Treatments For Parkinsons Disease Dementia And Dementia With Lewy Bodies
Treatments for DLB are similar to PDD and are aimed at symptom control. The motor symptoms of slowness, stiffness and walking difficulties can be treated with Levodopa. However, Levodopa can cause or exacerbate hallucinations, making it difficult to use it as a treatment for patients who have or are at risk of having hallucinations. Sometimes, clinicians will need to treat the hallucinations more aggressively in order for a patient to tolerate Levodopa given to help the motor symptoms. On the flipside, anti-psychotic medications to control hallucinations can worsen motor symptoms, so treating all the symptoms of LBD simultaneously can be a tricky balancing act.
Types Of Lewy Body Dementia
Lewy body dementia includes two related conditionsdementia with Lewy bodies and Parkinsons disease dementia. The difference between them lies largely in the timing of cognitive and movement symptoms. In dementia with Lewy bodies, cognitive symptoms are noted within a year of parkinsonism, any condition that involves the types of movement changes, such as tremor or muscle stiffness, seen in Parkinsons disease. In Parkinsons disease dementia, movement symptoms are pronounced in the early stages, with cognitive symptoms developing years later.
Dementia with Lewy Bodies
People with dementia with Lewy bodies have a decline in thinking ability that may look somewhat like Alzheimers disease. But over time they also develop movement and other distinctive symptoms that suggest dementia with Lewy bodies. Symptoms that distinguish this form of dementia from others may include:
- visual hallucinations early in the course of dementia
- fluctuations in cognitive ability, attention, and alertness
- slowness of movement, difficulty walking, or rigidity
- sensitivity to medications used to treat hallucinations
- REM sleep behavior disorder, in which people physically act out their dreams by yelling, flailing, punching bed partners, and falling out of bed
- more trouble with complex mental activities, such as multitasking, problem solving, and analytical thinking, than with memory
Parkinsons Disease Dementia
What Causes Lewy Body Dementia
Lewy body dementia is a broad term covering two separate neurological disorders: dementia with Lewy bodies and Parkinsons disease dementia. The same biological changes to the brain cause both disorders.
A buildup of Lewy bodies causes LBD. Lewy bodies build up in neurons located in certain areas of the brain that are responsible for behavior, movement, and cognitive ability.
Doctors do not know why you or your loved one develop LBD while others do not. There is some thought that the combination of mutation in a persons genes, environmental risk factors and natural aging might lead to the development of LBD in some people. Research into specific causes is ongoing.
Don’t Miss: Alzheimer’s Disease Color Ribbon
Kathleen Poston Md Msco
Dr. Kathleen Poston is Associate Professor of Neurology at Stanford University. She completed her Movement Disorders fellowship training at Columbia University and a post-doctoral research fellowship at the Feinstein Institute, joining the Stanford faculty in 2009. In addition to LBD RCOE Co-Director, she is the Pacific Udall Center Clinical Core Leader at Stanford and the ADRC Clinical Core Co-Leader. Dr. Postons research lab is focused on understanding the cognitive and other non-motor impairments that develop in patients with Lewy body pathology. With this, the bulk of her clinical practice is caring for parkinsonian patients with cognitive impairments and, for her research studies, she has recruited over 200 parkinsonian patients with a wide range of memory impairments .
What Current Research Is Being Done For Dementia With Lewy Bodies
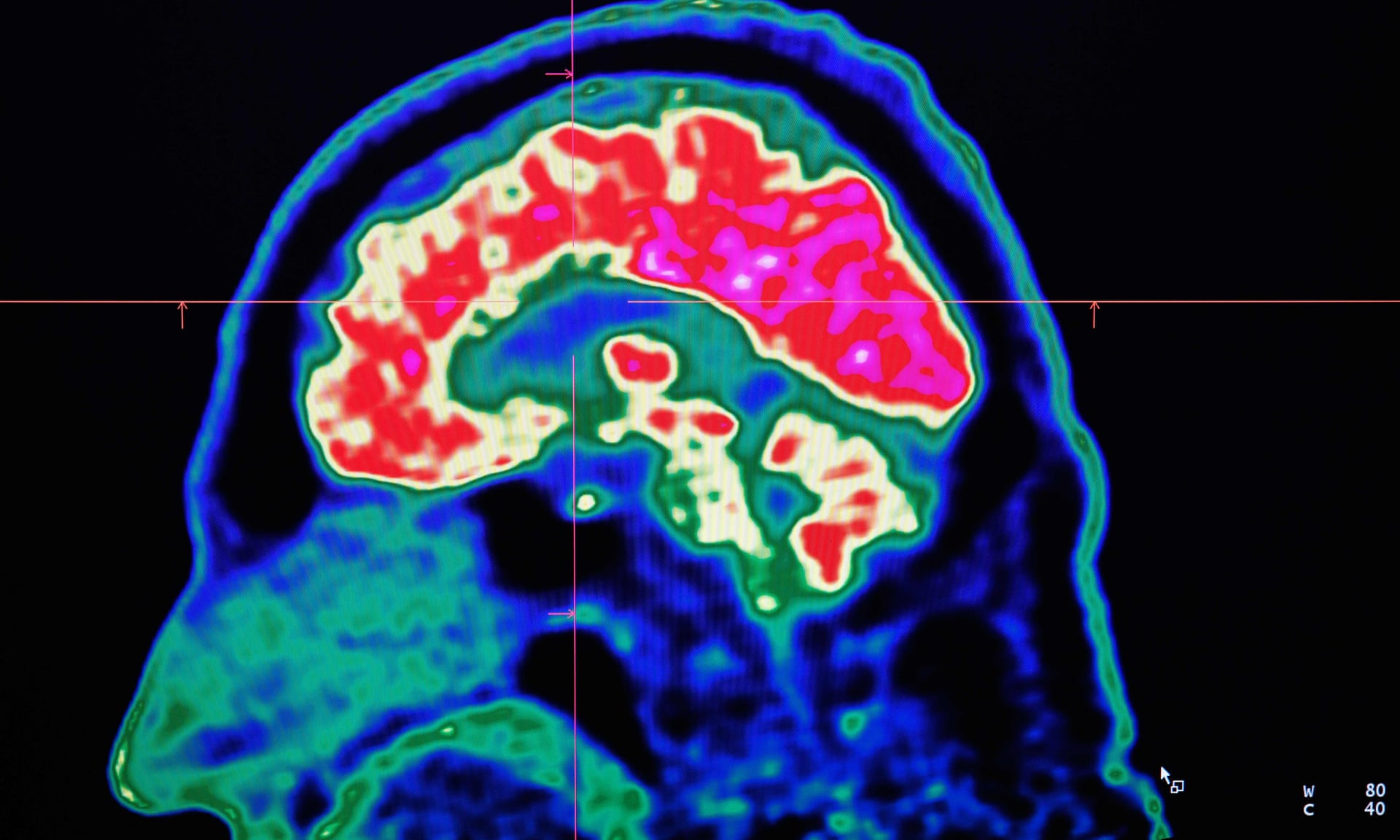
What research are we funding into dementia with Lewy bodies? Find out in our blog series looking at rarer forms of dementia.
Previously in this series we shined a research spotlight on vascular dementia and frontotemporal dementia.
Now, we’ll be taking a closer look at current research related to dementia with Lewy bodies. But first we need to understand a little more about the disease itself.
You May Like: Andrea Mitchell Drunk
About Dr Melita Petrossian
Melita Petrossian, MD, is Director of Pacific Movement Disorders Center and is a fellowship-trained neurologist with clinical interests and expertise in movement disorders such as Parkinsons disease, essential tremor, dystonia, gait disorders, ataxia, myoclonus, blepharospasm, hemifacial spasm, Meige syndrome, spasticity, tics, and Tourettes syndrome.
She also specializes in Parkinsons-related conditions such as Dementia with Lewy Bodies, progressive supranuclear palsy, multiple system atrophy, corticobasal degeneration, primary freezing of gait, and Parkinsons disease dementia.
Research: The Road Ahead
There is a great deal to learn about LBD. At a basic level, why does alphasynuclein accumulate into Lewy bodies, and how do Lewy bodies cause the symptoms of LBD? It is also of increasing interest to the Alzheimers and Parkinsons disease research communities. LBD represents an important link between these other brain disorders, and research into one disease often contributes to better understanding of the others.
Many avenues of research focus on improving our understanding of LBD. Some researchers are working to identify the specific differences in the brain between dementia with Lewy bodies and Parkinsons disease dementia. Others are looking at the diseases underlying biology, genetics, and environmental risk factors. Still other scientists are trying to identify biomarkers , improve screening tests to aid diagnosis, and research new treatments.
Scientists hope that new knowledge about LBD will one day lead to more effective treatments and even ways to cure and prevent the disorder. Until then, researchers need volunteers with and without LBD for clinical studies.
To find out more about clinical trials, talk with a doctor or visit the National Institutes of Health Web site at www.clinicaltrials.gov.
You May Like: Alz Ribbon
Genetic Study Of Lewy Body Dementia Supports Ties To Alzheimers And Parkinsons Diseases
NIH-led study locates five genes that may play a critical role in Lewy body dementia.
In a study led by National Institutes of Health researchers, scientists found that five genes may play a critical role in determining whether a person will suffer from Lewy body dementia, a devastating disorder that riddles the brain with clumps of abnormal protein deposits called Lewy bodies. Lewy bodies are also a hallmark of Parkinsons disease. The results, published in Nature Genetics, not only supported the diseases ties to Parkinsons disease but also suggested that people who have Lewy body dementia may share similar genetic profiles to those who have Alzheimers disease.
Lewy body dementia is a devastating brain disorder for which we have no effective treatments. Patients often appear to suffer the worst of both Alzheimers and Parkinsons diseases. Our results support the idea that this may be because Lewy body dementia is caused by a spectrum of problems that can be seen in both disorders, said Sonja Scholz, M.D., Ph.D., investigator at the NIHs National Institute of Neurological Disorders and Stroke and the senior author of the study. We hope that these results will act as a blueprint for understanding the disease and developing new treatments.
The study was led by Dr. Scholzs team and researchers in the lab of Bryan J. Traynor, M.D., Ph.D., senior investigator at the NIHs National Institute on Aging .
Article:
NIHTurning Discovery Into Health®
Support Stanford Research Into The Causes Of Lewy Body Dementia
A gift to the Sue Berghoff LBD Research Fellowship Fund will support the work of a post-doctoral Research Fellow dedicated to biomarker discovery in people with Lewy Body Dementia , the second most prevalent cause of dementia.
Stanford’s Poston Lab leverages research infrastructure from the Stanford Alzheimers disease Research Center and the Pacific Udall Center for Excellence in Parkinsons Research. These Centers collect in-depth clinical, biological, and imaging data on people with Alzheimers, Parkinsons, and Lewy Body Dementia diseases and older adults with no neurological problems.
Our dedicated Research Fellow would use this data, aiming to identify a biomarker to improve diagnostic accuracy, predict clinical symptoms, or identify underlying pathology. Such a biomarker is critical to the success of future LBD-specific clinical trials, which are critical to the development of potential therapies and a cure.
If youd like to make a donation for this purpose, choose from the following two options.
You May Like: Alzheimer’s Neurotransmitters
Lewy Body Dementia Research Center Of Excellence
We are proud to announce the Lewy Body Dementia Research Center of Excellence at Stanford University! In December 2017 researchers from across the country joined in the first-ever comprehensive network of research centers to conduct LBD clinical trials, provide community outreach, and expand professional continuing medical education. Representing 24 of medicines most prestigious academic medical research centers, these Research Centers of Excellence will help to streamline and standardize LBD science while connecting patients and families with the latest opportunities to participate in LBD clinical trials.
Diagnosis Treatment And Research
The Lewy Body Dementia Association maintains a list of its scientific and medical advisors. Many of these physicians see patients at their clinics or may make referrals to other specialists in your area. See . For general tips on finding a doctor, visit .
The Alzheimers Disease Education and Referral Center maintains a list of research centers funded by the National Institute on Aging at NIH where you may find medical specialists in Lewy body dementia: www.nia.nih.gov/alzheimers/alzheimers-disease-research-centers.
The American Academy of Neurology has a find a neurologist page on its website: .
The American Association for Geriatric Psychiatry has a physician finder on its website: .
Read Also: What Is The Color For Dementia Awareness
Causes And Risk Factors
The precise cause of LBD is unknown, but scientists are learning more about its biology and genetics. For example, they know that an accumulation of Lewy bodies is associated with a loss of certain neurons in the brain that produce two important neurotransmitters, chemicals that act as messengers between brain cells. One of these messengers, acetylcholine, is important for memory and learning. The other, dopamine, plays an important role in behavior, cognition, movement, motivation, sleep, and mood.
Scientists are also learning about risk factors for LBD. Age is considered the greatest risk factor. Most people who develop the disorder are over age 50.
Other known risk factors for LBD include the following:
Dementia With Lewy Bodies
The National Institute of Neurological Disorders and Stroke and other institutes of the National Institutes of Health conduct research related to DLB in laboratories at the NIH and support additional research through grants to major medical institutions across the country. Much of this research focuses on searching for the genetic roots of DLB, exploring the molecular mechanisms of alpha-synuclein accumulation, and discovering how Lewy bodies cause the particular symptoms of DLB and the other synucleinopathies. The goal of NINDS research is to find better ways to prevent, treat, and ultimately cure disorders such as DLB.
Information from the National Library of Medicines MedlinePlus
There is no cure for DLB. Treatments are aimed at controlling the cognitive, psychiatric, and motor symptoms of the disorder. Acetylcholinesterase inhibitors, such as donepezil and rivastigmine, are primarily used to treat the cognitive symptoms of DLB, but they may also be of some benefit in reducing the psychiatric and motor symptoms. Doctors tend to avoid prescribing antipsychotics for hallucinatory symptoms of DLB because of the risk that neuroleptic sensitivity could worsen the motor symptoms. Some individuals with DLB may benefit from the use of levodopa for their rigidity and loss of spontaneous movement.
Recommended Reading: Does Prevagen Help Dementia
Researching The Symptoms Of Dementia With Lewy Bodies
In 2014, Alzheimers Society established eight Doctoral Training Centres across the country to boost the number of PhD students and researchers working on dementia.
Our centre in Newcastle is focused on understanding more about the symptoms of dementia with Lewy bodies that are not related to memory and thinking. This includes investigating what causes fluctuations, understanding why people with dementia with Lewy bodies are more likely to experience depression and examining how the condition affects the ability to walk.
Professor Alan Thomas is leading the Doctoral Training Centre in Newcastle. He said:
Lewy Body Dementia Research Through A Researchers Eyes
Jim Leverenz is a neurologist by training, and hes been studying Lewy body disease since the 1980s. Dr. Leverenz is proud to be the Chair of the Lewy Body Dementia Associations Scientific Advisory Council , a post hes held for seven years. Hes been a part of the SAC for more than a decade, providing up-to-date medical and research information, which LBDA uses to create publications for the general public, caregivers, and healthcare professionals. LBDA and the SAC organize scientific meetings, award pilot grants for Lewy body dementia research, and advocate for increased research funding and the needs of LBD families.
Why did you decide to get involved with Lewy body dementia research?
It happened almost by accident. I was an undergraduate student and I wanted to get involved in research. A pathologist I was talking to said we sometimes see these Lewy bodies in people with dementia would that be something youd like to research? I went on to work on one of the first descriptions of the co-existence of Lewy bodies in Alzheimers. And after my medical training, residency, and fellowship, I got back to working in this area in the 1990s. Today I would say Ive had nearly 500 patients with Lewy body dementia under my care. We know much more than we did before, and there are a lot more options than there used to be but there are still miles to go.
Why do you think there are so few studies for Lewy body dementia?
Don’t Miss: Karen Vieth Edgar Knight
Investigating The Repurposing Of The Asthma Drug Clenbuterol For The Treatment Of Neurodegenerative Brain Disorders
This study is looking at repurposing an asthma drug, known as Clenbuterol, for people with Lewy body dementia.
There are two phases to this study and there will be a break of 14 days between the two. Participants will be given the drug in one of the two treatment periods, but will not know whether they are receiving the drug on the first or second visit.
The study team is initially recruiting people aged 50-80 with a diagnosis of Lewy body dementia, in Barnsley, Blackpool and Manchester. The study is being carried out by MAC Clinical Research and is sponsored by Curasen Inc. Participants will be reimbursed for their time and commitment, as well as reasonable travel and expenses. Other arms of this study are looking at repurposing the same drug for people with Parkinsons disease dementia and Mild Cognitive Impairment.
Caring For A Person With Lewy Body Dementia
As someone who is caring for a person with LBD, you will take on many different responsibilities over time. You do not have to face these responsibilities alone. Many sources of help are available, from adult day centers and respite care to online and in-person support groups.
Below are some important actions you can take to adjust to your new roles, be realistic about your situation, and care for yourself. See the Resources section for more information.
Educate Others About LBD
Most people, including many healthcare professionals, are not familiar with LBD. In particular, emergency room physicians and other hospital workers may not know that people with LBD are extremely sensitive to antipsychotic medications. Caregivers can educate healthcare professionals and others by:
- Informing hospital staff of the LBD diagnosis and medication sensitivities, and requesting that the persons neurologist be consultedbefore giving any drugs to control behavior problems.
- Sharing educational pamphlets and other materials with doctors, nurses, and other healthcare professionals who care for the person with LBD.
- Teaching family and friends about LBD so they can better understand your situation.
Adjust Expectations
Care for Yourself
Address Family Concerns
Helping Children and Teens Cope with LBD
The organizations listed in the Resources section can help with information about caregiver services and support.
You May Like: At What Age Alzheimer’s Start
Lewy Body Dementia Studies Currently Recruiting Participants
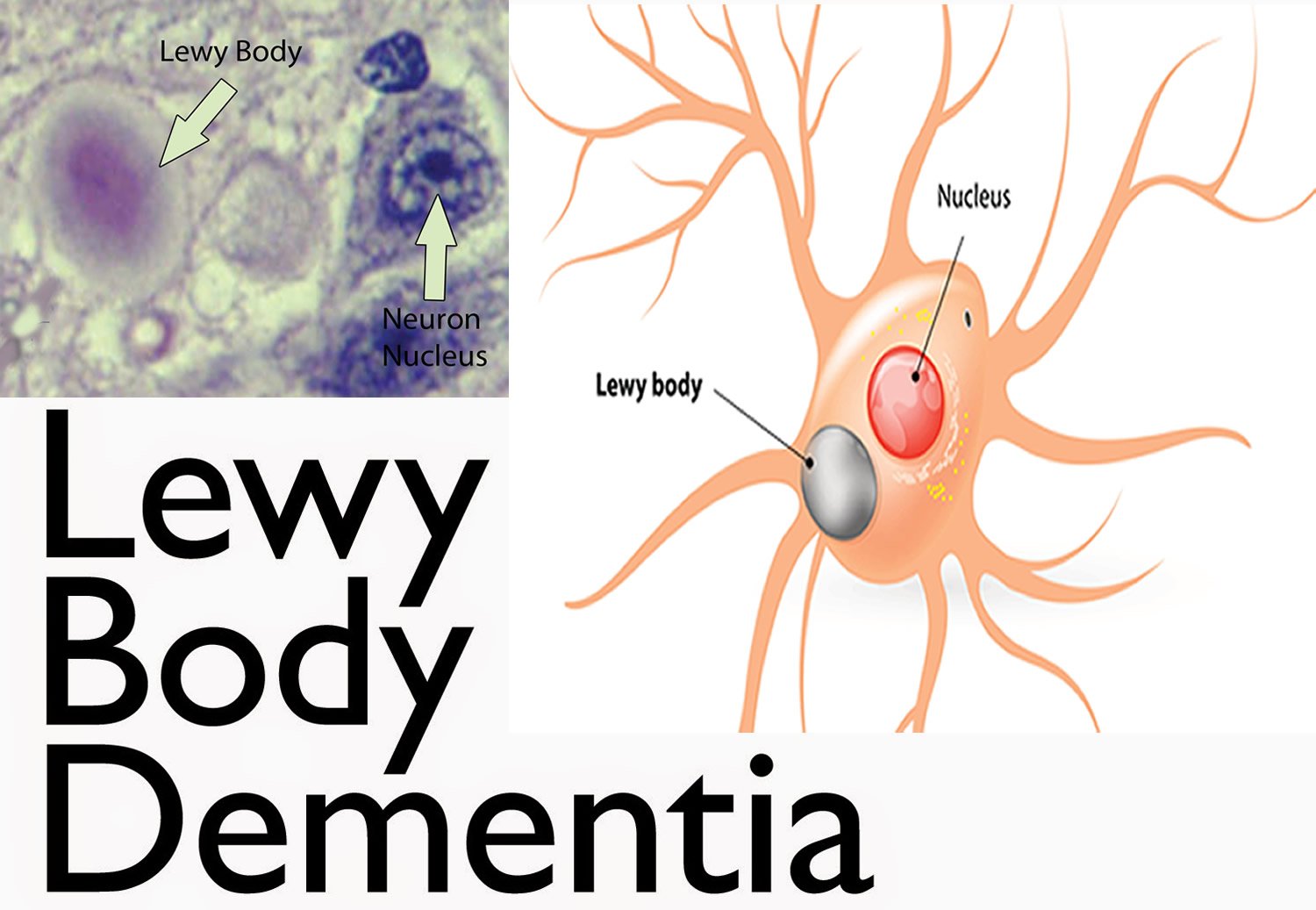
When someone develops this type of dementia, protein deposits called Lewy bodies develop in the brain regions involved in thinking, memory and movement.
Lewy body in a neuron affected by Parkinsons disease
Lewy body dementia and Parkinsons disease share similar symptoms including visual hallucinations movement disorders such as slowed movement, tremor or a shuffling walk cognitive problems and sleep difficulties.
We need to find out more about the indicators of the disease and see if existing medications can be repurposed to treat it.
Autonomic Dysfunction/anosmia And Other Nonspecific Prodromal Lb Disease Symptoms
Patients with DLB frequently report a history of autonomic dysfunction at first clinic attendance, with 25%50% complaining of one of more among constipation, orthostatic dizziness, urinary incontinence, erectile dysfunction, increased sweating, or increased saliva., In a cohort of patients with pure autonomic failure, 34% converted to an overt -synucleinopathy over 6 years of follow-up this was to DLB , PD , or MSA . However, because there are many other causes for autonomic dysfunction in older people, these symptoms, either alone or in combination, have low positive predictive value. The situation is similar for hyposmia, which also frequently occurs early in prodromal DLB and PD, but which can have many other causes in this age group.
Recommended Reading: Did Ronald Reagan Have Alzheimer
Clinical Trials On The Horizon
SAK3 administration promotes the destruction of misfolded proteins, meaning the therapeutic has the potential to solve the problems of diverse protein misfolding diseases, such as Parkinsons disease, Lewy body dementia, and Huntington disease, in addition to Alzheimers disease, he adds.
Prof. Dexter cautioned that there remains much more work to do.
While these findings are encouraging, this research is still at an early stage, he said.
The next crucial step will be to take this potential new drug forwards to test in people in clinical trials. Thats when well know whether it truly could be a game-changing treatment for people with degenerative brain conditions.
Prof. Fukunaga confirmed in an email to Medical News Today that his team is seeking a partner to carry out clinical trials of SAK3 in the United States. They hope to start trials within a year.