What Medications Treat Dementia In Head Injury Cases
Persons with head injury may require medication to treat symptoms such as depression, mania, psychosis, aggression, irritability, mood swings, insomnia, apathy, or impaired concentration. Headaches may also get better with drug treatment.
Drugs used to treat such symptoms are called psychotropic or psychoactive drugs. They work by changing the way the brain works. Head-injured persons are more sensitive to drug side effects. Doses and schedules may require frequent adjustment until the best regimen is found.
Most people with dementia due to head injury are treated with the same drugs used to treat dementia or other causes. In many cases, these drugs have not been specifically tested in persons with a head injury. There are no established guidelines on psychotropic drug treatment after head injury.
Antidepressants
These drugs are used to treat depressive symptoms due to head injury.
Dopaminergic agents
These drugs increase the amount of a brain chemical called dopamine.
- Increasing the amount of dopamine may improve concentration, attention, and interest level in people who have sustained a head injury.
- These drugs may interact with antidepressants to improve mood swings.
- The most potent of these drugs is levodopa it also has the most side effects.
- Other examples include bromocriptine and the stimulant dextroamphetamine , which increases levels of dopamine and another neurotransmitter called norepinephrine.
Antipsychotic agents
Antiepileptic drugs
Mood stabilizers
Are Brain Bleeds Fatal
Brain bleeds, regardless of location, usually happen suddenly. A brain bleed causes brain damage and yes, they can be life-threatening. The seriousness and outcome of a brain bleed depends on its cause, location inside the skull, size of the bleed, the amount of time that passes between the bleed and treatment, your age and overall health. Once brain cells die, they do not regenerate. Damage can be severe and result in physical, mental, and task-based disability.
Can Dementia Get Worse Suddenly
Dementia is a progressive condition, meaning that it gets worse over time. The speed of deterioration differs between individuals. Age, general health and the underlying disease causing brain damage will all affect the pattern of progression. However, for some people the decline can be sudden and rapid.
Also Check: Dementia Color Ribbon
How Is A Brain Hemorrhage Treated
Once you see a doctor, they can determine which part of the brain is affected based on your symptoms.
Doctors may run a variety of imaging tests, such as a CT scan, which can reveal internal bleeding or blood accumulation, or an MRI. A neurological exam or eye exam, which can show swelling of the optic nerve, may also be performed. A lumbar puncture is usually not performed, as it may be dangerous and make things worse.
Treatment for bleeding in the brain depends on the location, cause, and extent of the hemorrhage. Surgery may be needed to alleviate swelling and prevent bleeding. Certain medications may also be prescribed. These include painkillers, corticosteroids, or osmotics to reduce swelling, and anticonvulsants to control seizures.
How Is Vascular Dementia Diagnosed
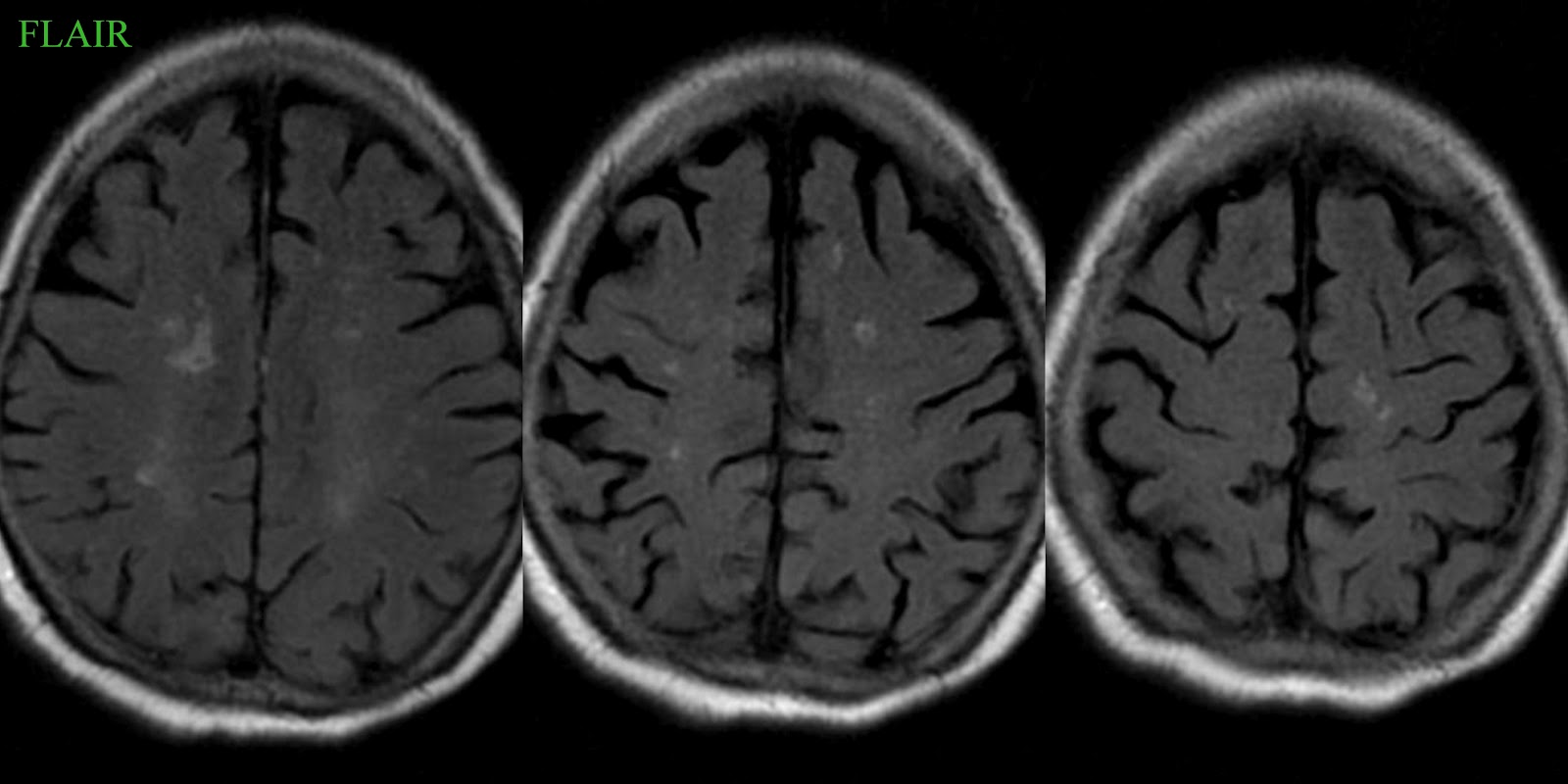
In addition to a complete medical history and physical exam, your healthcare provider may order some of the following:
- Computed tomography . This imaging test uses X-rays and a computer to make horizontal, or axial images of the brain. CT scans are more detailed than general X-rays.
- FDG-PET scan. This is a PET scan of the brain that uses a special tracer to light up regions of the brain.
- Electroencephalogram . This test measures electrical activity in the brain
- Magnetic resonance imaging . This test uses large magnets, radiofrequencies, and a computer to make detailed images of the brain.
- Neuropsychological assessments. These tests can help sort out vascular dementia from other types of dementia and Alzheimer’s.
- Neuropsychiatric evaluation. This may be done to rule out a psychiatric condition that may resemble dementia.
Read Also: Aphasia And Alzheimer’s
Alzheimers And Vascular Dementia
Unlike AD, VCI often begins with symptoms other than the loss of the ability to recall and reexperience specific episodes from ones past. Researchers have noted that people with VCI often develop more noticeable difficulty with attention, information processing, and executive functioning at the outset of the disease. Memory and language effects vary more. Changes in behavior including depression and apathy are common. Recognition of VCI is complicated by the fact that some standard dementia tests are less able to detect the impairment associated with VCI.
Also Check: What Shampoos Cause Alzheimerâs Disease And Cancer
When Dementia Isnt Alzheimers: Vascular And Lewy Body Dementias
Elizabeth Daghfal is a writer, teacher, speaker, and community volunteer. When she isn’t teaching or writing– Who are we kidding? Her husband and five kids say she’s ALWAYS teaching and writing. She has a passion to help people who are struggling and is happy to say her shoulders are drip-dry. Born and raised in the South, she now lives in Wisconsin and loves it–except for the fifteen months of winter. Read more about her at elizabethdaghfal.com.
You May Like: How Long Does A Person Live After Being Diagnosed With Alzheimer’s
Blood Vessel Disease Linked To Dementia
Strategies that protect blood vessels also fight aging-related memory loss.
Like a slow, invisible thief, Alzheimer’s disease steals memory and so much more. Its partner in crime, vascular dementia, has long lurked in the shadows. A scientific statement from the American Heart Association and American Stroke Association puts the spotlight on vascular dementia and offers recommendations for preventing it.
To continue reading this article, you must log in.
- Research health conditions
- Prepare for a doctor’s visit or test
- Find the best treatments and procedures for you
- Explore options for better nutrition and exercise
What Other Things Help
In addition to medications, there are various ways to help a person with vascular dementia. Research has shown that physical exercise and maintaining a healthy weight help to enhance brain health and reduce the risk of heart problems, stroke and other diseases that affect blood vessels. A balanced diet, enough sleep and limited alcohol intake are other important ways to promote good brain health and reduce the risk for heart disease. Other illnesses that affect the brain, such as diabetes, high blood pressure and high cholesterol, should also be treated if present.
Read Also: Neurotransmitter Involved In Alzheimer’s
How Is Traumatic Brain Injury Diagnosed
Diagnosis of traumatic brain injury is often based on history, assessment of the persons loss of consciousness, a detailed neurological exam and imaging studies.
Neuropsychological testing is the most sensitive means of identifying dementia in persons with a head injury. Its carried out by a specialist trained in clinical psychology and uses clinical rating scales to identify subtle cognitive issues. This testing also establishes clear baselines for measuring changes over time.
Head injury warrants a brain scan to determine whether any brain structures show physical abnormalities:
- CT scan is the standard test for a person with a head injury. A scan performed one to three months after injury may detect damage not visible immediately after the injury.
- MRI is more sensitive than CT scans in demonstrating certain types of injury.
- Single Photon Emission Computed Tomography scan is a relatively new imaging method that is still being studied in people with head injuries. It may be better than CT scans or MRIs in detecting functional problems in the brain for some types of dementia or other brain disorders. SPECT is available only at some large medical centres.
- Electroencephalogram measures the electrical activity of the brain. It may be used to diagnose seizures or abnormally slow rates of brain activity.
Are There Home Remedies For Stroke
A person with vascular dementia should be under medical care. There are steps you can take, however, to reduce your risk of further vascular damage or stroke. The most important thing you can do is adopt healthy habits. You should maintain a healthy weight, eat a balanced and healthy diet, exercise regularly, and not smoke.
You must develop a realistic attitude toward your limitations. You may require assistance with some everyday tasks, such as managing your finances. You may have to give up some of your independence . Your safety, and the safety of others, depends on it.
Many people with vascular dementia are eventually unable to live independently and care for themselves. Often, family members become responsible for their care. Your health care provider can discuss with you and your family how you should plan for future care.
Tips for the caregiver
Caregiving is best when it is structured, respectful, and friendly. This type of caregiving is the best way to approach the person’s behavioral problems.
You May Like: Bobby Knight Health
Research Into The Cause Of Vascular Dementia
Vascular dementia is the second most commonly diagnosed type of dementia, and may account for 15 â 20% of all cases. Vascular dementia is caused by chronic reduced blood flow to the brain, usually as a result of a stroke or series of strokes. It can often coexist with Alzheimerâs disease.
Stroke, small vessel disease, or a mixture of the two can cause vascular dementia. Most commonly there is a blockage of small blood vessels somewhere in the network of arteries that feeds the brain. Blockages may be caused by plaque build up on the inside of the artery wall, or by blood clots which have broken loose. Clots can form as a result of abnormal heart rhythms, or other heart abnormalities. Also, a weak patch on an artery wall can balloon outward and form an aneurysm, which can burst and deprive brain cells of oxygen.
It is estimated that about 50% of cases of vascular dementia result from high blood pressure, which can lead to a major stroke or a series of strokes and a build up of brain damage over time. Less common causes of vascular dementia are associated with autoimmune inflammatory diseases of the arteries such as lupus and temporal arteritis, which are treatable with drugs that suppress the immune system.
An inherited form of vascular dementia known as CADASIL is caused by a mutation on the Notch3 gene. This is a very rare form of dementia and only affects families carrying the Notch3 gene mutation.
You May Like: Taking Aricept Without Alzheimerâs
What Can I Expect If I Have Been Diagnosed With Vascular Dementia
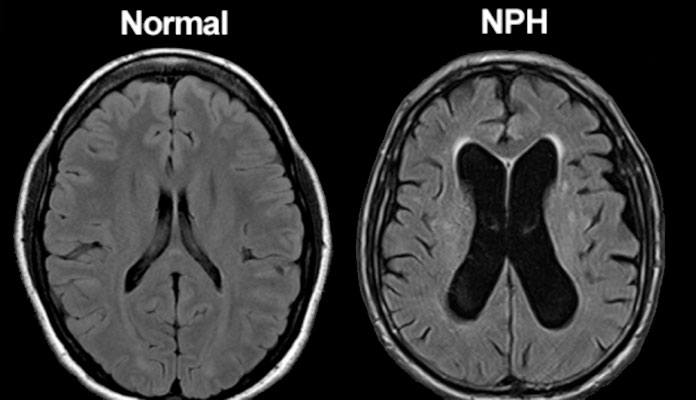
Vascular dementia may get worse over time. The changes can happen in sudden steps or gradually. Each person has their own unique journey. Generally, people with vascular dementia have a shorter life expectancy due to increased risk for additional stroke or heart attack. Treatments may help slow the progress of the disease. You and your healthcare provider will work together to develop a treatment plan best suited for managing your symptoms and stage of disease.
Also Check: Diet Soda And Alzheimer’s
Dementia Risk Is Higher In Those With Tbi History
The experts in the study concluded that the overall dementia risk in people with a history of TBI was 24% higher than those who did not have a history of traumatic brain injury.
They reached this conclusion after accounting for other risk factors of the neurodegenerative disease.
Severe traumatic brain injuries accounted for an increased risk of 35% while mild TBI increased the risk by 17%.
Men also have a slightly higher increased risk of dementia development when compared to women with traumatic brain injury histories at 30% versus 19%.
Jesse Fann the lead author of the study and a professor of behavioral sciences and psychiatry at the University of Washington School of medicine said that the relationship between the risk of dementia and the number of brain injuries was very clear according to the research.
Men are more likely to develop dementia after TBI
The study also indicated that the risk of dementia also increased based on the number of traumatic brain injuries.
Five or more TBIs increased the risk by 183%, four TBIs increased dementia risk by 51%, while the risk increased by 33% for two or three TBIs.
Fann also explained that if someone had a brain injury in their 20s chances of developing dementia increased by 60% in their 50s.
The researchers nonetheless clarified that the findings of the study do not suggest that everyone who sustains traumatic brain injury will end up developing dementia in his or her later years.
What Are The Symptoms Of Vascular Dementia
The symptoms of vascular dementia depend on the location and amount of brain tissue involved. Vascular dementia symptoms may appear suddenly after a stroke, or gradually over time. Symptoms may get worse after another stroke, a heart attack, or major surgery. These are signs and symptoms of vascular dementia
- Increased trouble carrying out normal daily activities because of problems with concentration, communication, or inability to carry out instructions
- Memory problems, although short-term memory may not be affected
- Confusion, which may increase at night
- Stroke symptoms, such as sudden weakness and trouble with speech
- Personality changes
- Mood changes, such as depression or irritability
- Stride changes when walking too fast, shuffling steps
- Problems with movement and/or balance
- Urinary problems, such as urgency or incontinence
- Tremors
Read Also: Farts And Dementia
Type Of Incident Stroke And Dementia Risk
During median follow-up of five years , 5,952 ischemic stroke survivors received a dementia diagnosis. During the same median follow-up , 1,540 ICH survivors received a dementia diagnosis. During median follow-up of 10 years , 565 SAH survivors received this diagnosis. The 30-year risk of dementia was 11.8% after ischemic stroke, 13.3% after ICH, and 11.6% after SAH. The 10-year risk was 7.65% after ischemic stroke, 8.89% after ICH and, reflecting the younger age distribution, 3.70% after SAH. The median age at dementia diagnosis was 81 years for ischemic stroke, 79 years for ICH, and 74 years for SAH.
Hemorrhagic stroke survivors had higher relative risks of dementia than ischemic stroke survivors. The unadjusted HRs were 1.72 after ischemic stroke, 2.70 after ICH, and 2.74 after SAH. The pattern of HRs by stroke type did not change during follow-up. However, for all three stroke types, the relative risk was higher during the first year after diagnosis, particularly among SAH survivors . After the first year, the increased risk of dementia persisted for all types of stroke, but at a lower level . The risks for ischemic stroke survivors were about 60% to 64% higher relative to the comparison cohort, whereas risks were about 2.1 to 2.6 times higher for survivors of ICH and SAH than for the comparison cohort .
Same Symptoms Different Disease
Exhibiting symptoms of dementia does not necessarily indicate dementiaââ¬âit could be another kind of brain condition, such as brain tumors and SDHs.
The loss of cognitive ability and difficulty with memory retention and recall are always causes for concern. It is important to fully understand which condition is causing these symptoms, because dementia is not always the source.
0651
Also Check: Does Alzheimer’s Cause Dementia
New Cause Of Brain Bleeds Identified
- Date:
- University of California – Irvine
- Summary:
- Neurologists have provided, for the first time, evidence that blood deposits in the brain may not require a blood vessel tear. The researchers found that brain endothelial cells, the cells that line blood vessels of the brain, have the capacity for engulfing red blood cells and depositing them outside the blood vessels and into the substance of the brain, without requiring a disruption of the vasculature.
A team of researchers including UCI project scientist Rachita Sumbria, PhD and UCI neurologist Mark J. Fisher, MD have provided, for the first time, evidence that blood deposits in the brain may not require a blood vessel tear. The researchers found that brain endothelial cells, the cells that line blood vessels of the brain, have the capacity for engulfing red blood cells and depositing them outside the blood vessels and into the substance of the brain, without requiring a disruption of the vasculature.
“It has long been believed that a tear or rupture of a brain blood vessel is the cause of cerebral microbleeds,” said Fisher, a professor of neurology at the UCI School of Medicine. “While more confirmatory work needs to be done, our study points to an entirely new direction in efforts to eliminate brain bleeding and its consequences.”
Story Source:
What Does The Research Say About High Blood Pressure And Dementia
According to the World Alzheimer Report 2014, multiple studies following large groups of people for 15-40 years have demonstrated that individuals who had high blood pressure in mid-life were more likely to develop vascular dementia in later life. Vascular dementia is the second most common form of dementia after Alzheimer’s disease. It is caused by reduced blood flow to the brain, which starves brain cells of the oxygen and nutrients they need to function correctly. The association between high blood pressure and Alzheimer’s disease is currently unclear.
However, despite this apparent link between vascular dementia and high blood pressure, the results from randomised controlled trials into whether lowering blood pressure can prevent dementia have so far been inconclusive.
This research demonstrates the importance of conducting studies that follow individuals over a long period of time , to connect a person’s lifestyle choices and health profile throughout their life to the risk of disease development in later life.
Recommended Reading: How To Stop Alzheimer’s Patient From Picking Skin
Dementia & Alzheimer’s Disease
The potential between increased risk of dementia and traumatic brain injury has become a pressing issue as scientists try to find the link between the two.
This is mostly because the immediate effects of head injury can include symptoms that are similar to those of dementia.
These include signs such as memory loss, confusion, and changes in speech, personality, and vision.
Best Advice For Atrial Fibrillation Patients
Bunch can’t yet say if the findings about dementia protection apply to the newer generation anticoagulants, the alternatives to warfarin. His team only studied warfarin.
“We don’t quite know if the will be translatable,” Bunch says. The newer anticoagulants include dabigatran , rivaroxaban and apixaban . One of their major selling points is the lack of a need for blood testing, although the ideal monitoring schedule is under some debate.
“The novel agents do not require frequent monitoring,” Bunch says. “There is not a blood test that is commercially available that measures their effectiveness in the blood.” He typically monitors kidney function with a blood test twice a year in his patients taking these newer drugs. “We do this because the drug elimination is greatly influenced by changes in kidney function, and if we see a decline, we lower the dose.”
The newer anticoagulants are safer in regards to bleeds in the brain, Bunch says, and all lower stroke risk. In general, patients find it easier to maintain target blood levels on the newer drugs, he says.
Until more research is in, you can take steps to improve your health, no matter which drug you are taking for atrial fibrillation, Bunch says. His tips:
Read Also: Alzheimer’s Dementia Definition