Aicd Does Not Alter App Processing Or Increase A Levels In Transgenic Mice
Most of the pathological features described above have also been observed in mouse models of AD, with accumulation of A being implicated as the underlying cause. To determine if the deleterious events in AICD transgenic mice could be due to increased A levels, we examined whether APP processing was altered in these mice. We found no significant changes in the levels of -CTF or -CTF in the hippocampus or cortex of wild-type versus FeC25 mice. We could not reliably measure the brain A levels, as determination of endogenous mouse A is technically challenging. To circumvent this problem, we crossed FeC25 with R1.40 transgenic mice, which produce higher levels of human A by 1 month of age . We measured the levels of total A by ELISA in 34-month-old mice and observed no significant differences between R1.40 and R1.40 × FeC25 mice . Finally, to determine if AICD could accelerate plaque formation, we crossed FeC25 mice to APPPS1 transgenic mice which co-express APPswe and L166P mutant PS1 proteins . These mice overproduce A 142 and exhibit A deposition as early as 68 weeks of age. We examined A-plaque load in 34-month-old APPPS1 and APPPS1 × FeC25 mice and found no significant changes in plaque number or plaque size. These data demonstrate that at the time we start to detect tau abnormalities in FeC25 mice , increased levels of AICD do not cause gross alterations in APP processing or increased A levels in vivo.
The Term Paper On Alzheimer’s Disease 2
1. What is Alzheimers Disease ? Alzheimers Disease is an organic brain disorder characterized by a progressive loss of mental skills and deterioration of the personality. 2. Who described Alzheimers disease? Dr. Alois Alzheimer, a German Physician described A.D. in 1906. 3. In what age Alzheimers disease strikes people? It most commonly strikes people who are over 65 about 10% of this age …
Sparing of occipital regions, parietal regions and the posterior two-thirds of the superior temporal gyrus is common .
MRI studies of AD show global cerebral atrophy, predominantly affecting the temporal and parietal lobes early in disease progression. Atrophy of gyri and widening of sulci of the cerebral hemispheres is also evident. Atrophy is most apparent in the medial temporal lobe, particularly localised to the parahippocampal gyrus. The occipital lobe and motor cortex are generally spared.
Imaging techniques clearly show that in both disorders the cortex becomes shrunken or atrophied and is reduced in volume. However, in contrast to AD in which the atrophy is relatively diffuse and mild, the changes seen in PiD are usually more circumscribed and are often asymmetrical. In contrast to this, circumscribed cortical trophy is a rare finding in AD and changes are usually bilateral and symmetrical.
Sergeant N Et Al Journal Neurochem 6: 834
Hong M, Zhukareva V, Volksberg-Ragaglia V, et al Mutation specific functional impairments in distinct tau isoforms of hereditary FTDP-17. Science 82:1814-1917.
Folstein MF, Folstein SE & McHugh PR Mini-mental state: a practical method of grading the cognitive state of patients for the clinician. Journal of Psychiatric Research 12:189-198.
Van Mansvelt J Picks Disease: a Syndrome of Lobar Cerebral Atrophy, Its Clinico-Anatomical and Histopathological Types. Enschede:Loeff
Knopman DS, Christensen KJ & Scut LJ The spectrum of imaging and neuropsychological findings in Picks disease. Neurology 39:362-368.
Corsellis JAN Picks disease. In Blackwood W & Corseillis JAN Greenfileds Neuropathology, 3rd edn, pp987-992. London: Edward Arnold.
Esiri MM The neuropathology of Alzheimers disease. In Dawbarn D, Shelley JA Neurobiology of Alzheimers disease, 2nd eds, pp33-53. Oxford University Press.
Wechsler AF, Verity A, Rosenschein S, Fried I, & Schiebel AB Picks Disease: A clinical, computed tomorgraphic and histologic study with golgi impregnation observations. Arch Neurol 39:287-290.
Heston LL, White JA, Mastri AR Picks Disease: Clinical genetics and natural history. Arch Gen Psychiatry 44:409-411.
Tolnay M, Probst A Review: tau protein pathology in Alzheimers disease and related disorder. Neuropathology and Applies Neurobiology 25:171-187.
Hirano LL, Zimmerman HM Alzheimers neurofibrially changes A topographic study. Arch Neurol 7:227-242.
You May Like: Alzheimers Ribbon Color
Drugs To Treat Alzheimer Disease
Cholinesterase inhibitors modestly improve cognitive function and memory in some patients. Four are available. Generally, donepezil, rivastigmine, and galantamine are equally effective, but tacrine is rarely used because of its hepatotoxicity.
Donepezil is a first-line drug because it has once-a-day dosing and is well-tolerated. The recommended dose is 5 mg orally once a day for 4 to 6 weeks, then increased to 10 mg once a day. Donepezil 23 mg once a day may be more effective than the traditional 10 mg once-a-day dose for moderate to severe Alzheimer disease. Treatment should be continued if functional improvement is apparent after several months, but otherwise it should be stopped. The most common adverse effects are gastrointestinal . Rarely, dizziness and cardiac arrhythmias occur. Adverse effects can be minimized by increasing the dose gradually .
Memantine, an N-methyl-d-aspartate receptor antagonist, appears to improve cognition and functional capacity of patients with moderate to severe Alzheimer disease. The dose is 5 mg orally once a day, which is increased to 10 mg orally twice a day over about 4 weeks. For patients with renal insufficiency, the dose should be reduced or the drug should be avoided. Memantine can be used with a cholinesterase inhibitor.
Neuropathological Alterations In Alzheimer Disease
You May Like: Does Prevagen Help Dementia
Neuropathology Of Mild Cognitive Impairment And Early Alzheimer Disease
Clinicopathological correlation studies have taught us that at the moment of the clinical diagnosis, patients with AD-type dementia often already have a Braak stage V or VI of neurofibrillary degeneration and a substantial and widespread synaptic and neuronal loss. To anticipate the clinical diagnosis of AD before the stage of full-blown dementia, a new clinical construct was needed. Petersen et al. proposed the concept of mild cognitive impairment as a new diagnostic entity for the transition between normal aging and AD dementia. Patients with MCI have already some cognitive complaints that are detectable with the appropriate cognitive tests and represent a decline from a previous higher baseline level but that, unlike the definition of dementia, do not interfere with their activities of daily life. Importantly, MCI patients have an increased risk of developing dementia, which has been reported between 10% and 15% per year .
On The Relation Between Aphasia And Dementia
Aphasia in the broadest sense of the word represents an acquired disorder of language comprehension, production, and/or symbolic knowledge . Given this broad definition, one might suspect that aphasia is evident across virtually all of the dementias, and indeed an inspection of formal diagnostic criteria across many of the dementias confirms this suspicion . Despite the ubiquity of aphasia in dementia, however, its qualitative nature and severity vary substantially as functions of disease process and localization. Such heterogeneity has led to a longstanding theoretical debate reflected in the dichotomy between disorders of degraded storage vs. impaired linguistic access in dementia and stroke aphasia .
Recommended Reading: Did Ronald Reagan Have Alzheimer
Distribution Of Amyloid Plaques
In AD, senile plaque and neurofibrillary tangle formation tend to form neuroanatomically in stereotypic patterns, which has led to several staging schemes . One of the first attempts to stage amyloid plaques in AD was proposed by Heiko and Eva Braak. A three stage scheme was proposed, with the basal frontal and temporal lobes affected in Stage A, extension into the association neocortices and hippocampus in Stage B, and finally reaching primary cortices, subcortical nuclei and cerebellum in Stage C . Within the cortical layers, layers III and Va are most affected, layers IV and Vb were affected less, and other layers were relatively spared . More recently, the Braak plaque staging has been modified by his research associate, Dietmar Thal, and this scheme of amyloid phases using highly sensitive silver staining or A antibodies has been adopted by NIA-AA and BrainNet Europe . In Thal Phase 1 the neocortex is involved, expanding to the allocortex in Phase 2, subcortical nuclei, including the striatum, in Phase 3, with involvement of brainstem in Phase 4 and cerebellum in Phase 5 . For practical work, phases 14 can be determined by amyloid deposition in the medial temporal lobe . It is not unusual for neurologically normal patients to have Thal 13 amyloid phase as shown in Table .
Alzheimer Neuropathology In Normal Aging
Longitudinal prospective clinicopathological studies in nondemented elderly people have revealed that up to 45% of nondemented elderly would meet the NIA-RI criteria for AD had they been demented, usually the intermediate likelihood category of these criteria, and rarely the high likelihood category . Moreover, the pattern of regional distribution of pathological changes in nondemented controls matches that of AD patients . Thus, mounting evidence from clinicopathological studies support the view that AD is a continuous spectrum between asymptomatic lesions in cognitively normal elderly and dementia, with MCI as a transition phase between these two ends.
Read Also: Neurotransmitter Related To Alzheimer’s
The Essay On Diseased Body In Wuthering Heights
In Wuthering Heights by Emily Bronte it can be viewed that there is more suffering caused by a diseased mind than by a diseased body. The idea of a diseased mind is a mental illness or madness and the diseased body is a physical illness or injury, both of which are displayed by many characters in Wuthering Heights. Heathcliff is a prime example of a character with a diseased mind that …
It is also apparent that atrophy of limbic structures is evident in both diseases, but is often more pronounced in early stages of Alzheimers disease, where it correlates well with early cognitive deficits. The involvement of the hippocampus in AD is so pronounced that it has been suggested that the disease should be defined as a hippocampal dementia .
However, it is hard to compare the two disorders with regards to hippocampal involvement as there appears to be a lack of consensus concerning the extent of hippocampal involvement in Picks disease. The changes seen in the hippocampus have been described as slight- to moderate to severe .
Nevertheless, both dementias have in common a certain degree of degeneration of the hippocampus and amgydala, although the involvement of the hippocampus is less consistent and intense in PD compared to AD.
Age Related Tau Pathologies
Primary age-related tauopathy and aging-related tau astrogliopathy are independent tau pathologies commonly observed in patients over 80years of age, and PART may account for a proportion of the misdiagnosed clinical AD cases in the elderly . Neurofibrillary pathology in PART is similar to AD, being composed of 3R and 4R isoforms. Lesions are found in the hippocampus and adjacent regions similar to those observed in Braak I-IV, but PART is distinct from AD in that it lacks amyloid plaques, and it has distinct morbidity and age range . The frequency of PART increases in the 80s and 90s when AD prevalence is level or declining . NFTs in PART may pass through similar phases as those observed in AD, with progression from pretangles to NFTs and eventually extracellular ghost tangles. The latter, when frequent, are associated with memory complaints observed in the elderly . Differentiating PART from AD remains a challenge . ARTAG represents astrocytic tau pathology distinct from that observed in primary tauopathies including PSP, CBD and GGT. It is associated with 4R tau deposits in subpial or perivascular thorn-shaped astrocytes or granular fuzzy astrocytes in gray matter . It is recommended that location, region and severity of ARTAG be noted, but its relationship to neurological symptoms is not well characterized .
Read Also: Did Reagan Have Alzheimers
Imaging Cerebral Amyloid Angiopathy
CAA is characterized by the deposition of A – in small and medium-sized arteries, capillaries, and less frequently in the veins of the cerebral cortex.50 For imaging, a 10 magnification objective was utilized. Figure 7 shows a schematic drawing of a vessel wall. A – mostly accumulates in the tunica media and tunica externa .51 Approximately, one-quarter of brains diagnosed with AD are also diagnosed with CAA.50 In histologic sections of the investigated CAA brains, A accumulations were found, see Figs. 7 and 7.
Criteria For The Pathological Diagnosis Of Alzheimer Disease
Of all pathological features described above, amyloid plaques and NFTs are the most characteristic of AD and, understandably, the criteria for the pathological diagnosis of AD rely on their amount and/or distribution.
Current pathological criteria for AD were defined in 1997 by a workshop of the National Institute of Aging and the Reagan Institute. The NIA-RI consensus recommendations combine the CERAD semiquantitative score of neuritic plaques and the Braak and Braak staging of NFTs to distinguish three probabilistic diagnostic categories: high likelihood, if there are frequent neuritic plaques and abundant isocortical NFTs intermediate likelihood, if there are moderate neuritic plaques and NFTs are restricted to limbic regions , and low likelihood, if there are infrequent neuritic plaques and NFTs are restricted to the entorhinal cortex and/or hippocampus . A diagnosis of AD is made when the criteria for intermediate or high likelihood of AD are met and the patient had a clinical history of dementia . Because experience has revealed infrequent cases with many AD pathological lesions but no or few cognitive symptoms and these circumstances were not addressed by the NIA-RI consensus workgroup, these diagnostic criteria are currently under review.
You May Like: Color For Alzheimer’s Ribbon
The Neuropathological Diagnosis Of Alzheimers Disease
2.1. Neuropathological Entities Mimicking Aspects of Alzheimers Disease
2.1.1. Primary Age-Related Tauopathy
Practical Considerations
2.1.2. Aging-Related Tau Astrogliopathy
Practical Considerations
2.1.3. Argyrophilic Grain Disease
Practical Considerations
2.1.4. Chronic Traumatic Encephalopathy
Practical Considerations
2.1.5. Other Tauopathies-Picks Disease , Progressive Supranuclear Palsy , Corticobasal Degeneration , Globular Glial Tauopathy , Microtubular-Associated Protein tau Mutations
The Term Paper On Cell Components Part 1
Cell Components Let’s imagine clouds of cold fog billow up through a circular hatch in the top of a stainless steel tank as a biologist pulls out the lid and its one-foot thickness of styrofoam insulation. As the fog rolls down to the floor, Hay peers into the dark tank, where the temperature is all the time 321 degrees below zero Fahrenheit. It is kept so cold because that is a temperature at …
Don’t Miss: What Color Is For Alzheimer’s
Pathology Of Alzheimers Disease
Macroscopic features
Fig. 1
Gross Anatomy of Alzheimers Brain. Lateral view of an Alzheimers brain can show widening of sulcal spaces and narrowing of gyri compared to a normal brain. This may be more readily observed in coronal sections as indicated by the arrowheads, and this atrophy is often accompanied by enlargement of the frontal and temporal horns of the lateral ventricles as highlighted by the arrows. Additionally, loss of pigmented neurons in the locus coeruleus is commonly observed in the pontine tegmentum as shown with the open circle. None of these features is exclusive to Alzheimers disease
Microscopic features
The definitive diagnosis of AD requires microscopic examination of multiple brain regions employing staining methods that can detect Alzheimer type neuropathologic change , with diagnosis based upon the morphology and density of lesions and their topographic distribution. Several of the brain regions that are vulnerable to Alzheimer type pathologic change are also vulnerable to other disease processes, such as -synucleinopathy and TDP-43 proteinopathy. Mixed pathology is common. Indeed in the Mayo Clinic Brain Bank from 2007 to 2016 , the majority of AD cases had coexisting non-Alzheimer pathologies, and comorbidities increased in frequency with age. Furthermore, when the original clinical diagnoses were examined for cases with pure AD pathology, it is clear that a number of clinical syndromes can masquerade as Alzheimers disease.
Melatonin: Prevention And Treatment
Experimental models of AD pathology show that melatonin may decrease oxidative injury and apoptosis, inhibit A deposition and fiber formation, prevent loss of cholinergic signaling, and improve cognitive function . Yet the effects of melatonin supplementation on the reduction of A have been mixed . In humans, it has been shown that melatonin administration improves sleep disturbance in old age and AD patients and improves cognitive function in older adults with no dementia Peck et al. .
Findings on the effects of melatonin in patient populations have been mixed . Some evidence shows that melatonin administration may improve cognitive function and depressive symptoms in older adults with MCI or dementia . Hormone treatment has also been found to diminish afternoon agitation, or sundowning, in AD patients and improve cognitive function . In a study by Brusco et al. , AD patients treated with melatonin over 2235 months did not show progression of cognitive and behavioral deterioration associated with the disease during the time of treatment. Benefits for cognitive performance may be stronger for individuals with MCI . Yet, a recent meta-analysis of RCTs showed beneficial effects for sleep disturbances and for prolonging total sleep time, but not for cognitive function . Caution must be taken when considering melatonin treatment as RCTs are required to evaluate long-term safety, optimal dosing, and administration term .
P. Pressman, G.D. Rabinovici, in, 2014
Recommended Reading: Alzheimer’s Neurotransmitters Affected
The Essay On Alzheimers Disease Drug Protein Alzheimer
Introduction WeAlzheimer’s Disease Alzheimer’s Disease Introduction We did our project on Alzheimer’s Disease. This is a degenerative brain disorder that is found in older adults. This disease is characterized by the destruction of nerve cells and neural connections in the cerebral cortex of the brain and by a large loss of brain mass. When an autopsy is performed on an Alzheimer’s patient, it is …
They are differentiated from other neruons by swollen cytoplasm and laterally displaced nucleus in the cell. They are most abundant in areas of severe cortical atrophy, like the frontal cortex
Pick bodies are spherical cytoplasmic inclusions that are well demarcated, amorphous and slightly basophilic on hematoxylin-eosin stain. They are argentophillic with Bielschowsky and Bodian silver stains but fail to react with Gallyas stain. They are primarily made up of abnormal aggregates of tau, a neuron specific protein usually associated with stabilization of microtubules. Studies of topographic distribution of Picks Bodies in cortex show that they are found in large numbers in the dentate fascia and pyramidal cell layer of the hippocampus, entorhinal cortex and frontal and temporal neocortices and are not uniformly or randomly distributed, but instead they are found in clusters.
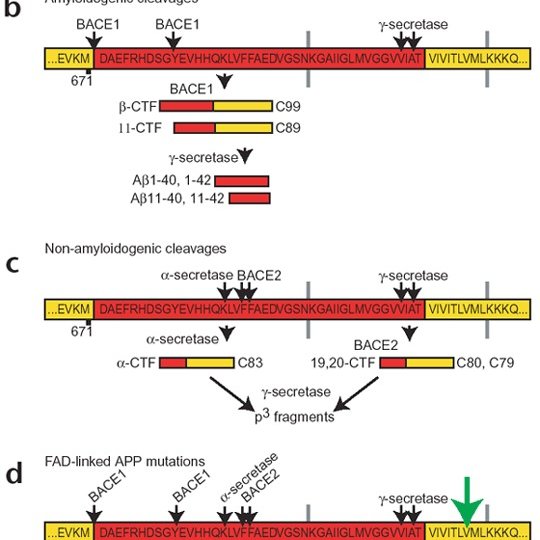
This abnormal processing of APP produces peptides with 40 and 42 amino acids, instead of 40 amino acids, that rapidly aggregate to form fibrils with -sheet structure.
References