Other Relevant Mechanisms Of Disease: Interactions
Although a history of head trauma of sufficient severity to result in unconsciousness may increase the risk of developing AD, this likely makes a minor contribution to the burden of the disease. However, individuals with a history of traumatic head injury and the APOE-4 genotype have a demonstrated increased risk for AD 69 this highlights the crucial interactions between genetic and environmental variables that can culminate in disease expression.
A number of epidemiological studies have reported that poor education is an important risk factor for AD others have found no correlation, however. The brain reserve hypothesis states that education, through the modification of synapses, increases the complexity of cerebral circuitry. Thus, when a biological destructive process occurs the better educated are able to call on their ‘reserves’ before a critical threshold of brain complexity is crossed and dementia is manifested clinically.74 If this were true, one would expect the AD lesions in the brains of better-educated individuals to be more severe several studies have now shown this is not likely to be the case. Individuals with more education may have an advantage when performing the tests used for the diagnosis of dementia, however. An alternative explanation is that the greater prevalence of AD in people with less education might reflect more comorbid cerebrovascular disease and cerebral infarcts.
Identified Rare Risk Loci
A flurry of recent reports has confirmed that a proportion of AD is explained by rare variation with larger effect sizes than normally seen with common variation. Such variants point to the involvement of novel genes in the pathophysiology of disease and importantly highlight protein-coding changes that are novel therapeutic targets.
In 2012, Jonsson and colleagues showed, for the first time in sporadic AD, an association with the amyloid precursor protein gene that causes familial forms of AD. The identified protein-coding change p.Ala673Thr was identified in WGS data from 1795 Icelanders and was shown to protect against disease, and cognitive decline in elderly non-diseased participants . The protein change is thought to reduce -cleavage of APP with approximately 40% reduction in the formation of amyloidogenic peptides in vitro.
It must be noted that these associations have largely been observed in Caucasian populations, However, the majority of non-Caucasian studies are underpowered . The disparity of results in non-Caucasian studies of TREM2 , the work of Kunkle et al. , the cross-population and population-specific associations seen at ABCA7 and the identification of putative association at the AKAP9 gene in an African American cohort emphasise the ethnic specific genetic aetiology of AD and the need for further research in this area.
Genome Wide Association Studies
The next major leap forward came about via the advent of the genome wide association study . GWAS enable researchers to test for association between a given disease or trait and virtually all loci within the human genome in a single pass. A caveat of this is that with such a large number of tests being conducted, the sample sizes required to give sufficient power are very large. This technique was facilitated by the coming together of a number of crucial factors. Firstly, international collaborative efforts such as the 1000 genomes project, which set out to catalog all common human variation across multiple populations . This meant in turn that genotyping arrays could be developed that captured the vast majority of human variation in a single array. Finally, and again through large collaborations, sample cohorts of a large enough size to give sufficient power to these studies became available.
Recommended Reading: Dementia Ribbon Colour
What Causes Alzheimers Disease
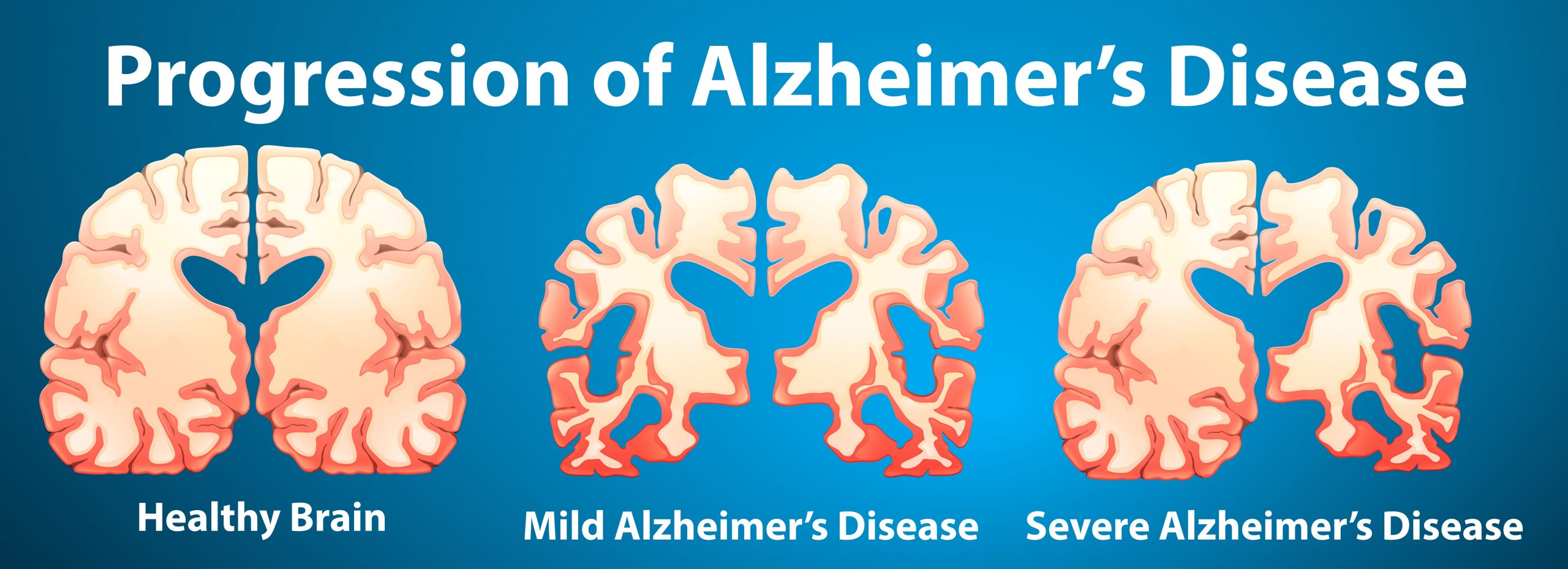
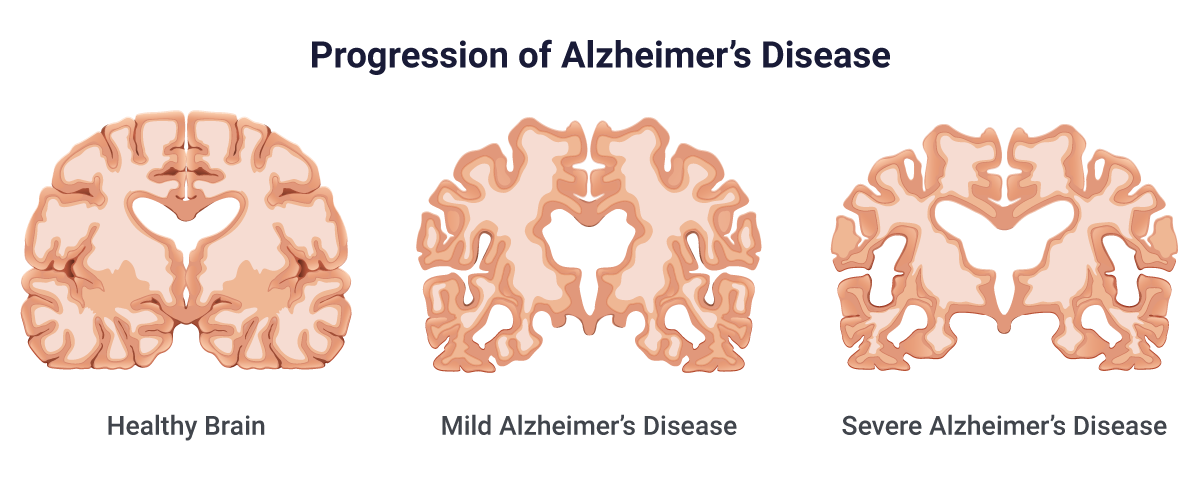
The causes of Alzheimers disease are unknown. Scientists believe that Alzheimer’s disease may be caused by an abnormal buildup of proteins: beta-amyloid and tau. Beta-amyloid buildup forms plaques around brain cells. Tau deposits form twisted fibers called tangles within brain cells. As these proteins accumulate in and around the brain cells, the brain starts to lose its ability to function properly, this leads to loss of brain tissue, and eventually, the brain dies. The tissue damage also causes the affected parts of the brain to shrink .
Initially plaques and tangles damage parts of the brain that control memory, thought, and language. Later they spread and damage other parts of the brain, leading to neuronal degeneration and progressive cognitive decline.
Risk factors for developing Alzheimer’s disease:
The factors that increase the risk are:
- Age: Risk increases with age, affecting 15% of people older than 65 years and 50% of people older than 85 years.
- Family history: Family member with the disease increases the risk. Inherited gene mutations also increase the probability of developing the disease.
- Gender: Women have a higher risk than men.
Rarer Types Of Dementia
Alzheimer’s disease is the most common cause of dementia, but there are many rarer diseases and conditions that can lead to dementia, dementia-like symptoms or mild cognitive impairment.
Most people who are living with dementia have Alzheimers disease or vascular dementia. However, many other diseases and conditions can also cause dementia. These pages explain some of these rarer types.In the UK, about 1 in 20 people living with dementia have a rarer type. Alzheimers Society provides support and information for anyone affected by dementia. These pages include information about how to get in touch with specialist organisations that specifically help people with rarer causes of dementia:
- Atypical Alzheimers disease Frontal variant Alzheimers disease Posterior cortical atrophy
- Normal pressure hydrocephalus
- Progressive supranuclear palsy
Dementia Connect support line
Also Check: Bobby Knight Health Update
Myth #: Doctors Cannot Definitively Diagnose Someone With Alzheimers Disease Until After Death
Before researchers developed biomarker tests in the early 2000s, the only sure way to know whether a person had Alzheimers disease was through autopsy, a procedure that is performed after death. Now, lab and imaging tests are available to help a doctor or researcher see the biological signs of the disease in a living person. For example, it is now possible for doctors to order a blood test to measure levels of beta-amyloid, a protein that accumulates abnormally in people with Alzheimers. Several other blood tests are in development. However, the availability of these tests is still limited. NIA-supported research teams continue to study options for faster, less-expensive, and less-invasive ways to diagnose Alzheimers. Learn more about biomarkers and Alzheimers detection and research.
The Pld3 Mutations Affect A Levels Via Mtor Pathway
To examine whether PLD3 mutations were involved in the regulation of autophagy in cellular model, western blotting was performed to detect the expression levels of the autophagy-associated proteins LC3-II and p62. These PLD3 mutations reduced the level of LC3-II and increased the level of p62 protein , suggesting autophagic activity was remarkably reduced. Autophagy is controlled by several kinases including mTOR, a negative regulator of autophagy. Further study showed that these PLD3 mutations increased the phosphorylation of mTOR and S6K , suggesting that mTOR was markedly activated. We further investigate whether mTOR signaling was involved A accumulation induced by PLD3 mutations. As shown in Figure 2AC, the notion that the inhibition of mTOR kinase by RAPA could induce autophagy was confirmed. As demonstrated by Figure 2D, in the presence of RAPA, these PLD3 mutations failed to increase A42 levels in HEK293-APP695 cells.
You May Like: Etiology Of Dementia
Reducing Your Risk Of Alzheimer’s: What One Greek Island Shows Us
But something frightening happens when you bring those same healthy Ikarian genes to the U.S., as NBC special anchor Maria Shriver discovered for TODAYs Brain Power Today series. You can see it in Cleveland, Ohio, which is home to a number of first- and second-generation immigrants from Ikaria.
When these Ikarians come here to Cleveland, you start seeing Alzheimers at the same rate as you see in the rest of America. They bring all their values here and they get sick, said Dan Buettner, a National Geographic fellow and author of The Blue Zones Solution: Eating and Living Like the World’s Healthiest People.
How To Detect Early Signs Of Alzheimer’s
The modern lifestyle may make you miss something else that keeps the brain sharp: Enjoying the company of other people. Your ancestors never had to try to be social, it just came with the territory theyd just bump into others all the time in the village and talk, he pointed out. So one of the most powerful things people can do is to move to an area with sidewalks, bike lanes and nearby shops so theyre more likely to meet their neighbors and make friends.
Jim Gemelas feels the isolation, too.
People came over and just dropped by nobody drops by anymore. You have to set a time, you have to plan for it, he said.
But on a recent night, everything worked out perfectly as the family came together in the backyard to celebrate their mothers 87th birthday. Her recent diagnosis is a reminder they still have the power to fend off the disease.
About 90 percent of Alzheimers is preventable, Buettner said. Most of your mental health is up to you and the environment you create for yourself.
Read Also: What Color Is For Alzheimer’s
Aphasia Restricts Ones Ability To Speak But Memory Doesnt Suffer
Participants with Alzheimers listened to a list of common words and were later given those words along with others and asked to choose the ones they had heard before. They were tested again an average of almost two years later. Both groups also had their language skills tested.
Scans were taken of the people with PPA to look at how the disease was affecting their brains, especially in the areas related to memory. The study also analyzed brain autopsies from eight of the people who later died with primary progressive aphasia and all of those with typical Alzheimers. The aphasia group had similar amounts of the plaques and tangles that are the hallmark signs of Alzheimers, says Mesulam.
There was less shrinkage on the left side of the brain of aphasia patients and a lower incidence of proteins known as ApoE4 and TDP-43. These proteins were identified as potential contributors to the preservation of memory in this rare form of Alzheimers.
The National Aphasia Association describes PPA as a neurological syndrome in which language capabilities become slowly and progressively impaired. It commonly begins as a subtle disorder of language, progressing to a nearly total inability to speak, in its most severe stage, their website states.
According to the World Health Organization, deaths from dementia have doubled since 2000. Its now the fifth biggest killer worldwide.
The study is published in Neurology.
SWNS writer Mark Waghorn contributed to this report.
What Is Alzheimer’s Disease
Alzheimers disease is a brain disorder that slowly destroys memory and thinking skills and, eventually, the ability to carry out the simplest tasks. In most people with the disease those with the late-onset type symptoms first appear in their mid-60s. Early-onset Alzheimers occurs between a persons 30s and mid-60s and is very rare. Alzheimers disease is the most common cause of dementia among older adults.
The disease is named after Dr. Alois Alzheimer. In 1906, Dr. Alzheimer noticed changes in the brain tissue of a woman who had died of an unusual mental illness. Her symptoms included memory loss, language problems, and unpredictable behavior. After she died, he examined her brain and found many abnormal clumps and tangled bundles of fibers .
These plaques and tangles in the brain are still considered some of the main features of Alzheimers disease. Another feature is the loss of connections between nerve cells in the brain. Neurons transmit messages between different parts of the brain, and from the brain to muscles and organs in the body. Many other complex brain changes are thought to play a role in Alzheimers, too.
This damage initially takes place in parts of the brain involved in memory, including the entorhinal cortex and hippocampus. It later affects areas in the cerebral cortex, such as those responsible for language, reasoning, and social behavior. Eventually, many other areas of the brain are damaged.
Don’t Miss: Alzheimer’s Lack Of Neurotransmitter
Genetic Testing For Alzheimer’s Disease
A blood test can identify which APOE alleles a person has, but results cannot predict who will or will not develop Alzheimer’s disease. Currently, APOE testing is used primarily in research settings to identify study participants who may have an increased risk of developing Alzheimer’s. This knowledge helps scientists look for early brain changes in participants and compare the effectiveness of possible treatments for people with different APOE profiles.
Genetic testing is also used by physicians to help diagnose early-onset Alzheimers disease and to test people with a strong family history of Alzheimers or a related brain disease.
Genetic testing for APOE or other genetic variants cannot determine an individuals likelihood of developing Alzheimers diseasejust which risk factor genes a person has. It is unlikely that genetic testing will ever be able to predict the disease with 100 percent accuracy, researchers believe, because too many other factors may influence its development and progression.
Some people learn their APOE status through consumer genetic testing or think about getting this kind of test. They may wish to consult a doctor or genetic counselor to better understand this type of test and their test results. General information about genetic testing can be found at:
The Problem Of Alzheimers How Science Culture And Politics Turned A Rare Disease Into A Crisis And What We Can Do About It By Dr Jason Karlawish
Reviewed by David Godfrey, Senior Attorney, ABA Commission on Law and Aging
Now Available!
The Problem of Alzheimers How Science, Culture, And Politics Turned a Rare Disease Into A Crisis And What We Can Do About It, by Dr. Jason Karlawish
The PDF in which this article appears can be dowloaded here:
Listen to a brief interview with the author.
The Problem of Alzheimers is the most enlightening book about Alzheimers that I have ever read. The book explores Alzheimers, the leading cause of dementia in older adults, from the first reported case in the early 1900s, to current medical research and state of the art medical and personal care treatment for persons living with dementia and their families. Alzheimers touches the lives of virtually everyone one of us. We are all either related to someone, work with someone, or are friends with someone who either is a person living with dementia or is a caregiver of a person with dementia.
The book details clinical trials of diagnostic tools and treatments. In a very understandable way, the book explains what drugs have been tried, how the drugs were hoped to work, and what the outcome has been. Dr. Karlawish has been a part of many of the clinical trials and he knows or collaborates with most of the researchers in Alzheimers, giving him a very first person center-of-the-storm perspective on research and testing.
Entity:
Also Check: Can I Buy Jelly Drops For Dementia
What Is Known About Alzheimers Disease
Scientists do not yet fully understand what causes Alzheimers disease. There likely is not a single cause but rather several factors that can affect each person differently.
- Age is the best known risk factor for Alzheimers disease.
- Family historyresearchers believe that genetics may play a role in developing Alzheimers disease. However, genes do not equal destiny. A healthy lifestyle may help reduce your risk of developing Alzheimers disease. Two large, long term studies indicate that adequate physical activity, a nutritious diet, limited alcohol consumption, and not smoking may help people. To learn more about the study, you can listen to a short podcast.
- Changes in the brain can begin years before the first symptoms appear.
- Researchers are studying whether education, diet, and environment play a role in developing Alzheimers disease.
- There is growing scientific evidence that healthy behaviors, which have been shown to prevent cancer, diabetes, and heart disease, may also reduce risk for subjective cognitive decline. Heres 8 ways.
Myth #: Alzheimers Disease Symptoms Are Normal As We Get Older
Many people become more forgetful as they age, and some forgetfulness, such as losing things from time to time, is normal. However, common signs and symptoms of Alzheimers, such as making poor judgments and decisions a lot of the time, having problems recognizing friends and family, or losing track of the date or time of year are not a normal part of aging.
If you are worried about your memory or other possible Alzheimers symptoms, talk with your doctor. The doctor may ask questions about your health history, perform assessments of your thinking and memory, and carry out medical tests to determine your diagnosis. Learn more about the signs and symptoms of Alzheimers disease.
Recommended Reading: What Causes Senile Dementia
What Is The Burden Of Alzheimers Disease In The United States
- Alzheimers disease is one of the top 10 leading causes of death in the United States.2
- The 6th leading cause of death among US adults.
- The 5th leading cause of death among adults aged 65 years or older.3
In 2020, an estimated 5.8 million Americans aged 65 years or older had Alzheimers disease.1 This number is projected to nearly triple to 14 million people by 2060.1
In 2010, the costs of treating Alzheimers disease were projected to fall between $159 and $215 billion.4 By 2040, these costs are projected to jump to between $379 and more than $500 billion annually.4
Death rates for Alzheimers disease are increasing, unlike heart disease and cancer death rates that are on the decline.5 Dementia, including Alzheimers disease, has been shown to be under-reported in death certificates and therefore the proportion of older people who die from Alzheimers may be considerably higher.6
Aging
Identification Of Rare Variants In Alzheimers Disease
- 1Department of Psychiatry, Washington University School of Medicine, St. Louis, MO, USA
- 2Hope Center Program on Protein Aggregation and Neurodegeneration, Washington University School of Medicine, St. Louis, MO, USA
Much progress has been made in recent years in identifying genes involved in the risk of developing Alzheimers disease , the most common form of dementia. Yet despite the identification of over 20 disease associated loci, mainly through genome wide association studies , a large proportion of the genetic component of the disorder remains unexplained. Recent evidence from the AD field, as with other complex diseases, suggests a large proportion of this missing heritability may be due to rare variants of moderate to large effect size, but the methodologies to detect such variants are still in their infancy. The latest studies in the field have been focused on the identification of coding variation associated with AD risk, through whole-exome or whole-genome sequencing. Such variants are expected to have larger effect sizes than GWAS loci, and are easier to functionally characterize, and develop cellular and animal models for. This review explores the issues involved in detecting rare variant associations in the context of AD, highlighting some successful approaches utilized to date.
Also Check: Difference Between Dementia And Senility