Clinical Diagnosis Of Mci And Mild Dementia
A medical history and a mental status examination are the principal tools for making a diagnosis of MCI or mild dementia. The medical history is the principal means by which the clinician establishes whether or not the patient has impairment in daily functioning. The mental status examination is the means by which the clinician establishes whether there is objective evidence of cognitive impairment. Clinical judgment is required to integrate information from the two sources. The general neurological examination should also be performed, but its role in the diagnostic process is largely in contributing to an understanding of the etiology of the cognitive disorder.
How Is Mild Cognitive Impairment Managed
There currently is no standard treatment or approved medication for MCI, but there are things a person can do that may help them stay healthy and deal with changes in their thinking.
Because MCI may be an early sign of more serious memory problems, it’s important to see a doctor or specialist every six to 12 months. A doctor can help track changes in memory and thinking skills over time. Keeping a record of any changes can also be helpful.
People with MCI might also consider participating in clinical trials or studies. Clinical trials are research studies that help test if a treatment, like a new drug, is safe and effective in people. People with and without memory problems can take part in clinical trials, which may help themselves, their families, or future generations.
To find out more about participating in clinical trials for people with memory problems and people without cognitive impairment, visit Alzheimers.gov or call the Alzheimers and related Dementias Education and Referral Center toll-free at 1-800-438-4380.
Facts About Mild Cognitive Impairment
Mild cognitive impairment is a condition that falls somewhere between normal age-related memory loss and Alzheimerâs disease or a similar impairment. Not everyone with MCI develops dementia. And like dementia, MCI is not an illness, but a cluster of symptoms that describes changes in how you think or process information. Memory problems are the most common indicators of MCI. A person with MCI may also experience difficulties with judgment, thinking, and language beyond what one might expect with normal aging. For unknown reasons, MCI appears to affect men more than women.
Family members and friends who notice these problems might not express concern because the early symptoms can mimic normal, age-related changes. People suffering from MCI often recognize they are having trouble but are still able to carry on most of their usual activities and live independently.
Don’t Miss: What Color Is The Dementia Ribbon
What Is Mild Cognitive Impairment
Some older adults have more memory or thinking problems than other adults their age. This condition is called mild cognitive impairment, or MCI.
There is no single cause of MCI. The risk of developing MCI increases as someone gets older. Conditions such as diabetes, depression, and stroke may increase a persons risk for MCI.
Memory Loss Related To Emotional Problems
Emotional problems, such as stress, anxiety, or depression, can make a person more forgetful and can be mistaken for dementia. For instance, someone who has recently retired or who is coping with the death of a spouse, relative, or friend may feel sad, lonely, worried, or bored. Trying to deal with these life changes leaves some people feeling confused or forgetful.
The confusion and forgetfulness caused by emotions usually are temporary and go away when the feelings fade. Emotional problems can be eased by supportive friends and family, but if these feelings last for more than 2 weeks, it is important to get help from a doctor or counselor. Treatment may include counseling, medication, or both. Being active and learning new skills can also help a person feel better and improve his or her memory.
Also Check: Shampoos That Cause Alzheimer’s Disease
Apathy: A More Important Indicator
The reported prevalence of apathy in MCI is between 10.7% and 44.8% . Studies report differences in apathy prevalence depending on MCI type: 6.9% in amnestic-MCI and 14.7% in multidomain-MCI . Apathy is defined as diminished motivation for at least 4 weeks and accompanied by any two of the following: reduced goal-directed behavior, reduced goal-directed cognitive activity, and reduced emotions . Apathy may be more likely to occur in those with frontal lobe deficits . Increased apathy is found to mediate the relationship between cognition and depression . Apathy is the most common and persistent neuropsychiatric symptom in AD patients, occurring in 55% of dementia patients , which is a prevalent neuropsychiatric manifestation in individuals with AD. It can exert a greater impact on daily functioning than depression, which increases reliance on caregivers .
Depression Anxiety And Apathy In Mild Cognitive Impairment: Current Perspectives
- Department of Geriatrics, Xuanwu Hospital, Capital Medical University, China National Clinical Research Center for Geriatric Medicine, Beijing, China
Objective: Mild cognitive impairment is an important risk state for dementia, particularly Alzheimers disease . Depression, anxiety, and apathy are commonly observed neuropsychiatric features in MCI, which have been linked to cognitive and functional decline in daily activities, as well as disease progression. Accordingly, the studys objective is to review the prevalence, neuropsychological characteristics, and conversion rates to dementia between MCI patients with and without depression, anxiety, and apathy.
Methods: A PubMed search and critical review were performed relating to studies of MCI, depression, anxiety, and apathy.
Results: MCI patients have a high prevalence of depression/anxiety/apathy furthermore, patients with MCI and concomitant depression/anxiety/apathy have more pronounced cognitive deficits and progress more often to dementia than MCI patients without depression/anxiety/apathy.
: Depression, anxiety, and apathy are common in MCI and represent possible risk factors for cognitive decline and progression to dementia. Further studies are needed to better understand the role and neurobiology of depression, anxiety, and apathy in MCI.
Don’t Miss: What Color Ribbon Is Alzheimer’s
Does Mild Cognitive Impairment Lead To Dementia
Researchers have found that more people with MCI than those without it go on to develop Alzheimer’s disease or a related dementia. An estimated 10 to 20% of people age 65 or older with MCI develop dementia over a one-year period. However, not everyone who has MCI develops dementia. In many cases, the symptoms of MCI may stay the same or even improve.
Research suggests that genetic factors may play a role in who will develop MCI, as they do in Alzheimer’s and related dementias. Studies are underway to learn why some people with MCI progress to Alzheimer’s and others do not.
Why Does Mild Cognitive Impairment Appear
The widening of the population pyramid in the oldest strata, favored in part by a longer life expectancy, is increasing the number of people affected by cognitive alterations and possible dementia syndromes. A fact of special interest, especially if we think that advanced age is a key risk factor for the development of this pathology.
Other sociodemographic studies have found a higher prevalence of this deterioration for the female population between 71-80 years of age. Especially accused in married women with a family and few years of schooling. Although this does not mean that there is a causal relationship between being a woman and having mild cognitive impairment, of course.
For the rest, the causes of this disorder remain unknown and an object of study for researchers, who today continue to work to shed light on the questions that still need to be answered.
Don’t Miss: Dementia Ribbon Colors
Very Early Signs And Symptoms
There are very early signs and symptoms of dementia, mild cognitive impairment, mild dementia, moderate dementia, and severe dementia. Biomarkers are indicators, such as changes in sensory abilities, or substances that appear in body fluids like blood, cerebrospinal fluid, or urine. Biomarkers can indicate exposure to a substance, the presence of a disease, or the progression of a disease over time. Such tools are critical to helping scientists detect and understand the very early signs and symptoms of dementia.
Anxiety: Another Important Symptom
Anxiety symptoms have been studied less than depression, and the relationship between anxiety and cognition is complex. The reported prevalence of anxiety in MCI patients ranged between 9.9%52% . A meta-analysis showed that the prevalence of anxiety in patients with MCI was 14.3% in community-wide samples and was 31.2% in clinic-based samples . Such inconsistencies in reported prevalence may be attributed to differences in recruitment strategies and methodology . There is a high rate of comorbid depressive disorders in MCI patients with anxiety, confirming a positive correlation between the two neuropsychiatric disturbances in both demented and non-demented older people . Anxiety symptoms have been found to have a strict interaction with executive functions in MCI, and thus they may be a marker of incipient cognitive decline in MCI .
Anticipatory anxiety is significantly associated with earlier conversion to AD, but this association does not remain significant following an adjustment for cognitive status at the baseline anxiety for upcoming events and purposeless activity frequently co-occur, which indicates anticipatory anxiety may be a marker of severity rather than an independent predictor of disease progression . Devier showed that different risk profiles have been described for state vs. trait anxiety: state anxiety was not a significant predictor of future conversion to AD, but higher trait anxiety predicted a lower risk of future conversion to AD .
Read Also: Purple Ribbon Alzheimer’s
How Mci Differs From Alzheimers
Symptoms of Alzheimers disease typically begin with MCI. MCI refers to relatively minor impairments in thought processes and memory, whereas Alzheimers is a specific disease in which memory and functioning continue to significantly decline over time.
Some researchers would like to identify MCI simply as a very early stage of Alzheimers, especially because studies have shown changes in the brains of people with MCI that are similar to those that are present in Alzheimers. However, since some people who are diagnosed with MCI don’t continue to decline or show other symptoms of dementia, this definition is unlikely.
How Is Mild Cognitive Impairment Diagnosed

Family and friends may notice memory lapses, and the person with MCI may worry about losing his or her memory. These worries may prompt the person to see a doctor about their memory problems.
In some cases, memory and thinking problems may be caused by conditions that are treatable. A doctor can perform tests and assessments to help understand whether the source of memory problems is something treatable or may be MCI. He or she also may suggest that the person see a specialist for more tests.
Read Also: Bob Knight Dementia
Whats The Difference Between Mild Cognitive Impairment And Decline Due To Normal Aging
Some gradual mental decline is seen with normal aging. For example, the ability to learn new information may be reduced, mental processing slows, speed of performance slows, and ability to become distracted increases. However, these declines due to normal aging do not affect overall functioning or ability to perform activities of daily living. Normal aging does not affect recognition, intelligence, or long-term memory.
In normal aging, a person may occasionally forget names and words and misplace things. With mild cognitive impairment, the person frequently forgets conversations and information that one would ordinarily remember such as appointments and other planned events.
What Are The Symptoms Of Mild Cognitive Impairment
The symptoms of MCI are not as severe as the symptoms of Alzheimer’s disease or dementia. For example, people with MCI do not experience the personality changes or other problems that are characteristic of Alzheimer’s. People with MCI are still able to take care of themselves and do their normal daily activities.
Signs of MCI may include:
- Losing things often
- Forgetting to go to events or appointments
- Having more trouble coming up with words than other people of the same age
Movement difficulties and problems with the sense of smell have also been linked to MCI.
You May Like: Dementia Vs Senility
Mci Patients Have Higher Rates Of Depression
Depressive symptoms were commonly associated with MCI, and anxiety-depression was found to be a significant risk factor . The reported prevalence of depression in MCI patients is sensitive to the criteria used to diagnose MCI and its subtypes . Subjects with MCI are more likely to develop depression compared with those with normal cognitive function, especially with those with amnestic MCI . However, some studies found that there is no difference in rates of depression between aMCI and non-aMCI groups . MCI patients with depressive symptoms showed more severe behavioral symptoms and verbally agitated behavior , and some studies reported an increased AD risk in MCI patients with depression , whereas other studies reported no effect .
What Causes Mild Cognitive Impairment
All possible causes of mild cognitive impairment have not been completely discovered. In a small number of cases, another condition may be causing the symptoms seen in mild cognitive impairment. Some of the possible conditions include:
- Depression, stress, and anxiety
- Diseases or conditions that affect blood flow in the brain
- Low vitamin B12 levels or other nutrient levels
- Eye or hearing problems
- An infection
- Side effects of certain prescription or illegal drugs
- History of alcoholism
Many of these causes of mild cognitive impairment are treatable.
Most cases of MCI, however, are due to a variety of diseases, such as Alzheimers or Parkinsons disease.
Also Check: Does Diet Coke Cause Alzheimer’s
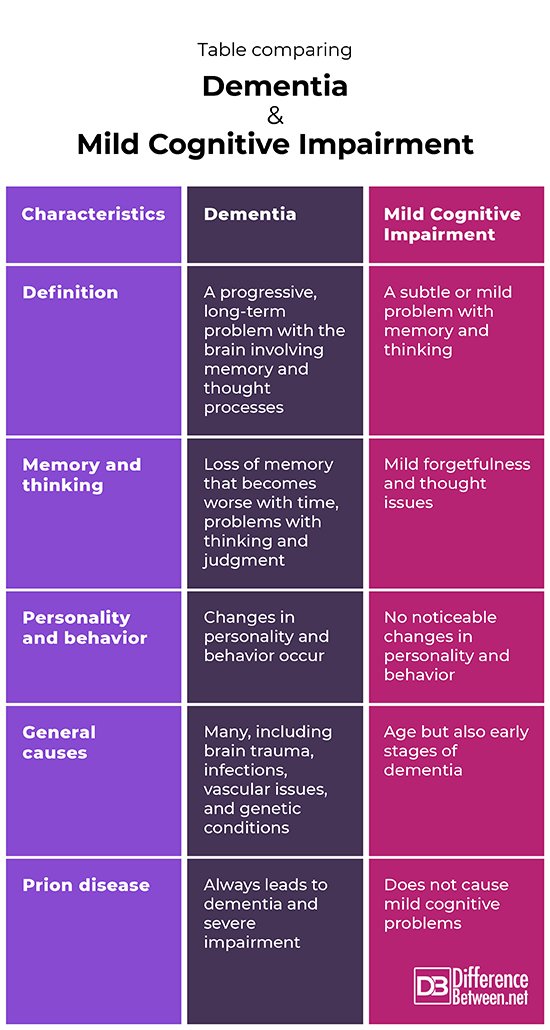
What Is The Difference Between Mci And Dementia
Both MCI and dementia are characterized by objective evidence of cognitive impairments. The main difference between mild cognitive impairment and dementia is that in the latter there is evident interference with daily life functioning.
Another big difference between MCI and dementia is simply that based on your testing, you fall into the range of the memory scores that we would consider not to be dementia.
Small Strokes Or Cerebrovascular Disease
Some strokes can be seen with brain imaging. Significant strokes are generally caught when a person is alive because they will have symptoms associated with them.
But you can observe so-called mini strokes under the microscope when you look at the brain following death. You may observe evidence that blood has leaked out from the blood vessels and into the brain tissue.
As with the abnormal clumps of proteins, the MCI group would fall in between a group of dementia patients and normal aging individuals with regards to these blood vessel changes.
The same group differences would apply to shrinkage of the hippocampus.
Also Check: Meredith Grey Alzheimer’s
Mild Cognitive Impairment Vs Dementia
Having short-term troubles with memory does not necessarily mean you are suffering from dementia. It takes at least two types of impairments that significantly disrupt your day to day activities to get you a diagnosis of dementia.
There is a possible connection between mild cognitive impairment and dementia. However, they are not same and affect people both similarly and differently. Mild cognitive impairment and dementia are not the same. Though persons suffering from mild cognitive impairment are at a greater risk of developing dementia, being affected by mild cognitive impairment does not necessarily mean that it will lead to dementia over time.
Mild cognitive impairment and dementia are not the same. In order to see the differences between the two conditions, let us first have a look at what both these conditions actually mean.
Roc Analysis Of Standard Screening Measures: A Comparison Of Cerad

The ROC curve analysis was used to evaluate the diagnostic accuracy of each measure to discriminate AD and MCI from each other and from healthy cognitive aging. Graphic representations of the ROC curves are provided in . shows clinically relevant cut-offs for the CERAD-NB, MMSE and MoCA. The diagnostic accuracies of the CERAD-NB, MMSE and MoCA were all excellent for HC vs. AD, with AUCs > 0.99. Diagnostic accuracies were lower, but still very good in the CERAD-NB , MMSE and MoCA for HC vs. MCI. The CERAD-NB resulted in a significantly higher AUC than either the MoCA or MMSE , and the MoCA was nominally better at differentiating HC from MCI than the MMSE . Diagnostic accuracies of all three cognitive measures were the lowest when differentiating AD from MCI, yet the AUCs were still good and equally high for the three measures: CERAD-NB , MMSE and MoCA .
ROC curve analysis of the MMSE, MoCA, CERAD-NB, and DSRS. HC=Healthy Controls AD=Alzheimers disease MCI= Mild Cognitive Impairment
Read Also: What Color Ribbon Is Alzheimer’s
Mci Patients With Depression Have Higher Conversion Rates To Dementia
However, there is research that demonstrated contrary conclusions. A 3-year prospective study of MCI outpatients demonstrated no increased risk of AD in patients with symptoms of depression . One study found a strong negative influence of depression on conversion to AD in MCI patients , while another study showed that depressive symptoms are not associated with the rate of progression to dementia in MCI patients and that gender moderated the association between depressive symptoms and conversion to dementia . Other studies found that the increased endorsement of memory problems is the only significant predictor of conversion to dementia, which likely represents insight into cognitive problems more than depressive symptomatology in MCI individuals . The different results about depression in MCI may be because studies did not account for length of depression, incident depression, if it was treated, etc., since depression is not a stable state and the clinical characteristics of the depression may play a role. One study found that persistent or incident depression worsens cognitive outcome while no or recovered depression does not affect it in early AD patients . Further studies on the type and clinical characteristics of depression in MCI patients are needed.
How Is Mci Diagnosed
Mild cognitive impairment is primarily identified in people who already have concerns about their cognition but, when tested, they dont quite rise to the clinical definition of dementia. Their memory or thinking abilities have declined over time but this does not impact their day-to-day activities.
This cognitive impairment is assessed through the use of standardized memory and thinking tests administered by a health care professional.
When doctors assess a persons mental performance, an MCI patients score may show a mild level of impairment for their age and education level. Medical professionals use tests such as the Mini-Mental State Examination or the Montreal Cognitive Assessment to do these evaluations.
The results for a person with MCI are typically not significant enough to be labeled dementia. It is important to note that a diagnosis of MCI typically requires significant clinical judgment by your doctor and this could include multiple tests of your memory and cognition, images of your brain, and blood tests.
Recommended Reading: Does Prevagen Work For Dementia