Movement Problems And Lewy Body Dementia
Some people with LBD may not experience significant movement problems for several years. Others may have them early on. At first, movement symptoms, such as a change in handwriting, may be very mild and easily overlooked. Movement problems may include:
- Muscle rigidity or stiffness
Apda In Your Community
APDAParkinson’s Disease SymptomsLewy Bodies, Dementia, and Parkinsons What Does it all Mean?
Here are two common scenarios that may sound familiar:
Scenario 1A patient develops a series of neurologic symptoms, is evaluated by a neurologist and is told that she has Parkinsons disease . She then visits another neurologist for a second opinion and is told she has Lewy Body Dementia .
Scenario 2A patient has his first visit with his neurologist and is told that he has PD, at a subsequent visit the diagnosis is changed to Parkinsons disease dementia , and at a follow up visit the diagnosis is changed yet again to Dementia with Lewy Bodies .
Both of these situations understandably cause great uncertainty and frustration.
Difference Between Parkinsons Disease Dementia And Dementia With Lewy Bodies
Technically, the difference between these two conditions lies in how quickly the cognitive difficulties and hallucinations develop in relation to the movement issues. In DLB, the cognitive difficulties and hallucinations develop much sooner in the disease course than in PDD, sometimes even prior to the movement difficulties. Because of the similarities between PD, PDD, and DLB, current thinking in the medical community is that they should be viewed as related diseases which fall along a continuum of Lewy body disorders.
Read Also: Alzheimer’s Progression Rate
How Exactly Is Lewy Body Dementia Related To Alzheimers Disease And Parkinsons Disease
Lewy body dementia is a broad, general term for dementia in which lewy bodies are present in the brain. Dementia with lewy bodies and Parkinsons disease dementia are two related clinical disorders that make up the general broader category of Lewy body dementia. Sometimes LBD is first diagnosed as Parkinsons disease or Alzheimers disease based on its symptoms.
- Parkinsons disease dementia : You might be diagnosed with Parkinsons disease if you start out with a movement disorder typical to Parkinsons but then have your diagnosis changed to PDD when dementia symptoms develop.
- Alzheimers disease : You might start out with memory or cognitive disorder that leads to a diagnosis of AD. Over time, other distinctive symptoms begin to appear and your diagnosis is then changed to dementia with lewy bodies. Distinctive symptoms of LBD include the changes in attention, alertness and cognitive ability changes in walking and movement visual hallucinations REM sleep behavior disorder and severe sensitivity to some antipsychotics used to treat hallucinations.
Epidemiology And Natural History Of Dlb And Pdd
Approximately 12% of those aged above 65 years are diagnosed with DLB worldwide , affecting approximately 5% of all dementia cases in those over the age of 75 . Its incidence is 0.71.4 new cases/100,000 person-years or 3.5/100,000 person-years . For PDD, the cumulative prevalence is of 75% of PD patients surviving more than 10 years , 83% after 20 years , and up to 95% by age 90 years , with an overall prevalence of 31.1% and incidence rates from 0.43 to 1.13/100,000 person-years , indicating that, annually, approximately 10% of a PD population will develop dementia . The data concerning age at disease or dementia onset are highly variable. Whereas in the Olmsted County study DLB patients were younger at symptom onset than those with PDD and had more hallucinations and cognitive fluctuations, others have reported younger age at disease onset in PDD , or no essential differences between disorders .
Don’t Miss: Farts And Dementia
Genetic Study Of Lewy Body Dementia Supports Ties To Alzheimers And Parkinsons Diseases
NIH-led study locates five genes that may play a critical role in Lewy body dementia.
In a study led by National Institutes of Health researchers, scientists found that five genes may play a critical role in determining whether a person will suffer from Lewy body dementia, a devastating disorder that riddles the brain with clumps of abnormal protein deposits called Lewy bodies. Lewy bodies are also a hallmark of Parkinsons disease. The results, published in Nature Genetics, not only supported the diseases ties to Parkinsons disease but also suggested that people who have Lewy body dementia may share similar genetic profiles to those who have Alzheimers disease.
Lewy body dementia is a devastating brain disorder for which we have no effective treatments. Patients often appear to suffer the worst of both Alzheimers and Parkinsons diseases. Our results support the idea that this may be because Lewy body dementia is caused by a spectrum of problems that can be seen in both disorders, said Sonja Scholz, M.D., Ph.D., investigator at the NIHs National Institute of Neurological Disorders and Stroke and the senior author of the study. We hope that these results will act as a blueprint for understanding the disease and developing new treatments.
The study was led by Dr. Scholzs team and researchers in the lab of Bryan J. Traynor, M.D., Ph.D., senior investigator at the NIHs National Institute on Aging .
Article:
NIHTurning Discovery Into Health®
Is Dementia A Symptom Of Both
One of the biggest similarities between PD and LBD is dementia. Some studies have found that approximately 78 percent of PD patients will eventually develop dementia.4 More specifically, almost half of Parkinsons patients will develop a certain type of dementia called Parkinsons Dementia, usually 10-15 years after their initial PD diagnosis.3 People with Parkinsons Dementia commonly experience poor memory and concentration, slowed thinking, confusion, depression, emotional changes, delusions, and visual hallucinations.
Parkinsons dementia is different than LBD, mainly in which symptoms occur first . Patients with Parkinsons Dementia will first show Parkinsons motor symptoms, followed by dementia many years after diagnosis. Conversely, LBD patients will first show dementia symptoms and may show motor symptoms later.3
Read Also: Fart Prevent Cancer
Managing Sleep Disorders In Lewy Body Dementia
Sleep problems may increase confusion and behavioral problems in people with LBD and add to a caregiver’s burden. A physician can order a sleep study to identify any underlying sleep disorders such as sleep apnea, restless leg syndrome, and REM sleep behavior disorder.
REM sleep behavior disorder, a common LBD symptom, involves acting out one’s dreams, leading to lost sleep and even injuries to individuals and their sleep partners. Clonazepam, a drug used to control seizures and relieve panic attacks, is often effective for the disorder at very low dosages. However, it can have side effects such as dizziness, unsteadiness, and problems with thinking. Melatonin, a naturally occurring hormone used to treat insomnia, may also offer some benefit when taken alone or with clonazepam.
Excessive daytime sleepiness is also common in LBD. If it is severe, a sleep specialist may prescribe a stimulant to help the person stay awake during the day.
Some people with LBD have difficulty falling asleep. If trouble sleeping at night persists, a physician may recommend a prescription medication. It is important to note that treating insomnia and other sleep problems in people with LBD has not been extensively studied, and that treatments may worsen daytime sleepiness and should be used with caution. Sleep problems can also be addressed by avoiding lengthy naps, increasing daytime exercise, and avoiding caffeine, alcohol, and chocolate late in the day.
Whats The Difference Between Lewy Body Dementia Parkinsons Disease And Alzheimers Disease
Lewy body dementia is an umbrella term for two related clinical diagnoses: dementia with Lewy bodies and Parkinsons disease dementia. These disorders share the same underlying changes in the brain and very similar symptoms, but the symptoms appear in a different order depending on where the Lewy bodies first form.
Dementia with Lewy bodies is a type of dementia that causes problems with memory and thinking abilities that are severe enough to interfere with everyday activities. It specifically affects a persons ability to plan and solve problems, called executive function, and their ability to understand visual information. Dementia always appears first in DLB. The motor symptoms of Parkinsons such as tremor, slowness, stiffness and walking/balance/gait problems usually become more evident as the disease progresses. Visual hallucinations, REM sleep behavior disorder, fluctuating levels of alertness and attention, mood changes and autonomic dysfunction are also characteristic of DLB.
Finally, Alzheimers is characterized by different abnormal clumps called amyloid plaques, and jumbled fiber bundles called tau tangles. These microscopic structural changes in the brain were discovered by Dr. Alois Alzheimer in 1906. These plaques and tangles, together with loss of connections between nerve cells, contribute to loss of coherence and memory, as well as a progressive impairment in conducting normal activities of daily living.
Also Check: Smelling Farts Helps Prevent Cancer
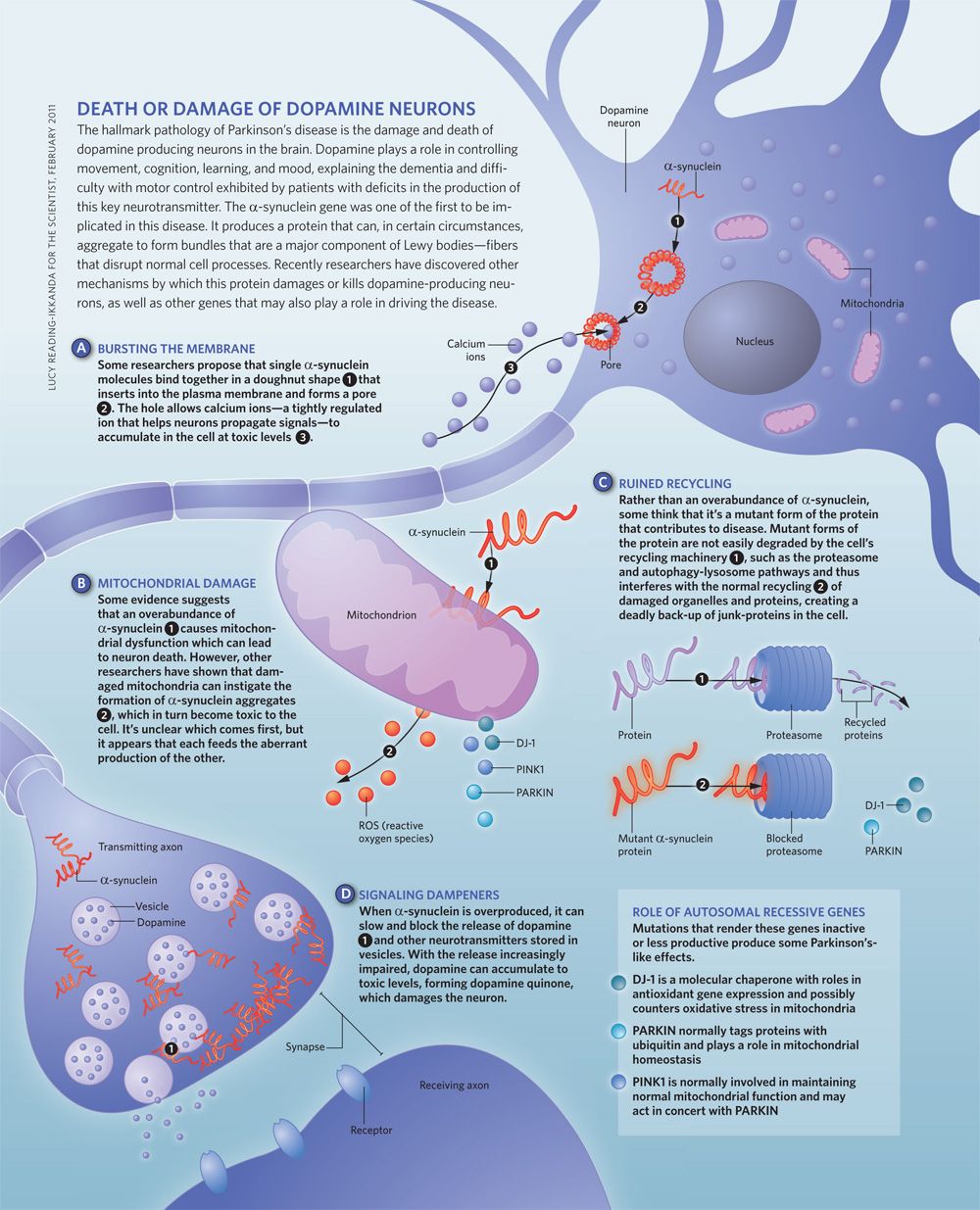
What Are The Causes Of Lewy Body Dementia
The precise cause of LBD is unknown, but scientists are learning more about its biology and genetics. For example, we know that an accumulation of Lewy bodies is associated with a loss of certain neurons in the brain that produce two important chemicals that act as messengers between brain cells . One of these messengers, acetylcholine, is important for memory and learning. The other, dopamine, plays an important role in behavior, cognition, movement, motivation, sleep, and mood.
Scientists are also learning about risk factors for LBD. A risk factor is something that may increase the chance of developing a disease. Some risk factors can be controlled while others cannot. Age is considered the greatest risk factor. No specific lifestyle factor has been proven to increase one’s risk for LBD.
Other known risk factors for LBD include certain diseases and health conditions, particularly Parkinson’s disease and REM sleep behavior disorder, which have been linked to a higher risk of LBD.
Having a family member with LBD also may increase a person’s risk, though LBD is not considered a genetic disease. Variants in three genes APOE, SNCA, and GBA have been associated with an increased risk, but in most cases, the cause is unknown.
Parkinsons Disease With Dementia Versus Dementia With Lewy Bodies
Some patients with Parkinsons disease experience no or only subtle cognitive decline, and their primary limitation is their motor disorder. However, other patients with Parkinsons disease develop dementia as a consequence of the disease. When dementia develops after an established motor disorder, we call the disease Parkinsons disease with dementia . In contrast, when dementia develops prior to or at the same time as the motor disorder, we call the disease DLB. Although the initial sequence of symptoms differs in PDD and DLB, as the disorders progress, the symptoms and the underlying brain changes are much more similar than they are different. As such, many researchers and clinicians think of PDD and DLB as being on a continuum of a similar disease process rather than as two distinct entities.
You May Like: Alzheimer Awareness Ribbon
Pathophysiology Of Cognitive Impairment
The neurobiological basis for cognitive impairment in DLB and PDD is multifocal, related to a synergistic effect of both Syn/LB and AD pathologies and dysfunction of dopaminergic, noradrenalinergic, serotonergic, and cholinergic systems . The emergence of PDD and DLB occurs on the background of severe dopamine deficits and correlates with a marked loss of limbic and cortically projecting dopamine, noradreanaline, serotonin, and ACh neurons. The relationship between these lesions is not yet fully understood.
Severe pathology also involves the noradrenergic locus ceruleus and the serotonergic dorsal raphe nucleus as well as the ventral tegmental area not always associated with coincidental AD lesions . LC neuronal loss and the accompanying norepinephrinergic deficiency are an important cause and pharmacological target for the treatment of PD/PDD/DLB . The prominent role of serotonergic degeneration also involving the anterior caudate nucleus, the orbitofrontal and cingulate cortex for neuropsychiatric symptoms in PD , emphasizes its important role in both PDD and DLB, and stimulates new insight into novel treatments by modulating 5-HT receptors .
What Causes Lewy Body Dementia
The causes of LBD are not yet well understood, but research is ongoing in this area. There are probably multiple factors involved, including genetic and environmental risk factors that combine with natural aging processes to make someone susceptible to LBD.
For more information, visit www.lbda.org.
Modified with permission from the Lewy Body Dementia Association
To learn more about motor symptoms related to Parkinsons, visit here.
To learn more about non-motor symptoms related to Parkinsons, visit here.
Don’t Miss: Does Prevagen Help Dementia
Tests For Dementia With Lewy Bodies
There’s no single test for dementia with Lewy bodies.
The following may be needed to make a diagnosis:
- an assessment of symptoms for example, whether there are typical symptoms of dementia with Lewy bodies
- an assessment of mental abilities this will usually involve a number of tasks and questions
- blood tests to rule out conditions with similar symptoms
- brain scans, such as an MRI scan, CT scan or a SPECT scan these can detect signs of dementia or other problems with the brain
What You Need To Know
- Lewy body dementia is a form of progressive dementia that affects a persons ability to think, reason, and process information.
- Diagnosing Lewy body dementia can be challenging an estimated 1.4 million Americans are living with the disease.
- LBD has three features that distinguish it from other forms of dementia:
- Fluctuating effects on mental functioning, particularly alertness and attention, which may resemble delirium
- Recurrent visual hallucinations
- Parkinson-like movement symptoms, such as rigidity and lack of spontaneous movement.
Lewy bodies are clumps of abnormal protein particles that, for reasons that are not fully understood, accumulate in the brain. These deposits cause a form of dementia called Lewy body dementia, or LBD which is what the late actor and comedian Robin Williams suffered from.
LBD is not the same as Parkinsons, but the two are closely related: LBD causes some or all of the motor symptoms of Parkinsons. More than 1 million people in the U.S. are affected by Lewy body dementia, according to the Lewy Body Dementia Association.
You May Like: Does Diet Coke Cause Alzheimer’s
How Does Lewy Body Disease Progress
Lewy body disease differs from Alzheimer’s disease in that the progression of the disease is usually more rapid. However, like Alzheimer’s disease it is a degenerative condition, eventually leading to complete dependence. Death is usually a result of another illness, such as pneumonia or an infection. The average lifespan after the onset of symptoms is about seven years.
How Is Lewy Body Dementia Diagnosed
There isn’t one test that can diagnose LBD. It is important to see an experienced doctor to get a diagnosis. This would usually be specialist such as a neurologist. The doctor will:
- Do a medical history, including taking a detailed account of the symptoms. The doctor will talk to both the patient and caregivers.
- Do physical and neurological exams
- Do tests to rule out other conditions that could cause similar symptoms. These could include blood tests and brain imaging tests.
- Do neuropsychological tests to evaluate memory and other cognitive functions
LBD can be hard to diagnose, because Parkinson’s disease and Alzheimer’s disease cause similar symptoms. Scientists think that Lewy body disease might be related to these diseases, or that they sometimes happen together.
It’s also important to know which type of LBD a person has, so the doctor can treat that type’s particular symptoms. It also helps the doctor understand how the disease will affect the person over time. The doctor makes a diagnosis based on when certain symptoms start:
- If cognitive symptoms start within a year of movement problems, the diagnosis is dementia with Lewy bodies
- If cognitive problems start more than a year after the movement problems, the diagnosis is Parkinson’s disease dementia
Read Also: Colors For Alzheimer’s Awareness
What Happens In Dlb
People with DLB may have trouble focusing, remembering things, staying awake during the day, or staying asleep at night. They may become more frustrated or confused because of the lack of sleep. They may also hallucinate and see people, objects, or animals that are not there.
Some people with DLB will need help with walking, while others may have hunched posture or trouble using their hands and feet because of stiff muscles. People with DLB may appear to be better and need less help on some days, only to become worse and more confused again and need more help the next day or in a few days. This is because their energy level and focus will vary.
DLB is a disease that changes with time. A person with DLB can live for many years with the disease. Research suggests that a person with DLB may live an average of 57 years with the disease, although this can vary from person to person.
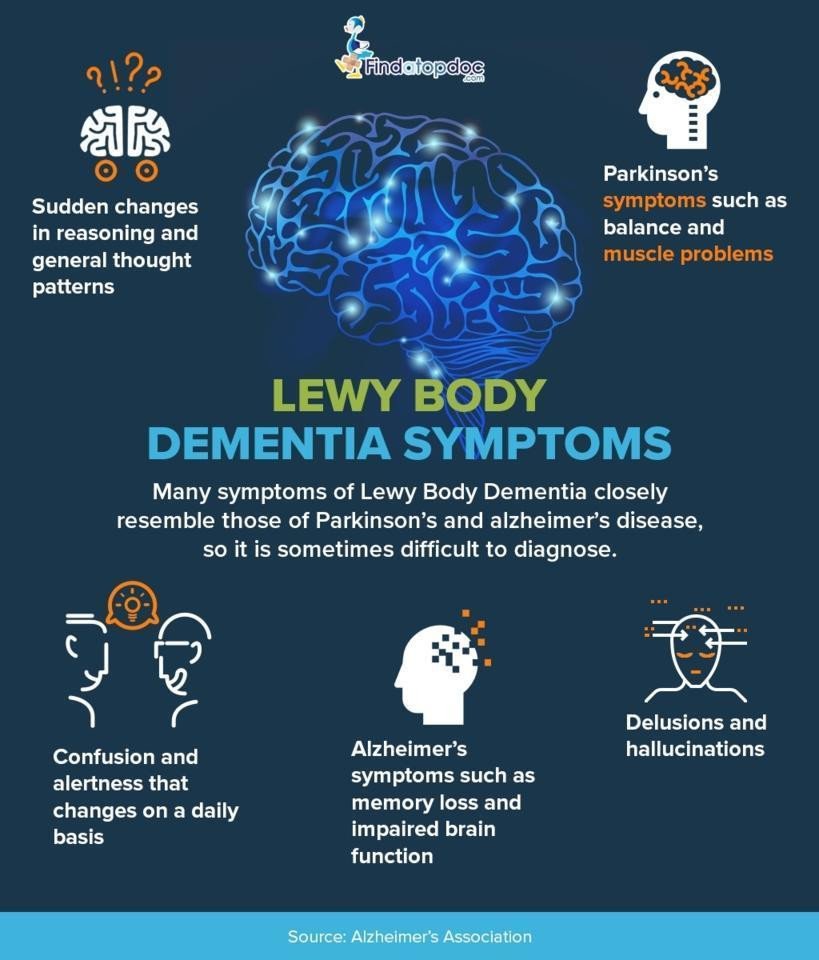
What Are The Symptoms
The symptoms of dementia with Lewy body disease include:
- Difficulty with concentration and attention
- Extreme confusion
- Difficulties judging distances, often resulting in falls.
There are also three cardinal symptoms, two of which must be present in order to make the diagnosis:
- Visual hallucinations
- Parkinsonism
- Fluctuation in mental state so that the person may be lucid and clear at one time and confused, disoriented and bewildered at other times. Typically this fluctuation occurs over a period of hours or even minutes and is not due to any underlying acute physical illness.
Some people who have Lewy body disease may also experience delusions and/or depression.
You May Like: Etiology Of Alzheimer’s
Lewy Body Dementia Vs Parkinsons Disease Dementia
Diagnoses of Lewy body dementia include dementia with Lewy bodies and Parkinsons disease dementia. Symptoms in both of these diagnoses can be similar.
Lewy body dementia is a progressive dementia caused by abnormal deposits of a protein called alpha-synuclein in the brain. Lewy bodies are also seen in Parkinsons disease.
The overlap in symptoms between Lewy body dementia and Parkinsons disease dementia include movement symptoms, rigid muscles, and problems with thinking and reasoning.
This seems to indicate that they could be linked to the same abnormalities, though more research is needed to confirm that.
The later stages of Parkinsons disease have more severe symptoms that may require help moving around, around-the-clock care, or a wheelchair. Quality of life can decline rapidly.
Risks of infection, incontinence, pneumonia, falls, insomnia, and choking increase.
Hospice care, memory care, home health aides, social workers, and support counselors can be a help in later stages.
Parkinsons disease itself isnt fatal, but complications can be.
Research has shown a median survival rate of about