Social Cognition Dysfunctions In Neurodegenerative Diseases: Neuroanatomical Correlates And Clinical Implications
Francesca Trojsi
1First Department of Neurology, Aeginition Hospital, Medical School, National and Kapodistrian University of Athens, Athens, Greece
2INSERM U 1127, CNRS UMR 7225, Sorbonne Universités, and Université Pierre et Marie Curie-Paris 6, UMRS 1127, Institut du Cerveau et de la Moelle Épinière , 75013 Paris, France
3Pontificia Universidad Javeriana Bogotá, Colombia, Centro de Memoria y Cognición Intellectus Hospital Universitario San Ignacio, Bogotá, Colombia
4Department of Psychology, University of Campania Luigi Vanvitelli, Caserta, Italy
5Department of Medical, Surgical, Neurological, Metabolic, and Aging Sciences, University of Campania Luigi Vanvitelli, Naples, Italy
Abstract
1. Introduction
This review aims to summarize some of the basic components of social cognition, also referring recent hypotheses derived from network-based approaches, and to discuss clinical manifestations of social cognitive dysfunctions in most NDs, addressing the pertinent literature published in the last 10 years.
1.1. Social Cognition, Social Behavior, and Social Functioning
1.2. Network-Based Approach to Social Cognition
1.3. Clinical Assessment of Social Cognition
2. Social Cognition Abnormalities in Neurodegenerative Disorders
2.1. Amyotrophic Lateral Sclerosis-Frontotemporal Disease Spectrum Disorders
2.1.1. Frontotemporal Lobar Degeneration
2.1.2. Amyotrophic Lateral Sclerosis and Its Disease Spectrum
2.2. Parkinsons Disease and Parkinsonisms
2.3. Alzheimers Disease
Criteria For The Pathological Diagnosis Of Alzheimer Disease
Of all pathological features described above, amyloid plaques and NFTs are the most characteristic of AD and, understandably, the criteria for the pathological diagnosis of AD rely on their amount and/or distribution.
Current pathological criteria for AD were defined in 1997 by a workshop of the National Institute of Aging and the Reagan Institute. The NIA-RI consensus recommendations combine the CERAD semiquantitative score of neuritic plaques and the Braak and Braak staging of NFTs to distinguish three probabilistic diagnostic categories: high likelihood, if there are frequent neuritic plaques and abundant isocortical NFTs intermediate likelihood, if there are moderate neuritic plaques and NFTs are restricted to limbic regions , and low likelihood, if there are infrequent neuritic plaques and NFTs are restricted to the entorhinal cortex and/or hippocampus . A diagnosis of AD is made when the criteria for intermediate or high likelihood of AD are met and the patient had a clinical history of dementia . Because experience has revealed infrequent cases with many AD pathological lesions but no or few cognitive symptoms and these circumstances were not addressed by the NIA-RI consensus workgroup, these diagnostic criteria are currently under review.
The Role Of Amyloid Plaques
Amyloid plaques are mostly made up of a protein called B-amyloid protein which is itself part of a much larger protein called APP . These are amino acids.
We do not know what APP does. But we do know that APP is made in the cell, transported to the cell membrane and later broken down. Two major pathways are involved in breakdown of APP . One pathway is normal and causes no problem. The second results in the changes seen in Alzheimer’s and in some of the other dementias.
Read Also: Dementia Ribbon Colour
Estimation Of Roi Volumentric Interval Change
For a subject to be included in our statistical analyses, several criteria needed to be satisfied: the baseline cortical parcellation and subcortical segmentation had to pass review, as described above for a tight comparison between cognitive and volumetric measures, a subject’s follow-up was eliminated unless both volumetric and cognitive data, including a clinical diagnosis, existed for that follow-up there was at least one good follow-up, along with the good baseline a healthy control needed to remain such at all follow-ups and finally, the volume-change field had to pass review. Quality control on the volume-change field reduced the number of healthy controls by 8.6% to 169, the number of MCI subjects by 8.5% to 299, and the number of AD subjects by 12.2% to 129.
Regions With Significant Grey Matter Differences Between Subjects With Mci And Healthy Controls
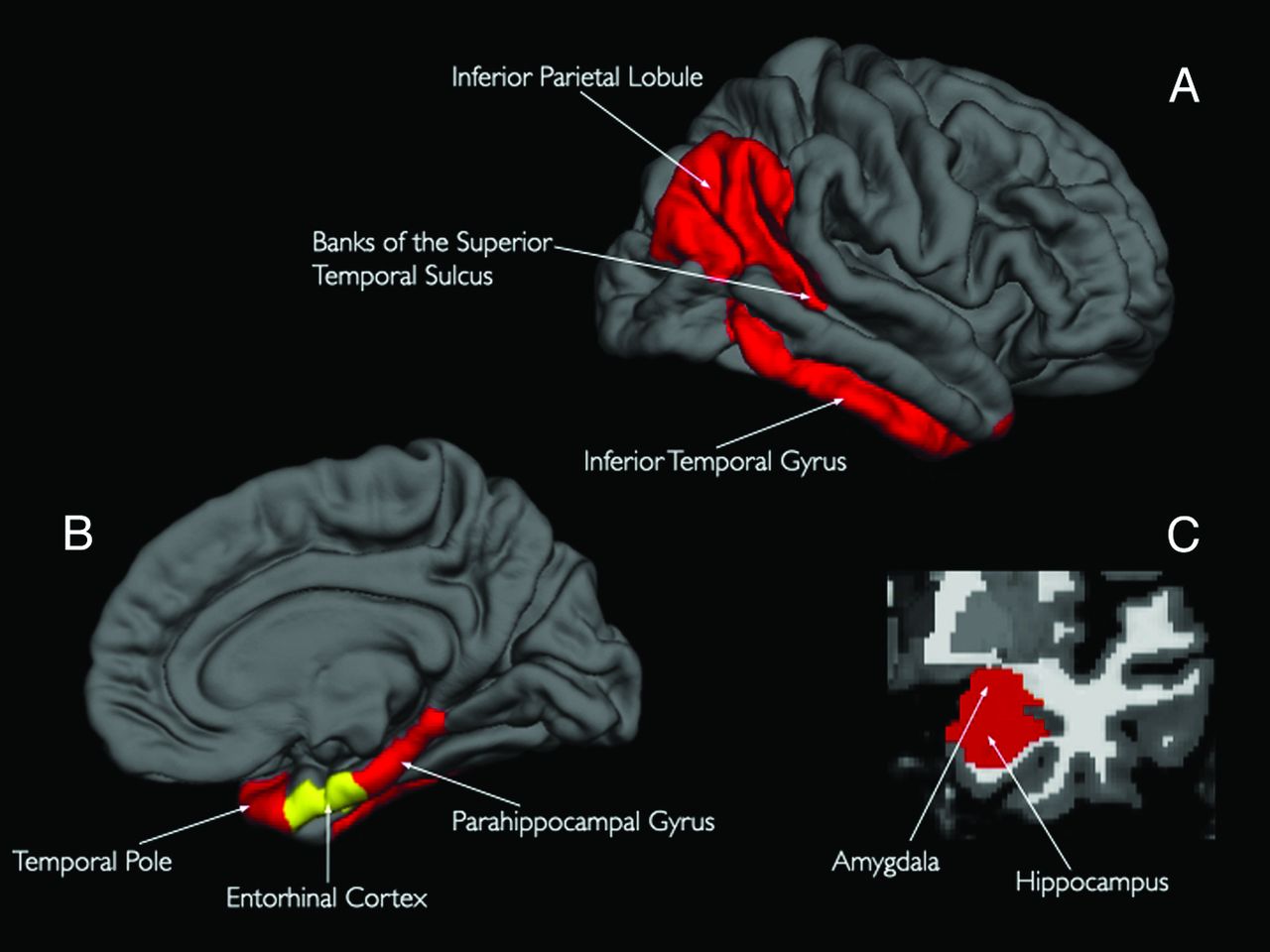
Across studies, we found in total three clusters of consistent grey matter reduction in MCI patients . The two largest clusters were situated in the medial temporal lobes. Analysis by cytoarchitectural probability showed that the largest cluster was mainly situated in the laterobasal part of the left amygdala, the left thalamus, the left medial temporal pole and the cornu ammonis region of the left hippocampus. The second largest cluster in the contralateral temporal lobe was primarily located in the right laterobasal amygdala and extended to the fascia dentate region of the right hippocampus. The third largest cluster was to be found in the parietal precuneus broadening to the posterior cingulate cortex bilaterally, accentuated on the right side.
Convergent areas of grey matter loss in MCI patients compared to healthy controls. Grey matter changes were found bilaterally in the amygdala/hippocampus region extending to the thalamus and medial temporal pole on the left side and to the parahippocampal gyrus on the right side. The third cluster was found accentuated on the right side in the parietal precuneus broadening to the posterior cingulate cortex
Recommended Reading: How To Get A Person With Dementia To Shower
What Is The Neuroanatomy Of Alzheimer Disease
Healthy neurons have an internal support structure partly made up of structures called microtubules. These microtubules act like tracks, guiding nutrients and molecules from the body of the cell down to the ends of the axon and back. A special kind of protein, tau, binds to the microtubules and stabilizes them.
In AD, tau is changed chemically. It begins to pair with other threads of tau, which become tangled together. When this happens, the microtubules disintegrate, collapsing the neurons transport system . The formation of these neurofibrillary tangles may result first in malfunctions in communication between neurons and later in the death of the cells.
The Mechanisms Which May Link Lc Degeneration To Ad
In early studies LC neurons were quantified without stereology. This explains a great variability in LC cell counts even within control subjects.
Modern stereology confirms LC neuronal loss . P-Tau positive LC neurons are associated with a dramatic reduction of synaptophysin-positive perineural dots, which leads to a loss of synaptic connectivity, a sort of anatomical de-afferentiation of these neurons from activating inputs . These authors found over-expression of 2-adrenergic receptors at stage I, while these receptors were reduced at stage IV in the hippocampus .
Altogether these pieces of information suggest that P-Tau accumulates within LC very early, producing subtle, yet potentially relevant, functional alterations affecting NE release in target areas.
At advanced stages, the loss of NE neurons enhances the accumulation of A in cortical regions: this in line with experimental evidence. In fact, the neurotoxin DSP-4 enhances A plaque accumulation in the brain . Thus, the loss of NE appears to directly foster A plaque accumulation and LC degeneration alters microglial activity, which may indirectly induce amyloid mismetabolism . These changes correlate with cognitive impairment .
Again, a damage to LC produces a lack of neuroprotection. In fact 2-receptor stimulation is key in activating autophagy which removes P-Tau from the trans-Golgi network.
Don’t Miss: Color For Dementia Awareness
Data Acquisition And Preparation
Raw Digital Imaging and Communications in Medicine MRI scans, including two three-dimensional T1-weighted volumes per subject per visit, were downloaded from the public ADNI site . These data were collected across a variety of scanners with protocols individualized for each scanner, as defined at www.loni.ucla.edu/ADNI/Research/Cores/index.shtml. In our laboratory, MRI data were reviewed for quality and automatically corrected for spatial distortion caused by gradient nonlinearity . For each subject at each visit, the two three-dimensional T1-weighted images were rigid-body aligned to each other, averaged to improve signal-to-noise ratio, and resampled to isotropic 1-mm voxels. Baseline volumetric segmentation and cortical surface reconstruction and pacrellation were performed using a data analysis pipeline based on the FreeSurfer software package and customized Matlab code, optimized for use on large multisite data sets. The automated whole-brain segmentation procedure uses a probabilistic atlas and applies a Bayesian classification rule to assign a neuroanatomic label to each voxel. The atlas consists of a manually derived training set created by the Center for Morphometric Analysis from 40 non-ADNI subjects across the adult age range, including individuals with AD. Automated volumetric segmentation required only qualitative review to ensure that there was no technical failure of the application.
The Neuroanatomy Of Lc In Ad
LC is a tube-like shaped group of NE neurons placed in the upper part of the pons it is composed of medium-sized neurons . LC extends rostrocaudally for approximately 16 mm . These neurons send their branched axons to innervate the entire cerebral cortex . Thus, by releasing NE through bouton en passage , LC modulates the activity of several cortical areas. In fact, LC modulates sleep/wake cycle, learning and memory, early gene expression and neuroprotection . LC mostly innervates limbic cortex compared with neocortex . The ventral part of caudal LC sends projections even to lower medulla and spinal cord, and regulates autonomic functions , while neurons which innervate the allocortex are placed in the rostral part of the nucleus .
Also Check: Bobby Knight Health
Demographics And Screening Measures
Table summarizes demographic and screening measures. Within each age group there were no significant differences in mean participant age between ApoE+ and ApoE- participants . Dementia Rating Scale scores did not differ significantly between ApoE groups or age groups and all participants DRS scores were in the range of normal cognitive functioning. Analysis of odor threshold test performance revealed that all participants scored in the normal range of olfactory functioning. While all participants were normosmic, the older participant group exhibited poorer olfactory threshold scores than the middle and young age groups =8.93, p < .001, 2=.24), with no interaction of ApoE status.
Pathology Of Alzheimers Disease
Macroscopic features
Fig. 1
Gross Anatomy of Alzheimers Brain. Lateral view of an Alzheimers brain can show widening of sulcal spaces and narrowing of gyri compared to a normal brain. This may be more readily observed in coronal sections as indicated by the arrowheads, and this atrophy is often accompanied by enlargement of the frontal and temporal horns of the lateral ventricles as highlighted by the arrows. Additionally, loss of pigmented neurons in the locus coeruleus is commonly observed in the pontine tegmentum as shown with the open circle. None of these features is exclusive to Alzheimers disease
Microscopic features
The definitive diagnosis of AD requires microscopic examination of multiple brain regions employing staining methods that can detect Alzheimer type neuropathologic change , with diagnosis based upon the morphology and density of lesions and their topographic distribution. Several of the brain regions that are vulnerable to Alzheimer type pathologic change are also vulnerable to other disease processes, such as -synucleinopathy and TDP-43 proteinopathy. Mixed pathology is common. Indeed in the Mayo Clinic Brain Bank from 2007 to 2016 , the majority of AD cases had coexisting non-Alzheimer pathologies, and comorbidities increased in frequency with age. Furthermore, when the original clinical diagnoses were examined for cases with pure AD pathology, it is clear that a number of clinical syndromes can masquerade as Alzheimers disease.
Read Also: Bob Knight Health Condition
Alzheimers Disease Pattern Similarity Score
The Alzheimers disease pattern similarity score was derived using a high-dimensional supervised machine learning algorithm based on the elastic net regularized logistic regression to analyse structural brain MRI data pattern at voxel level , comparing Alzheimers disease cases and cognitively normal individuals . The EN-RLR is known to produce sparse models , which translates in the context of our neuroimaging application into a variable selection mechanism able to identify voxels or brain areas relevant for classification that we call discriminative maps. The score formally is the class-conditional probability of membership to the Alzheimers disease group as modelled by the EN-RLR model when discriminating cognitively normal from Alzheimers disease participants in ADNI , interpreted as a measure of similarity of the brain spatial patterns found in one individuals MRI to those found in individuals diagnosed with Alzheimers disease.
Relationship Between Neuroanatomic Abnormalities And Behavioral Cognitive Impairment In Individuals At Risk For Asd
HealthDay News Neuroanatomic abnormalities are seen in cohorts at high risk for autism spectrum disorder , according to a study published in Radiology.
The researchers found that, compared with familial noncarriers and population control participants, the most prominent features for deletion carriers were dysmorphic and thicker corpora callosa and a greater likelihood of cerebellar tonsillar ectopia and Chiari I malformations. The most salient findings for duplication carriers compared with familial noncarriers and population controls were reciprocally thinner corpora callosa, decreased white matter volume, and increased ventricular volume. For deletion carriers, the presence of any imaging feature indicated worse daily living, communication, and social skills compared to those without any radiologic abnormalities. The presence of decreased white matter, callosal volume, and/or increased ventricle size was correlated with reduced full-scale and verbal IQ scores among duplication carriers.
Don’t Miss: Dementia Ribbon
Associations Between Pm25 Exposure And Change In Cvlt
Multilevel SEMs revealed significant linear declines in episodic memory before MRI-1 across all CVLT measures . Linear declines in CVLT performance were generally larger after the MRI-1 across all measures except for long-delay free recall. The observed between-individual variability was statistically significant for the level of CVLT performance at the MRI-1 and linear changes in individual-specific estimates of all CVLT trajectories before MRI-1. Between-individual variability in change was generally larger after the MRI-1 but not statistically significant.
Across all CVLT measures, PM2.5 exposure was not associated with the estimated level of performance at MRI-1 . There was evidence for adverse PM2.5 effects with greater declines in both CVLT measures of immediate recall and new learning , but no statistically significant associations were found with delayed-recalls or composite measure . Across each interquartile increment of PM2.5 , the average rate of annual decline in immediate recall/new learning was significantly accelerated by 0.040 SDs for Trials 1-3 and 0.057 SDs for List B. As compared with the effect of age at MRI-1 in the same model on post MRI-1 change in CVLT Trials 13, the magnitude of the adverse exposure effect was equivalent to 4 years of accelerated decline in immediate recall/new learning performance. Overall, the multicovariate-adjusted average rate of change was significantly accelerated by 19.3% for Trials 13 and 14.8% for List B.
The Effects Of Alzheimer’s On The Brain
Heather Mercer is native to Northwest Ohio and graduated from Loma Linda University with two doctorate degrees . She is currently a professor at Owens Community College, as well as a fact-checker for Verywell Health. She has gained experience in a variety of settings, ranging from corporate wellness and preventive medicine, to mental health, chronic disease, and end-of-life care.
Alzheimer’s disease is a degenerative disease of the brain. Understanding how the anatomy of the Alzheimer’s brain differs from a normal brain gives us insight. It can help us cope better with the changes that happen to our loved ones as a result of this debilitating disease.
In Alzheimer’s disease, the appearance of the Alzheimer’s affected brain is very different to a normal brain. The cerebral cortex atrophies. That means that this area of the brain shrinks and this shrinkage is dramatically different from the cerebral cortex of a normal brain. The cerebral cortex is the outer surface of the brain. It is responsible for all intellectual functioning. There are two major changes that can be observed in the brain using magnetic resonance imaging :
- The amount of brain substance in the folds of the brain is decreased
- The spaces in the folds of the brain are grossly enlarged.
Read Also: Alzheimer’s Disease Ribbon Color
Study Design And Population
We conducted a prospective cohort study that included community-dwelling females who were initially enrolled in the Womens Health Initiative Memory Study and subsequently participated in both the WHI Study of Cognitive Aging and the WHI Memory Study of Magnetic Resonance Imaging ancillary studies . WHIMS participants were postmenopausal females aged 65 years and older who were recruited from 1996 through 1999 across 48 states and free of dementia as determined by standardized study protocols, described elsewhere . A subsample of cognitively-intact WHIMS participants were followed in WHISCA with annual neurocognitive testing during the period of 19992010. Between April 2005 and January 2006, WHIMS participants across 14 active WHIMS sites were enrolled in the WHIMS-MRI study, yielding 1365 scans that met quality control standards. A total of 1050 females participated in both WHISCA and WHIMS-MRI. For the present study, we excluded subjects with missing data on relevant covariates, resulting in a final analytic sample of 998 females . A total of 531 females underwent a second MRI between 2009 and 2010.
Flowchart for selection of final analytical sample..
Verbal Memory Test Best Indicator Of Who Will Have Alzheimer’s Disease New Study Says
Early detection of Alzheimer’s could lessen the impact
Verbal memory test best indicator of who will have Alzheimer’s disease, new study says
CHICAGO Incidence of Alzheimer’s Disease is expected to increase as the population of elderly grows. Early diagnosis and treatment will be the key to lessening the disease’s worst effects, but, how to spot the disease before its symptoms become serious is a challenge for health professionals. A new study by psychologists Konstantine K. Zakzanis, Ph.D., and Mark Boulos, B.Sc., of the University of Toronto has determined that the best predictor of future Alzheimer’s type dementia is a verbal memory test. Their study will be presented in Chicago at the 110th Annual Convention of the American Psychological Association .
In a meta-analysis of 31 studies amounting to 1,144 Alzheimer’s patients and 6,046 healthy controls, Zakzanis and Boulos looked at both neuropsychological and neuroimaging tests to determine their ability to detect preclinical dementia and/or Alzheimer’s disease. They also paired a genetic susceptibility to dementia/Alzheimer’s with results on both neuropsychological and neuroanatomic tests again attempting to identify which types of tests would prove most accurate in identifying preclinical disease in patients with the ApoE gene.
Full text paper available from the APA Public Affairs Office
Second author will be available for interviews. He can be reached before and after the convention at 299-5653 or by .
You May Like: What Color Is The Alzheimer’s Ribbon