Care Options For Seniors With Alzheimers Disease
As a family caregiver for someone who has Alzheimers, you should know that even the most dedicated families often need to enlist outside memory care help, especially during the latter stages of the disease. Two of the best options for memory care services are in-home care and residential care in a specialized memory care community.;
In-Home Care
In-home memory care, often called home care or home health care, can be used to support your loved one while also giving you and your family a much-needed break from your caregiving duties.
In-home care services are provided on a one-on-one basis. A home care provider who specializes in working with individuals who have Alzheimers disease can be hired on an hourly or live-in basis. These professionals can help with activities of daily living, such as bathing, dressing and grooming, that your loved one might not want a family member helping them with.;
Home care providers can also assist with light housekeeping and laundry, meal prep and in some cases, pet care. This type of care may be ideal if youre looking for someone who can supervise your loved one while you attend to your own health and well-being or on a respite basis.;
Memory Care Communities
Stages Of Alzheimer Disease
The stages of Alzheimer disease usually follow a progressive pattern. But each person moves through the disease stages in his or her own way. Knowing these stages helps healthcare providers and family members make decisions about how to care for someone who has Alzheimer;disease.
Preclinical stage.;Changes in the brain;begin years before a person shows any signs of the disease. This time period is called preclinical Alzheimer disease and it;can last for years. ;
Mild, early stage.;Symptoms at this stage include mild forgetfulness. This may seem like the mild forgetfulness that often comes with aging. But it may also include problems with concentration.;
A person may still live independently at this stage, but may;have problems:
-
Remembering a name
-
Staying organized
-
Managing money
The person may be aware of memory lapses and their friends, family or neighbors may also notice these difficulties.;
Moderate, middle stage.;This is typically the longest stage, usually lasting many years. ;At this stage, symptoms include:
-
Increasing trouble remembering events
-
Problems learning new things
-
Trouble with planning complicated events, like a dinner
-
Trouble remembering their own name, but not details about their own life, such as address and phone number
-
Problems with reading, writing, and working with numbers
As the disease progresses, the person may:
Physical changes may occur as well. Some people have sleep problems. ;Wandering away from home is often a concern.;
Assessment Scales For Agitation
Several assessment scales are currently available to investigate the presence and severity of agitation . The Agitated Behavior Scale assesses an agitated state’s occurrence and duration after brain injury. The scale’s primary purpose is to monitor behavioral changes after admission to a hospital ward . The Behavioral Activity Rating Scale is often used in clinical trials. According to this scale, patients are classified into seven different levels of agitation . The Overt Agitation Severity Scale offers a helpful approach to detect and rate agitation when spanning from anxiety to aggression . The Modified Overt Aggression Scale , a scale divided into four sections, examines the frequency and severity of aggressive episodes . Another easy-to-use tool is the Pittsburgh Agitation Scale , which measures the dementia-related agitation severity . The Agitated Behavior Mapping Instrument is a diagnostic scale that evaluates 14 different physical and verbal agitated behavior features. Finally, the Cohen-Mansfield Agitation Inventory is a frequency rating scale completed by caregivers .
A screening tool for delirium is the 4AT, in which a score higher than four indicates a high risk for delirium . However, the Confusion Assessment Method for the ICU is a more sensitive and specific assessment to diagnose a delirium state .
Read Also: Is Reading Good For Dementia
Prevention Strategies For Home
Person-centered care is an operating system in healthcare, which considers the health practitioner and the patients as partners in achieving tailored care that meets patients’ needs in a unique way . In the PCC framework, the social and historical background, the personality, and the lifestyle of the patients are considered to promote a positive social environment, good compliance, and best outcomes for patients with dementia . The PCC approach is considered a successful option to prevent agitation in home-living and care home patients with dementia and reduce antipsychotic use . Nonetheless, not every PCC-based strategy is effective. For instance, the Dementia Care Mapping , which is based on patients’ systematic observations, has generated conflicting results. In contrast, the Managing Agitation and Raising Quality of Life intervention has failed to improve agitation prevention in care home settings.
Previous studies have indicated a role for boredom in the onset of physical agitation . Thus, activity-based strategies have been developed to prevent this condition. The application of combined stimuli has shown to be more effective than a single activity . However, the most effective activity was live socialization .
Data that emerged from other non-pharmacological approaches, such as acupuncture and electroconvulsive therapy, are mostly conflicting. Some ongoing trials could possibly clarify a potential role for these therapies .
What Is Alzheimers Disease
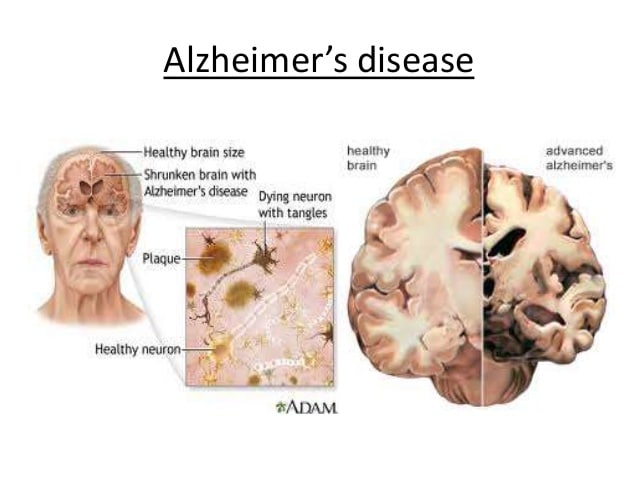
Alzheimers disease is the most common type of irreversible dementia . Nearly 7 out of 10 people with dementia have the Alzheimers type.
While Alzheimers disease affects up to 1 in 10 Australians over 65 years of age, and up to 3 in 10 Australians over 85, it is not a normal part of ageing.
The brain contains millions of brain cells that organise how the brain stores memories, learns habits and shapes our personality. Signals pass along the connections between brain cells in the form of chemicals called neurotransmitters. Alzheimers disease affects these cells and chemicals, disturbing memory, impairing thinking and causing behaviour changes over time. People with Alzheimers disease eventually need long-term care and support.
There are 2 main types of Alzheimers disease:
- Sporadic Alzheimers is the most common form and usually occurs after age 65. Its cause is not fully understood.
- Familial Alzheimers is caused by a very rare genetic condition and results in dementia, usually in people in their 40s and 50s. This is known as younger onset dementia.
You May Like: Can Low Fat Diet Cause Dementia
Mental Activity To Support Cognition
Many patients with normal cognition or those with mild impairment are concerned that they may develop AD. Many experts believe that mentally challenging activities, such as doing crossword puzzles and brainteasers, may reduce the risk in such patients. Whether such activities might slow the rate of disease progression in patients who already have AD is not known. Clinical trials are under way to determine the effect these cognitive activities have on AD progression.
Mental activities should be kept within a reasonable level of difficulty. Activities should preferably be interactive, and they should be designed to allow the patient to recognize and correct mistakes. Most important, these activities should be administered in a manner that does not cause excessive frustration and that ideally motivates the patient to engage in them frequently. Unfortunately, little standardization or rigorous testing has been done to validate this treatment modality.
Some investigators have attempted various forms of cognitive retraining, also known as cognitive rehabilitation. The results of this approach remain controversial, and a broad experimental study needs to be performed to determine whether it is useful in AD.
Dr Bahram Jam Dscpt Mphty Bscpt Credmdt
The following insightful article was written by Dr. Bahram Jam, DScPT, MPhty, BScPT, CredMDT. We are thankful to him for his permission to reproduce the article here. You can read more about Dr. Bahram Jam and the Advanced Physical Therapy Education Institute at
I originally assessed Mrs. A, a 65-year-old lady in 1998 where she reported of significant global neck pain. Her x-rays showed typical degenerative changes that were blamed for her ongoing symptoms. After several weeks of physical therapy, she regained some neck mobility, but her symptoms mostly persisted. I felt that my interventions had failed.
In 2002 I saw Mrs. A again reporting of bilateral knee symptoms. She reported little change in her neck pain in the past 4 years and in addition her knees were now problematic. Although she had some radiological evidence of degeneration in her knees, she was not yet a surgical candidate. I provided her with 6 weeks of physiotherapy treatments but she made minimal symptomatic improvements, and in the end, I recommended her to use a cane. She also received cortisone injections that were of little value. I felt that I had once again failed in my attempts to help this pleasant lady.;
General analgesic use is very;low among nursing home;residents with dementia1.
A German study showed that nursing home;residents with AD exhibited significantly less;additional pain-associated diagnoses when;compared to those with cancer orParkinsons disease5.
References:
Don’t Miss: How Is Alzheimer’s Disease Diagnosed In Humans
Microglial Activation And Neuroinflammation Increase In Ad
Recently, inflammation-associated PET studies demonstrated microglial activation in the brains of AD patients. In addition, microglial activation was found occurring before cognitive decline in AD patients, suggesting that it may be an early precipitant of AD progression . By using PET-MRI in AD patients, two peaks of microglial activation were detected during the trajectory of AD pathogenesis, which may represent an early protective peak and a later pro-inflammatory peak .
Microglial activation and neuroinflammation are found in the brains of AD animal models. For example, microglia show increased proliferation in well-characterized mouse models of AD, including APP/PS1, 5XFAD, and APP23 mice , and increased expression of pro-inflammatory markers such as CD36, CD14, CD11c, MHC-II, and iNOS .
Special Care Dementia Unit
The social environment is also significant in mollifying the behavioral manifestations of dementia. If demented individuals are grouped together on a special care dementia unit, many symptoms may be minimized. Grouping demented patients together further eliminates the problem of demented patients disrupting the routine of cognitively intact individuals by wandering into their rooms, rummaging through their belongings, or approaching them repeatedly with questions and unwanted physical contact. Well-designed studies are needed to demonstrate the benefits of such units.
Don’t Miss: What Type Of Genetic Disorder Is Alzheimer’s
Clearing Up The Confusion
The seemingly random ways in which these terms are applied can often create confusion in a patient’s expectations.
For example, can cancer truly be considered chronic when only a few types are able to be managed chronically? Should a traumatic injury like a broken leg be considered acute even if it fits within the broader definition of the term?
In the end, defining an illness or injury as acute or chronic may not only not be necessary, but it may confuse more than enlighten.
Some health experts advocate for a simpler approach to help clear up confusion and inconsistencies. Rather than adhering to a specific timeframe or list of conditions, they endorse definitions that express the concepts behind the terms more generally.
Merriam-Webster’s dictionary, for example, defines them as follows:
- Acute: “Having a sudden onset, sharp rise, and short course”
- Chronic: “Continuing or occurring again and again for a long time”
Acute Vs Chronic Inflammation
Injuries and infections produce acute inflammation, the body’s rapid response mechanism that aims to rid itself of the dangerous invader and return it to a state of balance. A release of warning chemicals sounds the alarm, which draws an army of white blood cells to the site of injury. Some of these cells neutralize the invaders, while others clean up the damage that results from the battle. Acute inflammation typically resolves quickly, within a period of hours to days.
Chronic inflammation can begin via the same process, with the body trying to rid itself of what the immune system interprets as foreign adversaries. But this can become a persistent state, even if the perceived threat isn’t truly harmful to one’s health. In autoimmune disorders like rheumatoid arthritis, lupus, type 1 diabetes, ulcerative colitis, and multiple sclerosis, the body mistakenly reacts to its own tissues as if they were foreign, and produces damaging inflammation against them.
This chronic kind of low-grade inflammation may continually simmer under the surface. An unhealthy lifestyle that includes smoking, a poor diet, alcohol consumption, sedentary behavior, stress, and weight gain can cause this type of persistent inflammation.
Read Also: How Early Can Dementia Start
Inflammation Acute Vs Chronic
The immune system operating via the lymphatic and circulatory systems acts as the defender of the body. It keeps out what needs to be kept out, fights when it needs to fight and protects by cleaning up and disposing of dead or damaged cells.
A key component of a healthy immune system is inflammation. Inflammation is triggered immediately when it detects damage in the cells or tissues as a result of injury or the presence of pathogens or other toxins. Acute inflammation is the initial phase of the inflammation process. It is the first line of defense against disease. It is the time period when function is impaired. The area may be swollen, hot, red and painful. It is the 911 call to the immune system that danger is present and the system must be activated to neutralize the threat. Acute inflammation is short lived and is a positive, protective, healing and renewing mechanism.
Chronic inflammation on the other hand is not beneficial. Chronic inflammation is not a friend to the body nor is it short lived. It is a sign that things are getting out of control and instead of attacking invaders the body is attacking itself. Chronic inflammation drains the immune system as it continues to prompt the immune system to send white blood cells to attack healthy tissue and organs setting up a chronic inflammatory process.
Chronic inflammation may be caused by:
Symptoms / signs of chronic inflammation include:
Caring For The Caregiver
Many caregivers are reluctant to ask for help. It is important that health care providers ask the caregivers if they need assistance and validate their feelings. Clinicians must be prepared to help the caregivers deal with anger, denial, anxiety, guilt, grief, and clinical depression as they adjust to the progression of the disease. The grief and adjustment process for a caregiver is complex and cyclical, potentially reactivated by the additional impairments at each new stage of the illness. Family and caregiver interventions will help not only the caregivers but also the patients with AD by preventing premature institutionalization . Educational program, training program, support, and respite services directed toward caregivers of dementia patients may improve their coping skills and reduce stress .
You May Like: Is Lewy Body Dementia A Genetic Disorder
Reduce Inflammation With Sleep And Relaxation
Loss of sleep hinders your immune system and can trigger inflammatory responses. Our bodies need between seven and nine hours of sleep every night to properly rest. There are many things you can do to improve your sleep, including turning off electronic devices in the evening, getting enough exercise, and creating a healthy, de-stressing routine before bed. Enough quality sleep will decrease inflammation.
Research has found that mind-body practices, such as meditation or yoga, can also help the brain manage stress which is known to trigger and aggravate inflammation. Even 5-10 minutes a day can be beneficial. Chronic stress is not good for your body. By relaxing more and engaging in mindfulness, your stress hormones will decrease, helping decrease inflammation. Other relaxation techniques may be as simple as taking deep breathes for 1 minute every hour and taking proper breaks every few hours.
Treatment Of Ad With Cheis In The Nursing Home Setting
Very little controlled data is available for the potential benefits of ChEIs in patients with AD in the LTCF setting. Donepezil was found to be beneficial in the domain of cognition and overall dementia severity compared to placebo in a 6-month treatment period of AD patients in the nursing home setting . Unfortunately, no significant differences were obtained in the noncognitive domains of behavioral disturbances and ADL in this study. An open-label, 52-week study of rivastigmine in nursing home patients with AD demonstrated improvement in many of the behavioral and psychiatric symptoms, such as irritability, anxiety, delusions, hallucinations, disinhibition, aberrant motor activity, nighttime behavior, and appetite . In addition, about 40% of patients who were on neuroleptic medications for these symptoms were able to reduce or discontinue these medications over the course of the study. Patients with AD in the nursing home are generally older, exhibit greater severity of dementia, and have more comorbid illness than do AD patients in the community.
Recommended Reading: How To Deal With Someone With Dementia
How Do Doctors Diagnose Alzheimer’s Disease
No specific blood test or imaging test exists for the diagnosis of Alzheimer’s disease. Alzheimer’s disease is diagnosed when:
What other conditions should be screened for besides Alzheimer’s disease?
Ten other causes of dementia are:
The importance of comprehensive clinical evaluation
Emotion And Behavior Treatments
The emotional and behavioral changes linked with Alzheimers disease can be challenging to manage. People may increasingly experience irritability, anxiety, depression, restlessness, sleep problems, and other difficulties.
Treating the underlying causes of these changes can be helpful. Some may be side effects of medications, discomfort from other medical conditions, or problems with hearing or vision.
Identifying what triggered these behaviors and avoiding or changing these things can help people deal with the changes. Triggers may include changing environments, new caregivers, or being asked to bathe or change clothes.
It is often possible to change the environment to resolve obstacles and boost the persons comfort, security, and peace of mind.
The Alzheimers Association offer a list of helpful coping tips for caregivers.
In some cases, a doctor may recommend medications for these symptoms, such as:
- antidepressants, for low mood
Don’t Miss: How Long Can Someone Live With Dementia