Where To Get Help
- Your local community health centre
- National Dementia Helpline Alzheimers Australia Tel. 1800 100 500
- Aged Care Assessment Services Tel. 1300 135 090
- My aged care 1800 200 422
- Cognitive Dementia and Memory Service clinics Tel. 1300 135 090
- Carers Victoria Tel. 1800 242 636
- Commonwealth Respite and Carelink Centres Tel. 1800 052 222
- Dementia Behaviour Management Advisory Service Tel. 1800 699 799 for 24-hour telephone advice for carers and care workers
When Words Fail Us
Many forms of dementia are progressive, getting worse as time goes by. If you have a loved one who has dementia, you may have experienced the communication and language challenges that can accompany the condition and progressively deteriorate over time.
For example, in the early stages of disease, people may have trouble coming up with the right name for a person or word for an object. As they enter the later stages of their condition, they may speak less and less.
> > Related:When Memory Issues Are Cause for Concern
How Dementia Affects Communication
To better understand the progressive breakdown in communication, we must first consider what occurs intellectually in normal language expression and comprehension. In research done by Bayles it was found that working memory is critical in normal communicative functioning because it is the engine of cognition, enabling us to form intentions, hold incoming stimuli in consciousness, reverse received input, activate and access stored knowledge, interpret stimuli, monitor expression and plan action. While storage of verbal material has been shown to activate Brocas area and left supplementary and premotor areas, spatial information storage recruits right hemisphere premotor cortex and storage of object information activates the prefrontal cortex.
As a result of deficits in working memory, individuals with dementia will often exhibit attentional impairments and disproportionate problem solving and visuospatial difficulties, as well as difficulty with open-ended questions which require searching memory for an answer.
As a result of the pathophysiological mechanisms of dementia, impaired communication is a common feature, therefore physiotherapists must take extra care with this population in order to facilitate a positive therapeutic interaction.
Also Check: Does Terry Bradshaw Have Alzheimer
Dont Say No Dont Or Cant
One of the biggest mistakes in dealing with patients and/or loved ones with memory loss is being negative and telling them that they cant do something. Words like no,” don’t, or can’t create resistance. This comes up regularly with family members when the patient and/or loved one might be still driving, and the caregiver and/or family member has made the decision to stop them from driving. One should never say, You can’t drive anymore. They can still technically drive , and they can get very combative when told no. A way to counter this is to say, I know you still can drive, that’s not even a question, but you know what happened the other day? I was out on the highway and this car cut me off, and I had to make a split-second decision it was really scary Its likely they will say, You know what? I’m having a little trouble with those decisions too. The issue isn’t the mechanical driving, it has more to do with comprehension, and many times this answer works much better than, You can’t drive anymore, which can be construed as confrontational.
You may find a patient and/or loved one up too early or confused about time. Instead of using messages such as, Youre up too early, you need to go to bed, try leading with statements such as, You know, I’m getting sleepy. Id like a little snack before I go to bed, and then gesture for the patient and/or loved one to sit with you.
Loneliness In People With Dementia Is Linked To Social Isolation And Depression

Ann Pascoe – Carer
After reading this Alert, I asked Andrew the question: Are you lonely? He responded saying No, I have lots of things to do: I have my radio to listen to I can watch cricket on the telly and Ive got you to talk to. This is of course true but the onus gets put on the carer then to provide those activities, their time to talk and to do all the things that the person with dementia wants to do. I believe that loneliness can therefore be dementia-specific, which is contrary to what the Alert highlights. If Andrew didnt have dementia, I wouldnt have to plan out his day and spend that extra time as a carer rather than a wife. So I think loneliness in people with dementia is indeed linked to social isolation and depression if they are on their own or if the carer or someone – isnt there to help them to do things.
Kathryn Walker – Clinical Research Nurse
You May Like: Andrea Mitchell Speech Problems
Use Your Name And Others Names
Identifying yourself and others by name rather than by relationship is helpful, Gurung says. People with dementia may be more present in an earlier time in their life. This could be before you were their child or partner.
Rather than trying to reorient to today, it can be better to say, Hi, its me, Brenda, instead of, Hi Mom. Its Brenda, your daughter. Even with family members, you may find it more useful to call them by their preferred name rather than their title.
How To Maintain An Interactive Lifestyle
Research has shown that people living with dementia often spend their days being passive, not interacting with their surrounding environment or engaging their mind to the degree that they once did. This can impact anxiety and agitation.
To overcome this challenge, a new game called Tovertafel has been introduced in a number of UK care homes, which involves light animations created by a projector and infrared sensors. The game provides cognitive stimulation, and promotes physical movement and conversation.
You May Like: Senility Vs Dementia
How Does Dementia Affect Communication
The effects of dementia on the brain can worsen a persons:
- Communication and cognition
- Visual perception
- Problem-solving skills
Signs of dementia begin when healthy neurons or nerve cells in the brain stop working with other brain cells and die, according to the National Institute of Neurological Disorders and Stroke. While losing neurons is more common with age, people with dementia experience a severe loss of neurons, which can contribute to personality changes, a decrease in communication skills, and losing emotional control.
Training Programme To Improve Communication Between Staff And Patients With Dementia In Hospital Shows Promise
Emma Williams – Behaviour Analyst
Communication between people with dementia and their carers is a recognised problem, which can cause distress and misunderstanding if handled inappropriately. This research and training programme has potential to be implemented in other areas, although further research is warranted. High staff turnover rates in places of care may be problematic to ensure people finish the course and implement the intervention successfully. The use of simple language has been documented to be successful in areas such as the provision of personal care, or engagement in activities. It is vital that we use evidence-based interventions to provide the best quality care to people with dementia.
Ann Pascoe – Carer
When Andrew was diagnosed with dementia I felt helpless. I realised that I knew nothing about the illness which is why I went back to university to do an MSc specifically in dementia. I have had to learn how to diffuse situations as opposed to arguing and have learned to walk away at the right moments. Im really passionate about training and believe it has given me the wherewithal to deal with caring responsibilities.
Kathryn Walker – Clinical Research Nurse
Isobel Chick – Speech and Language Therapist
Don’t Miss: Does Meredith Grey Have Alzheimer’s
How To Talk To Someone With Dementia: 10 Expert Alzheimers Communication Strategies
It can be painful to witness the deterioration of a loved one with or any other type of dementia. Fortunately, there are many kinds of Alzheimers communication strategiesthat can help you maintain and build your bond with a loved one.
Alzheimers and other dementias are difficult disease journeys, but there is so much opportunity for connection and success together, says Brenda Gurung, a certified dementia practitioner for the Alzheimers Association and a senior national account manager at A Place for Mom. When you understand even a bit of whats happening in the brain and when you embrace some simple techniques youll have more delightful visits with your loved one, deeper connections, and a smoother journey.
Learn more about how dementia affects communication skills, how to talk to someone with dementia, and discover 10 effective Alzheimers communication strategiesto help.
Caring For A Person With Dementia
While the language difficulties that often accompany dementia can make it challenging to communicate, they also underscore the importance of making a plan for the future if you or a loved one receives a dementia diagnosis. Everything from financial and legal issues to safety to long-term daily living concerns must be taken into consideration.
Indeed, there will likely come a time when a person with dementia will no longer be able to live on their own, so one of two scenarios typically will come into play: The person with dementia will either require an around-the-clock in-home caregivereither a loved one or a paid caregiveror they will need to be moved to a long-term care facility that includes specialized memory care services.
For some people, providing caregiver services to a loved one is tremendously fulfilling, perhaps allowing them to feel as though they are repaying an elder who cared for them when they were a child. But for others, caring for a family member who has dementia can be extremely taxing, leading to physical and emotional exhaustion.
> > Related:Caregiver Assistance- Addressing Caregiver Stress
Read Also: What Color Ribbon Is Alzheimer’s
Play To Their Strengths
Sometimes memory loss is so devastating that we all forget that there is a person still in there somewhere. Family members can be distraught by what’s missing and forget that there’s still a lot there within the person, and that they have strengths.
They still have long-term memory, so its up to the caregiver and/or family member to find them. It’s interesting that, medically, doctors do tests on other conditions but when it comes to memory loss, it’s often looked at like a switch: Either they got it, or they don’t. Just like everything else, there’s a progression of memory loss, and its up to the caregiver and/or family member to find out where the patient and/or loved one is, and bolster that.
Strength #1: Long-term memory & stories
Everyone has a short-term memory drawer and long-term memory drawer, and we put information in each. People with dementia and/or Alzheimers have a short-term memory drawer that has no bottom. He/she puts things in, and then they get lost. The long-term memory drawer, however, has a solid bottom. Lots of stories that are retrievable await . Encourage your patients and/or loved ones to tell you stories. You can even use photos to encourage stories. Photos are wonderful long-term memory reminders.
Strength #2: Humor & music
Strength #3: Spirituality
Tips For Using Communication To Overcome Barriers To Therapeutic Interaction
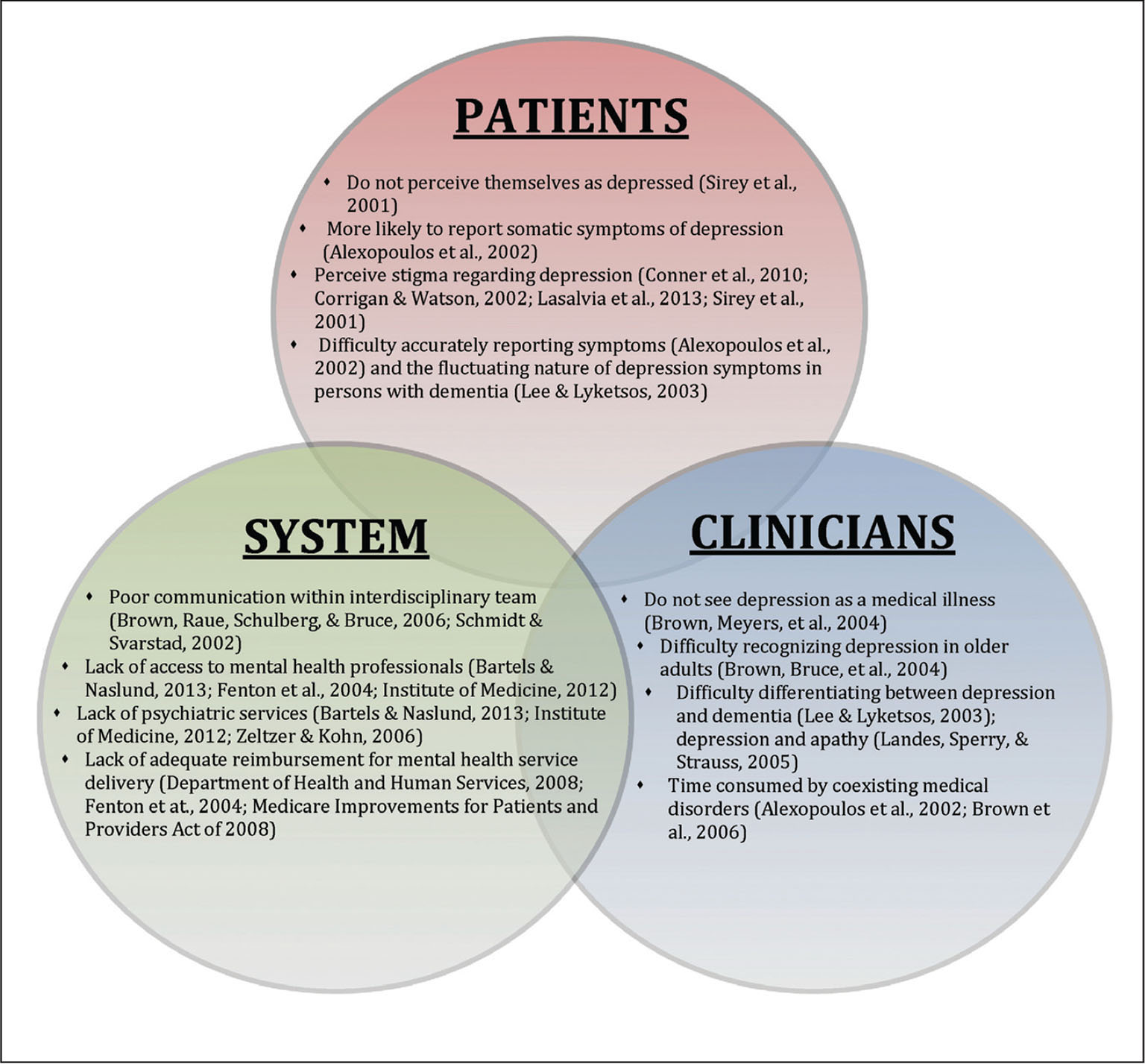
Dementia can pose as a barrier to communication, which many may find upsetting or frustrating. These barriers can impact a wide range of issues, including the therapeutic interaction between physiotherapist and patient. There are methods and strategies which help facilitate interaction with people with dementia and those who support them, to communicate in a way that is most effective . These methods may require the physiotherapist to adjust skills, behaviours and the delivery of information such as those discussed regarding the non-dementia patient population. These alterations should meet the needs of the person living with dementia and facilitate and strengthen therapeutic interaction
The following are some tips from the Alzheimers Society for using communication to enhance the therapeutic interaction with people living with dementia:
BEFORE YOU SPEAK:
HOW TO SPEAK:
WHAT TO SAY:
LISTEN:
Listening is one of the most important elements of communication, and is more than the physical process of hearing. Active listening is the highest form of listening and therefore is a special communication skill. It requires listening not only for what is said, but also for the intent and feeling of the speaker. It needs to occur in a non-rushed manner, using appropriate body language, showing interest in the speakers words . It is a vital tool for a physiotherapist in communicating with a person with dementia , as is discussed below:
You May Like: Smelling Farts Prevents Cancer
How To Manage Personal Finances
The onset of dementia, and the memory loss that comes with it, can cause difficulties when using the bank and looking after one’s money. For example, it can become increasingly hard to remember a PIN number and keep on top of the amount of money being spent and received.
There are promising steps in making day-to-day tasks a more easily-navigable aspect of life.
As a result, banks such as HSBC are becoming more accessible to those living with dementia, with voice technology recognition being introduced, so that individuals do not have to memorise a PIN. These are promising steps in making day-to-day tasks a more easily-navigable aspect of life. Ask your bank for details about the services they provide.
How People With Disabilities Due To Dementia Are Marginalised
We continue to share written or video stories, poems, and other stories of interst from our members, as part of o ur World Alzheimers Month Dementia wareness Month activities. Today we are sharing a presentation made by DAI Board member Phyllis Fehr.
On June 8, Phyllis provided a statement for the United Nations Online Regional Consultations with people with disabilities and their representative organizations in the Caribbean and North America
From isolation, invisibility and segregation into inclusion of people with disabilities in the community. Identifying and overcoming barriers to the successful process of deinstitutionalization
How people with disabilities isolated, marginalized, excluded, segregated or institutionalized in the Caribbean and in North America regions? How can these practices end?
As a woman living with Young Onset Dementia, I sat back with dread, fear and utter disbelief as I watched what was happening in the long-term care sector for people living with dementia.
These people were being further isolated and segregated. They were subject to disgraceful living conditions, in some instances. They were placed in their rooms with no interaction from others. Some received no assistance with activities of daily living or feeding. They were unable to have visitors or even accept video calls in the early stages of the COVID pandemic.
Thank you for your time.
Phyllis Fehr, 2021
You May Like: Scientists Say Smelling Farts Prevents Cancer
Domain : Innovation Characteristics
This was a key domain, with three constructs emerging as important to implementation: relative advantage, trialability, and complexity.
Relative advantage
Team members reported that the team-based standardized evidence-based assessment flow sheets helped them provide better care by providing a template or guide to assessment steps. They reported increased confidence and feeling empowered to provide better care without having to refer all patients to specialists.
We knew that the dementia part of our patients was important and assessment of thatwe just didnt quite know how to put all together and bring everybody together. So thats been huge.
The providers did the best they could in their appointments they didnt feel like it was very standardized so they wanted a process for when a patient complains of cognitive difficulties, what exactly do we do, what are the steps that we take.
The team approach also allowed team members to contribute their individual disciplinary skills to the assessment. They felt valued by other team members and in turn appreciated other team members roles. The format of the one-day clinic allowed team members to discuss their findings and learn from each other, thus increasing their confidence in the diagnosis and treatment plan. The synergies of working together resulted in better care, which was rewarding.
As a provider I feel much more confident dealing with these people AND because I know theres a team that backs me up too.
Complexity
Dont Counter Aggressive Behavior
People with dementia and/or Alzheimer’s may become aggressive in response to the environment. Bath time is often when the aggressive behavior is displayed. The caregivers and/or family member’s approach may also play a part. Rushing, speaking harshly, or forcing a person may result in an aggressive response. When someone with memory loss displays aggressive behavior, it is a form of communication. It may be the only way a person has left to say, Pay attention to me! I don’t want to take a bath! When someone is communicating vigorously, it is the caregivers and/or family member’s job to respect that communication. Hitting, kicking, or biting are ways of saying, stop. The appropriate response is to stop. That doesnt mean not to try again in five minutes or a half an hour.
Read Also: Does Prevagen Work For Dementia
Speak Naturally And Use Gestures
Its important to speak clearly, simply, and in complete sentences, while using a calm and friendly voice to talk to someone with dementia.
Besides using your voice, try to communicate using your body, incorporating subtle movements. Demonstrate your meaning with visual cues or gestures. For example, if you say, Lets go for a walk, use an arm motion with your invitation.
What Not To Do When Communicating With A Person With Dementia
- argue with the person it will only make the situation worse
- order the person around
- tell the person what they cant do instead, state what they can do
- be condescending a condescending tone of voice may be picked up, even if the words are not understood
- ask a lot of direct questions that rely on a good memory
- talk about people in front of them as if they are not there.
Read Also: Meredith Grey Alzheimer’s