Current Barriers To Provision Of Speech And Language Therapy Services Across The Uk Usa And Australia
So why are all people with PPA not being seen by speech and language services? It is clear that there are several barriers that limit access.
First, many people with PPA are never referred to speech and language therapy services in the first place. There may be scepticism on the part of the referrer, due to the lack of evidence that these interventions give clinically meaningful benefit in PPA. The healthcare community undoubtedly has poor awareness of the breadth of the speech and language therapist role, and the potential benefit of non-pharmacological interventions for PPA. Neurologists more often refer people with PPA to speech and language therapy than other professionals, across the UK and Australia,, perhaps due to their familiarity with this professions role with people with post-stroke aphasia.
The Patient With Late Stage Or Global Aphasia
All PPA syndromes tend ultimately to give rise to global language failure with mutism or sparse, stereotyped utterances as well as more widespread cognitive decline. Accordingly, diagnosis later in the course may be more informed by associated neurological features such as Parkinsonism. On the other hand, âmixedâ aphasia does not of itself signify advanced disease: some patients exhibit deficits that transcend canonical syndromic boundaries early on . In our experience, this includes cases with progranulin mutations and Alzheimerâs, Pickâs and other pathological associations are reported .
Common Recommendations To Prevent Stroke And Aphasia
- Exercise, according to your doctors recommendations
- Eat healthy, including cutting back on sodium
- If you smoke, quit
- Maintain a healthy weight
Additionally, be sure to monitor your cholesterol, blood sugar, and blood pressure levels. Make sure they are in a normal range and if not, ask your doctor how to lower them.
Don’t Miss: Alzheimer’s Awareness Color
A Clinical Framework For Assessing Language Functions In Primary Progressive Aphasia
When confronted by an aphasic patient, it is important firstly to establish the context of the language disturbance. This usually requires the help of an informant who knows the patient well and can supply reliable background information. A diagnosis of PPA requires that speech or language dysfunction was the initial and most salient clinical complaint . However, the patientâs previous verbal skills are relevant to interpreting current deficits. It is also necessary to determine the extent of any uncorrected peripheral hearing or visual impairments as these can impact significantly on everyday communication and performance on language tests. In defining the history of the language problem, it is essential to establish the circumstances of onset and very first symptoms , overall duration and tempo. The length of the history bears strongly on the interpretation of deficits, since PPA syndromes tend to converge over time . In PPA, a history of gradual, but unrelenting decline over a number of months or several years is typical, but some apparent fluctuation is not uncommon, particularly under conditions that stress the language system, such as public speaking or conversations by telephone or in a non-native tongue. There may have been a sentinel event such as a family celebration or minor head injury that first drew attention to the patientâs difficulties informants may interpret this as an acute onset but a searching history usually reveals a more insidious prodrome.
You Are In The Section
- Frontotemporal dementia
- Progressive Non Fluent Aphasia
Progressive Non Fluent Aphasia is a condition which affects a persons ability to use language. Its part of a group of conditions known as frontotemporal dementia .
A person may experience symptoms like:
- Slow or hesitant speech e.g. speaking in shorter sentences
- Difficultly speaking or starting a conversation preferring to listen instead
- Difficulty finding the right word
- An increase in grammatical mistakes and pauses in speech
- Difficulty understanding complex sentences
- Making mistakes in sounds used in speech.
Recommended Reading: Color For Dementia Awareness
Home Healthcare In Lewisville
Having a family members health decline is a tough thing to experience. In fact, as Alzheimers disease progresses, many families may feel that caring for someone who was diagnosed with the diseases is a full-time job. Because of this, it is important that your loved one has quality home care services.
At Aspen Healthcare, we strive to meet the needs of our patient who may require care at home. Located in the Lewisville area, our services range from skilled nursing care and rehabilitation to personal care and living assistance services.
Unfortunately, it is very hard to cope with the reality that your family member will not be able to live a normal life without the help of health care. Our highly qualified and educated staff is what sets us apart from other home health care agencies. When you entrust the care of your family members health in our hands, you can rest assured they will be in the best of care.
Contributions Of Ppa To Neurolinguistics And Cognitive Neuroscience
The clinicopathological correlations of classic aphasiology were based mostly onobservations in patients with focal cerebrovascular lesions where the injury site,usually including cortical as well as subcortical areas, is abruptly and completelydestroyed. In primary progressive aphasia, the gradual and selective loss ofcortical neurons in the language network leads to more subtle perturbations anddissociations, some of which have shed new light on the neurobiology of languagefunction. One of the most consequential new insights has been the realization thatthe classic neurological account of language is incomplete and that the anteriortemporal lobe of the left hemisphere needs to be inserted into the language networkas a third major hub with a critical role in language comprehension, especially ofwords denoting concrete entities.,- In fact, some of these observations have castserious doubts on existing characterizations of Wernicke’s area and its role inlanguage comprehension. Anotherequally important insight has been the realization that grammatical ability andfluency can be dissociated neuropsychologically as well as anatomically., It is quite likely that future research in PPA will lead toadditional revisions of the language network.
Read Also: Dementia Vs Senility
Causes Of Aphasia And Dementia
We have already established that both dementia and aphasia are caused when there are damages in the brain.
What sets the two conditions apart is the section of the brain that is hurt.
For aphasia, people will get the illness when the part of the brain that controls speech is damaged. This mostly happens because of traumatic brain injury or a stroke.
Infections and brain tumors are other probable causes of aphasia.
Dementia is quite different from this.
Even though a stroke or traumatic brain injury can also cause it, it is mostly a result of amyloid plaque build-up in the brain, which leads to the development of the most common dementia type known as Alzheimers disease.
This build-up cuts off neurons in the brain that are responsible for relaying messages from one part of the brain to the next.
It ends up affecting the entire brain and not the speech part, as is the case with aphasia.
This is why a person with dementia may not know the name of a familiar face or even remember how to hold a fork because they cannot access their memories.
The person with aphasia only has problems accessing the part of the brain that deals with speech.
These differences between aphasia and dementia are instrumental when it comes to diagnosis.
A doctor can study the symptoms to know whether a person is only having trouble with speech or they are having communication problems as well as other challenges with their day to day lives to understand what the person is suffering from.
Fluent Production Normal Repetition And Preserved Comprehension: Anomic Aphasia
The main feature of anomic aphasia is a supramodal word-finding difficulty, with little effect on comprehension. Supramodal implies that the anomia is present regardless of the sense modality through which the item to be named is presented. Language production is fluent, but it is devoid of substantive content, circumlocutory, and paraphasic. Repetition is normal, which means that anomic aphasia is a transcortical disorder, and it has been suggested that it is on a continuum with TSA.
Norman Geschwind’s adaptation of the Wernicke-Lichtheim model attributed the role of name retrieval to the angular gyrus, which is widely recognized as a zone of convergence for visual, auditory, and tactile information and a repository for semantic information. It is anatomically well placed as a nodal structure for the activation of semantically specified concepts. It is richly interconnected with the posterior temporal region, where activated concepts are converted to phonemic form. Angular gyrus lesions produce the features of anomic aphasia, but it is recognized that dysnomic features can arise from multiple loci and are therefore poorly localizing. In the author’s own experience, however, extra-angular lesions seldom produce the prominent fluent and circumlocutory output disturbance of anomic aphasia. For example :13
Examiner: Can you tell me about your illness?
Patient: I had a. I had a one or two three There’s one I had a a I know the exact part of it.
Examiner: Anesthesia?
Also Check: Colors For Alzheimer’s Awareness
How Is Aphasia Diagnosed
Aphasia is usually first recognized by the physician who treats the person for his or her brain injury. Most individuals will undergo a magnetic resonance imaging or computed tomography scan to confirm the presence of a brain injury and to identify its precise location. The physician also typically tests the person’s ability to understand and produce language, such as following commands, answering questions, naming objects, and carrying on a conversation.
If the physician suspects aphasia, the patient is usually referred to a speech-language pathologist, who performs a comprehensive examination of the person’s communication abilities. The person’s ability to speak, express ideas, converse socially, understand language, and read and write are all assessed in detail.
How Common Is Aphasia
If you or someone you know has aphasia, youre not alone!
Most people have never heard of aphasia. Unless you or a loved one is impacted by aphasia, youre not likely to know much about it. So, it might surprise you to learn that aphasia is actually a relatively common condition. Approximately 2 million people in the United States have aphasia, though estimates vary. Approximately 180,000 people are diagnosed with aphasia every year. About 1/3 of people who have strokes get aphasia.
Aphasia affects more people than many other conditions that you probably have heard of, such as Parkinsons Disease, multiple sclerosis and cerebral palsy. However, according to a 2016 survey, 85% of people had never even heard the term aphasia.
Recommended Reading: Bobby Knight Health Update
Dementia & Alzheimer’s Disease
It is easy to confuse some of the symptoms of aphasia and dementia, which often leads to questions on whether the two medical conditions are related.
Before we go deeper into answering the query, it is important to first define these conditions.
Aphasia is a language or speech disorder that is a result of complications in the brain.
In Greek, the word Aphasia translates to speechlessness.
Dementia, on the other hand, is a general term that describes a range of medical conditions that are caused by abnormal brain changes.
In Latin, the term dementia stands for madness which implies severe memory loss in a person who was previously normal beyond what is expected as a person grows older.
What Types Of Aphasia Are There
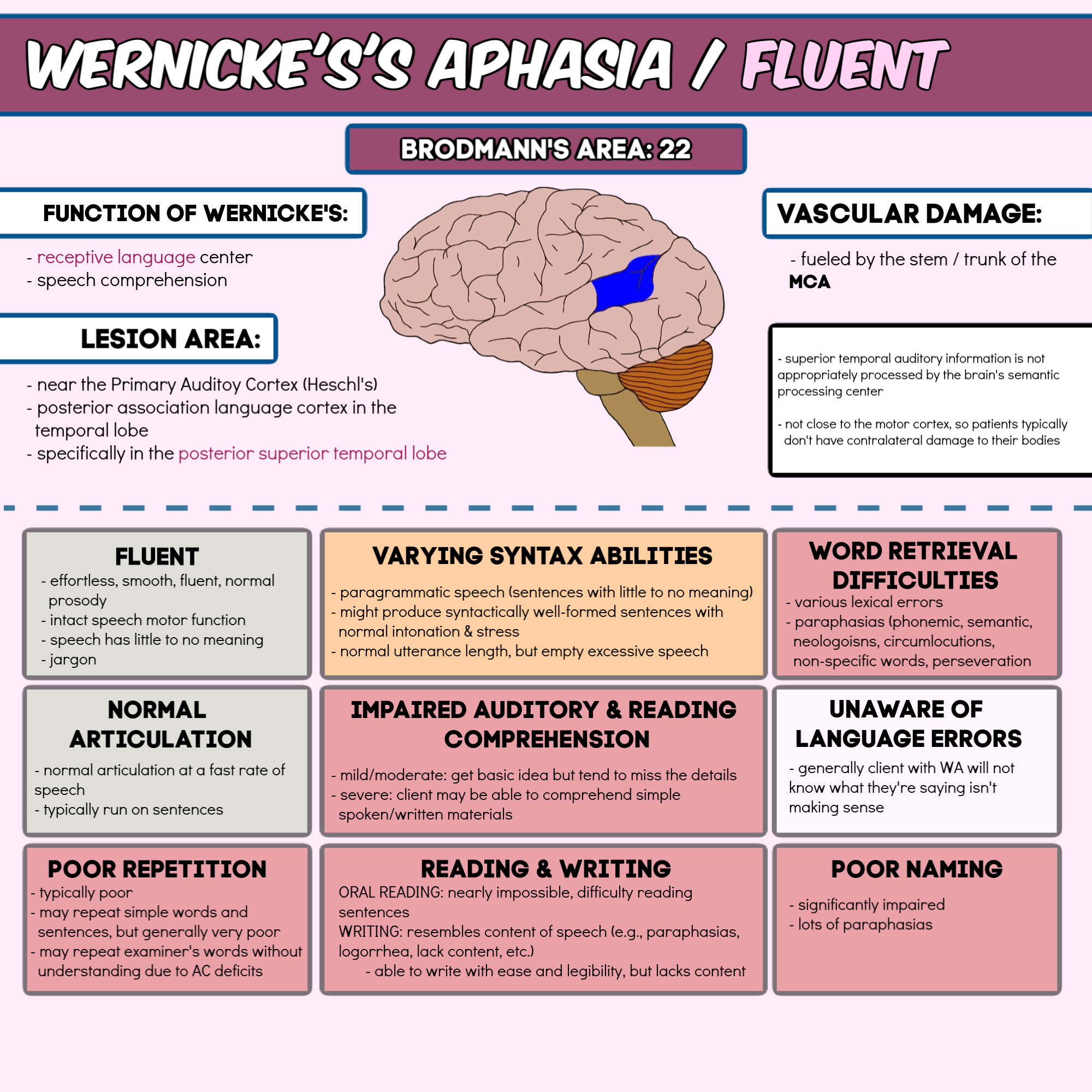
There are two broad categories of aphasia: fluent and nonfluent, and there are several types within these groups.
Damage to the temporal lobe of the brain may result in Wernicke’s aphasia , the most common type of fluent aphasia. People with Wernicke’s aphasia may speak in long, complete sentences that have no meaning, adding unnecessary words and even creating made-up words.
For example, someone with Wernicke’s aphasia may say, “You know that smoodle pinkered and that I want to get him round and take care of him like you want before.”
As a result, it is often difficult to follow what the person is trying to say. People with Wernicke’s aphasia are often unaware of their spoken mistakes. Another hallmark of this type of aphasia is difficulty understanding speech.
The most common type of nonfluent aphasia is Broca’s aphasia . People with Broca’s aphasia have damage that primarily affects the frontal lobe of the brain. They often have right-sided weakness or paralysis of the arm and leg because the frontal lobe is also important for motor movements. People with Broca’s aphasia may understand speech and know what they want to say, but they frequently speak in short phrases that are produced with great effort. They often omit small words, such as “is,” “and” and “the.”
Recommended Reading: What Are Complications Of Alzheimer Disease That Cause Death
Tips For Communicating With Someone With Dementia
- Make sure you have the full attention of the person before you speak to them.
- Make sure they can see you clearly.
- Make eye contact with them. This will help them to focus on you.
- Minimise background noise and other distractions, such as the radio, TV or other peoples conversations.
- Give the person plenty of time to talk. Don’t press them to remember the right word unless you need it to understand what they are saying.
- If the person has difficulty finding the right word or finishing a sentence, ask them to explain it in a different way.
- If they are struggling to speak, suggest other ways of expressing themselves, such as drawing, gesturing or pointing.
- Avoid asking open-ended questions.
Frontotemporal Dementia Of The Temporal Type
Semantic dementia is the fluent type of progressive aphasia and is primarily associated with temporal lobe involvement. As in PNA, the onset of semantic dementia is insidious and the course of the impairment is progressive. SD is characterized by effortless, fluent, grammatical speech. Repetition and writing skills are basically intact. By contrast, word production and word comprehension are impaired. As in fluent aphasia , speech often appears empty, due to the increased use of vague terms. Word substitutions are common, especially as the dementia progresses. Researchers have pointed out that the lexical deficit in SD can indicate loss of semantic knowledge. Evidence for this can be found in the semantically based word production errors and in word and object recognition errors produced by individuals with SD.
Lee Goldman MD, inGoldman-Cecil Medicine, 2020
Don’t Miss: Progressive Aphasia Dementia
The Worried Well Or Functional Patient
Word-finding difficulty is a very common complaint in patients attending memory clinics . Many will be experiencing the effects of normal ageing and intercurrent stressors they typically describe inefficiency in recalling names or clearly expressing their thoughts when preoccupied or fatigued and have no evidence of language deficits on objective testing. A taxonomy of neurologically unexplained, âfunctionalâ or ânon-organicâ speech disorders has been described . In our experience, these cases are rare and tend to present as excessively deliberate, but immaculately executed speech or with isolated disturbances of prosody . Dysprosody is a regular accompaniment of nfvPPA and âpureâ primary progressive dysprosodia is a rare satellite syndrome in the PPA spectrum . Indeed, âforeign accent syndromeâ has been described as a presentation of PPA . Our patients with nfvPPA have exhibited degraded native accents or loss of a previously competent second language accent, rather than developing a facsimile foreign accent. âOrganicâ dysprosody tends to be brought out by circumstances calling for heightened control of vocal intonation .
When interpreting a language disorder as âneurologically unexplainedâ, it is important to appreciate that bona fide PPA syndromes can have quite counter-intuitive manifestations. An expert second opinion may be useful and the passage of time often clarifies the situation.
Hearing Loss And Dementia
Overall, 15% of the adult population in the United States age 18 and older report having some trouble hearing . Self-reported hearing loss increases with age, with 5.5% of adults ages 1839, 19% of adults ages 4069, and 43% of adults over age 70 reporting difficulty hearing without a hearing aid .
Adjusting for other risk factors , studies show that hearing loss is independently associated with increased risk of dementia . For individuals over 60 years of age, more than one third of the risk of all-cause dementia was found to be associated with hearing loss .
Further, individuals with baseline hearing loss were found to have greater rates of cognitive decline over time than individuals with normal hearing , and the mean time to develop dementia was reported to be faster for individuals with self-reported hearing loss than for individuals without self-reported hearing loss .
Several hypotheses have been proposed to account for the association between hearing loss and dementia. They include the following:
It is possible that the mechanism proposed by each of these hypotheses is not mutually exclusive, and that each contributes individually or in combination to increase the risk of dementia. Further investigation is needed to clarify the relationship between hearing loss and dementia .
Roles and Responsibilities
Recommended Reading: What Color Represents Dementia
What Are The 7 As Of Dementia
The Seven As are an easy way for caregivers to remember which areas of the brain can be affected by dementia. Each of these As represents damage to a particular part of the brain:
- Anosognosia the individual no longer realizes there is something wrong.
- Amnesia the individual suffers memory loss beginning with short-term and eventually long-term memories.
- Aphasia the individual experiences loss of language skills, including the ability to speak, understand, read or write.
- Agnosia the individual is unable to recognize things through the senses: sight, sound, taste, touch and smell.
- the individual has difficulty with movement and activities involving coordination, like tying shoelaces, doing up zippers, and driving.
- Altered perceptions the individual suffers loss of depth perception, for example.
- Apathy the individual is unable to, or lacks interest in beginning activities, or staying involved in a conversation or task.
As a caregiver, keep in mind that a person with dementia may not experience all of the As. Dementia can affect several different areas of the brain, but not always at the same time.
Who Gets Frontotemporal Dementia
FTD can affect anybody. It typically affects people at a younger age than Alzheimers disease, with symptoms beginning in the 50s or 60s, and sometimes younger.
Almost a third of people with FTD have a family history of dementia. However, only about 10-15% of cases have familial FTD, in which a gene mutation is passed on that causes the disease.
The genetic basis of FTD is not fully understood and is actively being researched.
Don’t Miss: Alzheimer’s Neurotransmitters