Life Expectancy And Treatment
About 10 15% of dementia cases are thought to be frontal lobe dementia, the disease affecting 1 in 5000 of the population. However in those under 65 it is believed to be 20 50% of cases. Onset of frontal lobe dementia is normally identified when the patient is between 45 and 65 years of age, although it has been seen in people aged 20 to 30 years of age. Only 10% of cases are identified in those 70 years and over.
The disease takes from three to ten years to progress, although there are instances of much shorter or longer times. The average life expectancy of a person diagnosed with frontal lobe dementia is eight years. Approximately 50% of deaths are as a result of pneumonia, following complications associated with inability of the person to move or care for themselves.
As with other forms of dementia there is no current cure for the disease, but there are a range of treatments that can help to manage and deal with the symptoms, and to help people to regain some of their lost functions.
These include drugs such as SSRI antidepressants to help control the symptoms like obsession, over-eating and depression. Antipsychotics may be given to address challenging and inappropriate behaviours. Psychological treatments such as cognitive stimulation and behavioural therapy can help maintain memory function address anxiety. Rehabilitative practices such as, occupational therapy, physiotherapy and speech therapy can help the brain to learn new ways to do things.
References:
Frontotemporal Dementia Causes And Risk Factors
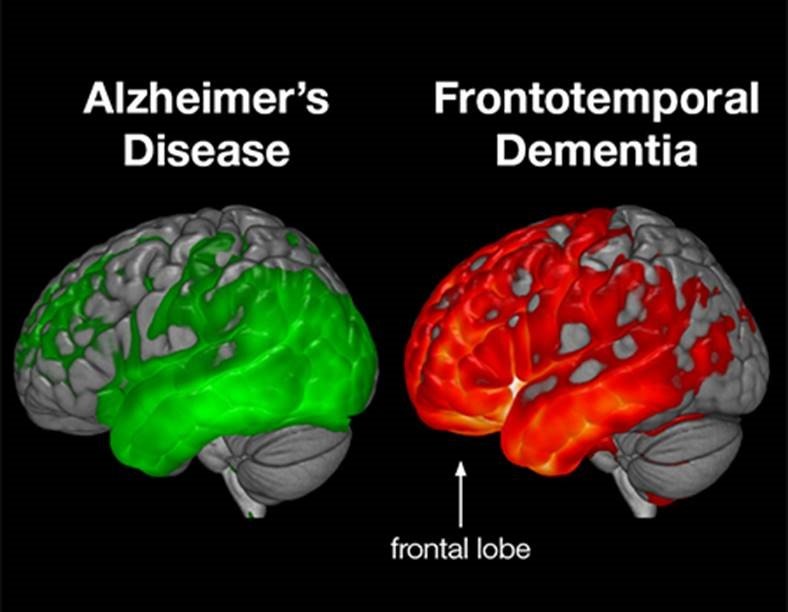
Scientists donât know for sure what causes FTD. But it starts when nerve cells in two parts, or âlobes,â of the brain — the front and the side — die. That causes the lobes to shrink.
Doctors believe FTD may be genetic. About 4 out of 10 people who have it also have a relative who had it or some other form of dementia.
Genetic FTD happens when you have a mutation, or change, in one of three genes:
- C9ORF72
The type of mutation you have affects the type of symptoms you have.
Alzheimer Disease And Ftd
Alzheimer disease, by far the most common dementing pathology, has also been associated with syndromes of PPA and FTD in some cases. Alzheimer disease is uncommonly found at autopsy in patients with primary progressive, nonfluent aphasia, but the association is more common in semantic dementia and is especially frequent in patients with logopenic progressive aphasia. The relationship of Alzheimer disease to the primary progressive aphasia syndromes is covered in more detail in the section on Primary Progressive Aphasia. In addition, there is now a recognized syndrome of frontal variant Alzheimer disease.
Recommended Reading: What Is The Difference Between Dementia And Senility
Understanding Different Types Of Dementia
When most people hear the word dementia, one of the first things that comes to mind is Alzheimers. In common speech, the two terms are often used interchangeably, and when a persons loved one shows signs of memory loss, its not uncommon for them to say, I hope its not Alzheimers.
However, Alzheimers is just one cause of dementia, which is the umbrella term for decline in memory, thinking and reasoning skills that significantly impacts daily life. If a loved one is experiencing memory issues, Alzheimers could be a potential diagnosis, but there are four other common types of dementia that should also be considered: Lewy body, frontotemporal, vascular and mixed.
Each variety of dementia has different characteristics, and for caregivers, knowing the difference can help in monitoring a loved ones symptoms and accessing the right resources. Here is a breakdown of the five most common varieties:
The Aftd Helpline: A Vital Source Of Support And Information
The FTD journey can be filled with many questions. Having a place to turn to for answers and reliable help is important.
The AFTD HelpLine is available for anyone looking for information, resources, and support related to FTD. Trained members of AFTDs staff are available to answer calls and emails with available research and the most current resources. HelpLine staff ensure that each inquiry receives an individualized, supportive, and timely response.
Whether its a question about managing symptoms, accessing local resources and services, or updates on FTD research initiatives, the AFTD HelpLine is available to assist with your inquiries.
If you have a question about living with FTD or caring for a loved one who is diagnosed, please contact our HelpLine by phone at or via email at .
For more information on the HelpLine and the additional AFTD support services, visit our Resources page here.
Stay Informed
Sign up now and stay on top of the latest with our newsletter, event alerts, and more
Recommended Reading: Does Bob Knight Have Dementia
Signs And Symptoms Of Frontotemporal Dementia
Each case of FTD is different, but the illness generally becomes more distinguishable from other brain conditions as it progresses. Symptoms may occur in clusters, and some may be more prevalent in early or later stages. Here is a list of ten signs of FTD:
What Causes Frontal Lobe Dementia/frontotemporal Dementia
Scientists dont know what causes the majority of cases of frontal lobe dementia. However, abnormal accumulations of proteins, either tau or TDP-43, have been found during autopsy in the brains of people who suffered from frontal lobe dementia.
Furthermore, a number of genes linked to the abnormal production of these proteins have been identified and are responsible for the disease in the 15 to 40 percent of people who suffer from a hereditary form of it.
Also Check: Does Meredith Grey Get Alzheimer’s
Clinical Diagnostic Criteria For Ftd: Strengths And Limitations
The most recently revised consensus criteria for the clinical diagnosis of bvFTD are those by Rascovsky et al. . In this hierarchical framework, three levels of diagnostic certainty are distinguished. The first degree determines whether or not the termpossible bvFTD is appropriate and is based upon presence of core symptoms alone. For probable and definite bvFTD, results of imaging and histopathology/DNA analysis, respectively, are taken into account. The consensus criteria for possible bvFTD have a sensitivity of 8595% and a specificity of 82%, irrespective of the underlying proteinopathy . For probable bvFTD, sensitivity and specificity values are 7585 and 95%, respectively . A higher sensitivity is reached in early onset dementia compared with late onset, as in younger age groups there is significantly more disinhibition, loss of empathy and compulsive behavior . False positive diagnoses are most common in patients with a later onset, an absence of family history for dementia and a more apathetic presentation. They mainly turn out to be AD upon neuropathological examination .
Several other clinical tools exist to measure frontal lobe dysfunction and therefore differentiate between FTD and AD. Many assessment batteries of neurobehavioral symptoms, such as the Schedules for Clinical Assessment in Neuropsychiatry , the Scale for Emotional Blunting , the Middelheim Frontality Score and the Frontal Behavior Inventory have a good discriminative ability .
Imaging Biomarkers In A Research Setting
Diffusion Tensor Imaging
Diffusion tensor imaging is an MRI imaging technique visualizing the diffusion of water molecules throughout the brain. It is used as a technique for white matter tractography .
Studies have shown that white matter damage is an early marker for disease in FTD, and DTI may be used as a tool to screen for such abnormalities at the presymptomatic stage . Reduced integrity of the uncinate fasciculus and anterior corpus callosum is typical for FTD, and the degree of damage is correlated to age and disease severity . Even here, specific patterns can be recognized for different clinical subtypes, and for carriers of different causal mutations. These abnormalities are consistent with characteristic brain atrophy distributions . The increase in white matter damage over time has been reported to be greater than that of gray matter atrophy, although only at the symptomatic stage, indicating the possible use of this technique as a marker for disease progression .
Studies comparing FTD cohorts with AD patients and with normal controls found significantly more white matter pathology mostly in bilateral uncinate fasciculus, cingulum bundle, and corpus callosum in FTD compared to both other groups . More studies are needed to consolidate these findings and define the diagnostic accuracy for FTD of DTI, as well as its power to distinguish FTD from other types of neurodegenerative brain diseases.
Resting-State fMRI
Arterial Spin Labeling
Tau PET Imaging
Also Check: How To Stop Alzheimer’s Patient From Picking Skin
What Are The Stages Of Frontotemporal Dementia
On the surface, Joseph, Barbara, and Lloyd may not seem to be experiencing related changes. Each of them, though, turned out to be in the early stage of frontotemporal dementia . FTD is the diagnosis for about 5 percent of people with major neurocognitive disorders . About 70 percent of cases begin before age 65, so it is a more common dementia among the young old. FTD involves degeneration of the frontal and temporal lobes of the brain. The frontal lobes are important regulators of behavior and the temporal lobes assist in our understanding and expression of language. The symptoms of FTD, therefore, include major changes in behavior, impairment of language, or both.
People diagnosed with FTD and family members often ask What stage of dementia is occurring? and the answer to this question can be useful in knowing what to expect in the future. FTD often begins during years when adults expect to be healthy and productive. The average course of the disease takes 6 to 8 years after diagnosis, so patients and their families must confront very serious and increasingly difficult needs. Detailed and complex timelines of the stages of FTD are not very accurate, but it is useful to think of the development of FTD through early, middle, and late stages. Lets look at the stages of frontotemporal dementias to see how these related disorders evolve:
Frontal Lobe Anatomy And Function
The brain has two hemispheres, the left and the right, which are further divided into three sections: the forebrain, the midbrain, and the hindbrain. Differentiation of these separate parts occurs during fetal development. Each has specific functions:
- The hindbrain controls respiration and heart rate
- The midbrain controls reflex actions such as eye movement
- The forebrain controls emotional perceptions and responses, involuntary movements, sleep patterns, memory, and organizational ability
The forebrain eventually develops into the cerebrum, the outer layer of which is called the cerebral cortex. The frontal lobe is one of the four lobes of the cerebral cortex, which also includes the temporal lobe, the parietal lobe, and the occipital lobe.
Each of these regions carries out specific functions, and damage to any of these lobes results in corresponding impairment.
The frontal lobes are relatively large compared to other regions of the brain, and the extensive functions controlled by the frontal lobe is reflected in its proportional size.
You May Like: Does Smelling Farts Help Prevent Dementia
How Is Frontal Lobe Dementia Diagnosed
General practitioners or health professionals are unable to diagnose frontal lobe dementia with a single test alone. Instead, diagnosis usually requires a multifaceted approach to first rule out other conditions and diseases. Following this, GPs and health professional may recommend a series of tests to aid in diagnosis.
Alzheimers Association cites several tests that are commonly used to diagnose frontal lobe dementia. These include:
- Blood tests to help identify other possible causes.
- Genetic testing may be recommended to determine whether a persons condition is caused by a specific gene.
- Neuropsychological testing to check your judgement and memory skills, and help determine what type of dementia you may have.
- Brain imaging to examine the brain and check for tumours or blood clots. If further tests are needed, more specialised brain scans will be carried out, such as a positron emission tomography or a single photon emission computerised tomography to measure the persons brain activity.
- Magnetic Resonance Imaging to give GPs and health professionals a detailed image of your brain to assess any affected areas or damage.
- Computerised Tomography scan which creates images of your brains in layers to enable a more thorough examination.
What Are The Prognosis And Options For Treatment
FTD worsens over time and impairs the individuals ability to live and function independently. Although there is no cure for FTD, there are medications that can help control the behavioral symptoms of the disorder. With an accurate diagnosis, unnecessary medications can be removed that might otherwise worsen the disease symptoms.
You May Like: What Color Represents Dementia
Neuronal Intermediate Filament Inclusion Disease
Neuronal intermediate filament inclusion disease is a rare distinct variant. The inclusion bodies that are present in NIFID are cytoplasmic and made up of type IV intermediate filaments. NIFID has an early age of onset between 2356. Symptoms can include behavioural, and personality changes, memory and cognitive impairments, language difficulties, motor weakness, and extrapyramidal symptoms. NIFID is one of the FTLD-FUSproteopathies.Imaging commonly shows atrophy in the frontotemporal region, and in part of the striatum in the basal ganglia. Post-mortem studies show a marked reduction in the caudate nucleus of the striatum frontal temporal gyri are narrowed with widened intervening sulci, and the lateral ventricles are enlarged.
Is It Genetic Can It Be Passed On To Family Members
- A combination of genetic, environmental and lifestyle factors have been suggested by researchers. While a variety of changes on multiple genes have been linked to specific subtypes of frontotemporal dementia, more than half of people who develop frontotemporal dementia have no family history of dementia.
- A persons risk of developing frontotemporal dementia is higher if they have a family history of dementia. Roughly 10-15 per cent of persons living with the disease have a strong family history of the disease. Typically, in these cases, FTD is inherited from a parent as a defect in one of three genes: MAPT, GRN or C9ORF72.
- Currently, there are no other known risk factors.
Also Check: What Color Is The Dementia Ribbon
Language And Neuropsychological Testing
Other than brain imaging studies, the most specific tests for evaluating frontotemporal lobe dementia are evaluation with standardized language batteries and neuropsychological testing. Such studies assess the specific pattern of language abnormality and the presence of other cognitive and memory deficits. Preservation of many of these functions distinguishes FTD and primary progressive aphasia syndromes from Alzheimer disease.
In distinguishing FTD from Alzheimer disease, the involvement of specific cognitive functions is the most important differentiating factor.
Grossman pointed to a double dissociation between immediate and short-term memory in a comparison study of 4 patients with PPA versus 25 patients with presumed Alzheimer disease. Immediate memory was more impaired in PPA patients, whereas short-term memory deficits characterized the deficits of patients with Alzheimer disease. The frontal cortex, especially on the left side, is thought to be the site of working or immediate memory, whereas the hippocampus and other medial temporal structures, often affected early in Alzheimer disease, represent the site of short-term memory.
PPA is a syndrome, not a pathological diagnosis. Although the term initially implied a pathology other than Alzheimer disease, we must now consider that some cases may have a syndrome of PPA but a pathological diagnosis of Alzheimer disease, or vice versa.
Disinhibition
Frontal Lobe Dementia Onset
One main difference between frontal lobe dementia and Alzheimers disease is that, on average, frontal lobe dementia first presents itself significantly earlier in life. Frontal lobe dementia symptoms usually appear between 45 and 65 years of age, while the majority of Alzheimers cases occur in those over 65.
Read Also: Will Meredith Get Alzheimer’s
Brain Fdg Pet And Perfusion Spect Scan To Diagnose Ftd
Another part of the investigation of patients with suspected FTD is based on functional imaging of the brain . A commonly used technique is the FDG PET scan, which visualizes the cerebral glucose metabolism. Another method for functional imaging is perfusion SPECT, which also requires the intravenous injection of a radiolabeled tracer molecule, but instead is a measure of cerebral blood flow . The radiotracers most commonly used are 99mtechnetium-hexamethylpropylenamine oxime or 99mtechnetium-ethyl-cysteinate dimer .
In FTD, hypometabolism and hypoperfusion are typically seen in the frontal and anterior temporal lobes, more specifically in bilateral medial, inferior and superior lateral frontal cortices, anterior cingulate, left temporal, and right parietal cortices and the caudate nuclei. Usually, the hypometabolism correlates with, but often precedes, the atrophy on MRI . Local hypometabolism is best observed in the frontal regions for bvFTD, temporal regions for sv-PPA and perisylvian regions for nfv-PPA .
For FTD, the sensitivity of FDG PET scan ranges from 47 to 90% the specificity from 68 to 98% . In subjects with late onset behavioral changes, bvFTD could be differentiated from other diagnoses with a sensitivity of 96% and a specificity of 73% when combined with structural MRI . An increase of the abnormalities can be seen over time, indicating the potential usefulness of FDG PET as a biomarker of disease progression .
Core Ad Csf Biomarkers: A142 A142/a140 Ratio T
The currently most used panel to assess pathological markers of neurodegenerative brain disease is a combination of amyloid- of 42 amino acids , total tau protein , and hyperphosphorylated tau in CSF . They are not, in fact, used for the diagnosis of FTD, but rather to make the diagnosis of AD less likely when doubt exists. A CSF biomarker profile characteristic for AD, with good diagnostic accuracy , shows decreased A142 values, in combination with increased T-tau and P-tau values . Some patients do not completely match this typical AD CSF profile. As amyloid pathology is measurable much earlier in the disease process than tau pathology, there may be an isolated decrease in A142 in early disease stages . CSF tau markers are more strongly associated with cognitive decline and disease progression in AD than A142 . The opposite may also be true, as between-individual variations in total A production or secretion from neurons and variations in CSF dynamics may cause A142 to fall within a normal range, while underlying amyloid pathology is present .
To further improve diagnostic performance for AD, the use of the A142/A140 ratio has been proposed with good results , improving accuracy with 1436% compared to A142 alone . An isolated decrease in A142 is more specific to AD, while a global decrease in both A isoforms may be correlated with subcortical damage in general or may even be due to interindividual variability .
You May Like: Dementia Ribbon Colors