . They are not, in fact, used for the diagnosis of FTD, but rather to make the diagnosis of AD less likely when doubt exists. A CSF biomarker profile characteristic for AD, with good diagnostic accuracy , shows decreased A142 values, in combination with increased T-tau and P-tau values . Some patients do not completely match this typical AD CSF profile. As amyloid pathology is measurable much earlier in the disease process than tau pathology, there may be an isolated decrease in A142 in early disease stages . CSF tau markers are more strongly associated with cognitive decline and disease progression in AD than A142 . The opposite may also be true, as between-individual variations in total A production or secretion from neurons and variations in CSF dynamics may cause A142 to fall within a normal range, while underlying amyloid pathology is present .
To further improve diagnostic performance for AD, the use of the A142/A140 ratio has been proposed with good results , improving accuracy with 1436% compared to A142 alone . An isolated decrease in A142 is more specific to AD, while a global decrease in both A isoforms may be correlated with subcortical damage in general or may even be due to interindividual variability .
You May Like: Dementia Ribbon Colors
You May Like: How To Change Diaper Of Dementia Patient
Can Adhd Medication Cause Dementia
Proper use of ADHD medications, like Adderal and Ritalin, is not associated with a greater risk of dementia.
But a 2018 study suggests that abuse of Adderall by people who do not need the drug is associated with at least temporary memory problems. Healthy college students sometimes take Adderall to heighten their focus when studying, and others take it for work or recreational purposes.
Who Gets Frontotemporal Dementia
FTD can affect anybody. It typically affects people at a younger age than Alzheimers disease, with symptoms beginning in the 50s or 60s, and sometimes younger.
Almost a third of people with FTD have a family history of dementia. However, only about 10-15% of cases have familial FTD, in which a gene mutation is passed on that causes the disease.
The genetic basis of FTD is not fully understood and is actively being researched.
Also Check: Alzheimer’s And Dementia Ribbon
What Are The Stages Of Frontotemporal Dementia
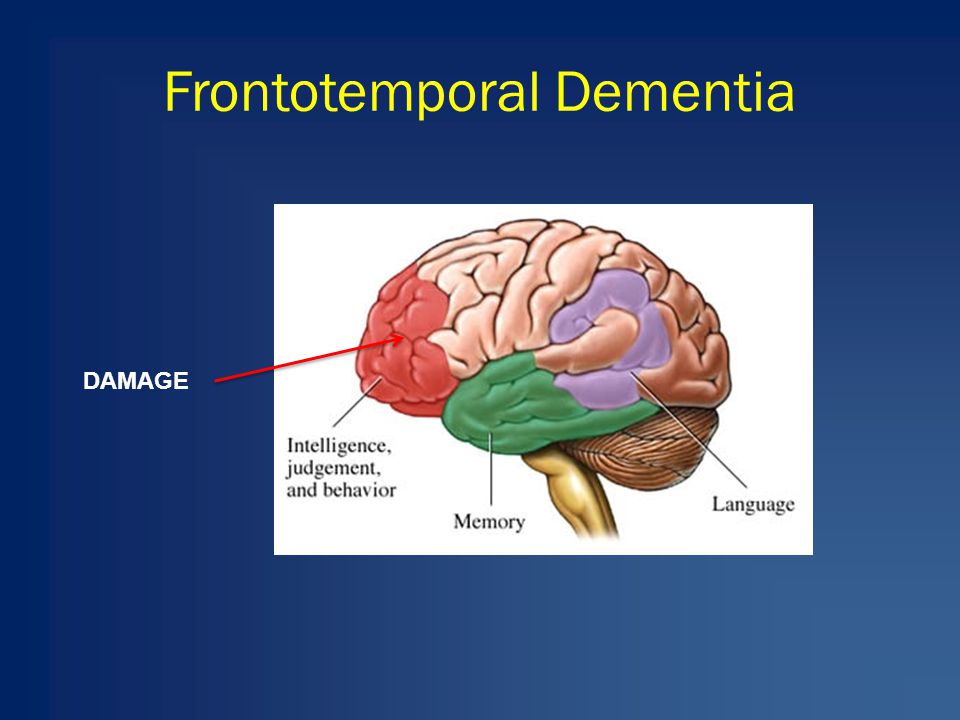
On the surface, Joseph, Barbara, and Lloyd may not seem to be experiencing related changes. Each of them, though, turned out to be in the early stage of frontotemporal dementia . FTD is the diagnosis for about 5 percent of people with major neurocognitive disorders . About 70 percent of cases begin before age 65, so it is a more common dementia among the young old. FTD involves degeneration of the frontal and temporal lobes of the brain. The frontal lobes are important regulators of behavior and the temporal lobes assist in our understanding and expression of language. The symptoms of FTD, therefore, include major changes in behavior, impairment of language, or both.
People diagnosed with FTD and family members often ask What stage of dementia is occurring? and the answer to this question can be useful in knowing what to expect in the future. FTD often begins during years when adults expect to be healthy and productive. The average course of the disease takes 6 to 8 years after diagnosis, so patients and their families must confront very serious and increasingly difficult needs. Detailed and complex timelines of the stages of FTD are not very accurate, but it is useful to think of the development of FTD through early, middle, and late stages. Lets look at the stages of frontotemporal dementias to see how these related disorders evolve:
What Do The Terms Mean
One of the challenges shared by people living with these disorders, families, clinicians, and researchers is what terminology to use. Here, we have used the term frontotemporal disorders to characterize this group of diseases and the abbreviation FTD, which is commonly used to refer to them. Other terms used include frontotemporal lobar degeneration and frontotemporal dementia, but it’s important to note that with some frontotemporal disorders, the primary symptoms are problems with speech or movement, rather than dementia symptoms. Physicians and psychologists diagnose the different forms of FTD based on a persons symptoms as well as the results of brain scans and genetic tests.
You May Like: Alzheimers Awareness Ribbons
When To See Your Gp
Talk to your GP if you think you have early symptoms of dementia. If you’re worried about someone else, encourage them to see their GP. You could suggest going with them.
The GP can do some simple checks to try to find the cause of your symptoms. They can refer you to a memory assessment service or another specialist for further tests if needed.
The Role Of Specialists
Many primary care physicians are uncomfortable making the diagnosis of FTD. Given the uncommon nature of the condition, and the implications of an incorrect diagnosis, it is reasonable to refer those suspected of having FTD to a specialty center in cognitive disorders. Most of these are directed by neurologists, though an interested geriatric psychiatrist or geriatrician may also be appropriate. Psychiatrists are helpful when behavioral or emotional problems are predominant. Geriatricians are desirable in older FTD patients with concurrent medical comorbidities.
Some individuals seek rehabilitation services. These are appropriate when there are functional disabilities in communication , mobility or self-care . Cognitive therapies are sometimes appropriate when specific tasks need to be learned. A referral for behavioral management strategies can also be helpful for caregivers since most individuals with FTD are more functional in a structured, consistent environment.
Don’t Miss: Does Diet Coke Cause Memory Loss
What Are The Causes Of Frontotemporal Dementia
The cause of FTD is not known, and may differ between individuals. In about half of FTD patients, a normal brain protein called tau accumulates abnormally and forms deposits. In others, a separate protein known as TDP43 accumulates in the same way.
Unlike other dementias, FTD is highly heritable. Approximately 40% of individuals with FTD have an affected family member. In these individuals, FTD is usually caused by changes in one of their genes.
The diagnosis may be confirmed after death with a brain autopsy. Genetic testing can help reveal an underlying mutation responsible for FTD in about 40% of patients.
What Is The Outlook For Frontotemporal Dementia
In the early stages, the symptoms and signs of frontotemporal dementia can be cared for and treated with good results. Late-stage frontotemporal dementia can take years to develop. As the disease progresses, 24-hour care may become necessary.
Frontotemporal dementia shortens a persons life span. The condition will eventually cause a person to have difficulty with bodily functions such as:
- swallowing
Don’t Miss: Dementia Color Ribbon
How Is Frontal Lobe Dementia Diagnosed
General practitioners or health professionals are unable to diagnose frontal lobe dementia with a single test alone. Instead, diagnosis usually requires a multifaceted approach to first rule out other conditions and diseases. Following this, GPs and health professional may recommend a series of tests to aid in diagnosis.
Alzheimers Association cites several tests that are commonly used to diagnose frontal lobe dementia. These include:
- Blood tests to help identify other possible causes.
- Genetic testing may be recommended to determine whether a persons condition is caused by a specific gene.
- Neuropsychological testing to check your judgement and memory skills, and help determine what type of dementia you may have.
- Brain imaging to examine the brain and check for tumours or blood clots. If further tests are needed, more specialised brain scans will be carried out, such as a positron emission tomography or a single photon emission computerised tomography to measure the persons brain activity.
- Magnetic Resonance Imaging to give GPs and health professionals a detailed image of your brain to assess any affected areas or damage.
- Computerised Tomography scan which creates images of your brains in layers to enable a more thorough examination.
What Other Things Help
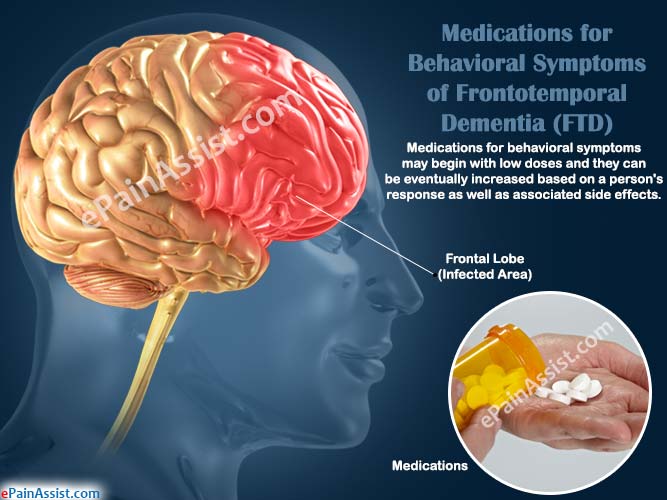
In addition to medications, there are various ways to help a person with bvFTD. Research has shown that physical exercise helps to enhance brain health and improves mood and general fitness. A balanced diet, enough sleep and limited alcohol intake are other important ways to promote good brain health. Other illnesses that affect the brain, such as diabetes, high blood pressure and high cholesterol, should also be treated if present.
Recommended Reading: Does Medicare Cover Respite Care For Alzheimer’s
Treatment And Life Expectancy
Unfortunately, it is impossible to cure this type of dementia. The treatment of frontal lobe dementia is based on relieving the symptoms. The treatment includes taking medications, such as antidepressants, antipsychotic medications, etc. There is also a speech therapy that will help individuals who have difficulties with speaking.
Not only medications are enough for proper treatment of frontal lobe dementia, but it is also important to change a lifestyle. It is very important for people with this type of dementia to live in a comfortable place.
The environment should be familiar and peaceful, without noise and crowds. Also, people who have problems with speaking will need an environment where they will communicate without difficulties.
In frontal lobe dementia is in its early stage, it can be treated well. But, when disease has already progressed, people will need all-day care. It is proved that this condition will shorten the life of a patient. Studies have shown that most people with frontal lobe dementia live only 6 to 8 years after the disease was discovered.
If someone in your family or your close relative or friend suffers from frontal lobe dementia, you should consult the doctor and talk with him about all symptoms that you notice. But, if you are the one who have this condition, it is necessary to find support in a group. Also, you should learn to cope with all the effects of this condition.