Latinos And Alzheimers Disease
The U.S. Census Bureau projects that the Latino population will double from approximately 49 million in 2009 to 106 million people by the year 2050. In fact, by 2044, more than half of all Americans are projected to belong to a minority group. The growth of the Latino community will have tremendous implications for our nations health, education, and workforce sectors. It is essential that our nations policymakers and community leaders better understand these consequences to adequately address the public health needs of an increasingly multicultural society.
Shifting Demographics
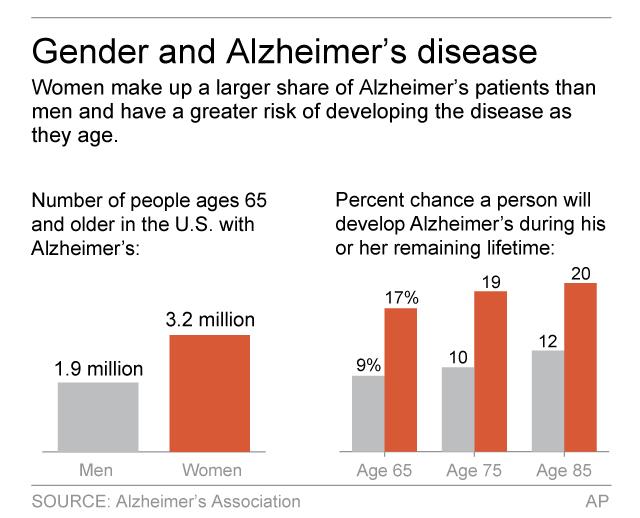
According to the Administration on Aging, between 2008 and 2030 the Latino population aged 65 years and older will increase by 224% compared to a 65% increase for the non-Latino white population in the same age category. There are approximately four million Latinos over the age of 65 living in the United States today, twice as many as in 2000. The flip side of this increased longevity includes an increased risk for Alzheimers. The chances of developing the disease double approximately every five years after age 65, and after age 85 the risk reaches nearly 50%.
Latino families are highly under-resourced in terms of income, retirement benefits, and pension benefits. As the Latino population ages, a growing number of Latino communities, families, and systems of care will be confronted by increasing rates of Alzheimers with the fewest resources to manage it.
Risk Factors
Evidence Of Racial And Ethnic Disparities
Prevalence, Incidence, and Diagnosis
Incidence estimates also suggest higher risk of Alzheimer’s disease among non-White populations. In a 7-year study in the Washington Heights and Inwood communities of New York City, overall adjusted incidence rates for probable and possible Alzheimer’s disease among Whites were 0.4% per person-year for ages 65-74, 2.6% for ages 75-84, and 4.2% for ages 85+ . Incidence was higher among African Americans and Caribbean Hispanics in the same community. One recent study found that the unadjusted hazard ratio for developing dementia over 12 years was 1.44 for Black participants compared to White, but after adjusting for demographics, apolipoprotein E4, comorbidities, lifestyle factors, and socioeconomic status, the Black-White difference was reduced to 1.09 and was no longer significant .
Health OutcomesParticipation in Clinical TrialsUse of Long-Term Services and SupportsHealth Care Expenditures
TABLE 1. Use of and Medicare Payments for Health Care Services among Medicare Beneficiaries with a Dementia Diagnosis, by Race/Ethnicity, 2006
| 8.8% |
: Adapted from Alzheimer’s Association, 2011.
Caregiving
Why Do These Differences Exist
While genetic factors can increase the risk of Alzheimer’s, multiple studies have looked at race and genetics and have not found a clear correlation between these factors and dementia risk. Researchers have, however, found a connection between certain health conditions, race, and risk of cognitive impairment.
Also Check: Alzheimer’s Disease Neurotransmitters
Health Disparities Race And Alzheimers
Addressing inequities in brain health is vital for families, communities and the nation. By 2030, nearly 40 percent of all Americans living with Alzheimers will be Black or Latino. Black Americans are twice as likely as non-Hispanic Whites to develop Alzheimers Latinos are 1.5 times as likely. It’s time to make brain health equity a priority.
What Is The Difference Between Alzheimer’s And Dementia
First, some explanation of dementia vs. Alzheimer’s. According to the Alzheimer’s Association, dementia is a general term for a decline in mental ability that interferes with daily life. Not a normal part of aging, most dementias are typically caused by damaged brain cells.
Of all the dementias, Alzheimer’s disease is the most common, accounting for 60-80% of the cases. In other words, it is a specific disease while “dementia” is a general term for a life-altering decline in brain function .
Recommended Reading: Smelling Farts Dementia
Race May Affect Alzheimer’s Survival
Study Shows Latinos and African-Americans With Alzheimer’s Disease Live Longer Than Whites
The findings from a study involving nearly 31,000 patients treated at more than 30 Alzheimer’s centers across the country revealed that, compared with whites, Latinos were 40% and African-Americans were 15% less likely to die during the study period.
The ethnic differences were seen even after researchers accounted for other factors known to influence survival, including education level and age at symptom onset.
Researcher Kala Mehta, DSc, who is an epidemiologist at the University of California, San Francisco, says she went into the study expecting to find that whites live longer than the other ethnic groups studied following an Alzheimer’s diagnosis.
“That was our original hypothesis, but it wasn’t what we found,” she tells WebMD.
What Are Risk Factors
- Risk factors are aspects of your lifestyle, environment and genetic background that increase the likelihood of getting a disease.
- Risk factors on their own are not causes of a disease. Rather, risk factors represent an increased chance, but not a certainty, that dementia will develop.
- Similarly, having little or no exposure to risk factors does not necessarily protect a person from developing dementia.
There are some risk factors that can be changed, and some that cannot â read on to know which are which!
Read about risk factors for dementia in our downloadable, print-friendly infosheet.
This sheet also contains strategies and lifestyle changes that can help you reduce your risk of developing dementia.
Read Also: Alzheimer’s Lack Of Neurotransmitter
Estimates Of The Number Of People With Alzheimer’s Dementia By State
Table lists the estimated number of people age 65 and older with Alzheimer’s dementia by state for 2020, the projected number for 2025, and the projected percentage change in the number of people with Alzheimer’s between 2020 and 2025.,
| Projected Number with Alzheimer’s | Percentage Increase |
|---|---|
| 30.0 |
- Created from data provided to the Alzheimer’s Association by Weuve et al.,
As shown in Figure , between 2020 and 2025 every state across the country is expected to experience an increase of at least 6.7% in the number of people with Alzheimer’s. These projected increases in the number of people with Alzheimer’s are due solely to projected increases in the population age 65 and older in these states. Because risk factors for dementia such as midlife obesity and diabetes can vary dramatically by region and state, the regional patterns of future burden may be different than reported here. Based on these projections, the West and Southeast are expected to experience the largest percentage increases in people with Alzheimer’s dementia between 2020 and 2025. These increases will have a marked impact on statesâ health care systems, as well as the Medicaid program, which covers the costs of long-term care and support for many older residents with dementia, including more than a quarter of Medicare beneficiaries with Alzheimer’s or other dementias.
FIGURE 3
What Happens In Alzheimer Disease
You probably know that your brain works by sending signals. Chemical messengers, called neurotransmitters , allow brain cells to talk to each other. But a person with Alzheimer disease has lower amounts of neurotransmitters.
People with Alzheimer disease also develop deposits of stuff that prevent the cells from working properly. When this happens, the cells can’t send the right signals to other parts of the brain. Over time, brain cells affected by Alzheimer disease also begin to shrink and die.
You May Like: Senile Dementia Treatments
What Are Some Complications Of Alzheimers Disease
Alzheimers disease is an irreversible form of dementia. The rate of progression differs between people: some people have it only in the last 5 years of their life, while others may have it for as long as 20 years. Alzheimers disease eventually leads to complete dependence and increasing frailty. This means a secondary illness, such as pneumonia, may eventually cause death.
Other complications of Alzheimers disease may include:
- an inability to complete daily tasks such as planning meals and managing money
- a tendency to wander from home
- personality changes such as anxiety, depression and irritability that make relationships more difficult
- delusions and hallucinations in advanced stages of the disease
Medications To Treat The Underlying Alzheimer’s Disease Process
Aducanumab is the first disease-modifying therapy approved by the FDA to treat Alzheimers disease. The medication helps to reduce amyloid deposits in the brain and may help slow the progression of Alzheimers, although it has not yet been shown to affect clinical outcomes such as progression of cognitive decline or dementia. A doctor or specialist will likely perform tests, such as a PET scan or analysis of cerebrospinal fluid, to look for evidence of amyloid plaques and help decide if the treatment is right for the patient.
Aducanumab was approved through the FDAs Accelerated Approval Program. This process requires an additional study after approval to confirm the anticipated clinical benefit. If the follow-up trial fails to verify clinical benefit, the FDA may withdraw approval of the drug. Results of the phase 4 clinical trial for aducanumab are expected to be available by early 2030.
Several other disease-modifying medications are being tested in people with mild cognitive impairment or early Alzheimers as potential treatments.
Read Also: What’s The Difference Between Dementia And Alzheimer’s And Senility
What The New Study Found
Researchers from the Florida State University College of Medicine examined health data from a long-term aging study and 18 other studies, involving nearly 3,000 participants in total. They found more amyloid and tau deposits in people with these personality traits:
-
High levels of neuroticism, the tendency to have negative feelings
-
Low levels of conscientiousness, the tendency to be careful, organized, goal-directed and responsible.
“We have done studies showing who’s at risk of developing dementia, but those other studies were looking at the clinical diagnosis,” said Antonio Terracciano, professor of geriatrics at the College of Medicine. “Here, we are looking at the neuropathology that is, the lesions in the brain that tell us about the underlying pathological change. This study shows that even before clinical dementia, personality predicts the accumulation of pathology associated with dementia.”
Ethnic Differences And Cognitive Testing
The most commonly accepted research criteria for probable or possible AD require the diagnosis to be confirmed by neuropsychological tests demonstrating impairments of performance in memory and two other cognitive domains. However, few cognitive ability measures have been properly validated for use among ethnic minorities in the United States. Lack of such validation may account for the fact that, based on neuropsychological test performance, ethnic minorities are judged to be cognitively impaired more often than non-Hispanic whites. This section will review studies within and outside the United States that have compared the cognitive test performance of different ethnic groups, and describe constructs that might allow for more sophisticated investigations of ethnic differences in the future.
Translators of cognitive measures must use extreme caution and proper methods to adapt measures into another language. describe several examples of Spanish versions of tests that include syntactic, lexical, and spelling errors. These authors also suggest that investigators consult only those who possess native fluency and indepth knowledge of the culture before attempting to translate a measure. The accuracy of translated and adapted instruments should be checked following established guidelines . Researchers and clinicians must also develop standards to determine in which language bilinguals should be assessed .
Norms
Use of Interpreters
You May Like: What Color Ribbon Is For Alzheimer Disease
What Can We Do About This Discrepancy
Speak Up: Raise awareness. Talk to your neighbor. Tell your story. Dementia is not something that should be hidden or hushed, and neither is this disparity in dementia risk based on ethnicity.
Volunteer for Clinical Trials: We need more people from minority backgrounds to participate in clinical trials and other research studies. Many studies consist of populations with limited diversity. You can see a list of clinical trials here at TrialMatch, a service of the Alzheimer’s Association.
Go to Regular Screenings: Medicare coversat no cost to youan annual wellness exam, and this can include screening and testing of your cognition for symptoms of dementia. Be sure to tell your healthcare provider if you’re concerned about your memory . Early detection is very beneficial. It allows for the diagnosis and treatment of conditions that might cause memory loss and confusion but could be reversed if caught and treated. It also can allow for earlier treatment of Alzheimer’s and other types of dementia.
Advocate for Culturally Competent Services and Support Systems: Training in cultural competence helps ensure that healthcare services are provided in a way that honors diversity and encourages minority leadership and participation.
Alzheimer’s Association. Cognitive assessment.
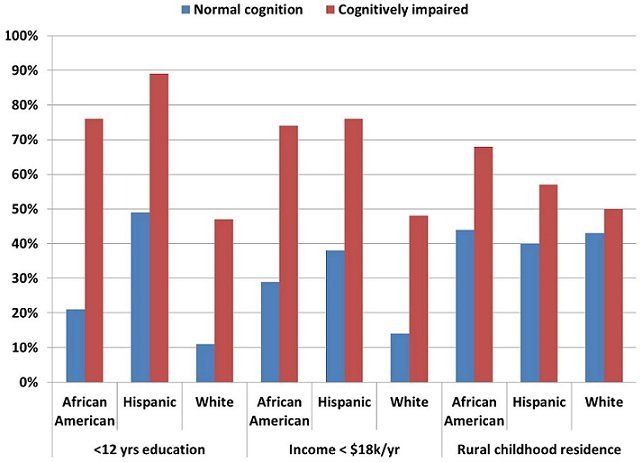
Education And Income Levels
The Alzheimer’s Association outlined three risks that were connected with increased risk of dementia including living in rural areas, a lower education level and having a lower income level. They also found that African Americans and Hispanics were more likely to have a lower education and income level, thus placing them at increased risk for developing dementia.
Read Also: Does Alzheimer’s Cause Dementia
The Costs Of Alzheimers For African Americans
The economic burden of Alzheimers and other dementias for African Americans was $71.6 billion in 2012. Caregiving for African Americans with AD represents the bulk of these costsmore than 60%. More than 60% of the costs are borne by the families of African American women with Alzheimers disease, and close to half of the costs are concentrated in the southern states.
Where people live can also effect Alzheimer’s prevention and treatment for the Black community.
AfricanAmericansAgainstAlzheimers is the nations first organization dedicated to building a coordinated national response to eliminate and address Alzheimers disease among African Americans. The fourth leading cause of death for older African Americans, Alzheimers disease has a disparate impact on African Americans.
Recruitment Of Study Cohorts
In the last decade, innovative approaches that situate disparities within the historical inequities that caused them, while at the same time celebrating cultural assets, have also been shown to be effective strategies for increasing recruitment and engagement in research studies,,,. One study blended use of technology, neighbourhood walking and social reminiscence with the aim of maintaining cognitive health in older African American individuals with and without MCI. Another study was a randomized trial within senior centres that evaluated the ability of a community choir programme called The Community of Voices to promote health and well-being. Such approaches integrated with rigorous mixed methods can reveal unique participant perspectives about barriers to and facilitators of study participation, particularly for studies that require a higher level of commitment, such as brain autopsy,.
You May Like: Does Prevagen Help With Dementia
Impact On Families And Carers
In 2019, informal carers spent on average 5 hours per day providing care for people living with dementia. This can be overwhelming . Physical, emotional and financial pressures can cause great stress to families and carers, and support is required from the health, social, financial and legal systems. Fifty percent of the global cost of dementia is attributed to informal care.
Possible Reasons For Racial And Ethnic Disparities
Possible reasons for racial and ethnic disparities include factors related to measurement of Alzheimer’s disease, genetics, cardiovascular and cerebrovascular disease, socioeconomic factors, cultural differences, and racial and ethnic discrimination. A range of pathways have been suggested that link race and ethnicity with cognitive impairment, some of which have implications for disparities . In this section, we describe the evidence underlying selected factors, mediators, and pathways associated with disparities in this population.
FIGURE 3. Pathways Linking Race/Ethnicity and Cognitive Impairment
: Adapted from Glymour and Manly, 2008.
Read Also: Can Aricept Make Memory Worse
Health Environmental And Lifestyle Factors
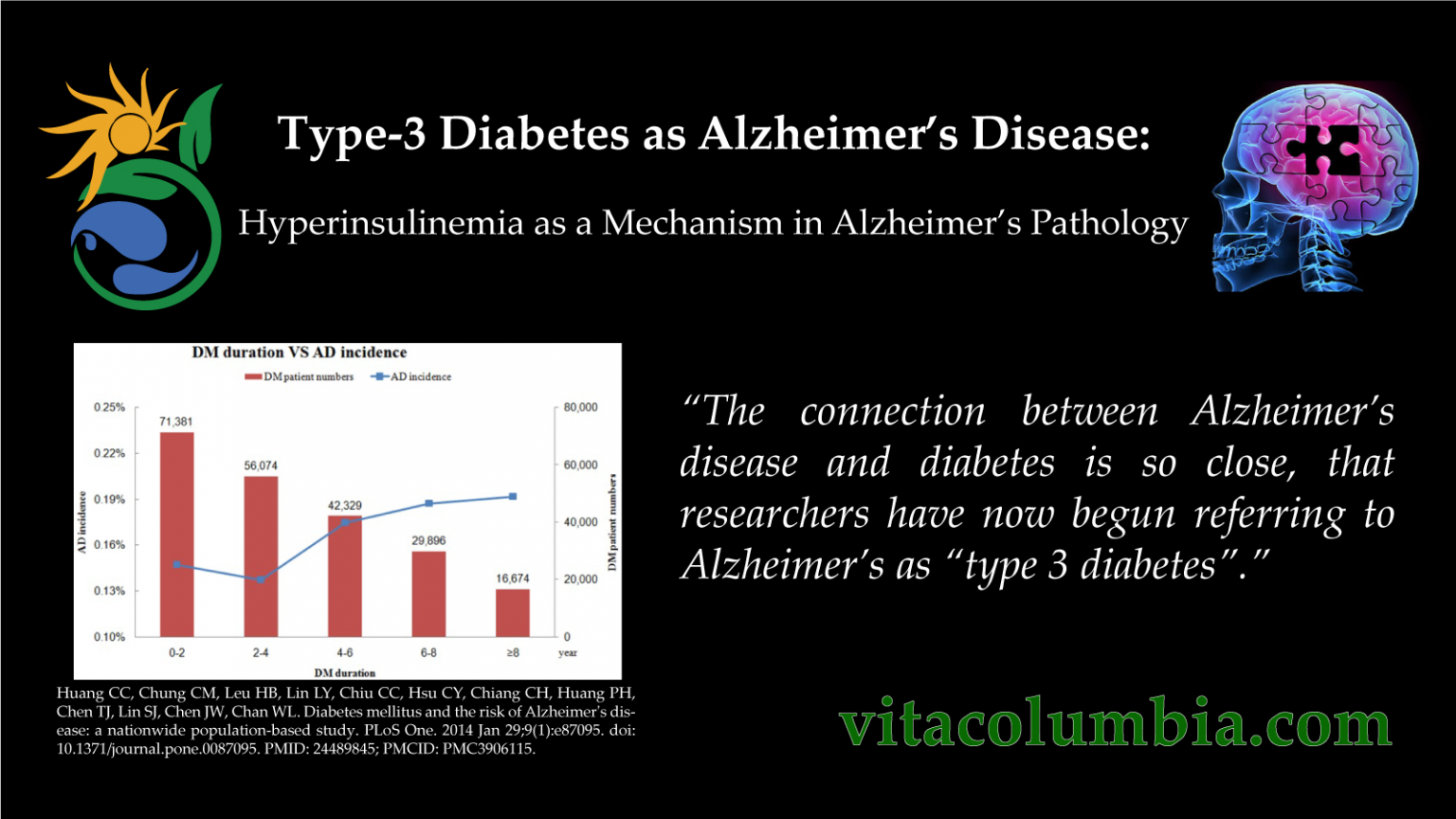
Research suggests that a host of factors beyond genetics may play a role in the development and course of Alzheimers. There is a great deal of interest, for example, in the relationship between cognitive decline and vascular conditions such as heart disease, stroke, and high blood pressure, as well as conditions such as diabetes and obesity. Ongoing research will help us understand whether and how reducing risk factors for these conditions may also reduce the risk of Alzheimers.
A nutritious diet, physical activity, social engagement, and mentally stimulating pursuits have all been associated with helping people stay healthy as they age. These factors might also help reduce the risk of cognitive decline and Alzheimers. Researchers are testing some of these possibilities in clinical trials.
What Are The Symptoms Of Early
For most people with early-onset Alzheimer disease, the symptoms closely mirror those of other forms of Alzheimer disease.
Early symptoms:
-
Withdrawal from work and social situations
-
Changes in mood and personality
Later symptoms:
-
Severe mood swings and behavior changes
-
Deepening confusion about time, place, and life events
-
Suspicions about friends, family, or caregivers
-
Trouble speaking, swallowing, or walking
-
Severe memory loss
Recommended Reading: Alzheimers Dement
How Is Dementia Treated
One of the best things to do if you’re diagnosed with dementia is to keep your mind active and stay busy, maintain a healthy diet and get plenty of sleep.
“Treatment of dementia depends on the underlying cause. Neurodegenerative dementias, like Alzheimer’s disease, have no cure, though there are medications that can help protect the brain or manage symptoms such as anxiety or behavior changes. Research to develop more treatment options is ongoing,” the CDC says. “Leading a healthy lifestyle, including regular exercise, healthy eating, and maintaining social contacts, decreases chances of developing chronic diseases and may reduce the number of people with dementia.” And to protect your life and the lives of others, don’t visit any of these 35 Places You’re Most Likely to Catch COVID.
Avoidable Use Of Health Care And Long
6.5.1 Preventable hospitalizations
Preventable hospitalizations are one common measure of health care quality. Preventable hospitalizations are hospitalizations for conditions that could have been avoided with better access to, or quality of, preventive and primary care. Unplanned hospital readmissions within 30 days are another type of hospitalization that potentially could have been avoided with appropriate post-discharge care. In 2013, 21% of hospitalizations for fee-for-service Medicare enrollees with Alzheimer’s or other dementias were either for unplanned readmissions within 30 days or for an ambulatory care sensitive condition . The total cost to Medicare of these potentially preventable hospitalizations was $4.7 billion . Of people with dementia who had at least one hospitalization, 18% were readmitted within 30 days. Of those who were readmitted within 30 days, 27% were readmitted two or more times. Ten percent of Medicare enrollees had at least one hospitalization for an ambulatory care-sensitive condition, and 14% of total hospitalizations for Medicare enrollees with Alzheimer’s or other dementias were for ambulatory care sensitive conditions.
FIGURE 16
| 15,417 | 46,252 |
Also Check: Does Diet Coke Cause Dementia