As A Care Worker How Can You Help
There are many conditions and circumstances where you may see signs and symptoms that may be confused with dementia. As a care worker, it is not your responsibility to try to diagnose the condition. However, as you may be the one person who sees the individual on a regular basis, you are well placed to notice any changes. Encouraging an older person to visit their GP on a regular basis can help them to maintain their general health and wellbeing.
Give New Interventions A Try
Even though research is still emerging, studies suggest that psychosocial interventions are currently the best and lowest-risk treatments for depression and anxiety in older adults with cognitive impairment. A broad range of supportive approaches for nonmedication treatments exists, and should be used if available as a first-line treatment.
Targeting Anxiety May Slow Alzheimers
Previous studies have suggested that depression and anxiety might be indicators of Alzheimers, since symptoms of these mental health conditions often occur in the early stages of the disease.
For their study, Dr. Donovan and colleagues sought to determine whether or not beta-amyloid might play a role in this association.
The research included 270 adults between age 62 and 90, with normal cognitive functioning, all of whom underwent positron emission tomography at study baseline and annually during 5 years of follow-up, in order to determine levels of beta-amyloid in their brains.
Symptoms of anxiety and depression among the adults were assessed using the 30-item Geriatric Depression Scale.
It was found that adults who showed an increase in anxiety symptoms over 5 years of follow-up also had higher levels of beta-amyloid in their brains. The researchers say that this indicates that worsening anxiety might be an early sign of Alzheimers disease.
If further research substantiates anxiety as an early indicator, it would be important for not only identifying people early on with the disease, but also, treating it and potentially slowing or preventing the disease process early on.
Dr. Nancy Donovan
The scientists point out that follow-up studies are required to determine whether older adults who experience an increase in anxiety symptoms actually go on to develop Alzheimers.
Read Also: Senility Vs Dementia
What Constitutes The Best Source Of Information To Assess Anxiety In Dementia
In the general population, the most common source of information to determine the presence of an anxiety disorder is the patient him- or herself. In dementia, this option may not always be optimal, as some patients have difficulty communicating and remembering their symptoms. To avoid these difficulties, some authors have chosen to rely exclusively on caregiver report. This strategy may work well for situations in which the core symptom is behavioral . In the case of GAD, however, the core symptoms of worrying and difficulty controlling the worry are private in nature, and caregivers might not be aware of them, particularly if the relationship between patient and caregiver is strained. Moreover, as we have seen, some of the outward manifestations of anxiety are highly confounded with symptoms of dementia. Thus, exclusive reliance on caregiver report may be the only choice when patients are too impaired to communicate effectively. In other cases, however, it would deprive the examiner of a valuable source of information.
Earlier Screening May Help
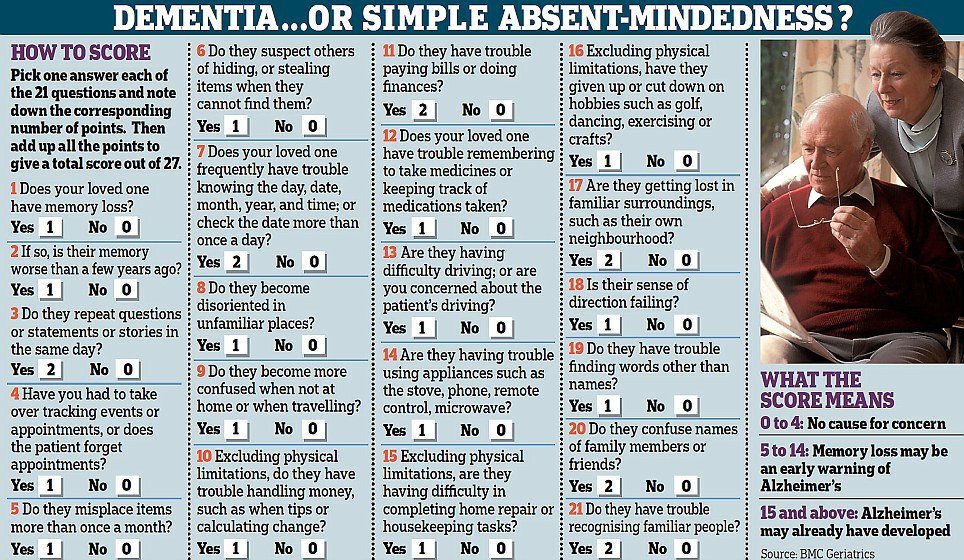

Behavioral and psychological changes could also be a sign of other underlying conditions, so be sure to speak with your doctor, Roe said.
Its also important for doctors to look beyond the usual suspects, such as anemia in someone complaining of low energy. Maybe they should also consider giving the person some sort of memory or cognitive screening. This could help pinpoint some other areas that might need to be explored, said Roe.
This study only included people who had no symptoms of depression or memory loss at the beginning of the analysis. Since depression is relatively common in seniors, Roe said a more realistic sample would have included volunteers with some depression symptoms.
We were just really interested in learning when these symptoms occurred relative to each other, Roe said.
She stressed that some of the people who didnt develop dementia during the study might still have gone on to develop it later.
Recommended Reading: Color For Alzheimer’s Ribbon
Anxiety Symptoms May Be Early Indicator Of Alzheimer’s Disease
New research suggests that anxiety symptoms in late-middle-aged adults may be an indicator of the earliest stage of Alzheimer’s disease.
The study, led by Monash University Turner Institute for Brain and Mental Health researchers Stephanie Perin and Associate Professor Yen Ying Lim, examined the relationship between symptoms of depression and anxiety, and memory and thinking, in 2657 middle-aged adults.
Higher anxiety was found to be related to poorer attention and memory.
“The observation that anxiety symptoms are related to poorer memory, particularly in late-middle-aged adults, suggests that anxiety may also be an indicator of the earliest stage of Alzheimer’s disease, or that it may be related to the development of dementia in some way,” Associate Professor Lim said.
Associate Professor Lim said individuals with high depressive and anxiety symptoms also reported more concerns about their own memory and thinking.
“This suggests that subjective concerns about one’s own memory and thinking abilities may be related to psychological or mood symptoms, rather than true dysfunction in memory or thinking, at least in middle-aged adults,” Associate Professor Lim said.
Associate Professor Lim said the findings suggest that anxiety symptoms in midlife may increase a person’s risk of developing dementia later in life.
“Screening for these symptoms may be a means of identifying people experiencing or at risk of cognitive decline,” Associate Professor Lim said.
Depression And Anxiety In Dementia
and anxiety symptoms are extremely common in dementia and mild cognitive impairment . As a result of these symptoms, many people with dementia experience a decrease in their quality of life. Depression and anxiety may lead to disengagement from daily activities, which may further exacerbate memory difficulties. Social withdrawal and discontinuation of cognitively stimulating activities as a result of depression increase the likelihood of nursing home placement.
Recommended Reading: Alzheimer’s And Neurotransmitters
Dementia And Anxious Behavior: How To Deal With Anxiety And Agitation
Anxiety is very common in dementia, but treatments for anxiety can be hard to come by. Family and non-professional caregivers can help their loved ones deal with anxiety with some knowledge of the condition and how to relieve it.
First, here are some basics about anxiety in dementia.
- Anxiety disorders are about twice as common among people who have dementia as they are in people who do not have dementia.
- Any kind of dementia can provoke anxiety, but persistent symptoms of anxiety are most common in Parkinson’s disease and vascular dementia. Anxiety is less common in Alzheimer’s disease.
- There isn’t any one medication that is always effective in treating anxiety, although antidepressants sometimes help. It is essential for the doctor in charge of the case to choose the medication because of interactions and side effects.
- Likewise, there isn’t any single psychological intervention that always helps to relieve anxiety, but a mixture of methods is usually optimal.
Evaluation Of Assessment Measures
Based on our discussion of the optimal way to define anxiety in dementia, several recommendations can be made to evaluate existing instruments. First, because it is unclear at this point whether anxiety is part of a broader syndrome in this population, it should be assessed independently. Second, instruments should focus on symptoms of anxiety that are less likely to be affected by the presence of dementia. Concentration difficulties, in particular, are not likely to discriminate well between anxious and non-anxious individuals with dementia . Third, instruments should whenever possible be scored based on information from multiple sources, including at least the patient him- or herself and a caregiver. Finally, instruments should have strong psychometric properties, i.e., reliability, validity and sensitivity to change.
Our third criterion recommends the use of multiple sources of information. Only the RAID fulfills this criterion, while the NPI and BEHAVE-AD rely only on caregiver report. The Worry Scale, which relies solely on self-report, can be used only with individuals with mild dementia, which limits its usefulness. Such an approach also ignores difficulties related to lack of insight, which is common in dementia, even in the mild stage .
Read Also: Does Diet Coke Cause Dementia
Health Fears Are An Anxiety Symptom
One of the problems with living with anxiety is that it tends to cause itself, using its own symptoms. Feelings of dementia are a great example of this. Anxiety causes the mind to think differently and feel funny, and this causes people to worry they have a serious brain condition, which in turn causes them to be oversensitive to the way their mind works and suffer from the very problems they’re monitoring.
Men and women of all ages have convinced themselves of:
- Early Onset Alzheimer’s
- Brain Tumors
- Huntington’s Disease
These are all serious diseases, and if you truly think you have one of these, you should see a doctor. But you should also note that anxiety causes the very same issues. Not just dementia, but also the nerve impulses and other brain health issues that make people fear those diseases in the first place.
Why anxiety causes dementia like feelings is a bit less clear and less obvious. It is likely caused by many different factors, including those below:
These are all examples of issues that can cause feelings of dementia, despite no dementia present.
What Are The Causes Of Mci
MCI is not dementia , but it’s not normal thinking, either. It often stems from disease or treatments for disease, including
-
degenerative brain disease, such as Alzheimer’s disease
-
stroke or other vascular disease
-
traumatic brain injury
-
an underlying health problem, such as sleep deprivation, depression, or anxiety.
Recommended Reading: Bobby Knight Health Update
Going For An Assessment
The list of conditions and problems above isnt everything. Theres a whole range of things that can occasionally cause dementia-like symptoms for some people.
There isnt always a quick answer to the question, Is it dementia or something else? If someone has dementia-like symptoms, the most important thing to do is see their GP for a full assessment.
What Causes These Behaviours
There are many reasons why behaviours change. Every person with dementia is an individual who will react to circumstances in their own way. Sometimes the behaviour may be related to changes taking place in the brain. In other instances, there may be events or factors in the environment triggering the behaviour. In some instances a task may be too complex. Or the person may not be feeling well.
You May Like: Senility Vs Dementia Vs Alzheimer’s
Anxiety And Dementia Subtype
Six studies compared anxiety prevalence in distinct, well-defined types of dementia . In one study , rates of OCD, phobia, and GAD did not differ between AD and vascular dementia . Among four studies that examined rates of anxiety symptoms in AD and VaD, two found greater anxiety in VaD , and the other two did not find any significant difference . In both studies with null findings, anxiety was qualitatively greater in the AD group. Moreover, in one study , sample size was relatively small , and in the other study , rates of anxiety symptoms were unusually low . Thus, anxiety symptoms appear greater in VaD than in AD. Compared to AD, rates of anxiety symptoms may be greater in fronto-temporal dementia and similar in dementia associated with Parkinsonâs disease .
Characteristics Of The Study Population
Compared with the CH group, the AD and FTD groups were older at participation in the HUNT2 study and were more likely to have heart disease, diabetes, metabolic disease, obesity, anxiety, and depression. Compared with the AD group, the FTD group was younger at participation in the HUNT2 study and at time of diagnosis. The FTD cases were also more likely to have hypertension, metabolic disease, obesity, as well as anxiety and to smoke . All cases in the FTD group received their dementia diagnosis after the year 2000. In the AD group, 26 cases received their dementia diagnosis between 1995 and 1999 and the remainder after the year 2000.
Table 1.
Characteristics of the study population
Recommended Reading: Does Coke Cause Alzheimer’s
Anxiety Is A Risk Factor For Dementia
All of the studies included in the final analysis found statistically significant associations between clinically diagnosed anxiety and an increased risk of late-onset dementia at least 10 years from the time the diagnosis of anxiety was formed. Each study found the results to be true after adjusting for potential confounders. These results contribute to the increasing canon of research that has found that being diagnosed with common mental health conditions in middle age is a precursor for developing neurodegenerative disorders, such as dementia, later in life.
Past research has found only inconclusive evidence of anxietys effect on the development of dementia. Limitations of previous research have included shorter follow-up periods, around two to three years, which is why the researchers behind the current analysis focused only on studies with a follow-up period of 10 years or longer. The results of the previous research found stronger associations between anxiety and dementia, leading them to believe that anxiety may result from a prodromal state of dementia, where an increase in anxiety may be due to an individuals insight into their early subjective experience of cognitive decline.
Also read:
Strengths And Limitations Of The Study
The main strength of our study is its longitudinal, population-based, nested case-control design. Another strength is the use of a validated dementia diagnosis and data on anxiety and depression from the HADS . We were able to investigate risk factors measured in the HUNT2 years before the FTD and AD diagnoses were made. Furthermore, our study has a comparable number of FTD cases to other studies, where populations have varied from 61 to 129 cases . An exception was the study by Deutsch et al. on head trauma as a risk factor for FTD, which had 1,016 FTD cases. A further advantage of our study was that in the multivariable analyses we were able to adjust for a large number of potential confounding factors.
The HADS is self-rated and scoring could be biased by the persons feelings at the time they filled out the questionnaire. There is also a possibility that some FTD or AD cases developed cognitive impairment before participation in the HUNT2 study. Filling out a self-rated questionnaire may be problematic for individuals with cognitive impairment because insight and the ability to quantify emotional states may be impaired. Understanding and interpretation of the questions in the HADS may also be subject to individual variation. However, previous studies have shown the HADS to be satisfactory in terms of internal consistency, factor structure, and intercorrelation .
Recommended Reading: Did Reagan Have Alzheimers
Recommendations For Defining Anxiety In Dementia
Existing studies have examined anxiety in individuals with dementia both as a set of diagnostic entities and as continuous measures of symptomatology. Both approaches can be useful and even complementary, for instance in treatment studies where patient selection is often based on diagnostic criteria and estimates of treatment effects on symptom severity. Given the overlap between symptoms of anxiety and symptoms of dementia, it is unclear whether traditional definitions of anxiety are adequate in this population. Modified criteria for GAD have been suggested , although they probably require expert consensus for greater validity and wide adoption. Given the private nature of core symptoms of anxiety , defining anxiety based solely on behavioral observations or caregiver report may be insufficient.
Anxiety Could Be An Early Manifestation Of Alzheimer’s Says Study
Symptoms of increasing anxiety may be an early warning sign of Alzheimer’s disease years before cognitive impairment is evident, a new study suggests.
Researchers have long studied the risk factors that increase the chances of developing Alzheimer’s including neuropsychiatric conditions such as depression. Now, scientists say anxiety symptoms could be a dynamic marker of the disease’s early stages.
“Rather than just looking at depression as a total score, we looked at specific symptoms such as anxiety,” explains geriatric psychiatrist Nancy Donovan from Brigham and Women’s Hospital in Boston, Massachusetts.
“When compared to other symptoms of depression such as sadness or loss of interest, anxiety symptoms increased over time in those with higher amyloid beta levels in the brain.”
Amyloid beta is a protein that’s comprehensively been linked to Alzheimer’s disease, building up in the brain in clumps that form plaques and disrupting communication between neurons.
That disruption is thought to be a chief culprit behind the cognitive impairment of Alzheimer’s disease, but it could also be implicated in the condition’s pre-clinical phase, potentially as far back as 10 years before memory decline is diagnosed.
Donovan and fellow researchers examined data from the Harvard Ageing Brain Study, an observational, five-year study of 270 healthy men and women aged between 62 and 90 with no active psychiatric disorders.
You May Like: What Are Complications Of Alzheimer Disease That Cause Death
Depression Common With Age
The link between depression and dementia is even more significant considering that depression becomes more common with age. All of the following may put you at risk for depression as you get older:
-
the death of a spouse, friends, or family members
-
having to move out of your home and into an assisted living facility
-
side effects of medicines you’re taking for health conditions.
You’re also more likely to develop illnesses such as diabetes, heart disease, and cancer as you get older. These conditions can increase your risk for depression, and vice versa. Depression can make a chronic illness worse, says Dr. Cremens.
Anxiety Modifies Relationship Between A Deposition And Cognitive Impairment
Study data published in Alzheimers & Dementia suggest that anxiety may mediate the relationship between cortical amyloid beta deposition and risk for mild cognitive impairment . In a longitudinal study of older adults, anxiety appeared to exacerbate the progression of MCI in amyloid-positive patients.
Elevated A deposition has been associated with cognitive decline in older adults and can be an early sign of Alzheimer disease . Additional studies have also identified anxiety and depressive symptoms as independent risk factors for cognitive impairment. However, the intersecting associations between anxiety, depression, A deposition, and MCI are relatively unexplored. To inform this gap, investigators conducted a population-based study of community-dwelling adults aged 50 years.
Patients were followed up for a median of 5.5 years, during which they underwent regular neuropsychiatric screenings. Baseline cortical A was measured using Pittsburgh compound B positron emission tomography . Elevated deposition was defined by a standardized uptake ratio 1.48. Cox proportional hazards models were used to estimate the effect of anxiety and depression on the relationship between A deposition and MCI. Clinical anxiety was defined by a Beck Anxiety Inventory score 10 clinical depression was defined by a Beck Depression Inventory score 13.
Reference
Also Check: Bob Knight Alzheimer’s