D Physical Examination Findings
-
Thickened and tender temporal arterial branches. On physical examination, involved vessels are nodular and tender, pulses are reduced or absent.
-
Cranial nerve involvement: ranges from vision loss/amaurosis fugax to diplopia and pupillary defects. Loss of vision is usually sudden,painless and permanent.On ophtlamologic examination, anterior ischemic optic neuropathy is recognized by optic disc edema followed by optic atrophy, with optic disc cupping.
-
Intermittent claudication of the masseter and temporalis muscles caused by compromised blood flow in the extracranial branches of the carotid artery.
Headache Occurs In 70% To 80% Of People With Giant Cell Arteritis
Britany Klenofsky, MD and Huma U. Sheikh, MD
Giant cell arteritis , commonly referred to as temporal arteritis, is a chronic, idiopathic granulomatous vasculitis of medium- to large-sized vessels.1,2 Initially GCA was considered a vasculitis affecting the carotid and vertebral artery branches only but was later redefined to include all medium and large vessels when autopsies showed involvement of large vessels in 80% of cases.1,3 In countries where GCA is known to occur, it is the most frequent primary vasculitis and may be a medical emergency in some individuals.4
A History Part I: Pattern Recognition:
The diagnostic category of GCA encompasses multiple variants , but there are four predominant clinical scenarios:
Cranial arteritis
-
visual loss is due to ischemia of the optic nerve or its tracts
-
claudication of jaw or tongue
-
stroke or CNS ischemia
-
pain in shoulder and pelvic girdle muscles
-
stiffness
-
depression
You May Like: Difference Between Senility And Dementia
What Causes Giant Cell Arteritis
Doctors dont know the exact cause of giant cell arteritis, but they think aging has something to do with the diseases onset and progression. In all cases of giant cell arteritis, an unknown trigger causes the immune system to attack and inflame the arteries. Certain genetic factors and environmental conditions can increase your risk of developing giant cell arteritis, but there are no known, widespread triggers.
Interestingly, Caucasian women over the age of 50 are at the highest risk of developing the condition. If you fit into this category and are experiencing giant cell arteritis symptoms, contact your doctor.
Why Is Temporal Arteritis More Common In Minnesota
People with a northern European background show a higher risk of developing temporal arteritis. The exact reason is not clear.
One study into rates of temporal arteritis in the United States looked at where the population is largely made up of that ethnic background: Minnesota.
Studying Olmsted County in particular, the researchers found that the rate here was as high as in Sweden, a country with one of the highest rates of temporal arteritis.
Over a 50-year period, the study found that there were almost 20 cases for every 100,000 in people across that time. In the Mediterranean region, the number of cases is low. In northern Italy, where temporal arteritis is at its lowest, there are 6.9 cases for every 100,000 people.
The authors wrote that the north-south divide could be due to environmental, genetic or ethnic factors.
However, average rates of temporal arteritis in the population overall are relatively low, although they are more common in older people.
You May Like: How Quickly Does Alzheimer’s Progress
What Are The Symptoms Of Giant Cell Arteritis
The symptoms of giant cell arteritis change over time, but the condition most often begins with a persistent headache, typically around the temples. People with giant cell arteritis can then develop fatigue, loss of appetite, a flu-like feeling, and weight loss. As the condition progresses, you may experience jaw pain, tongue and throat pain, and double vision. In the most severe cases, permanent blindness can occur.
Youll notice that these symptoms are also characteristic of other conditions, which makes giant cell arteritis notoriously difficult to catch. If you are worried about any possible symptoms, the best thing to do is to visit a doctor.
Pain and stiffness experienced in the neck, hips, and/or shoulders may also be associated with polymyalgia rheumatica, a related disorder. Close to 50 percent of people diagnosed with giant cell arteritis also have polymyalgia rheumatica, so it is important to communicate any symptom overlap to your doctor.
Who Gets Giant Cell Arteritis
GCA is a disease of older people. The average age at onset is 72, and almost all people with the disease are over the age of 50. Women are afflicted with the disease 2 to 3 times more commonly than men. The disease can occur in every racial group but is most common in people of Scandinavian descent.
You May Like: Smelling Farts Prevent Cancer
Timing Of Death After Diagnosis
The first study to compare the survival of GCA patients to that of matched controls was published in 2009 . The authors found an excess mortality in GCA patients at 5years after GCA diagnosis, but also that the survival rates for cases and controls converged after approximately 11years. Some other studies have reported similar findings . Baslund et al. analyzed death and causes of death in three time periods: 02, 210 and > 10years after GCA diagnosis . They argued that this subdivision reflects the clinical course of GCA, usually remitting within 624months of disease onset but with a possibility of late involvement of the large vessels. Baslund and colleagues found an increased risk of death due to circulatory diseases during 02years and > 10years after the diagnosis of GCA. Increased vascular risk associated with GCA has also been reported by others and includes cardiovascular disease, thromboembolic disease, and LV complications . However, the underlying mechanisms of all the vascular risks are not entirely understood and may encompass both disease-related and treatment-related causes . The possibility of incomplete capture of deaths due to late vascular complications is a limitation of every study with a short follow-up period. In contrast, the very long follow-up period in our study reduces the risk of missing late-occurring complications and diminishes the risk of an erroneous conclusion based on variations through time.
Historical Note And Terminology
Vasculitis rarely affects the central nervous system, as opposed to other organ systems and the peripheral nervous system, because it is an immunologically privileged site. Many arteritides can affect the CNS and ultimately progress to dementia, but the primary presentation of vasculitis as dementia is extremely rare. Dementia usually occurs late in the course of the disease and is preceded by a history of stroke attributable either to the vasculitis directly, to abnormal coagulation, or to cardiac embolism. Other vasculitides may cause a rapid decline in cognition and memory in the presence of altered consciousness these conditions cannot be said, by definition, to cause dementia. This review does not discuss these and refers only to those conditions wherein the primary presentation may be dementia. Conditions in which dementia or cognitive impairment may occur but in which dementia has not been reported as the primary presenting feature, conditions in which the dementia is preceded by stroke, and conditions that cause an encephalopathic syndrome rather than a dementia are not discussed.
You May Like: Alzheimer’s Ribbon Color
Myth : Dementia Is A Normal Part Of Aging
While your risk of developing dementia and Alzheimers increases as you age, dementia is not an inevitable part of the aging process. The World Health Organization estimates that 5% to 8% of people older than 60 have dementia. That number increases to at least 40% for people older than 80.
And while our countrys population is aging, a 2016 study published in the New England Journal of Medicine showed the incidence of Alzheimers has actually decreased over the past 30 years. The authors couldnt completely explain the decrease but did find that risk reduction was observed only in people who had at least a high school diploma. They also noted a few trends, particularly a decrease in the risk of dementia associated with stroke, atrial fibrillation, and heart failure.
In Medical Terms By David Hellmann Md
A discussion of Giant Cell Arteritis written in medical terms by David Hellmann, M.D. , Co-Director of the Johns Hopkins Vasculitis Center, for the Rheumatology Section of the Medical Knowledge Self-Assessment Program published and copyrighted by the American College of Physicians . The American College of Physicians has given us permission to make this information available to patients contacting our Website.
Giant cell arteritis is vasculitis of unknown cause that affects the elderly and is characterized by panarteritis of medium- to large-sized arteries, especially in the extracranial branches of the carotid artery. The average age of onset is 72 years, and women are affected two times as often as men. Irreversible blindness, the most commonly feared complication, results from necrosis of the posterior ciliary branch of the ophthalmic artery and is usually preventable by early diagnosis and corticosteroid treatment.
You May Like: What Color Is The Dementia Ribbon
How Is Giant Cell Arteritis Diagnosed
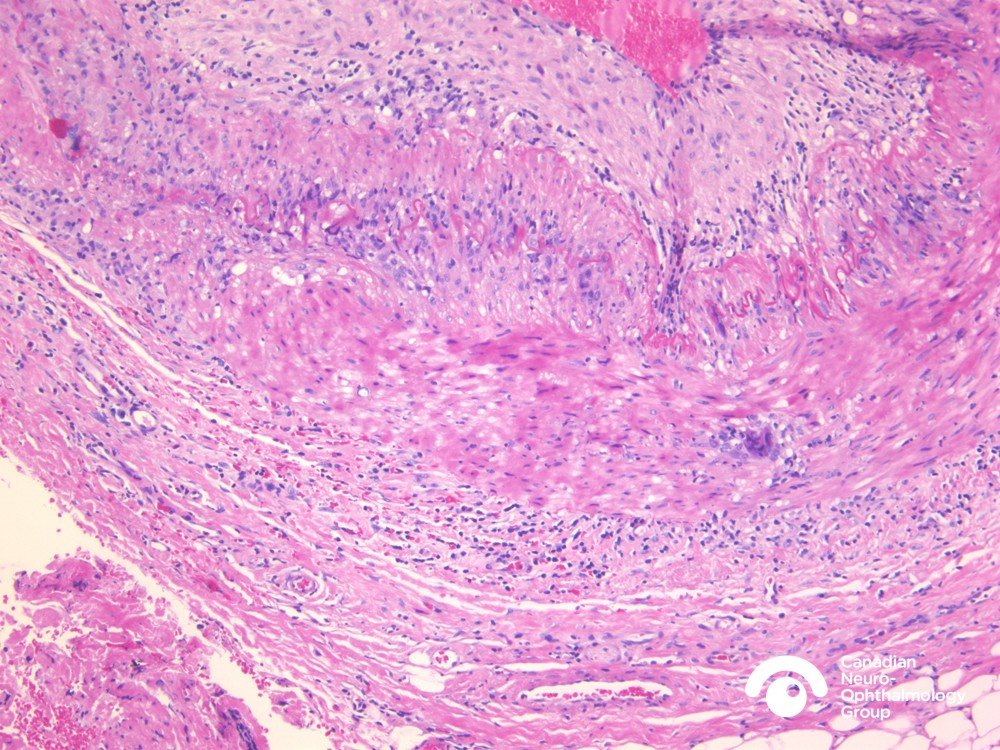
The diagnosis is made by doing a biopsy of the temporal artery. Using a local numbing medication , the doctor can remove a small part of the temporal artery from under the scalp and look at it under the microscope for evidence of inflammation. A temporal artery biopsy is almost always safe, causes very little pain, and often leaves little or no scar. An example of this is pictured below
There are blood tests that help the doctor decide who is likely to have GCA. Almost everyone with the condition has an elevated erythrocyte sedimentation rate . The sed rate measures how fast a patients red blood cells settle when placed in a small tube. In inflammatory conditions, red blood cells settle more quickly than in noninflammatory states. In addition, most patients with GCA have a slightanemia, or low red blood cell count. Other conditions can also cause a high sed rate or anemia, so the final diagnosis depends on a temporal artery biopsy.
A few patients with GCA do not have positive biopsies. We now know that GCA does not affect every part of every temporal artery but can skip around. When one biopsy is negative, biopsying the temporal artery on the other side can lead to the diagnosis.
Alzheimers Disease And Dementia: Sorting Myths From Reality
There are many misconceptions about dementia and Alzheimers disease. Some people may think these terms are interchangeable, but they aren’t.
Learning about the conditions their differences and similarities can empower patients, families, and caregivers to make more confident healthcare decisions.
Dementia is an umbrella term for a group of brain disorders that affect memory, decision-making, and behavior. Alzheimers disease is the most common type of dementia, accounting for 60% to 80% of cases. It is thought to be caused by beta-amyloid proteins that clump together and build up in the brain, and neurofibrillary tangles, which are accumulations of tau protein, damaging or destroying nerve cells.
The second most common form of dementia is vascular dementia. This can be caused by damage to blood vessels or blockages that lead to strokes or bleeds within the brain. There are many other types of dementia. Lewy body dementia, caused by abnormal deposits of protein in the brain, is another common form.
“I look forward to a day when we can prevent dementia, instead of treating it after the fact.”
Tara Duval, M.D.
All dementias regardless of the underlying cause have one thing in common. They all result in cognitive decline that ultimately impairs ones function and ability to carry out normal daily activities.
Recommended Reading: Dementia Anger Paranoia
Diagnosis And Diagnostic Testing
The diagnosis of GCA is made based on history or clinically. There should be a high degree of suspicion in individuals who are more than age 50 and presenting with headache, especially new-onset headache or with visual changes, fevers, jaw claudication, and/or muscle aches. A delay in diagnosis can lead to significant morbidity. Definitive diagnosis of GCA is made with histopathologic analysis of a temporal artery biopsy.7
Diagnostic Testing
Blood Tests. The most widely used blood tests to help make the diagnosis are the ESR and CRP, both of which are markers of inflammation, which is typically elevated in arteritis. However, neither is specific to GCA, and both can be elevated with age.13 Typically, the combination of ESR and CRP is used together to help make the diagnosis. In some cases, ESR can be normal or only slightly elevated, but this should not exclude the diagnosis, because the risk of vision loss is similar.14
Angiography with MRI and contrast can be used as well. Expected changes with GCA include mural edema. Similar to CDUS, the sensitivity decreases with corticosteroid treatment. A meta-analysis showed approximately 73% sensitivity and 88% specificity for GCA.7 Other imaging modalities, include fluorodeoxyglucose positron emission tomography/CT, although this also decreases in sensitivity with steroid treatment and the sensitivity and specificity is lower than biopsy.7
Classic Symptoms Of Giant Cell Arteritis
The most common symptoms of GCA are headache, pain in the shoulders and hips , pain in the jaw after chewing , fever, and blurred vision. Other symptoms can include tenderness of scalp , cough, throat pain, tongue pain, weight loss, depression, stroke, or pain in the arms during exercise. Some patients have many of these symptoms others have only a few. Blindness the most feared complication can develop if the disease is not treated in a timely fashion.
Also Check: Purple Ribbon Alzheimer’s
E What Diagnostic Tests Should Be Performed
The gold standard for diagnosing giant cell arteritis is a temporal artery biopsy. If there is a clinical suspicion of giant cell arteritis , a temporal artery biopsy should be performed, generally on an outpatient basis, by a vascular surgeon, an ophthalmologist, general surgeon or other surgical subspecialist.
The biopsy should be performed on the same side as the symptoms or abnormal findings on physical exam. Patients who manifest only symptoms of polymyalgia rheumatica do not require biopsy. However, these patients should be questioned carefully about headache, jaw or arm claudication, visual symptoms, and any pain in the face, throat or tongue, suggestive of giant cell arteritis.
If one temporal artery is abnormal on clinical exam , then the biopsy should be taken from that artery. However, when the extracranial arteries are not obviously abnormal, it is important to biopsy a longer segment of the temporal artery,to increase the chance of arterial specimens showing inflammatory changes. The rate of false-negative biopsies can be minimized by taking a sufficient length of biopsy, examining serial sections and removing the contralateral temporal artery in cases in which the first biopsy is free of disease.
Statistical models have been used successfully in predicting a negative temporal artery biopsy. The following combination of findings correlated with a 95 percent probability of a negative temporal artery biopsy:
I What Every Physician Needs To Know
Giant cell arteritis , also known as temporal arteritis, is a chronic vasculitis of large and medium sized vessel that should be considered in individuals older than 50 who present with new onset of headache, visual dysfunction, polymyalgia rheumatica or systemic inflammatory symptoms.
Giant cell arteritis is commonly associated with cranial symptoms and acute phase inflammatory response, but large vessel involvement is frequent and can lead to severe complications such as visual loss, stroke, limb claudication or aortic aneurysm.
Don’t Miss: Does Neil Diamond Have Alzheimer’s
B Physical Examination Tips To Guide Management
Disease relapses can occur in up to 60% of patients during the course of treatment. GCA relapse should be suspected when patients experience return of symptoms from their original presentation, or new symptoms compatible with GCA or polymyalgia rheumatica occur. Symptoms of systemic inflammation are frequently seen with disease reactivation, but vascular complication are not usually noted.
Table 1 Vasculitic Conditions With Dementia Or Other Cognitive Impairment As The Presenting Feature
|
Primary angiitis of the CNS Anticardiolipin antibodies Retinocochleocerebral vasculopathy Sjögren syndrome Polyarteritis nodosa Behçet disease |
Stroke occurs in 3% to 15% of cases of systemic lupus erythematosus. This is usually due to cardiac embolism, rather than vasculitis, as a true cerebral vasculitis is rare in systemic lupus erythematosus . Dementia may rarely occur in systemic lupus erythematosus in such cases, dementia is invariably preceded by clinical and immunological manifestations of systemic lupus erythematosus, and in all but 1 reported case, a clear association with stroke is evident. Cognitive decline in systemic lupus erythematosus is much more common than frank dementia and affects a substantial minority of patients. It is typically of insidious onset and may have prominent effects on visuospatial and memory functions. It may resolve, and correlation with disease activity is poor. Much of the cognitive loss may be due to coexistent psychiatric illness. Antilymphocyte antibodies cross-reactive against neurons and anti-ribosomal antibodies may be part of the etiology.
Cerebral involvement in giant cell arteritis occurs in about 7% of cases , and when it occurs, it is usually encephalopathic or in association with infarcts.
Behçet disease may cause dementia in about 10% of those with neurologic involvement, but this invariably occurs in association with other neurologic deficits.
Read Also: Bob Knight Health Condition
What Is The Treatment For Giant Cell Arteritis
Like most autoimmune disorders, there is no cure for giant cell arteritis. Instead, temporal arteritis treatment focuses on symptom control and alleviation. Most strategies target damaged tissue and work to alleviate inflammation that hinders blood flow. The best treatment for giant cell arteritis includes glucocorticoids, like oral prednisone. For the majority of patients, this also includes using corticosteroids.
However, corticosteroids come with their own side effects. The drugs can increase a persons risk of developing osteoporosis, glaucoma, cataracts, and high blood pressure, and they may cause weight gain, increased bruising, increased blood sugar levels, and decreased immune system function. It is important to talk to your doctor about potential treatment options and how they may affect your body.
How Is Vasculitis Treated
Treatment for vasculitis is aimed at reducing inflammation, controlling the anti-inflammatory response, and suppressing the abnormal immune system activity.
Medications to treat vasculitis include:
- Corticosteroid drugs such as prednisone to reduce blood vessel inflammation
- Immunosuppressive drugs such as cyclosporine to suppress or weaken the immune system
- Monoclonal antibodies that attach to certain abnormally functioning immune cells and kill them
- Blood thinners and anti-clotting medications
- Immunoglobulin therapy involves intravenous injections of antibodies that are collected from a pool of healthy volunteers to lessen the infectious attack on the immune system
Other procedures to treat vasculitis include:
- Plasma exchange, or plasmapheresis, which involves taking blood out of the body and removing components in the bloods plasma that are thought to be harmful and then transfusing the blood plus replacement plasma back into the body
- Surgery to bypass blocked vessels or treat aneurysms
Don’t Miss: Alzheimer Ribbon