Alzheimers Is A Brain Disease
People diagnosed with Alzheimers disease may display similar traits to those with mental illness. However, Alzheimers disease is more accurately defined as a brain disease, specifically, a progressive neurodegenerative condition. The American Psychiatric Association describes the brain disorder as a group of symptoms that lead to a decline in mental function severe enough to disrupt daily life.
The progression of the various stages of Alzheimers leads to memory loss, which affects ones ability to reason, learn, and make sound decisions. A person with Alzheimers can lose the ability to communicate effectively, and eventually, accomplishing simple daily activities becomes an overwhelming challenge.
Alzheimers disease is treatable, but not curable. Treating Alzheimers disease helps to slow its devastating progression and assists in providing quality of life through the multiple stages of the disease.
Dementia affects both mental and physical health, but it is not strictly defined as mental illness. Unlike mental illness, dementia is a disease that primarily affects seniors. Mental illness is nondiscriminatory and can be prevalent at any age. Yet while it differs from dementia, one in three seniors suffers from mental illness.
Episodic Memory And Imagination
When thinking is understood in a wide sense, it includes both and . In episodic memory, events one experienced in the past are relived. It is a form of mental time travel in which the past experience is re-experienced. But this does not constitute an exact copy of the original experience since the episodic memory involves additional aspects and information not present in the original experience. This includes both a feeling of familiarity and chronological information about the past event in relation to the present. Memory aims at representing how things actually were in the past, in contrast to imagination, which presents objects without aiming to show how things actually are or were. Because of this missing link to actuality, more freedom is involved in most forms of imagination: its contents can be freely varied, changed, and recombined to create new arrangements never experienced before. Episodic memory and imagination have in common with other forms of thought that they can arise internally without any stimulation of the sensory organs. But they are still closer to sensation than more abstract forms of thought since they present sensory contents that could, at least in principle, also be perceived.
Risk Factors For Mental Health Problems Among Older Adults
There may be multiple risk factors for mental health problems at any point in life. Older people may experience life stressors common to all people, but also stressors that are more common in later life, like a significant ongoing loss in capacities and a decline in functional ability. For example, older adults may experience reduced mobility, chronic pain, frailty or other health problems, for which they require some form of long-term care. In addition, older people are more likely to experience events such as bereavement, or a drop in socioeconomic status with retirement. All of these stressors can result in isolation, loneliness or psychological distress in older people, for which they may require long-term care.
Mental health has an impact on physical health and vice versa. For example, older adults with physical health conditions such as heart disease have higher rates of depression than those who are healthy. Additionally, untreated depression in an older person with heart disease can negatively affect its outcome.
Older adults are also vulnerable to elder abuse – including physical, verbal, psychological, financial and sexual abuse abandonment neglect and serious losses of dignity and respect. Current evidence suggests that 1 in 6 older people experience elder abuse. Elder abuse can lead not only to physical injuries, but also to serious, sometimes long-lasting psychological consequences, including depression and anxiety.
You May Like: How Fast Can Alzheimer’s Progress
Common Mental Illnesses In The Elderly
If a senior is displaying signs of mental illness, its important to recognize the symptoms and seek treatment as soon as possible. Some of the common mental illnesses the elderly experience are:
- Depression. Depression is considered the most common mental disorder among seniors. Social isolation plays a major role in emotional wellness, so when a senior spends long periods alone because they are unable to drive or live far away from friends and family, depression can easily set in. It is also a symptom of dementia and tends to get overlooked as a treatable ailment.
- Late onset bipolar. Most bipolar patients are diagnosed in early adulthood. Late onset bipolar can be difficult to diagnose because of its similarities to dementia symptoms like agitation, manic behavior and delusions.
- Late onset schizophrenia. This disorder also presents a challenge to diagnose. It can manifest in adults after age 45 and appears as the patient ages. Symptoms are similar to dementia, once again, with hallucinations and paranoia the most common, but these symptoms are milder than when this illness appears in younger adults.
Mental illnesses are treatable, but the trick is a correct diagnosis. Even if a senior had good mental health throughout their entire life, the risk of mental illness in later years is still there. Seek medical treatment as soon as possible if there are any noticeable changes beginning to occur.
What Are The Symptoms Of Dementia
Early symptoms of dementia include :
- Forgetting recent events or information
- Repeating comments or questions over a very short period of time
- Misplacing commonly used items or placing them in usual spots
- Not knowing the date or time
- Having difficulty coming up with the right words
- Experiencing a change in mood, behavior or interests
Signs that dementia is getting worse include:
- Ability to remember and make decisions further declines
- Talking and finding the right words becomes more difficult
- Daily complex tasks, such as brushing teeth, making a cup of coffee, working a tv remote, cooking, and paying bills become more challenging
- Rational thinking and behavior and ability to problem solve lessen
- Sleeping pattern change
- Anxiety, frustration, confusion, agitation, suspiciousness, sadness and/or depression increase
- More help with activities of daily living grooming, toileting, bathing, eating is needed
- Hallucinations may develop
The symptoms mentioned above are general symptoms of dementia. Each person diagnosed with dementia has different symptoms, depending on what area of the brain is damaged. Additional symptoms and/or unique symptoms occur with specific types of dementia.
Also Check: What Is The Difference Between Alzheimer’s And Parkinson’s Disease
Symptoms Interrelation And Evolution
The unitary concept of BPSD encompassing the full range of emotional, psychological, and behavioral abnormalities occurring in dementia reflects the clinical heterogeneity and complexity of the symptoms and the difficulty in characterizing more specific sub-syndromes or proprieties clusters co-varying during the course of the disease. Several studies have tried to identify neuropsychiatric sub-syndromes by grouping a number of individual symptoms which contingently co-occur during the course of dementia . Ultimately, the recognition of discrete clinical entities is important to disclose underlying causal mechanisms and to develop etiological-based therapeutic interventions, even if the precise delineation of each syndrome remains elusive.
Table 1. Neuropsychiatric sub-syndromes reported in patients with dementia.
The debate about the definition of the several psychiatric and behavioral symptoms in dementia continues as a number of symptoms have not been grouped consistently across studies. Particularly, the relation between apathy and the mood sub-syndrome remains unclear. Studies conducted on outpatients and in nursing-homes support that apathy and depression are distinct phenomena and belong to different neuropsychiatric syndromes. However, other studies group both symptoms in the same factor .
Table 2. BPSD and dementia severity: cross-sectional studies.
Table 3. BPSD evolution: longitudinal studies.
Disturbances In Motor Function
Unlike the prior psychopathological domains, disturbances in motor function can be directly observed and consist in reduced or increased motor activity, not necessarily associated with specific motor abnormalities. In motor retardation the patient presents with slowed movements and speech, reduced body tone, and decreased number of spontaneous body movements, whereas motor hyperactivity is characterized by an increased energy level with more frequent movements and/or rapid speech.
Agitation has been defined as inappropriate verbal, vocal, or motor activity that is not judged by an outside observer to result directly from the needs or confusion of the agitated individual . This term is used interchangeably with aberrant motor behavior and encompasses a range of activities such as wandering away from home repetitive, purposeless behaviors social inappropriate activities including those associated with disinhibition . According to Cohen-Mansfield four distinct categories of agitation are: physically non-aggressive behavior verbally non-aggressive behavior physically aggressive behavior and verbally aggressive behavior.
Read Also: What Color Is Alzheimer’s Ribbon
Symptoms For Dementia Sufferers
Alzheimers may also co-exist with psychotic conditions. Older adults who have schizophrenia are just as likely to develop AD as those who have no severe mental illness. They are also at a higher risk for depression, translating to a possible trifecta of co-occurring mental disorders. Symptoms of these disorders include:
- Extreme sadness
- Disinterest in people and previously-enjoyed activities
- Irritability
- Anxiety about change, going out of the house, strangers, etc.
- Feelings of suspicion or paranoia
- Sleep disturbances
Pathophysiology And Neurobiology Of Bpsd
The behavioral or psychological disturbances occurring in dementia can be understood as ineffective attempts of the patient to cope with environmental or physiological stress factors. Indeed, BPSD are also common in non-demented older adults with rates of 5.6% for anxiety, 4.5% for irritability and 2.8% for agitation/aggression while psychotic symptoms are present in up to 10.5% of Swedish 85 years-old people . It is important, therefore, to trace back these symptoms to premorbid psychosocial functioning which is determined by constitutional factors , past experiences and level of education. Abnormalities in the intensity, magnitude, duration, timing, and modifiability of internal conditions and/or observable behaviors are expected to emerge beyond the limits of normal variability as the ongoing neuropathological changes of dementia undermine the individuals usual psychological capacities to adequately respond to everyday demands. Defining these neuroanatomical and neurochemical correlates of BPSD has been an area of active research with a hope that clarification of the underlying neurobiology will lead to more effective treatments .
Table 6. BPSD and structural changes in neuroimaging exams.
Don’t Miss: Multi Infarct Dementia Treatment
Assessment Of Cognitive Function
The Mini-Mental Status Examination or the Montreal Cognitive Assessment is often used as a bedside screening test. When delirium is absent, the presence of multiple deficits, particularly in patients with an average or a higher level of education, suggests dementia. The best screening test for memory is a short-term memory test patients with dementia fail this test. Another test of mental status assesses the ability to name multiple objects within categories . Patients with dementia struggle to name a few those without dementia easily name many.
Neuropsychologic testing should be done when history and bedside mental status testing are not conclusive. It evaluates mood as well as multiple cognitive domains. It takes 1 to 3 hours to complete and is done or supervised by a neuropsychologist. Such testing helps primarily in differentiating the following:
-
Age-associated memory impairment, mild cognitive impairment, and dementia, particularly when cognition is only slightly impaired or when the patient or family members are anxious for reassurance
-
Dementia and focal syndromes of cognitive impairment when the distinction is not clinically evident
Testing may also help characterize specific deficits due to dementia, and it may detect depression or a personality disorder that is contributing to poor cognitive performance.
Writing Literacy And Technology
Throughout history a number of different ways of representing language in graphic media have been invented. These are called .
The use of has made language even more useful to humans. It makes it possible to store large amounts of information outside of the human body and retrieve it again, and it allows communication across physical distances and timespans that would otherwise be impossible. Many languages conventionally employ different genres, styles, and registers in written and spoken language, and in some communities, writing traditionally takes place in an entirely different language than the one spoken. There is some evidence that the use of writing also has effects on the cognitive development of humans, perhaps because acquiring literacy generally requires explicit and .
The invention of the first writing systems is roughly contemporary with the beginning of the in the late . The archaic and the are generally considered to be the earliest writing systems, both emerging out of their ancestral proto-literate symbol systems from 3400 to 3200 BC with the earliest coherent texts from about 2600 BC. It is generally agreed that Sumerian writing was an independent invention however, it is debated whether Egyptian writing was developed completely independently of Sumerian, or was a case of . A similar debate exists for the , which developed around 1200 BC. The are generally believed to have had independent origins.
Also Check: Did Ronald Reagan Have Alzheimer
Language Families Of The World
The world’s languages can be grouped into consisting of languages that can be shown to have common ancestry. Linguists recognize many hundreds of language families, although some of them can possibly be grouped into larger units as more evidence becomes available and in-depth studies are carried out. At present, there are also dozens of : languages that cannot be shown to be related to any other languages in the world. Among them are , spoken in Europe, of , of Mexico, of Japan, of , and many others.
The language family of the world that has the most speakers is the , spoken by 46% of the world’s population. This family includes major world languages like , , , , , and . The Indo-European family achieved prevalence first during the , and subsequently through the , which brought the Indo-European languages to a politically and often numerically dominant position in the and much of . The are spoken by 20% of the world’s population and include many of the languages of East Asia, including Hakka, , , and hundreds of smaller languages.
is home to a large number of language families, the largest of which is the , which includes such languages as , , and . Speakers of the Niger-Congo languages account for 6.9% of the world’s population. A similar number of people speak the , which include the populous such as , , and the languages of the region, such as the and .
Social Contexts Of Use And Transmission

While humans have the ability to learn any language, they only do so if they grow up in an environment in which language exists and is used by others. Language is therefore dependent on in which children from their elders and peers and themselves transmit language to their own children. Languages are used by those who speak them to and to solve a plethora of social tasks. Many aspects of language use can be seen to be adapted specifically to these purposes. Owing to the way in which language is transmitted between generations and within communities, language perpetually changes, diversifying into new languages or converging due to . The process is similar to the process of , where the process of descent with modification leads to the formation of a .
However, languages differ from biological organisms in that they readily incorporate elements from other languages through the process of , as speakers of different languages come into contact. Humans also frequently speak more than one language, acquiring their or languages as children, or learning new languages as they grow up. Because of the increased language contact in the globalizing world, many small languages are becoming as their speakers shift to other languages that afford the possibility to participate in larger and more influential speech communities.
Don’t Miss: Dementia Awareness Ribbon
What Medications Are Available To Treat Dementia
Drugs approved for the most common form of dementia, Alzheimers disease, are discussed below. These drugs are also used to treat people with some of the other forms of dementia.
- cholinesterase inhibitors
- NMDA receptor antagonist memantine
These two classes of drugs affect different chemical processes in the brain. Both classes have been shown to provide some benefit in improving or stabilizing memory function in some patients. Although none of these drugs appear to stop the progression of the underlying disease, they may slow it down.
If other medical conditions are causing dementia or co-exist with dementia, the appropriate drugs used to treat those specific conditions are prescribed.
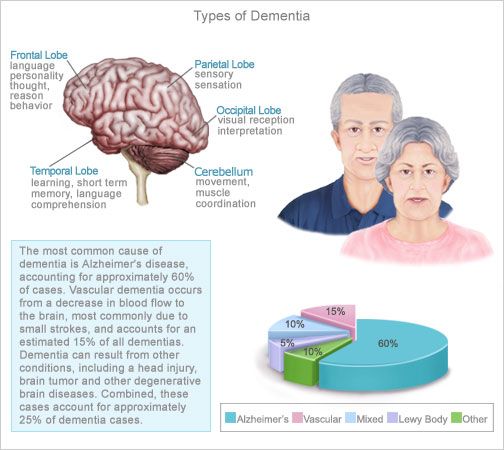
What Are The Types Of Dementia
Dementias are often broken down into two main categories — Alzheimer type or non-Alzheimer type. Dementias of the Alzheimers disease type are defined by the symptoms of memory loss plus impairment in other brain functions, such as language function inability to move the muscles associated with speech or perception, visual or other inabilities to recognize speech or name objects .
Non-Alzheimer dementias include the frontotemporal lobar degenerations, which are further broken down into two main types. One type primarily affects speech. An example is primary progressive aphasia syndromes. The other type is defined by changes in behavior, including lack of feeling, emotion, interest or concern loss of a social filter personality change and loss of executive functions . In both of these frontotemporal lobe dementias, memory loss is relatively mild until later in the course of the disease.
Other non-Alzheimers disease dementias include vascular disorders , dementia with Lewy bodies, Parkinson’s dementia, and normal pressure hydrocephalus.
You May Like: When Does Late Onset Alzheimer’s Start
Unusual Neurological Syndromes That May Present As Psychiatric
In the second part of this article, we highlight a number of neurological syndromes which, because of their predominantly behavioural and sometimes bizarre presentations, are often mistakenly diagnosed as psychiatric. We group these according to the neuropsychiatric function most prominently disturbed.
Home / Why Ncds / Ncds / Mental Health And Neurological Disorders
Mental and neurological disorders include diseases such as depression & dementia.
Mental and neurological disorders, diverse in problems and symptoms, affect thoughts, emotions, behaviour and relationships. Neurological and mental disorders, for example depression, dementia, autism, epilepsy and schizophrenia, can be experienced in isolation, or as co-morbidities with other NCDs. There is overlap with risk factors with the other non-communicable diseases, and neurological and mental diseases are also often chronic in nature.
Recommended Reading: What Color Represents Alzheimer’s