Differential Diagnosis Of The Older Patient With Psychotic Symptoms
A survey of clinicians experienced in managing LBD found a significant preference for quetiapine and trial data suggests that clozapine might be used for control of dementia symptoms such as hallucinations and delusions in the non-acute situation. If any antipsychotic is administered to a person with LBD it is suggested …
Difference between Dementia and Psychosis | Dementia vs Psychosis
WEDNESDAY, Feb. 14, 2018 — The “overmedication” of agitated dementia patients — with the use of powerful antipsychotic drugs — is an ongoing issue in U.S. health care. Now, British researchers say they may have found a medicine that helps ease those symptoms, but in a much safer way. The newer …
Phase Iii Trials For Experimental Dementia
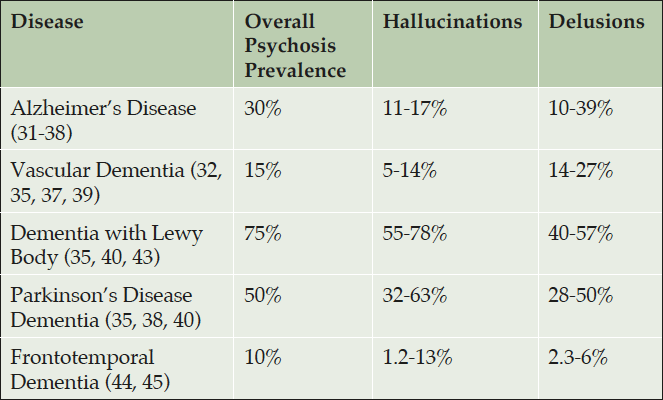
As many as half of the 45 million people worldwide who are living with Alzheimers will experience psychotic episodes, and that number is even higher among people living with some other forms of dementia. Psychosis is linked to a faster deterioration in dementia.
To date, there is no approved, safe, effective treatment for symptoms linked to dementia-related psychosis. Antipsychotics, while widely used , can lead to sedation, cause falls, and may double the speed at which brain function deteriorates. They have been linked to higher rates of hospitalization among people living with dementia, and when it comes to ICU delirium, they have been found to be ineffective. Patients, doctors and caregivers have long sought safer alternatives.
But there is growing optimism on the experimental drug front: The makers of a dementia symptoms treatment, pimavanserin, have reported a robust reduction in the severity of psychosis symptoms during a 12-week, open-label phase of a large-scale, international phase III relapse-prevention trial, according to a presentation at the Alzheimers Association International Conference this week. There, researchers from University of Exeter, in collaboration with ACADIA Pharmaceuticals, reported that the drug substantially reduced psychotic symptoms as well as reducing risk of relapse of those symptoms, compared to placebo in people with dementia.
Behavior Disorders Of Dementia: Recognition And Treatment
ABI V. RAYNER, M.D., M.P.H., JAMES G. OBRIEN, M.D., and BEN SCHOENBACHLER, M.D., University of Louisville School of Medicine, Louisville, Kentucky
Am Fam Physician. 2006 Feb 15 73:647-652.
Patient information: See related handout on dementia, written by the authors of this article.
Virtually all patients with dementia will develop changes in behavior and personality as the disease progresses.1 The nature and frequency of symptoms vary over the course of the illness, and psychotic features tend to present later, particularly when the patient becomes more dependent. Psychotic manifestations and other behavior problems may be more troubling and challenging than cognitive losses these features result in an increased burden for caregivers, earlier institutionalization, and an acceleration in cognitive decline.2
Psychotic features of dementia include hallucinations , delusions, and delusional misidentifications. Hallucinations are false sensory perceptions that are not simply distortions or misinterpretations. They usually are not frightening and therefore may not require treatment. Delusions are unshakable beliefs that are out of context with a persons social and cultural background. Delusional misidentification may result from a combined decline in visual function and cognition.2 For example, patients may suspect that their family members are impostors , believe that strangers are living in their home, or fail to recognize their own reflection in a mirror.
Recommended Reading: Dementia Vs Senility
Overview Of Potential Druggable Targets For Pharmacological Treatment Matching The Etiology Of Dementia
The etiology of dementia-related psychosis and agitation/aggression is very complex and is often a cluster of biological factors as well as psychological and social aspects . Alzheimers disease is the most common type of dementia, and the pathophysiology of this particular disease is related to the loss of neurons. Depending on the degree of neurodegeneration, the cerebral region involved, and consequently the extent of deficits in neurotransmitters, various psychiatric symptoms may appear . For instance, psychosis has been associated with neurodegeneration in the frontal and mesotemporal areas of the brain , while depression has been linked to the degeneration of brainstem aminergic nuclei and a decrease in serotonergic neurotransmission . Additionally, neuropathological changes that cause hypofunction of the cholinergic and serotonergic systems and hyperfunction of dopaminergic and noradrenergic transmission have been linked to agitation manifested by patients with dementia . Alterations in multiple neurotransmitter systems cause changes in the expression of specific receptors, which have a direct impact on the regular functioning of the central nervous system .
Dementia And Alzheimer’s Disease

Between May 2007 and April 2008, Dementia and Alzheimer’s together accounted for 28% of atypical antipsychotic use in patients aged 65 or older. The U.S. Food and Drug Administration requires that all atypical antipsychotics carry a black box warning that the medication has been associated with an increased risk of mortality in elderly patients. In 2005, the FDA issued an advisory warning of an increased risk of death when atypical antipsychotics are used in dementia. In the subsequent 5 years, the use of atypical antipsychotics to treat dementia decreased by nearly 50%.
You May Like: How Fast Can Alzheimer’s Progress
What Not To Do When Speaking With Someone With Psychotic Thoughts:
Overall What Is The Takeaway Is For The Physicians And Clinicians Who Are Treating These Patients
I think we’ve had a very good experience with pimavanserin in Parkinson disease psychosis, and this study is large enough to be reassuring across most of the other dementia groups. It’s going to depend on what the FDA decides. Does the FDA regard these data as sufficiently strong that it will be approved for a broader indication of dementia-related psychosis, or will additional work have to be done? That’s the information that we’re waiting on, for now, that would allow clinicians to decide how to use pimavanserin best.
Transcript edited for clarity.
Recommended Reading: Alzheimer’s Awareness Ribbon
Cholinesterase Inhibitors And Other Drugs
The new generation of cholinesterase inhibitor drugs were originally developed to improve memory and the ability to carry out day-to-day living activities in people with Alzheimers disease.
Evidence suggests that these drugs also have slight beneficial effects on behavioural symptoms, particularly apathy , mood and confidence, delusions and hallucinations. Taking cholinesterase inhibitor drugs may therefore reduce the need for other forms of medication. However, in higher doses these cholinesterase inhibitor drugs may occasionally increase agitation and produce insomnia with nightmares.
Memantine is the most recent antidementia drug to be developed. It works in a different way to the anticholinesterase drugs and is the first drug approved for those in the middle to later stages of Alzheimers disease.
There is some evidence that memantine has a positive effect on mood, behaviour and agitation.
Substance Abuse And Psychosis
Substance abuse because of loneliness or boredom or overuse of prescription drugs is a common problem in elderly patients. Consequently, acute and chronic substance abuse can be a factor in the development of psychosis in this population. Acute alcohol withdrawal can elicit delirium complete with vivid hallucinations and delusions.
Elderly patients may not report alcohol or substance abuse. A drug screen is useful when the etiology of psychotic symptoms is unknown, particularly if the patient’s medication use has not been supervised. The risk of seizures due to abrupt withdrawal must be considered when recent medication use is not completely known. It is also important to exclude thiamine deficiency in these patients who may have poor nutrition and may suffer from Korsakoff’s psychosis or Wernicke’s encephalopathy.
Read Also: Alzheimer’s Purple Ribbon
Side Effects Of Antipsychotic Drugs For Alzheimers / Dementia
This part is important. The side effects of antipsychotics are powerful, particularly in older people who are far-and-away the majority with Alzheimers and other dementias. One of the side effects, especially after taking the drugs for more than two weeks, is faster cognitive decline, meaning thinking and memory actually worsen.
Any prescription should include a pamphlet that lists the side effects. They vary depending on which specific medicine the doctor recommends, but will probably include most, if not all, of these: shakiness, involuntary movements of the mouth and jaw, lethargy , weight gain, constipation, dry mouth, and blurred vision.
Crucially for people with Alzheimers or related dementia, studies have found an increased likelihood of femur fractures. The combined side effects of sedation and shakiness mean an elderly person on antipsychotics can be prone to falling, and a bad fall can break the bone above the knee.
The potential for blood clots and stroke increases when a person is taking antipsychotics, and mortality rates on these drugs are increased almost double for users over 65.
Are Antipsychotic Drugs Justified For Alzheimers / Dementia
Studies have found antipsychotics should be considered as a last resort to temper abusive behavior in someone with Alzheimers or related dementia, but the drugs still have a role in treatment. Antipsychotics have been prescribed to address symptoms including those listed above and also inappropriate social behaviors, oppressive anxiety, and even physical motions that are repetitive and worrisome, like tremors or hand-kneading.
The most commonly prescribed antipsychotics for dementia behavior are aripiprazole , olanzapine , quetiapine and risperidone . The federal Food and Drug Administration has approved all these drugs for the treatment of mental health problems including schizophrenia, bipolar disorder, and severe depression. The FDA, importantly, has not officially approved these drugs for behaviors in patients with dementia. These drugs, the FDA has warned of antipsychotics, are not approved for the treatment of behavioural symptoms in elderly patients with dementia. The reasons for this warning are further explained below.
A last thing to consider is that studies comparing the effects of an antipsychotic to a placebo have found only marginal difference in elderly people with dementia. Only about half of people with dementia who take antipsychotics demonstrate any benefit, and, of those, the benefits may be marginal.
Read Also: Alzheimer Vs Dementia Vs Senility
A Word Of Encouragement:
When someone is psychotic we may have to shift how we measure improvement. The immediate goal may be the maintenance of a relationship, building trust, and having the opportunity to listen. If you have a relationship with the person you can watch for early warning signs of relapse or worsening of the current psychotic episode. You can keep an eye on medication compliance, side effects, and their physical health. You can also alert the treatment team to any concerning changes.
This website has a great toolkit for intervention with psychosis. It is full of helpful and supportive resources.
It can take a village to help someone in a psychotic episode. Be kind to yourself and give yourself space if you need it. Get support and see a therapist. See a psychiatrist for a consult about your loved one. The psychiatrist can help educate about symptoms and treatment options, brainstorm with you, and coach you about ways to handle situations.
Visit my Mental Health Bookstore for doctor recommended books about psychosis and schizophrenia.
Read here to learn more about 3 different types of paranoia.
Drugs For Treating Sleep Disturbance
Sleep disturbance, and in particular persistent wakefulness and night-time restlessness, can be distressing for the person with dementia and disturbing for carers. Many of the drugs commonly prescribed for people with dementia can cause excessive sedation during the day, leading to an inability to sleep at night. Increased stimulation and activity during the day can reduce the need for sleep-inducing medications at night. Hypnotics are generally more helpful in getting people off to sleep at bedtime than they are at keeping people asleep throughout the whole of the night. They are usually taken 30 minutes to one hour before going to bed.
Side-effects
If excessive sedation is given at bedtime, the person may be unable to wake to go to the toilet and incontinence may occur, sometimes for the first time. If the person does wake up during the night despite sedation, increased confusion and unsteadiness may occur.
Hypnotics are often best used intermittently, rather than regularly, when the carer and person with dementia feel that a good nights sleep is necessary for either or both of them. The use of such drugs should be regularly reviewed by the doctor.
Recommended Reading: Smelling Farts Might Prevent Cancer
What Kinds Of Questions Should You Ask Your Doctor About Any Drug Being Prescribed
- What are the potential benefits of taking this drug?
- How long before improvement may be noticed?
- What action should be taken if a dose is missed?
- What are the known side-effects?
- If there are side-effects, should the dosage be reduced or should the drug be stopped?
- If the drug is stopped suddenly, what happens?
- What drugs might interact with the medication?
- How might this drug affect other medical conditions?
- Are there any changes that should be reported immediately?
- How often will a visit to the doctor who prescribed the drug be needed?
- Is the drug available at a subsidised rate?
What To Do Instead:
Don’t Miss: Mri Alzheimer’s Vs Normal
Dementia & Psychosis Hallucinations Delusions
Up to one-third of all nursing home residents, primarily patients with dementia or agitation predisposes to worse long-term outcomes, including a …
Psychotic Symptoms in the Elderly – NCBI – NIH
This page includes the following topics and synonyms: dementia, Dementia with Comorbid Psychosis.
How to treat agitation and psychosis in dementia? – Cognitive …
New research involving King’s College London and the University of Exeter has highlighted the benefits of a promising new treatment which could relieve dementia related to Parkinson’s …
Cognitive Decline With Psychosis Can Deeply Upset And Burden Both The Patient And Caregiver
Dementia affects every aspect of life, including relationshipsso its no surprise that psychosis can be challenging and even emotionally painful for patients and their families to deal with. For patients, these symptoms impact their overall health and quality of life, such as their ability to sleep, participate in family and social life, and their emotional state, Dr. Foff says. In the beginning, hallucinations and delusions might be quite rare, but as the condition progresses, they may happen as often as every day.
Dealing with dementia can be isolating and distressing for caregivers. For Cynthia Kent, Dons wife, his condition has brought on feelings of loss. Theres a sadness that goes with losing your partner, she says. Not to mention, the financial burden is real. A study in Journal of the American Geriatrics Society found that total care costs for dementia patients can be hundreds of thousands of dollars and are more than twice as expensive as caring for seniors without dementia. Unfortunately, family members bear the brunt of those costs.
Recommended Reading: Life Expectancy Dementia Age 80
How Are Antipsychotic Drugs Reviewed
Antipsychotic drug treatments should be reviewed after six or 12 weeks, or both.
When the prescription of an antipsychotic is reviewed, the doctor may suggest stopping the drug in one go or a more gradual reduction known as tapering. In either case, the effects on the persons behavioural and psychological changes should be closely monitored. If they seem to be getting worse, it may be necessary to restart or increase the dose again.
If the person had a pre-existing mental health condition before they developed dementia and this was managed with antipsychotic drugs, they should continue to take them as prescribed by their psychiatrist.
Issues With The Use Of Antipsychotic Drugs
Antipsychotic drugs can cause serious side effects, and the risk increases with continued use over weeks and months.
Possible negative effects of antipsychotics include:
- drowsiness or confusion
- shaking, unsteadiness and reduced mobility
- worse than usual dementia symptoms, such as problems with thinking and memory
- higher risk of swelling around the lower limbs
- higher risk of infections
- higher risk of falls and fractures
- higher risk of blood clots
- higher risk of having a stroke
- higher risk of dying earlier than if they hadnt taken the drugs.
The decision to use antipsychotics should be taken very seriously. Benefits may sometimes come at the expense of the persons health and quality of life.
When considering prescribing an antipsychotic, the doctor will check if the person has high blood pressure, an irregular heartbeat, diabetes or a history of strokes. This is because these conditions carry additional risks for a person taking antipsychotic drugs.
There is evidence that some people with dementia who may not need antipsychotics are still being prescribed them. For example, they are being prescribed to treat distress or aggression before non-drug approaches have been tried thoroughly. Also, some people are kept on an antipsychotic for too long without a review at 12 weeks or a clear plan for when they should come off the drug.
Read Also: Alzheimer’s Purple Color Code