Numbers Of People With Dementia
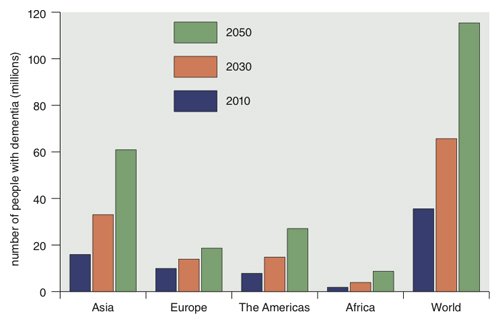
Someone in the world develops dementia every 3 seconds. There are over 55 million people worldwide living with dementia in 2020. This number will almost double every 20 years, reaching 78 million in 2030 and 139 million in 2050. Much of the increase will be in developing countries. Already 60% of people with dementia live in low and middle income countries, but by 2050 this will rise to 71%. The fastest growth in the elderly population is taking place in China, India, and their south Asian and western Pacific neighbours.
Demographic ageing is a worldwide process that shows the successes of improved health care over the last century. Many are now living longer and healthier lives and so the world population has a greater proportion of older people. Dementia mainly affects older people, although there is a growing awareness of cases that start before the age of 65.
There are over 10 million new cases of dementia each year worldwide, implying one new case every 3.2 seconds.
Monetary Costs Of Dementia Care Shouldered By Families
Dementia care is more costly than other conditions and puts a disproportionate burden on families. What people with dementia need most is supervision and help with personal care and household activitiesservices not covered by Medicarewhereas the drugs or surgeries commonly used to treat conditions such as heart disease and cancer are covered.
The lifetime cost of dementia is high, report researchers from the RAND Corporation. Using HRS data, RAND researchers found that those who live with dementia for at least six months pay, on average, $38,500 more out of pocket from age 65 to death .24 These dementia-related costs are nearly all composed of spending on nursing homes.
Similarly, Amy Kelley and colleagues used HRS data to show that health care for Medicare beneficiaries in the last five years of life was far more costly and involved significantly higher uncovered out-of-pocket costs for those with dementia than for those with heart disease, cancer, or other medical conditions.25 Out-of-pocket costs averaged $62,000 for people with dementia, more than 80% higher than for someone with heart disease or cancer.
The challenge, according to the researchers, is that Medicare does not cover health-related expenses most valuable to those with chronic diseases or a life-limiting illness, such as homecare services, equipment, and non-rehabilitative nursing home care. These costs are largely borne by individuals and families, particularly among vulnerable subgroups.26
Figure 1 Dementia Prevalence Rates Vary Widely Across Different Groups
Prevalence of Probable Dementia Among the U.S. Population Ages 70 and Older, 2015
Note: Excludes persons in nursing homes. Vicki A. Freedman et al., Short-Term Changes in the Prevalence of Probable Dementia: An Analysis of the 20112015 National Health and Aging Trends Study,Journals of Gerontology, Series B 73 : S48-S56.
Dementia prevalence increases with age. About 5% of adults ages 70 to 79 had probable dementia in 2015, compared with 16% of adults ages 80 to 89 and 31% of adults ages 90 and older. As the U.S. population grows older, the number of people with dementia is projected to increase sharply.10
Women are slightly more likely to have dementia than men. Among adults ages 70 and older, 10.1% of women and 9.6% of men had probable dementia.
Non-Hispanic whites have lower rates of dementia than other racial/ethnic groups. The rates of probable dementia among Hispanic and other racial/ethnic minorities ages 70 and older was double the rate among non-Hispanic white older adults . Recent declines in dementia prevalence have been concentrated among non-Hispanic white and non-Hispanic black groups, whereas dementia prevalence has been persistently higher among the Hispanic/Latino population.11
You May Like: What Color Is The Dementia Ribbon
Trends In Subjectively Rated Memory Iadl Limitations And Nursing Home Residence
Some variables that are known to correlate with cognitive ability are available both in proxy and in self-interviews. These include subjectively rated memory, number of limitations in instrumental activities of daily living , and whether the respondent lives in a nursing home. As they are available in all interviews, they do not suffer from selection into proxy interviews.
shows the trends in those variables. We find little improvement in subjectively rated memory except among older females, for whom the proportion with poor memory decreased by more than 4 percentage points. We find some improvements in IADL: the fraction living with more than three such limitations decreased from 8.0% in 2000 to 7.0% in 2012, with a noticeably larger decrease among males. The overall proportion living in nursing homes also decreased from 4.6% in 2000 to 2.9% in 2012. These trends indicate some moderate improvements in cognitive ability for HRS respondents 65 years of age or older.
What Can You Do Today
Early screening is by far the most effective way to help detect Alzheimers and other types of dementia. Early detection of dementia may be able to allow intervention to ameliorate or delay the onset of symptoms. This can improve the overall quality of life for both you and your loved ones. While there is currently no cure for dementia, there are several medications that can help treat symptoms. Knowing sooner can also allow you to make many important decisions, such as planning for long-term care, and organizing estate affairs.
Currently, the easiest and most convenient way to screen for Alzheimers and dementia is by using the BrainTest® app. The app offers an easy-to-use electronic version of the SAGE test, a test designed by The Ohio State University Wexner Medical Center to detect early signs of cognitive, memory or thinking impairments. Screen early and take control of your brain health today.
Pennington Biomedical Research Center. FAQ. Institute for Dementia Research & Prevention. Retrieved from
WHO. . Dementia. World Health Organization. Retrieved from
Read Also: Smelling Farts Cure Cancer
Differences Between Women And Men In The Prevalence And Risk Of Alzheimer’s And Other Dementias
More women than men have Alzheimer’s or other dementias. Almost two-thirds of Americans with Alzheimer’s are women., Of the 5.8 million people age 65 and older with Alzheimer’s in the United States, 3.6 million are women and 2.2 million are men., Based on estimates from ADAMS, among people age 71 and older, 16% of women have Alzheimer’s or other dementias compared with 11% of men.
The prevailing reason that has been stated for the higher prevalence of Alzheimer’s and other dementias in women is that women live longer than men on average, and older age is the greatest risk factor for Alzheimer’s.- But when it comes to differences in the actual risk of developing Alzheimer’s or other dementias for men and women of the same age, findings have been mixed. Most studies of incidence in the United States have found no significant difference between men and women in the proportion who develop Alzheimer’s or other dementias at any given age., , – However, some European studies have reported a higher incidence among women at older ages,, and one study from the United Kingdom reported higher incidence for men. Differences in the risk of dementia between men and women may therefore depend on age and/or geographic region.,
How To Gain Weight
If you want to add on numbers to the weight and reach the adequate weight number, it is compulsory to do it in the right direction. But, people often do it in the wrong way and drive their journey in the wrong direction. They stick to junk food and affect their health.
- Ingest protein in every meal. A high amount of protein can increase muscle density and regulate overall health.
- Load your diet with good carbohydrates and fats.
- Have a meal at least 3 times per day.
- Include dry fruits and nuts.
- Have peanut butter, which increases good fats in the body
- Have dairy products.
- Have meat, like chicken, pork and lamb.
- Include tubers like potatoes, sweet potatoes and yams.
- Exercise thrice a week to build muscles.
- Have dark chocolates and avocado.
- Have a quality sleep.
You May Like: Purple Ribbon Alzheimers
Most People With Dementia Live In Settings Other Than Nursing Facilities
In 2015, about 85% of Americans with probable dementia lived at home in the community or in supportive care settings , whereas about 15% lived in nursing facilities.16 Among those with dementia living in settings other than nursing homes in 2011, 80% were in traditional community settings and about 20% lived in residential care settings .17
The availability and capacity of family and other informal caregivers, income and asset levels, and the type of care needed all contribute to determining the setting in which older adults with dementia live. Eligibility for government programs and the availability of services, some of which vary by state, also play key roles.
People with advancing dementia who live at home are more likely to be racial and ethnic minorities, foreign born, and less educated. Krista Harrison and colleagues used NHATS data to examine the living arrangements of older adults with advancing dementia, defined as probable dementia that interferes with some aspects of personal care or household activities.18 Those living at home were much more likely to be black or Hispanic, not born in the United States, and lack a high school diplomacharacteristics that are linked to socioeconomic disadvantage and health disparities .
Where People With Dementia Live And How They Receive Care Depends Partly On Their Ability To Pay
Most older people, including those with dementia and their caregivers, prefer to receive care at home rather than in nursing facilities, and many families take pride in providing care themselves. Reflecting these preferences, an increasing proportion of Medicaid funds for lower-income older adults are being spent on home- and community-based services and support rather than on institutional care.20 These services vary considerably by state and aim to enable people with dementia to continue living at home or in a residential care setting rather than in more costly nursing facilities.
Higher-income people with dementia are somewhat more likely to live in residential care, whereas lower-income people with dementia are more likely to live in nursing homes or at home.21 Medicare and Medicaid policies contribute to shaping these residential patterns. Medicare does not pay for most long-term support and care in either a residential care setting, such as an assisted living facility, or a nursing home. For lower-income older adults , Medicaid may pay a portion of supportive care costs, primarily in nursing facilities, depending on the state. The median annual cost of assisted living, one type of residential care that typically provides social but not medical support, was $49,000 in 2019. The median annual cost of a nursing facility that provides medical support, which often serves lower-income older people with Medicaid coverage, was $90,000.22
Don’t Miss: Dementia Ribbon Color
Dementia Cases May Triple Globally By : Study
Smoking, obesity and high blood sugar are risk factors for dementia.
Dementia cases may triple by 2050, study warns
Unless countries act swiftly to address dementia risk factors, global cases of dementia may triple by 2050, according to a new study published Thursday in the Lancet.
“Our study offers improved forecasts for dementia on a global scale as well as the country-level, giving policy makers and public health experts new insights to understand the drivers of these increases, based on the best available data,” lead author Emma Nichols, from the Institute for Health Metrics and Evaluation at the University of Washington, said in a statement.
A new mathematical model used for the study estimates that the global prevalence of dementia could nearly triple by 2050 — from 57 million to 153 million — with cases in the U.S. increasing from 5.2 million to 10.5 million.
Dementia is currently the seventh-leading cause of death worldwide, according to the World Health Organization. It contributes to significant disability in older people with associated costs globally reaching $1 trillion U.S. in 2019, the WHO reported.
While there are higher rates of dementia in older individuals, it should not be viewed as a normal part of aging. Many risk factors have been linked to dementia, but researchers focused on four predictive risk factors that can be improved: obesity, smoking, high blood sugar and low education.
Who Is Dementia Australia
Dementia Australia is the source of trusted information, education and services for the estimated half a million Australians living with dementia, and the almost 1.6 million people involved in their care. We advocate for positive change and support vital research. We are here to support people impacted by dementia, and to enable them to live as well as possible.
No matter how you are impacted by dementia or who you are, we are here for you.
Dementia Australia, the new voice of Alzheimers Australia, is the national peak body for people, of all ages, living with all forms of dementia, their families and carers. It provides advocacy, support services, education and information.
Don’t Miss: Neurotransmitters Involved In Alzheimer’s Disease
Dementia Assessment And Diagnosis
All participants were assessed for dementia in person in their residence by a nurse and neuropsychology technician. The full details of this assessment and diagnostic procedures have been previously described . Briefly, the following information about the respondent was collected from a knowledgeable informant: a detailed chronological history of cognitive and functional symptoms, medical history, current medications, current neuropsychiatric symptoms, measures of severity of cognitive and functional impairment, and family history of memory problems. During the assessment, the respondent completed: a battery of neuropsychological measures a self-report depression measure a standardized neurological examination a blood pressure measurement collection of buccal DNA samples for apolipoprotein E genotyping, and a 7-min videotaped segment covering portions of the cognitive status and neurological examinations. The neuropsychological battery has been described elsewhere and included measures of orientation, verbal and visual immediate and delayed memory, language, attention, executive function, praxis, reading ability and general intellect. Medical record releases were also sought to obtain relevant prior neuroimaging and laboratory results from the respondents physicians.
What Is Dementia And What Is Alzheimer’s Disease
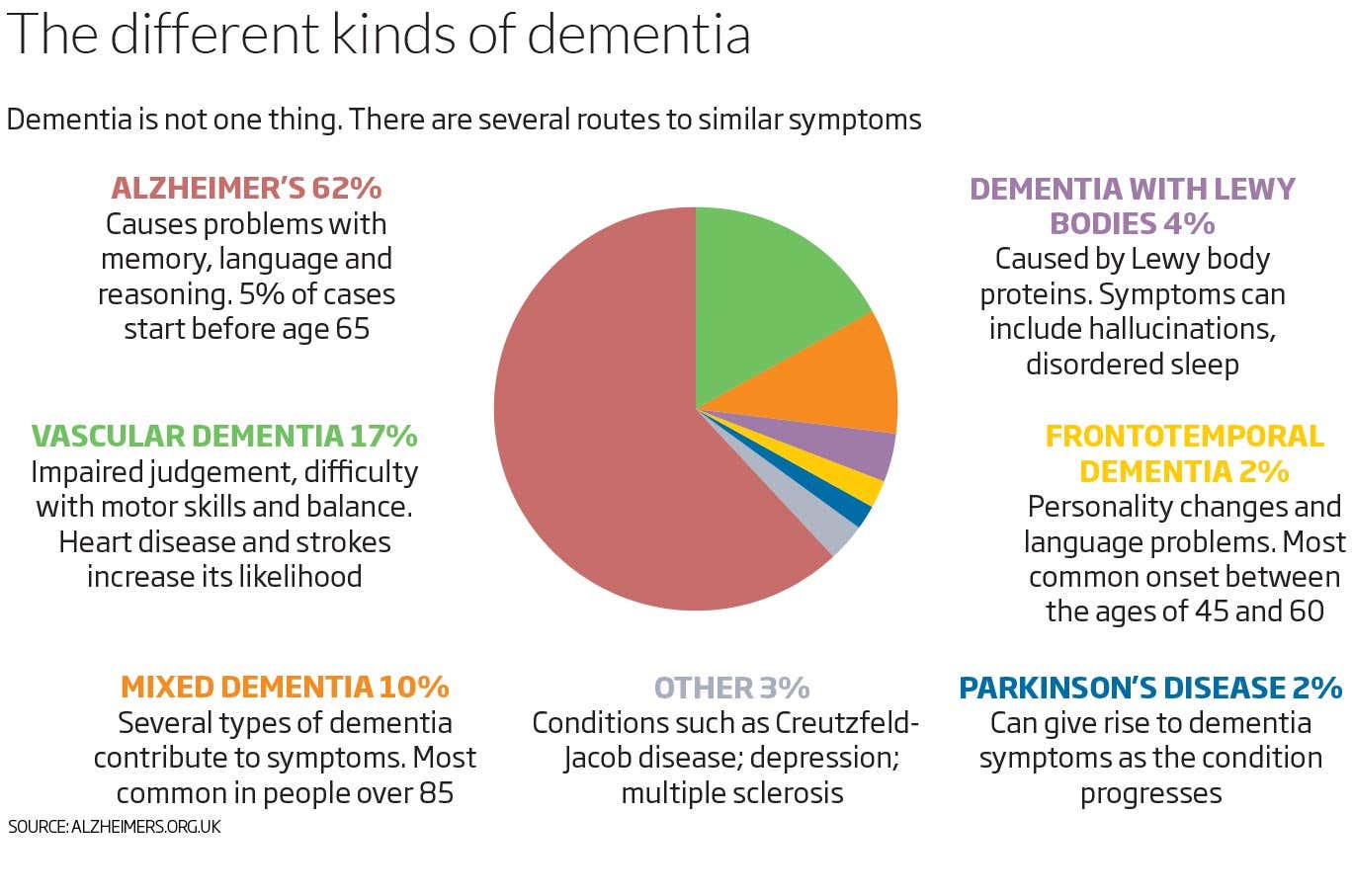
Dementia refers to a set of symptoms and signs associated with a progressive deterioration of cognitive functions that affects daily activities. It is caused by various brain diseases and injuries. Alzheimer’s disease is the most common cause of dementia. Vascular dementia, frontotemporal dementia, and Lewy body dementia constitute other common types. Symptoms of dementia can include memory loss, judgement and reasoning problems, and changes in behaviour, mood and communication abilities.Footnote 4
Recommended Reading: How Fast Does Ftd Progress
Avoidable Use Of Health Care And Long
6.5.1 Preventable hospitalizations
Preventable hospitalizations are one common measure of health care quality. Preventable hospitalizations are hospitalizations for conditions that could have been avoided with better access to, or quality of, preventive and primary care. Unplanned hospital readmissions within 30 days are another type of hospitalization that potentially could have been avoided with appropriate post-discharge care. In 2013, 21% of hospitalizations for fee-for-service Medicare enrollees with Alzheimer’s or other dementias were either for unplanned readmissions within 30 days or for an ambulatory care sensitive condition . The total cost to Medicare of these potentially preventable hospitalizations was $4.7 billion . Of people with dementia who had at least one hospitalization, 18% were readmitted within 30 days. Of those who were readmitted within 30 days, 27% were readmitted two or more times. Ten percent of Medicare enrollees had at least one hospitalization for an ambulatory care-sensitive condition, and 14% of total hospitalizations for Medicare enrollees with Alzheimer’s or other dementias were for ambulatory care sensitive conditions.
FIGURE 16
| 15,417 | 46,252 |
Number Of People With Dementia Set To Jump 40% To 78 Mln By 2030
Register now for FREE unlimited access to Reuters.com
- More than 55 million people living with dementia – report
- Prevalence on rise, set to affect 78 million by 2030
- Risk factors include diet, hypertension, depression
GENEVA, Sept 2 – More than 55 million people worldwide are living with dementia, a neurological disorder that robs them of their memory and costs the world $1.3 trillion a year, the World Health Organization said on Thursday.
The progressive condition can be caused by stroke, brain injury or Alzheimer’s disease. With populations ageing, the number of sufferers is projected to rise to 78 million by 2030 and 139 million by 2050, the WHO said in a report.
Only one in four countries has a national policy in place to support dementia patients and their families, it said, urging governments to step up to the public health challenge.
Register now for FREE unlimited access to Reuters.com
“Dementia robs millions of people of their memories, independence and dignity, but it also robs the rest of us of the people we know and love,” said Tedros Adhanom Ghebreyesus, WHO director-general.
“The world is failing people with dementia, and that hurts all of us,” he said.
Health ministers agreed in 2015 on a global action plan, including early diagnosis and providing care, but are falling short on meeting targets by 2025, it said.
Dementia affects memory, orientation, learning capacity, language, judgement, and the ability to perform everyday tasks.
Recommended Reading: Senility Vs Alzheimer’s
Heart Disease And Stroke
According to the Alzheimers Society, a person who has had a stroke or has heart disease is twice as likely to develop vascular dementia.
In the United States, a Black person is around one and a half times more likely to have a stroke than a white person. Data from 2018 suggests Black Americans were 30% more likely than white Americans to die from heart disease.
But a raised risk of developing heart disease may due to factors such as high blood pressure or poor diet.
Poor diet can be the result of socioeconomic difficulties. Data from the 2019 census shows that 17.4% of African American families were living under the poverty line at that time. Just 5.5% of non-Hispanic white families were living in the same situation.
Socioeconomic difficulties may mean a person has limited access to fresh food and fewer opportunities to exercise.