Study Design And Population
Participants were members of the Dunedin Multidisciplinary Health and Development Study, a longitudinal investigation of health and behaviour in a population representative birth cohort. The full cohort comprises all individuals born between April 1972 and March 1973 in Dunedin, New Zealand, who were eligible based on residence in the province and who participated in the first assessment at age 3years. The cohort represents the full range of socioeconomic status in the general population of South Island, New Zealand . The cohort matches the New Zealand National Health and Nutrition Survey on adult health indicators and the NZ census on educational attainment. The cohort is primarily white , which matches the demographics of the South Island . Assessments were carried out at birth and at ages 3, 5, 7, 9, 11, 13, 15, 18, 21, 26, 32, 38, and most recently 45years, when 94.1% of the 997 participants still alive took part. A total of 875 also completed MRI scanning. Scanned participants did not differ from other living participants on childhood social economic status or childhood intelligent quotient . The relevant ethics committees approved each phase of the study, and informed consent was obtained from all participants.
Is White Matter On Mri Normal
White matter hyperintensities are common in MRIs of asymptomatic people, and their prevalence rises with age, from about 10% to 20% in people around 60 years old to nearly 100% in people over 90 years old.
The Syndrome Of White Matter Dementia
Neurologists since at least the time of Jean-Martin Charcot in the 19th century have appreciated that cerebral white matter disease may produce important neurobehavioral sequelae, including dementia. In 1988, based largely on experience with toluene leukoencephalopathy and MS , the syndrome of WMD was proposed to describe the dementia.that can accompany cerebral white matter involvement. Implicit in the idea was that white matter disorders typically involve widespread areas of the brain, and the disruption of myelinated tracts affects cognition regardless of the specific neuropathology present. WMD is thus defined as a dementia syndrome resulting from diffuse or multifocal cerebral white matter damage .
Don’t Miss: How Can You Get Alzheimer’s
White Matter In The Brain
Think of the brain as a computer system, and it might be easier to understand. According to the UC Davis Health System, the gray matter of our brain is the computer and the white matter is the cables that connect everything together and transmit signals.
Want more of a biological explanation? White matter is tissue in the brain composed of nerve fibers. The fibers connect nerve cells and are covered by myelin . The myelin is what gives white matter its white color.
Myelin speeds up the signals between the cells, enabling the brain cells to quickly send and receive messages. It also provides insulation for the fibers, preventing the brain from short-circuiting.
White matter makes up about half of the brain, with gray matter making up the other half.
How Is White Matter Disease Treated
Healthcare providers focus treatment for white matter disease on managing symptoms and the risk factors associated with cardiovascular disease.
Treating underlying health issues like high blood pressure, diabetes and high cholesterol as well as quitting smoking can help prevent more white matter lesions from forming.
While there are no treatments to repair white matter thats already been damaged, people with more uncontrolled health problems generally experience greater white matter damage and disability.
Treatment for white matter disease symptoms
Physical therapy may help with balance and walking problems caused by white matter disease, including education and therapy to prevent falls.
Seeing a psychologist to talk about problems with depressed mood and seeing a psychiatrist for medications like antidepressants can help with symptoms of depression.
There are several treatments for managing urinary incontinence, including medications, lifestyle changes and procedures.
Managing cardiovascular disease risk factors
Managing the risk factors associated with cardiovascular disease can help slow the progression of white matter disease and help prevent life-threatening cardiovascular conditions like strokes.
Treatments that can help manage cardiovascular disease risk factors include:
Recommended Reading: Does George Strait Have Dementia
Why Do Westudy It
A large number of peopleliving with dementia will have Alzheimers disease and white matter disease atthe same time. Understanding the white matter disease component of theirdementia might lead to improved or specific treatments. This is because white matterdisease is in part linked to common problems with the heart and blood vessels causedby smoking, diabetes, high blood pressure and high cholesterol. These arethings we can prevent or treat.
Histopathological Evidence Of White Matter Abnormalities
The neuroimaging studies establish that there is some degree of white matter abnormality in the context of AD, which may be radiological manifestations of more widespread white matter pathological abnormalities. White matter hyperintensities have been associated histopathologically with myelin pallor, myelin loss and the loss of myelinated axons, as well as changes in arterial adventitia in deep white matter . In our aim to review the widespread white matter abnormalities, we focus on the changes in the myelin sheath and oligodendrocyte lineage cells.
Fig. 1
This figure demonstrates examples of white matter myelin loss in brain sections from a patient with Alzheimers disease. Tissues from frontal and occipital areas are stained with Luxol fast blue-hematoxylin and eosin . b2 and b1 represent the regions with and without myelin pallor in the frontal area, respectively. d2 and d1 represent the regions with and without myelin pallor in the occipital area, respectively. The scale bars in images a, b, c and d are 1000 m. The scale bars in images b1, b2, d1 and d2 are 100 m
Recommended Reading: Why Do Dementia Patients Talk In Their Sleep
White Matter Disease Exacts Heavy Toll Increasing Risk Of Stroke Alzheimer’s Dementia
- Date:
- British Psychological Society
- Summary:
- More evidence has been accumulated that damage to cognitive areas is widespread from white matter disease. White matter disease is responsible for about a fifth of all strokes worldwide, more than doubles the future risk of stroke, and is a contributing factor in up to 45% of dementias. Unlike Alzheimer’s disease, which shrinks the hippocampus causing progressive memory loss, white matter disease is a more diffuse mind-robbing condition that targets small blood vessels deep within the brain’s white matter. The disease hardens the tiny arteries, gradually restricting nutrients to white matter — the connections between brain regions involved in executive abilities such as planning, organizing, problem-solving, and attention.
Researchers have found further troubling evidence that cognitive damage from white matter disease is more widespread than first thought. A comprehensive meta-analysis of twenty seven published studies comparing healthy older adults to those who have cognitive impairment due to white matter disease has revealed that the disease can sabotage several cognitive areas.
Led by the Rotman Research Institute at Baycrest Health Sciences in Toronto, in collaboration with the University of Toronto Scarborough, the findings are published online today in the British Journal of Neuropsychology, ahead of print publication.
Quick Stats
Story Source:
Physical Activity Level In People With Age Related White Matter Changes Correlates To Better Motor Performance Lower Comorbidity And Higher Cognitive Level
The authors look at the impact of physical activity and inflammation on grey matter volume and cognitive function in older people, as well as the impact of aerobic fitness on cerebral white matter integrity. Low-intensity daily walking activity is linked to hippocampal volume in older people.Fazekas F, Barkhof F, Wahlund LO, Pantoni L, Erkinjuntti T, Scheltens P, et al. CT and MRI assessment of white matter lesions. J Am Geriatr Soc. 2001 49:21u20137. The Association of Aging with White Matter Integrity and Functional Connectivity Hubs. Front Aging Neurosci. 2016 15:143.
Recommended Reading: How Many Types Of Dementia Are There Nhs
What Causes White Matter Disease
Researchers are still learning about white matter disease and its cause. So far, they think its caused by chronically reduced blood flow to nerve fibers in white matter, which can cause damage to the fibers.
With aging, your arteries become hard and have more difficulty stretching . This can lead to less blood flow to nerves in your brain, causing damage to your white matter.
White matter disease can also be caused by atherosclerosis, which is the thickening and hardening of the walls of your arteries that happens due to the buildup of plaque in your arteries over time. It can affect any arteries in your body, including ones in your brain.
Having cardiovascular risk factors, such as high blood pressure, elevated blood sugar , high dietary fat intake and smoking can all increase the number of white matter spots or lesions in your brain.
Other causes of white matter lesions
Any process leading to a change in the chemical composition of, damage to or decreased blood flow of myelinated fibers can present as white matter lesions on magnetic resonance imaging .
While white matter disease involves several white matter lesions caused by blood vessel issues, you could have small white matter lesions for other reasons. Lesions are common features of non-vascular conditions, including demyelinating inflammatory disorders, such as multiple sclerosis, and genetic causes like leukodystrophy.
How Is It Diagnosed
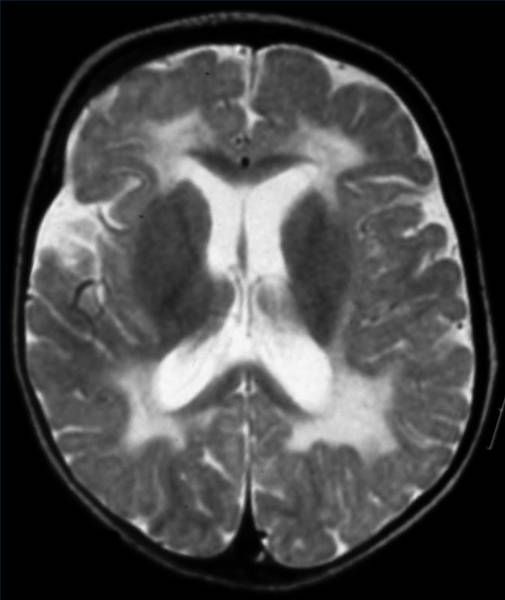
Advances in medical imaging have made white matter disease easier to spot. A magnetic resonance imaging test, which takes pictures of the inside of your brain, can show any damage. Changes to white matter will show up super-bright white on an MRI scan. You may need more tests to rule out other causes.
Don’t Miss: What Is Early Onset Dementia Called
Chronic Traumatic Encephalopathy/brain Injury
Initial symptoms: Symptoms of brain injury include loss of consciousness, memory loss, personality and behavior changes, and slow, slurred speech.
Progression: While symptoms from a single concussion are often temporary and resolve with appropriate treatment, chronic traumatic encephalopathy typically develops over time from repeated head injuries and is generally not reversible. Later symptoms include poor decision-making ability, aggression, impaired motor function and inability to communicate effectively.
Prognosis: Life expectancy varies according to the severity of injuries.
Association With Stroke Severity And Post
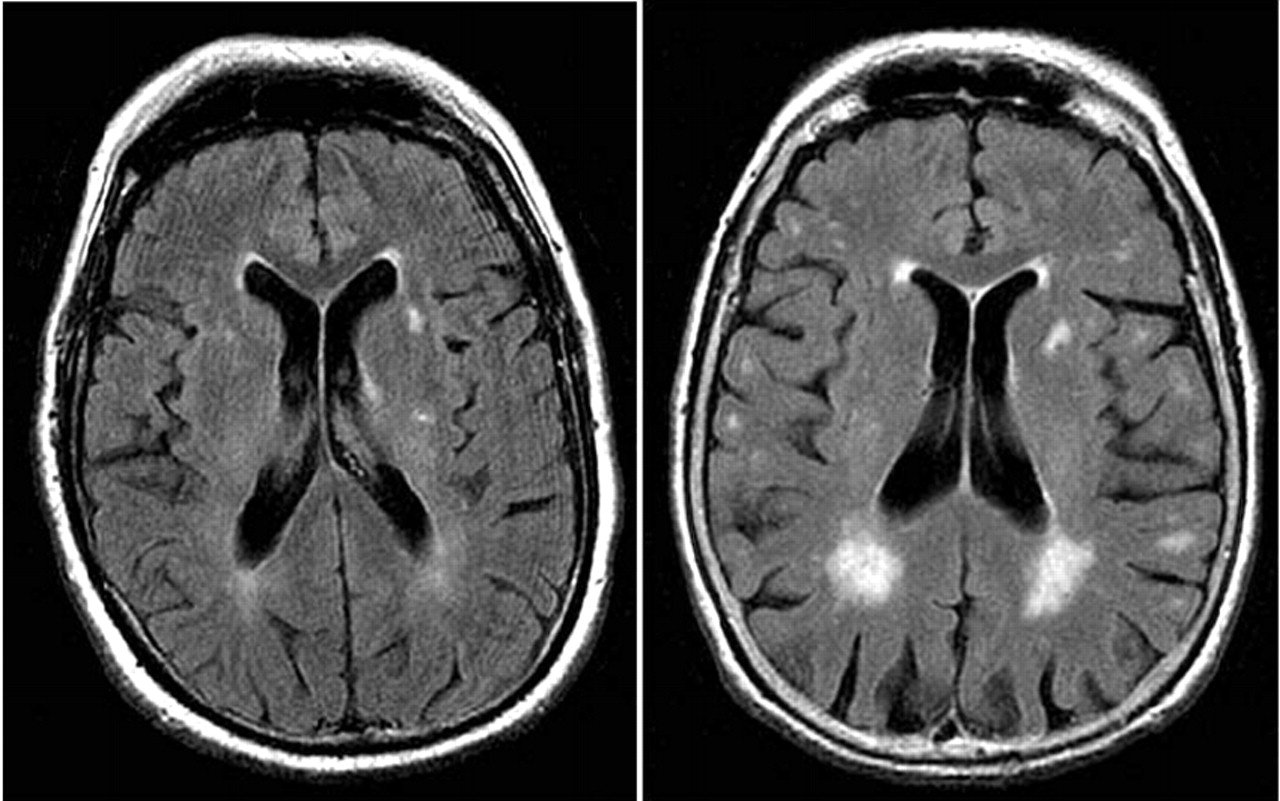
Severity of leukoaraiosis has been linked to poor functional post-stroke outcome in both short- and long-term follow-up studies. In patients with acute ischemic stroke, severity of WMH is significantly associated with poor functional outcome at 3 months and beyond. When the topography of WML is considered, PVH burden, but not subcortical or deep WMH, appears to be linked to unfavorable clinical outcome in both short- and long-term studies. A study in patients with spontaneous ICH also showed that higher leukoaraiosis burden was an independent marker of worse functional outcome. [38
Besides being a predictor of functional outcome after stroke, severity of leukoaraiosis was independently associated with larger infarct cores , greater infarct volume growth , and increased risk of hemorrhagic transformation and parenchymal hematoma following intra-arterial thrombectomy for treatment of acute ischemic stroke, especially leukoaraiosis in deep white matter region. [43
Don’t Miss: How To Care For Alzheimer Patients
How Is White Matter Disease Diagnosed
Brain magnetic resonance imaging is the main way healthcare providers diagnose white matter disease. An MRI scan is a painless test that produces very clear images of different parts of your body. MRI uses a large magnet, radio waves and a computer to produce these detailed images without any radiation .
Brain MRI scans allow healthcare providers to see the extent of white matter damage in your brain and to diagnose white matter disease.
White matter changes are visible on magnetic resonance imaging as lesions. An MRI report can call white matter changes a few different things, including:
- Cerebral or subcortical white matter disease or lesions.
- Microvascular disease.
- Non-specific white matter changes.
- T2 hyperintensities .
In some cases, your provider might see signs of white matter disease in your MRI results that you underwent for a different medical reason. In other cases, your provider may order an MRI if nothing else explains your symptoms, such as balance and memory issues.
While there are other types of imaging tests, such as CT scans, MRI has the best imaging quality and sensitivity for diagnosing white matter disease.
Your provider may also perform a neurological exam to assess your symptoms when diagnosing white matter disease.
Since white matter disease is associated with cardiovascular disease risk factors, your provider may also order the following blood tests to assess your risk:
Should You Request An Mri If Youre Concerned About Cerebral Svd
Not necessarily. In my opinion, older adults should only get MRIs of the brain if the following two things are true:
For most older adults, an MRI showing signs of cerebral SVD will not, in of itself, change the management of medical problems.
If you have high blood pressure, you should consider treatment. If you are having difficulties with walking or balance, signs of cerebral SVD do not rule out the possibility of other common causes of walking problems, such as medication side-effects, foot pain, neuropathy, and so forth.
What if youre concerned about memory or thinking problems? Well, you probably will find signs of cerebral SVD on an MRI, just because this is a common finding in all older adults, and its especially common in people who are experiencing cognitive changes.
However, the MRI cannot tell you whether the cognitive changes you are noticing are only due to cerebral SVD, versus due to developing Alzheimers disease, versus due one of the many other dementia mimics. You will still need to pursue a careful evaluation for cognitive impairment. And no matter what the MRI shows, you will likely need to consider optimizing cardiovascular risk factors.
So in most cases, a brain MRI just to check for cerebral SVD is probably not a good idea.
You May Like: Does Ted Turner Have Dementia
The Behavioral Neurology Of White Matter: Diagnosis Of Major Disordersand Syndromes
More than 100 neurologic diseases, injuries, and intoxications are known to prominently or exclusively involve the white matter of the brain.
More than 100 neurologic diseases, injuries, and intoxications are known to prominently or exclusively involve the white matter of the brain.1,2 Without exception, these disorders have the potential to disrupt aspects of cognitive and emotional function and to lead to important syndromes related to white matter dysfunction. Although not as familiar as the diseases of gray matter that have dominated thinking in behavioral neurology, the white matter disorders are emerging as common problems that erode neurobehavioral function.
Recognizing the clinical effects of white matter lesions helps illuminate the role of white matter tracts in the normal connectivity of the brain and illustrates how white matter makes an essential contribution to the distributed neural networks that subserve all higher functions. WHITE MATTER DISORDERS White matter disorders that affect the brain make up a widely diverse group of diseases, injuries, and intoxications . The range of these disorders encompasses all major categories of neurologic illness, and the variety of white matter neuropathology is impressively broad. This review focuses on disorders that prominently or exclusively involve brain white matter.
NEUROBEHAVIORAL SYNDROMES
COGNITIVE IMPAIRMENT
FOCAL NEUROBEHAVIORAL SYNDROMES
NEUROPSYCHIATRIC SYNDROMES
FUTURE DIRECTIONS
Automated Total And Region Of Interest
The individual FA maps were registered with the JHU atlas FA maps to assign detected WMH voxels to specific JHU tracts using the JHU max probability map . Additionally, WMH voxels were assigned to the JHU labels atlas . Whole-brain and tract-/label-specific WMH volumes were automatically calculated in mm3. Figure 1 summarizes major steps of the preprocessing pipeline.
Also Check: How To Get Power Of Attorney Over Parent With Dementia
Rarer Causes Of Dementia
There are many rarer diseases and conditions that can lead to dementia, or dementia-like symptoms.
These conditions account for only 5% of dementia cases in the UK.
They include:
- problems with planning and reasoning
These symptoms are not severe enough to cause problems in everyday life.
MCI can be caused by an underlying illness, such as depression, anxiety or thyroid problems.
If the underlying illness is treated or managed, symptoms of MCI often disappear and cause no further problems.
But in some cases, people with MCI are at increased risk of going on to develop dementia, which is usually caused by Alzheimer’s disease.
Read more about how to prevent dementia.
Urodynamic Findings In Wmd
DO is the major underlying pathophysiology of vascular incontinence. The incidence of DO in WMD cases is reported as 7091% of patients , and is more common than following hemispheric stroke . In our study , urodynamic studies were performed in 33 subjects. We found that subjects with grade 14 WMD had DO significantly more commonly than those with grade 0 WMD . Postmicturition residuals, low compliance, DSD, and uninhibited sphincter relaxation were also more common in grade 14 WMD than in grade 0 WMD, though not significantly so.
Also Check: What Is The Best Sleep Aid For Dementia Patients
Ischemic Demyelination And Ischemic Stroke Risk
Patients with ischemic white matter disease are at enhanced risk for stroke . In addition, white matter hyperintensities on MRI in elderly normal volunteers correlate with subtle cognitive deficit with reduced speed of complex mental processing . Lacunar-type stroke has been reported to have a recurrence rate of up to 12% per year, and one can hypothesize that asymptomatic small vessel disease is presumably associated with at least some heightened risk when compared with an age-matched population without evidence of ischemic demyelination on brain scan. Multiple studies indicate that it is the confluence of the ischemic white matter lesions on MRI brain scan that is associated with the greatest risk for clinically evident ischemic stroke . This confluence of larger white matter abnormalities correlates with the changes described as leukoaraiosis on CT brain scan.
Roger E. Kelley, Brian P. Kelley, in, 2018