Dementia With Lewy Bodies
Dementia with Lewy bodies is responsible for approximately 25% of dementias and belongs to the atypical Parkinson syndromes together with progressive supranuclear palsy and multi-system atrophy . The clinical manifestations can be similar to that of AD or dementia associated with Parkinson’s disease. Patients typically present with one of three symptom complexes: detailed visual hallucinations, Parkinson-like symptoms and fluctuations in alertness and attention.Pathologically, the disease is characterized by the presence of Lewy bodies in various regions of the hippocampal complex, subcortical nuclei and neocortex with a variable number of diffuse amyloid plaques. Cholinesterase inhibitors are currently the treatment of choice for this condition.
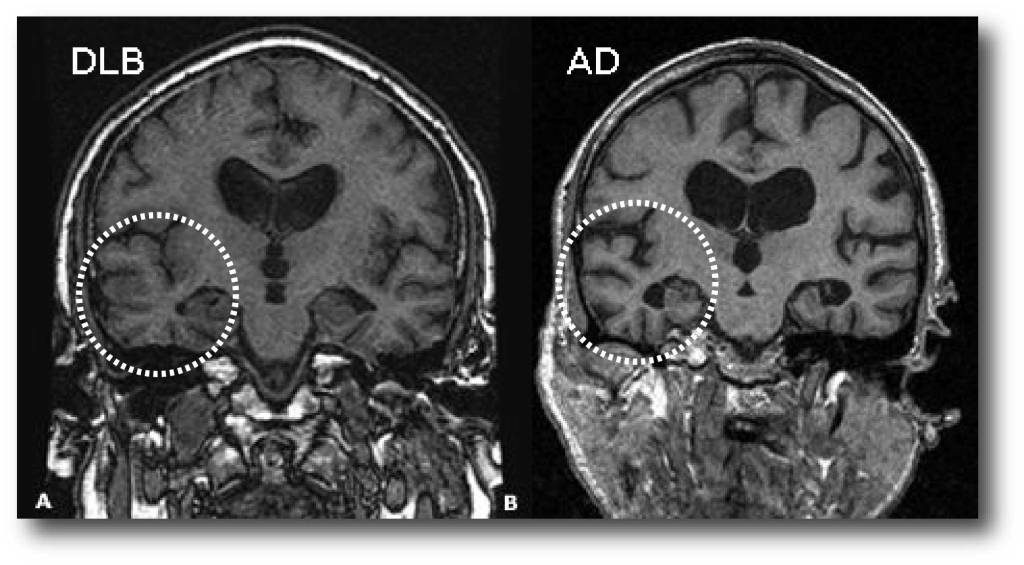
The role of imaging is limited in Lewy body dementia.Usually the MR of the brain is normal, including the hippocampus. This finding is important as it enables us to differentiate this disease from Alzheimer’;s disease, the main differential diagnosis. Nuclear imaging can be used to demonstrate an abnormal dopaminergic system
PSP with midbrain atrophy
Brain Imaging For Lewy Body Dementia
;to download a pdf of this document.
Imaging techniques like computerized tomography scans and magnetic resonance imaging scans have been around for many years and have been vital tools in diagnosing a very wide variety of diseases. While neither is diagnostic of Lewy body dementia , they can assist the physician in diagnosis. Additionally brain imaging plays an important role in advancing research to better understand the brain changes associated with LBD. This article will help you understand the different ways imaging techniques play an important role in diagnosing LBD and advancing LBD research.
Common Symptoms Of Lewy Body Dementia
The disease of Lewy Body Dementia affects cognitive response, changes physical and sleep pattern along with changing behavioral features. Some people may start developing the disorder in movement in the initial stage that further leads to dementia. This is often termed as Parkinsons disease dementia.
Another group of people may start developing cognitive disorder with two or more distinctive features of dementia. There are very few people that come up with neuropsychiatric symptoms. These include hallucinations, behavioral problems, and complex mental activities.
Generic symptoms of Lewy Body Dementia include:
- Impaired thinking like loss of execution, planning, processing and/or ability to understand visual information
- Fluctuation in alertness, attention, and cognition
- Sudden tremors, stiffness, and difficulty in walking
- Changes in bodily functions like blood pressure, temperature regulation bowel and bladder function.
Don’t Miss: Sandyside Senior Living
Cortical And Subcortical Involvement In Dlb
Serial MRI is an appealing biomarker of neurodegeneration and can assist in monitoring disease progression. Although longitudinal cerebral atrophy rates in AD are well-established and employed as outcome measures in clinical trials of potential disease-modifying agents, the atrophy rate in DLB has been reported to be analogous to or marginally greater than healthy controls . While longitudinal studies of DLB are challenging given the higher mortality rates compared to AD , further investigations into DLB patients with a more rapidly progressive disease would be valuable in elucidating the neurobiological underpinnings of disease heterogeneity in DLB.
Evidence of subcortical involvement in DLB has revealed the vulnerability of the thalamus, striatum and brainstem to Lewy-related pathology. Studies have demonstrated that thalamic diffusion and perfusion deficits are associated with DLB , and striatal volumetric loss appears to be more affected in DLB than AD , with prominent nigrostriatal dysfunction . Significant reductions in brainstem volume in DLB have also been reported , with Seidel et al. showing marked to severe neuronal loss in the ventral tegmental, pedunculopontine nucleus and locus coeruleus regions in DLB .
Treatments For Dementia With Lewy Bodies
There’s currently no cure for dementia with Lewy bodies or any treatment that will slow it down.
But there are treatments that can help control some of the symptoms, possibly for several years.
Treatments include:
- medicines to reduce hallucinations, confusion, drowsiness, movement problems and disturbed sleep
- therapies such as physiotherapy, occupational therapy and speech and language therapy for problems with movement, everyday tasks, and communication
- psychological therapies, such as cognitive stimulation
- dementia activities, such as memory cafes
Don’t Miss: How To Move A Parent With Dementia To Assisted Living
A Study Of Neuroimaging And Magnetoencephalography Biomarkers For Prodromal Dementia With Lewy Bodies
2019/20 Grant awarded to Dr Li Su, ARUK Senior Research Fellow, Department of Psychiatry, University of Cambridge. Study also supported by Windsor Research Unit, Cambridgeshire and Peterborough NHS Trust
Aim of the study
To use new imaging technologies to compare brain structure and function among people with mild-cognitive impairments, to try to identify which patients will go on to develop dementia with Lewy bodies or Alzheimers disease. This will help with earlier diagnosis and identifying those at risk of developing DLB.
Description of the study
Dementia with Lewy bodies is the second most common type of neurodegenerative dementia after Alzheimers disease . It often takes much longer to be diagnosed than other types of dementia and progresses more aggressively. There are currently no licensed drugs for DLB in the UK. To develop effective treatments, we need to discover new ways to detect DLB in its early and prodromal stages . This study uses new, state of the art brain scans aimed at identifying early changes in the brain that can lead to earlier detection.
;Our approach is to focus on individuals who meet the criteria for mild cognitive impairments with Lewy bodies but have not yet developed full-blown dementia. Previous research has shown that a large proportion of patients with MCI, in particular those with milder memory problems alongside other neuropsychiatric symptoms, develop into DLB rather than AD.
Click here for more information.
Donate
Comparison Between Dlb And Ad
MRI has been widely used to investigate patterns of gray matter atrophy. Advances in image processing have enabled automatic extraction of whole brain cortical thickness, which is retrieved from structural MRI. Although DLB has demonstrated some overlap with the cortical atrophy patterns seen in AD, atrophy is generally less diffuse in DLB with moderate preservation of the medial temporal lobe structures .
Although investigations into hippocampal atrophy have revealed that DLB patients have less severe atrophy compared to AD patients , with the entorhinal cortex, CA1 and subiculum areas of the hippocampus being most affected in AD , recently, Delli Pizzi et al. explored the differential contribution of hippocampal subfields and adjacent extrahippocampal structures to the pathophysiology of AD and DLB . They reported that the cornu ammonis and subiculum were preserved in DLB, but the perirhinal cortex and parahippocampus were damaged, highlighting the differential alteration of hippocampal subfields and adjacent extrahippocampal structures in DLB and AD .
Studies have also demonstrated greater atrophy in the substantia innominate, with increased dorsal mesopontine GM atrophy distinguishing patients with clinically diagnosed DLB from AD . These findings may suggest a greater cholinergic dysfunction in DLB, perhaps related to the presence of midbrain synuclein pathology.
You May Like: Does Meredith Have Alzheimer’s
Supportive Measures And Treatments
In addition to medication, there are;a number of therapies and practical measures that can help make everyday living easier for someone with dementia. These include:
- occupational therapy to identify problem areas in everyday life, such as getting dressed, and help work out practical solutions
- speech and language therapy to help improve any communication or swallowing problems
- physiotherapy to help with movement difficulties
- psychological treatments, such as cognitive stimulation, to help improve memory, problem-solving skills and language ability
- relaxation techniques, such as massage, and music or dance therapy
- home modifications, such as removing loose carpets and potential trip hazards, ensuring the home is well lit, and;adding grab bars and handrails
- checking for problems with vision and hearing that could be contributing to hallucinations
Read more about living well with dementia
Diagnosing Dementia With Lewy Bodies
If you think you may have early symptoms of dementia, it’s a good idea to see your GP. If you’re worried about someone else, encourage them to make an appointment, and perhaps suggest that you go along with them.
Your GP can do some simple checks to see if there is chance you could have dementia, and they can refer you to a memory clinic or another specialist clinic if necessary.
At one of these clinics,;you will be asked about your symptoms and have a physical check-up and memory test. You may also have;blood tests and brain scans.
The results of these checks and tests will give your doctor a good idea as to whether your symptoms are caused by;dementia with Lewy bodies, another type of dementia, or;something else;entirely.
Also Check: Senile Dementia Of The Alzheimer Type
What Does Lewy Body Dementia Look Like
Lewy body dementia affects a persons ability to think and process information and it can negatively impact memory and alter personality. Though it shares aspects of other forms of dementia, there are distinct hallmarks of LBD. Lewy body dementia symptoms include:
- Fluctuating attention/alertness: These shifts can last hours or go on for days. The person may stare into space, appear lethargic or drowsy, and have hard-to-understand speech, appearing a lot like delirium. At other times, the person may have much more clarity of thought.
- Visual hallucinations: Often, these are very detailed hallucinations and visions of people or animals, and they can recur.
- Movement disorders: Parkinsons-like movement issues, such as muscle rigidity, tremors, falls, or a shuffling gait or way of walking, may occur.
The Link To Parkinsons Disease
Most people with Parkinsons disease have Lewy bodies in their brains. Its these clusters that cause some or all of the motor symptoms of Parkinsons disease, as well as memory or cognitive problems, visual hallucinations, and problems with alertness.
We rarely know if a living patient has Lewy bodies with certainty, however. Its not until an autopsy that they can be seen, says Liana Rosenthal, M.D., assistant professor of neurology at the Johns Hopkins University School of Medicine. If we see Lewy bodies in someones brain during an autopsy, thats considered a pathologic certainty of Parkinsons disease, she says.
As with Parkinsons, Lewy body dementia is associated with a depletion of certain neurotransmitters in the brain. These are:
- Dopamine: This neurotransmitter helps transmit signals that control muscle movement. When the accumulation of Lewy bodies blocks dopamines production and transmission, the result is the hallmark movement issues of Parkinsons disease.
- Acetylcholine: This neurotransmitter does its work in the parts of the brain responsible for memory, thinking and processing. When Lewy bodies build up in these areas, they interfere with acetylcholine, causing symptoms of dementia.
Also Check: Senility Vs Dementia Vs Alzheimer’s
What Is Lewy Body Dementia And What Happens In It
The deposition of lewy bodies in the brain causes its function to decline and eventually ends up as dementia, which is termed as Lewy body dementia . LBD is a progressive condition, meaning that symptoms gradually get worse over time. People with the disease will notice the decline in mental function, memory and understanding that affects all people with dementia. However, individuals with Lewy body dementia may also experience some of the more confusing and upsetting symptoms of dementia including visual hallucinations and sleep disruption. The movement problems of Parkinson’s disease, including shaking, stiffness and slow movement are also prevalent.
Is Lewy Body Dementia Hereditary & What Is The Life Expectancy Of A Person With Lewy Body Dementia
Most patients suffering from Lewy Body Dementia prefer visiting a primary care physician at the initial stage. Diagnosing the disorder can be a real problem if the symptoms grow severe.
There are many families that have been affected by Lewy Body Dementia . However, it has been seen that very few individuals and even medical professionals are aware of the diagnostic criteria and symptoms. Some even dont have the idea whether or not the disease exists. Therefore, you should know about Lewy Body Dementia not only to save yourself but also your loved ones, families and friends. Lewy body dementia is a type of progressive dementia that comes only after Alzheimers disease dementia.
Read Also: Does Alzheimer’s Run In Families
Symptoms Of Dementia With Lewy Bodies
People with dementia with Lewy bodies may have:
- hallucinations seeing, hearing or smelling things that are not there
- problems with understanding, thinking, memory and judgement this is similar to Alzheimer’s disease, although memory may be less affected in people with dementia with Lewy bodies
- confusion or sleepiness this can change over minutes or hours
- slow movement, stiff limbs and tremors
- disturbed sleep, often with violent movements and shouting out
- fainting spells, unsteadiness and falls
These problems can make daily activities increasingly difficult and someone with the condition may eventually be unable to look after themselves.
Comparison Between Dlb And Pdd
Attempts to compare GM loss between DLB and PDD have revealed a pattern of more pronounced GM loss in DLB compared to PDD, which is in line with the fact that DLB encompasses greater amyloid burden . It is important to note, however, that localisations of GM reductions in DLB relative to PDD vary amongst different studies. For example, Burton et al. were unable to identify distinct cortical atrophy profiles of DLB and PDD , but Beyer et al. reported GM reductions in the temporal, parietal and occipital lobes in DLB using a voxel-based morphometry approach . Alongside the temporal and parietal atrophy, Lee et al. also reported occipital and striatal GM reductions in DLB . Studies investigating correlation patterns between brain structure and clinical and neuropsychiatric manifestations of the disease, revealed that decreased GM volume of the anterior cingulate, right hippocampus and amygdala were associated with cognitive performance , whilst reduced GM volume in the left precuneus and inferior frontal lobe correlated with visual hallucinations in DLB, but not in PDD .
You May Like: How Does Dementia Kill You
Can An Mri Detect Lewy Body Dementia
Imaging techniques, such as MRI and CT scans are doing the rounds for many years, and they act as vital tools to diagnose many diseases. Though MRI isnt a diagnostic test of Lewy body dementia, yet it can assist a physician in diagnosing the condition. Moreover, the brain imaging has a significant role in research to have a better understanding of the changes in the brain linked with Lewy body dementia.
What Complications Are Associated With Medications Used To Treat Lewy Body Dementia
Up to 50% of people living with Lewy body dementia can have severe side effects when treated with certain antipsychotic medications. These are known as the typical or traditional antipsychotics and include such drugs as thoridazine, haloperidol, chlorpromazine and perphenazine. This class of older, first-generation antipsychotics can cause sedation and make cognitive symptoms and movement problems worse. A life-threatening reaction to an antipsychotic medication, called neuroleptic malignant syndrome, is possible. Symptoms include rigid muscles, changing blood pressure, high fever, confusion and fast heart rate. Contact your healthcare provider immediately if you or your loved are taking an antipsychotic and develop these symptoms.
Visual hallucinations and behavioral changes may be treated with the newer, atypical antipsychotic medications pimavanserin , quetiapine or clozapine . However, because all antipsychotic medications both older, typical medications and newer atypical medications can increase the risk of death in elderly patients with dementia, you and your healthcare provider should carefully discuss the risks and benefits and using these medications.
Other medications, like antidepressants or sedative antihistamines, may increase confusion in people with LBD.
Don’t Miss: What Is The Difference Between Dementia And Senility
What Are Lewy Bodies
Dementia with lewy bodies is caused by lewy bodies, which are tiny deposits of a protein that build-up in the brains nerve cells, especially the areas that affect the memory, thought and movement. They were named after the German doctor that discovered them and are implicated in causing a form of dementia and Parkinsons disease.
Scientists dont fully understand the lewy body dementia pathophysiology; however, the proteins are associated with low levels of neurotransmitters, which are the chemicals that carry messages between nerve cells. The loss of connection between the nerve cells eventually leads to cell death and progressively deteriorating symptoms. The specific signs and symptoms depend on the area of the brain that has been affected.
How Dementia With Lewy Bodies Is Managed
There is no cure for dementia with Lewy bodies or any;medication that will slow it down.
However, a few different medicines can be effective in controlling some of the symptoms. In particular,;acetylcholinesterase inhibitors have been shown to improve symptoms such as hallucinations and confusion in some people.
Supportive;treatments; such as;physiotherapy, occupational therapy, and speech and language;therapy; can help improve any problems with movement, everyday tasks, and communication.
Psychological therapies and specific;dementia activities, such as memory cafés, can also help;with memory loss, confusion, and feelings of disorientation.
Read more about treating dementia with Lewy bodies
Read Also: Senile Dementia Of Alzheimer’s Type
Which Imaging Studies Are Indicated In The Workup Of Dementia With Lewy Bodies
Because vascular dementia can cause symptoms and signs similar to those of DLB, brain magnetic resonance imaging is indicated to distinguish DLB from vascular dementia. Patients with vascular dementia often have white matter lesions on MRI scans, whereas patients with DLB do not.
Patients with DLB usually have less hippocampal atrophy than do patients with Alzheimer disease , although whether this difference is clinically useful is under investigation, as is the diagnostic utility of functional imaging. MRI is superior to computed tomography scanning in identifying this atrophy.
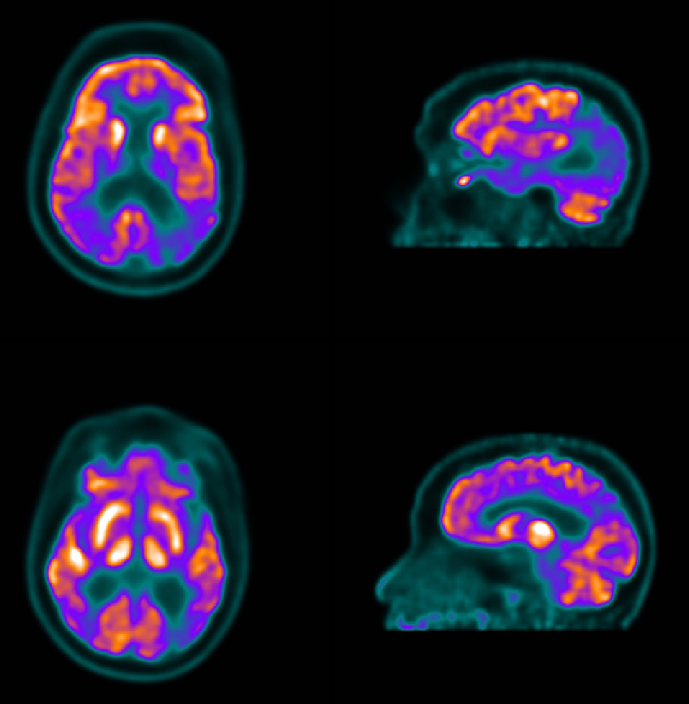
SPECT or positron emission tomography scanning may show decreased occipital lobe blood flow or metabolism in DLB but not in Alzheimer disease. SPECT using ligands that bind to the dopamine transporter molecule has been used to suggest the diagnosis of DLB. Abnormal dopamine transporter scans have been shown to have a sensitivity of over 75% and a specificity of over 90% for DLB.
A study by Lim et al using SPECT scanning with123 I-beta- carbomethoxy-3beta- tropane , as well as PET scanning with18 F-fluorodeoxyglucose , in 14 patients with a clinical diagnosis of DLB and 10 with Alzheimer disease found that relative preservation of the mid- or posterior cingulate gyrus had 100% specificity for DLB. SPECT and PET scanning each appeared useful for the diagnosis of DLB, but SPECT provided more robust results than did PET.
References