Box : Risk Factors Associated With Minor Neurocognitive Disordersa
Factors associated with developing minor neurocognitive disorders
- Lower scores on cognitive testing than controls including MMSE, ADAS-cog, and tests assessing memory and executive functioning
- APOE 4 genotype intermediate between controls and patients with AD
- CSF tau levels intermediate between controls and patients with AD
- Hippocampal volumes approximately one standard deviation smaller than controls
- Larger ventricular volumes than controls
- Decreased FDG-PET uptake in bilateral angular gyrus, posterior cingular, and bilateral inferior temporal gyrus compared with controls
Risk factors for progression from minor neurocognitive disorders to AD
- Amnestic subtype of mild cognitive impairment
- Smaller hippocampal volumes than controls
- More APOE 4 allele carriers higher CSF tau levels decreased FDG-PET uptake as above smaller hippocampal volumes larger ventricular volume lower ADAS-cog, memory, and executive function scores than patients with mild cognitive impairment at lower risk of developing AD
- Major depression
___________________
A major NCD is defined as a significant decline in cognitive abilities that is severe enough to interfere with the individuals everyday activities, such as paying bills, dressing, or preparing meals. The major NCDs are further defined as being probable or possible, classified on the basis of whether there is a behavioral disturbance, and rated for severity .
Delirium And Dementia Neurocognitive Disorders
- Comments
Over the years, delirium and dementia neurocognitive disorders have developed, and many people across the globe have been affected by these disorders. However, many people still do not know the difference between the two due to their similarities in causes and symptoms. Delirium is defined as the sudden change in a persons mental state. On the other hand, dementia is a range of signs that a persons brain is not functioning correctly. The primary difference between the two is that delirium occurs over a short period while dementia takes some time, a week, month or even a year to develop .
The two neurocognitive disorders have some common causes and symptoms. These similar causes include head injury, genetics, and downs syndrome. Studies show that dementia can also be caused old age while the chances of developing delirium due to old age are relatively low. Another vital difference between the causes of the two disorders is that dementia can be caused by illnesses such as CJD, AIDS infection and other abnormalities such as depression, vitamin deficiencies, and thyroid abnormalities are also known to damage brain cells and cause dementia. However, these cases do not result in delirium .
Works cited
Girard, Timothy D., et al. Delirium as a predictor of long-term cognitive impairment in survivors of critical illness. Critical care medicine 38.7 : 1513.
World Health Organization. Dementia: a public health priority. World Health Organization, 2012.
Versin Impresa Issn 0213
Resumen
PUJOL DOMENECH, Joaquim y AZPIAZU ARTIGAS, Pilar de.Dementia DSM-IV/ICD-10 or neurocognitive disorder DSM-5?. Eur. J. Psychiat. . 2015, vol.29, n.1, pp.45-50. ISSN 0213-6163. https://dx.doi.org/10.4321/S0213-61632015000100004.
Palabras clave:Dementia DSM-5 Neurocognitive disorders Mild Cognitive Impairment Mild Neurocognitive Disorder.
Also Check: Pathophysiology Of Dementia Disease
Causes And Risk Factors
The most significant predictor of developing major neurocognitive disorder is age.
Major neurocognitive disorder may be caused by a variety of factors noted in the DSM-5 as specifiers. These specifiers are:
- multiple etiologies
- unspecified
Females have a higher risk of developing a major neurocognitive disorder, especially Alzheimers disease. This may be because females live longer on average than males.
Major neurocognitive disorder is not currently curable. However, some treatments can alleviate symptoms or slow the progression of cognitive decline.
Treatment is mainly dependent on the specific cause.
In some cases, cognitive training may help improve cognition or slow down the progression of symptoms. This non-pharmacological treatment uses guided practices to improve memory, problem-solving, or attention. This type of skills training focuses on the improvement of specific cognitive functions.
One study in 2018 examined the pharmacological treatments of major neurocognitive disorders.
The researchers recommended that non-pharmacological treatments should be the first line of treatment for major neurocognitive disorders due to the risks and side effects linked with antipsychotics, such as mortality from stroke, myocardial infarction, or infection.
Doctors often prescribe antipsychotics as a treatment for major neurocognitive disorders.
Standard antipsychotics that can be effective for symptoms include:
Mild And Major Neurocognitive Disorder
Mild and major neurocognitive disorders are usually associated with but not restricted to the elderly. Unlike delirium, conditions under these disorders develop slowly and are characterized by memory loss. In addition to memory loss and cognitive impairment, other symptoms include aphasia, , agnosia, loss of abstract thought, behavioral/personality changes, and impaired judgment. There may also be behavioral disturbances including psychosis, mood, and agitation.
Mild and major neurocognitive disorders are differentiated based on the severity of their symptoms. Also still known as dementia, major neurocognitive disorder is characterized by significant cognitive decline and interference with independence, while mild neurocognitive disorder is characterized by moderate cognitive decline and does not interfere with independence. To be diagnosed, it must not be due to delirium or other mental disorder. They are also usually accompanied by another cognitive dysfunction. For non-reversible causes of dementia such as age, the slow decline of memory and cognition is lifelong. It can be diagnosed by screening tests such as the Mini Mental State Examination .
You May Like: Dementia Vs Senility
Diagnosing Mild Cognitive Impairment
Theres no official diagnostic test for MCI. Your doctor will likely take a thorough history and perform blood tests to look for any underlying conditions that may be contributing to memory issues.
They may conduct interviews and mental function tests, on top of brain imaging and neurological exams, to assist with a diagnosis. Biomarker tests can also help determine whether you have Alzheimers disease.
Your doctor will ask questions about your ability to carry out common activities associated with daily life. These activities, which are called instrumental activities of daily living include:
- taking medications
- using a phone or other electronic device
- shopping
What Is Dementia Dsm
DSM-5: Neurocognitive DisorderDementia is the umbrella term for a number of neurological conditions, of which the major symptom is the decline in brain function due to physical changes in the brain. It is distinct from mental illness. New diagnostic criteria for dementia were developed and released in 2013.
You May Like: At What Age Alzheimer’s Start
Walking And Physical Movement
Vascular dementia: Vascular dementia is often accompanied by some physical challenge. If a person has a stroke, they may have limited movement on one side of her body. Both the cognitive and physical impairments related to vascular dementia usually develop at the same time since they are often the result of a sudden condition like a stroke.
Alzheimers: Often, mental abilities like memory or judgment decline initially, and then as Alzheimer’s progresses into the middle stages, physical abilities like balance or walking show some deterioration.
Dementia In The Population
Prevalence, defined as the proportion of people with an illness in agiven population at a given time, is an index of the burden of disease in thepopulation. Incidence is the rate at which new disease occurs in a givenpopulation, i.e., the proportion of new cases in that population over a givenperiod of time. Incidence is therefore an index of the risk of disease in thatpopulation. Prevalence is a function of both incidence and duration. Since mostdementias are not curable, their duration reflects how long individuals livewith their dementia. Thus, the public health burden of dementia depends both onthe development of new cases and on the survival of those cases after onset holding incidence constant, groups with longer life expectancy will have higherprevalence.
You May Like: Dementia Ribbon
Understanding Mild Cognitive Disorder
The development and course of mild neurocognitive disorder varies greatly due to the number of causal subtypes. The symptoms associated with traumatic brain injury or stroke subtypes will improve after initial inflammation or swelling reduce.
Neurodegenerative diseases such as Alzheimers disease or frontotemporal lobar degeneration are associated with a slow onset and steady progression of symptoms. Environmental and genetic factors also vary by subtype and age of onset within the subtypes. Overall, the strongest risk factor for major and mild neurocognitive disorders is age due to the increased risk of neurodegenerative and cerebrovascular disease.
Individuals with neurocognitive disorders can present with a wide variety of mood disturbances including depression, apathy, anxiety, and elation. Sleep disturbance is also common and may include symptoms of insomnia, hypersomnia, or circadian rhythm disorder. Delirium commonly co-occurs with neurocognitive disorders in the older population. For younger individuals, neurodevelopmental disorders such as attention-deficit/hyperactivity disorder are a frequent comorbidity.
Whats In A Name: Senility Dementia Or Neurocognitive Disorder And Does It Matter
It used to be called senility which, according to the online etymology dictionary, comes from the French, sénile, or suited to old age, from Latin senilis of old age, etc. Senility, or what we now generally call dementia, was initially considered to be simply part and parcel with the aging process. We no longer recognize that to be the case , and generally the term senility has gone out of fashion to being outright discouraged , due to its ageist connotations.
Now, of course, even the term dementia is going out of fashion with the advent of the DSM-V and the preferred term is major neurocognitive disorder or MNCD. A couple of things to remember here since were talking about etymologies , the origin of the word dementia may even be a bit harsh as well, from the perspective of those who carry the diagnosis according to the same etymology dictionary dementia originates from the latin term demens literally mad, raving..
Don’t Miss: Dementia Ribbon Tattoo
What Is Mild Neurocognitive Disorder
Mild neurocognitive disorder is an acquired disorder that affects 2-10% of adults by age 65 and 5-25% of adults by age 85.
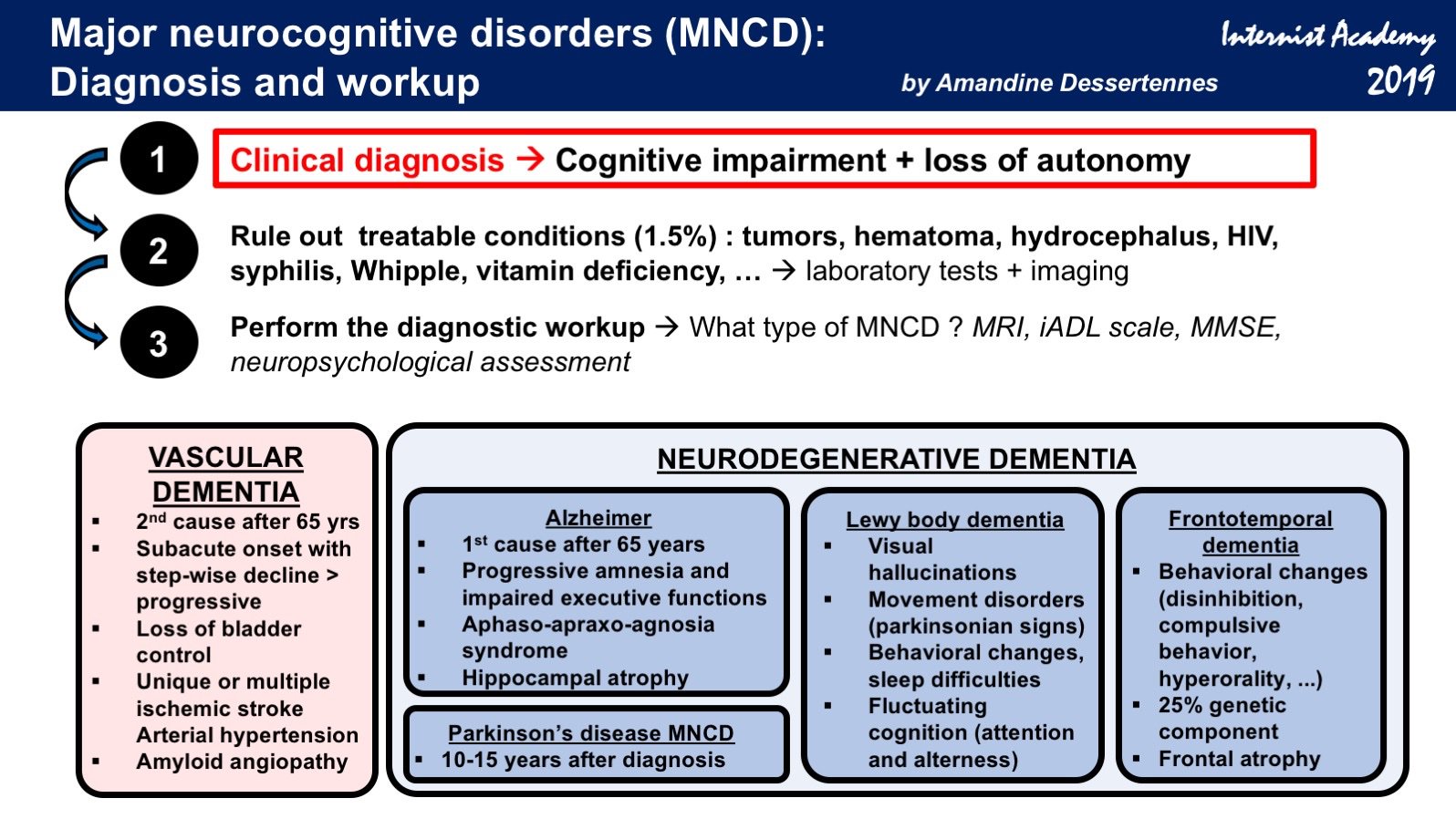
Mild neurocognitive disorder is characterized by moderate cognitive decline from a prior level of performance in one or more cognitive domains:
- Complex Attention: tasks take longer to complete than previously, work needs to be double-checked for errors, difficulty thinking and processing information when multi-tasking
- Executive Functions: requires more effort to finish multistep projects, trouble resuming a task that was interrupted, has difficulty organizing, planning or making decisions, trouble following shifting conversations
- Learning and Memory: difficulty recalling recent events, relies on reminders and list-making
- Language: word-finding difficulty, grammatical errors in expressive language
- Perceptual-Motor: may rely more heavily on maps or notes for directions, may expend more effort on motor tasks such as typing, knitting, or assembly
- Social Cognition: minor changes in behavior or personality, less ability to read social cues such as facial expressions, decreased empathy, or decreased inhibition
Where Does Alzheimer’s Fit In

Alzheimers disease is the most common type of major neurocognitive disorder, but it is only one of many possible causes. Vascular cognitive impairment, dementia with Lewy bodies, frontotemporal dementia, Parkinsons disease, Huntingtons disease, HIV, traumatic brain injury, and other conditions each can cause severe cognitive changes.
Recommended Reading: Aphasia And Alzheimer’s
Lets Break Down Dementias New Name: Neurocognitive Disorder
- neuro means having to do with the brain
- cognitive is a fancy way of saying thinking
- disorder the opposite of order, effectively means functioning in a new way
The basis for giving someone a neurocognitive disorder diagnosis amounts to determining that their brain works differently than most in at least two ways. Cognition, or thinking, is the easiest part of the dementia experience to measure. Eminent dementia researcher and practitioner Tom Kitwood in his article Positive long term changes in dementia: Some preliminary observations explained:
The culture of the western world has itself tended to set a high premium upon cognition its established system of education, for example, is designed to differentiate people on the basis of their cognitive performance, while neglecting the sensibilities. It is also the case that in dementia the changes that occur in cognitive function are relatively simple to measure, and these have provided a legitimate basis both for assessment and for drug trials.
I want to be clear I know and see daily the challenges and suffering dementia can bring. I also know and see daily the beautiful joys and learning it can bring, to those experiencing it and those that care for them. Can we have a perspective on dementia that holds both the challenges and the joys? They are not mutually exclusive.
For more on this perspective on dementia come see The ChangingAging Tours show Disrupt Dementia.
Education And Cognitive Activity
Where educational opportunities are universal, higher education mayreflect innate reserve the process of education may also promote thedevelopment of reserve through mechanisms such as increased dendritic branching.Education may also reflect general socioeconomic status and thus also representquality of environmental factors like nutrition, or health care. Regardless ofmechanism, higher education is associated with lowerprevalence of dementia.
Bilingualism has been associated with delayedonset of dementia,independent of education, and may specifically protect against declines inattention and executive functioning.
Cognitive activity: Lifelong occupations that donot require higher education or skilled vocational training appear to beassociated with a higher risk of dementia., Several popular leisureactivities have been found associated with lower risk of dementia. Cognitively stimulatingactivities appear to have both protective and enhancing effects oncognition.
Also Check: Does Alzheimer’s Cause Dementia
Predictors Of Hand Progression
Of the original 104 enrolled, 45 patients had a follow-up examination within 1 year. Others were seen at different time intervals so we excluded them from this ana lysis to ensure we had consistency with regard to the time elapsed from baseline to determine progression of HAND. Of the 45 patients, 32 were men, which was not significantly different from the total cohort. Of the 45 patients, 14 showed declines in neurocognitive function, 25 were stable and six showed improved function at 1-year follow-up relative to their baseline neuro cognitive status. Based on polytomous logistic regression, individuals with an age greater than or equal to 50 years were more likely to demonstrate neurocognitive decline compared with those with an age younger than 50 years , after adjusting for college education, gender, race, depression symptoms, substance abuse, hepatitis C status and CD4+ cell count less than 200 cells/mm3. In the same model, women were more likely to demonstrate worsening of neurocognitive status compared with men . Owing to this finding, we stratified the demographic and clinical data by gender. In this subset of 45 follow-up visits, of the 15 people aged 50 years or greater, four were women. Of the 30 people aged under 50 years, nine were women. There was no difference in distribution of gender between these two age groups . Women, however, had significantly fewer years of education and higher CD4+ cell counts compared with men.
Dementia Pagal Or Neurocognitive Disorder: What Is In A Name
A recent BBC news story has drawn attention to the fact that there isnt a word for dementia in many South Asian languages and some South Asian people living in the UK still use the stigmatising Punjabi word pagal, meaning crazy or mad. The news story implicitly assumes that the word dementia is non-stigmatising but this is disputed. If the word dementia is itself stigmatizing, are anglophones really in a position to criticize other languages? Can we adopt a non-stigmatising word for dementia?
Pagal is problematic for at least two reasons. First, it reduces all mental illness to a single category unhelpfully effacing the differences between them and thereby preventing targeted treatment and management. Second, to be labelled pagal comes with significant stigma. An interviewee in the BBC story, Mr Singh, tells us that his father, once diagnosed with Alzheimers, was no longer welcome at social events and his wife would stay at home with him while the rest of the family attended. Dr Sahdia Parveen, a senior research fellow at the Centre for Applied Dementia Studies , tells us that the stigma can also extend to the family. It can be more difficult to find a partner if ones relative has dementia because of an assumption that the condition is hereditary.
Pagal, or crazy for that matter, are obviously not helpful words to describe people living with dementia.
Don’t Miss: Alzheimer’s Awareness Color
What Is The Difference Between Mild And Major Alzheimer’s Disease
MCI refers to relatively minor impairments in thought processes and memory, whereas Alzheimers is a specific disease in which memory and functioning continue to significantly decline over time.
MCI isnt considered dementia, but roughly 10 to 15 percent of people with MCI may develop dementia each year, including a specific type of dementia known as Alzheimers disease.
What Does Major Neurocognitive Disorder Mean
Major Neurocognitive Disorder previously called dementia is a syndrome that progresses with significant deterioration of cognitive domains as compared to previous levels of cognitive performance in memory, speech, reasoning, intellectual function, and/or spatiotemporal perception, and may also be associated
You May Like: Does Medicare Cover Respite Care For Dementia
What Is Major Vascular Neurocognitive Disorder
Major vascular neurocognitive disorder is the second leading form of dementia after Alzheimers disease, accounting for 17-20% of all dementias. Vascular. NCD is a progressive disease caused by reduced cerebral blood flow related to multiple large volume or lacunar infarcts that induce a sudden onset and stepwise.
Neurocognitive Disorder Is The New Dementia
When I had to select a population to work with for my clinical psychotherapy training, I was drawn to elders because in contrast to other populations, I believed I would not be expected to fix anyone. We cannot cure aging, right? I was lucky enough to find a training site that believed as I did- a person is a person no matter what, an orientation called humanism.
Where I worked, the diagnosis I come across most often was that of dementia. The single greatest risk factor for dementia is age, therefore, in working with elders, it is an often presented diagnosis. Like other aspects of aging dementia affects everyone differently. From a humanistic orientation, a perspective on dementia can be opened to where one can hold the medical realities of decline AND be curious about what else is present or may be emerging. It is from this humanistic perspective that I will explore a dementia diagnosis, offering a foundation in the medical model and expanding from there.
Read Also: Alzheimer’s Purple Ribbon