How Can I Ensure My Wishes Are Followed When I Cant Choose Myself
If you have an early diagnosis of frontotemporal dementia of any kind, you may want to talk to your healthcare provider, your family or loved ones, and to anyone you trust to make important decisions for you. These discussions are important because they can help you ensure caregivers can honor your wishes if you cant choose for yourself in the future.
While these conversations often feel unpleasant or difficult, having them sooner rather than later can help avoid confusion about what you want for yourself in the years to come. They also mean your loved ones don’t face the painful, difficult situation of having to guess what you wanted.
In addition to those conversations, you should also put your wishes and decisions in writing. That includes preparing documents connected to legal issues and what happens if you can’t care for yourself or make decisions for your care or well-being. Many people choose to consult an attorney when preparing these documents. However, many of these are ones you can prepare on your own .
How Is Frontotemporal Dementia Treated
Currently, no treatments are available to cure or slow the progression of FTD, but healthcare providers may prescribe medicine to treat symptoms. Antidepressants may help treat anxiety and control obsessive-compulsive behaviors and other symptoms. Prescription sleeping aids can help ease insomnia and other sleep disturbances. Antipsychotic medicine may reduce irrational and compulsive behaviors.
Behavior modification may help control unacceptable or risky behaviors.
Speech and language pathologists and physical and occupational therapists can help adjustment to some of the changes caused by FTD.
Blood And Csf Biomarkers
The fluid biomarker field in genetic FTD has yet to identify many robust measures, e.g. neither CSF nor blood assays of tau or TDP-43 are yet to yield FTD-specific markers. However, recent work has identified three markers which will play an important role in forthcoming trials: neurofilament light chain , progranulin and poly dipeptide repeat proteins .
Increased NfL levels reflect axonal damage and appear to be a measure of disease intensity, and predict progression and survival in genetic FTD . Levels are highest in C9orf72-associated ALS and lowest in MAPT mutation carriers . Longitudinal analysis of samples seems to suggest that levels change not long prior to symptom onset in genetic FTD, increasing by three- to fourfold during conversion . Whilst an increase in NfL is not specific for FTD, and levels are increased in multiple neurological diseases, evidence from other diseases suggests that a decrease in levels could be a measure of successful disease modification in trials .
Low serum, plasma or CSF progranulin levels have almost perfect sensitivity and specificity for detecting pathogenic GRN mutations . Levels are low from the earliest time period of presymptomatic genetic FTD that they have been measured and are relatively stable over time . CSF and plasma levels are relatively poorly correlated will be a key biomarker for disease-modifying trials in GRN carriers.
Don’t Miss: Does Vitamin E Help Dementia
Signs And Symptoms Of Frontotemporal Dementia
There are several different types of frontotemporal dementia, with symptoms depending on which areas of the brain are affected first.
Frontotemporal dementia is progressive and affects everyone differently. This means that symptoms may be mild at first but will worsen over time.
Each type of frontotemporal dementia has its own signs and symptoms.
Behavioural-variant frontotemporal dementia
When the frontal lobes are affected first, the main changes are in personality and behaviour: this is known as behavioural-variant frontotemporal dementia. In this type of frontotemporal dementia, areas of the brain that control conduct, judgement, empathy and foresight are damaged.
Symptoms vary from person to person, depending on which areas of the frontal lobes are damaged. Some people become apathetic, while others become disinhibited some may alternate between apathy and disinhibition.
Common symptoms can include:
- repetitive motor behaviours such as collecting, counting and tapping.
Primary progressive aphasia
When the temporal lobes are affected first, there is a loss of language skills: this is known as primary progressive aphasia. In this type of frontotemporal dementia, other aspects of thinking, perception and behaviour are not affected as much in the early stages.
There are two more common types of frontotemporal dementia where language is impaired:
Semantic dementia
Symptoms of semantic dementia include:
Progressive non-fluent aphasia
Symptoms vary, but include:
How Genetic Counseling Works
The genetic counselors at InformedDNA working on this program are highly trained in hereditary neurological conditions. As part of this program, individuals will receive initial and post-test genetic counseling over the phone. Check out our easy-to-understand patient brochure.
At the initial appointment, the genetic counselor will:
Collect the individuals medical history and a 3-4 generation family history
Discuss the genetics of FTD
Review the benefits and limitations of genetic testing
If the individual elects to proceed with genetic testing, then the genetic counselor will coordinate the test order and sample collection
Results will be available in approximately three weeks from when the lab receives the sample
At the post-test appointment, the genetic counselor will:
Review the individuals genetic test result and implications for personal health and risks to family members
Provide a written summary of the discussion and a copy of the genetic test result to the individual
Because our appointments occur over the phone, family members or friends may participate in the call, regardless of location.
This testing program is sponsored by Passage Bio. No personal identifying information of individuals participating in this genetic counseling and testing program will be shared with Passage Bio.
You May Like: Does Medicaid Pay For Nursing Home For Alzheimer’s
Imaging Data Acquisition And Preprocessing
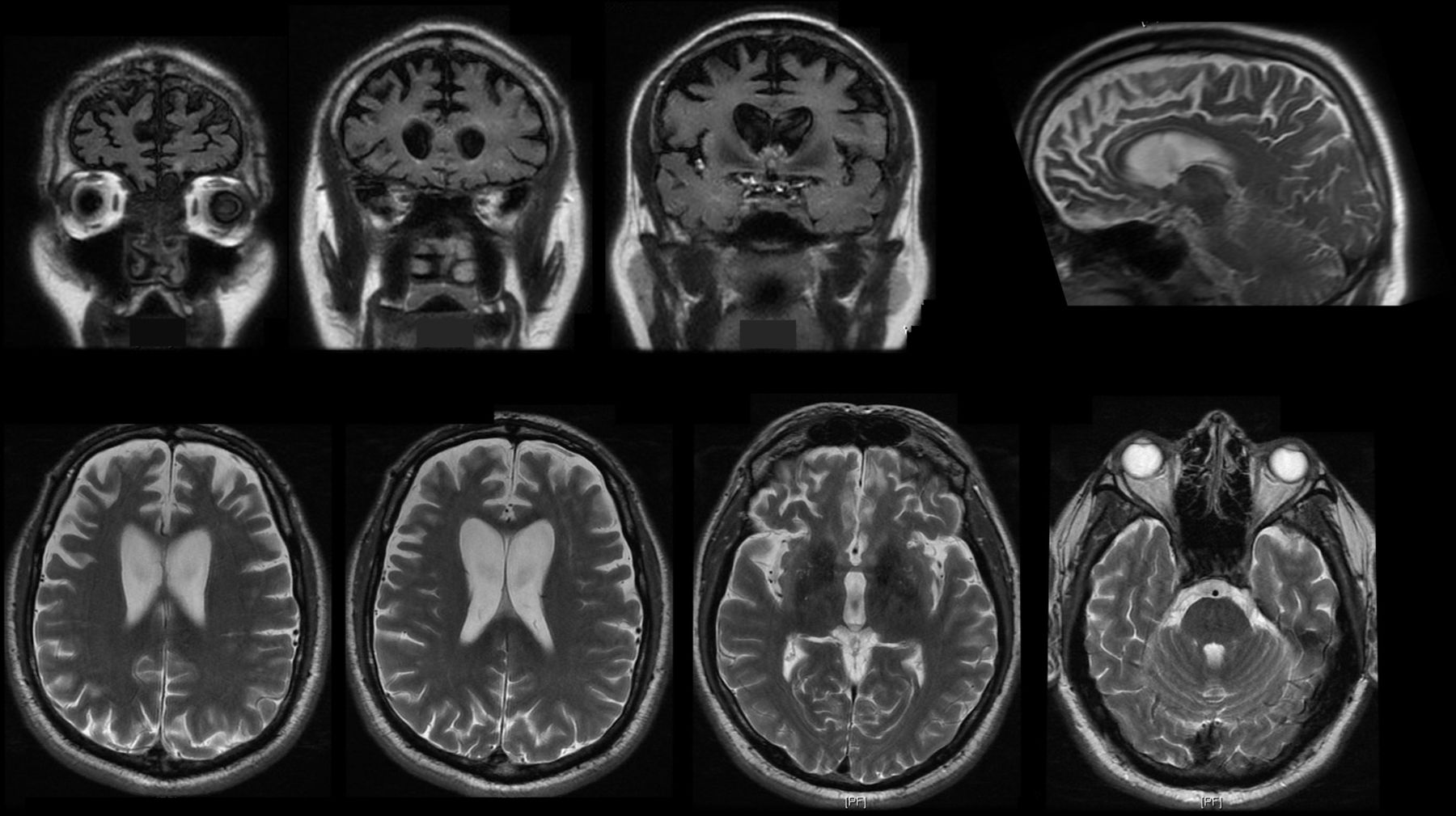
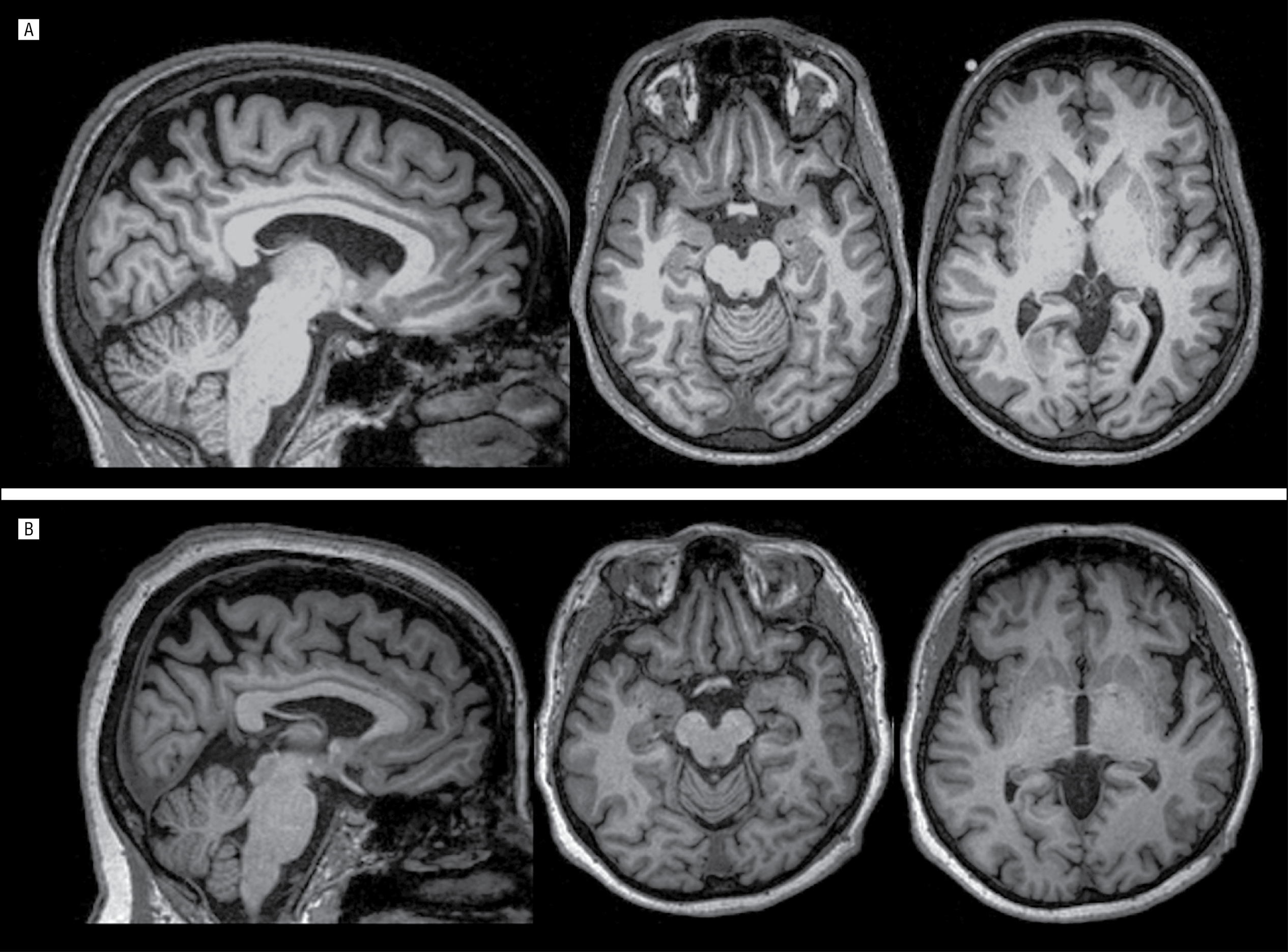
In DataFreeze 4, 573 out of 600 participants included in this study had at least one volumetric T1-weighted MRI scan on 3T within 2 years of follow-up. Magnetization Prepared Rapid Gradient Echo images were acquired at each site accommodating different manufacturers and field strengths. Gray matter regional volumes were extracted from the subcortical segmentation and cortical parcellation labeled by the Desikan-Killiany Atlas in Freesurfer 6.0 . For cases with more than one scan, all available follow-up images were included in the processing with the longitudinal stream in Freesurfer, creating an unbiased within-subject template for case-specific segmentation. Regional volumes were combined into bilateral frontal, temporal , parietal and occipital lobes, insula cortex, cingulate cortex, subcortical central structures , and brainstem. Carriers volumes were z-scored with reference to non-carriers. Total intracranial volume was estimated as the sum of gray matter, white matter, and cerebrospinal fluid segmentations using the Computational Anatomy Toolbox within Statistical Parametric Mapping software . CAT12 also provides imaging quality ratings considering noise, motion, and spatial resolution. Raw and parcellated data were visually inspected, and images with significant artifacts, or parcellation failure were excluded, such that all scans included in the analyses had CAT12 imaging quality ratings higher than 74/100 .
Diagnosing Frontal Lobe Dementia
No one test is able to diagnose frontal lobe dementia. Instead physicians are able to use the balance of evidence to diagnose frontal lobe dementia based on their best judgment. Because there is no foolproof test and diagnosis depends on the physicians knowledge, judgment, and observation of the patient, frontal lobe dementia is notoriously difficult to diagnose in its early stages. Although as the disease progresses, it becomes easier to definitely distinguish it between other disorders.
Recommended Reading: Can People With Dementia Drive
History Of Frontotemporal Dementia
In 1892, Arnold Pick, a neuropsychiatrist at the University of Prague, made the first description of frontotemporal dementia . In his case report, On the relationship between senile atrophy of the brain and aphasia, he described a 71-year-old man who developed progressive aphasia and apraxia. Upon autopsy, the patient’s brain showed asymmetric atrophy.
Pathologically, FTD is associated with atrophy of the frontal and/or temporal lobes, gliosis, neuronal swelling, and eventual microvacuolation., Pick bodies are hyperphosphorylated tau accumulations in the neuronal cytoplasm, which may be found with silver staining but are not pathognomonic for the disease. TAR DNAbinding proteins are hyperphosphorylated, ubiquinated, cleaved proteins and are the most commonly found neuropathology in FTD.
FTD is an uncommon disease compared with other neurodegenerative disorders such as Alzheimer disease. However, in presenile dementia, FTD incidence is similar to that of Alzheimer disease. In a study of 5059-year-old patients in Rochester, Minnesota, incidence of FTD cases and Alzheimer cases were both found to be 3.3/100,000 person years. In Cambridge, United Kingdom, FTD incidence was found to be 3.5/100,000 person years, whereas Alzheimer disease incidence was 4.2/100,000 person years. Although FTD is considered a presenile dementia, 20%25% of patients with FTD are older than 65 years. The median survival is 6 ± 1.1 years.,
Clinical Diagnostic Criteria For Ftd: Strengths And Limitations
The most recently revised consensus criteria for the clinical diagnosis of bvFTD are those by Rascovsky et al. . In this hierarchical framework, three levels of diagnostic certainty are distinguished. The first degree determines whether or not the term possible bvFTD is appropriate and is based upon presence of core symptoms alone. For probable and definite bvFTD, results of imaging and histopathology/DNA analysis, respectively, are taken into account. The consensus criteria for possible bvFTD have a sensitivity of 8595% and a specificity of 82%, irrespective of the underlying proteinopathy . For probable bvFTD, sensitivity and specificity values are 7585 and 95%, respectively . A higher sensitivity is reached in early onset dementia compared with late onset, as in younger age groups there is significantly more disinhibition, loss of empathy and compulsive behavior . False positive diagnoses are most common in patients with a later onset, an absence of family history for dementia and a more apathetic presentation. They mainly turn out to be AD upon neuropathological examination .
Several other clinical tools exist to measure frontal lobe dysfunction and therefore differentiate between FTD and AD. Many assessment batteries of neurobehavioral symptoms, such as the Schedules for Clinical Assessment in Neuropsychiatry , the Scale for Emotional Blunting , the Middelheim Frontality Score and the Frontal Behavior Inventory have a good discriminative ability .
Don’t Miss: How Is Frontotemporal Dementia Different From Alzheimer’s
Less Common Ftd Genes
CHMP2B
CHMP2B, located at chromosome 3p11.2, encodes a component of the heteromeric ESCRT-III complex with functions in the endosomallysosomal and the autophagic protein degradation pathway . Rare mutations were identified that resulted in a premature stop codon and C-truncating of the protein . Neuropathologically, CHMP2B carriers are associated with FTLD-UPS proteinopathy .
Clinically, CHMP2B carriers present commonly with bvFTD with early personality changes, frequently represented by less concern for others, an unkempt appearance, disinhibition, inappropriate emotional responses and restlessness which later can be accompanied by aggression. Apathy, hyperorality and motor symptoms such as parkinsonism, dystonia, pyramidal signs, and myoclonus occur later. MND is typically not present, although some cases have been reported . PPA syndromes have been described as well . The average onset age is 58 years, ranging between 46 and 65 years .
VCP
VCP, located on chromosome 9 at 9p13.3, is associated with impaired functioning of an ATPase with a wide range of cellular functions. This impairment is due to missense mutations, of which > 30 have been identified so far . Pathogenesis may occur because of a disturbance in the ubiquitinproteasome mediated protein degradation, autophagy, or both . The associated neuropathological correlation is FTLD-TDP type D .
Genetic Testing And Counselling
In families where a gene abnormality is known or suspected, expert genetic advice is important.
If someone is worried about their risk of developing familial FTD or wishes to discuss it further, their GP will be able to refer them to a specialist genetic counselling service to discuss their concerns and arrange genetic testing if needed.
The results of any genetic test have important implications not only for the person being tested but also for the rest of the family. It is important to discuss these carefully with a specialist who has expertise in genetic counselling and is familiar with the family, before any genetic tests are performed.
A genetic test for FTD can be performed on a blood sample and is usually done because several other family members have FTD or an associated disorder. However, it may also be performed when symptoms or brain scans suggest familial FTD. For more detailed information on genetic testing and counselling for FTD, please our I think I am at risk of fFTD. What next? page.
Living with fFTD: A short film
I think I am at risk of fFTD. What next?
Living with fFTD
Don’t Miss: Do Brain Games Help Prevent Alzheimer’s
Behavioral Variant Frontotemporal Dementia
Behavioral variant frontotemporal dementia was previously known as Pick’s disease, and is the most common of the FTD types. BvFTD is diagnosed four times as often as the PPA variants. Behavior can change in BvFTD in either of two waysit can change to being impulsive and disinhibited, acting in socially unacceptable ways or it can change to being listless and apathetic. About 1213% of people with bvFTD develop motor neuron disease.
The Pick bodies in behavioral variant FTD are spherical inclusion bodies found in the cytoplasm of affected cells. They consist of tau fibrils as a major component together with a number of other protein products including ubiquitin and tubulin.
Living With Frontotemporal Dementia
Coping with FTD can be frightening, frustrating, and embarrassing for the patient and family members. Since some symptoms cant be controlled, family members shouldn’t take their loved ones behaviors personally. Families need to maintain their own well-being, while ensuring that their loved one is treated with dignity and respect.
Caregivers should learn all they can about FTD and gather a team of experts to help the family meet the medical, financial, and emotional challenges they are facing.
Its important to find a healthcare provider knowledgeable about FTD. Other healthcare specialists who may play a role on the team are home care nurses, neuropsychologists, genetic counselors, speech and language therapists, as well as physical and occupational therapists. Social workers can help the patient and caregivers find community resources, such as medical supplies and equipment, nursing care, support groups, respite care, and financial assistance.
Attorneys and financial advisors can help families prepare for the later stages of the disease.
Advanced planning will help smooth future transitions for the patient and family members, and may allow all to participate in the decision-making process.
Recommended Reading: Can You Work With Dementia
Treatments For Frontotemporal Dementia
There’s currently no cure for frontotemporal dementia or any treatment that will slow it down.
But there are treatments that can help control some of the symptoms, possibly for several years.
Treatments include:
- medicines to control some of the behavioural problems
- therapies such as physiotherapy, occupational therapy, and speech and language therapy for problems with movement, everyday tasks and communication
- dementia activities such as memory cafes, which are drop-in sessions for people with memory problems and their carers to get support and advice
- support groups who can offer tips on managing symptoms from dementia experts and people living with frontotemporal dementia, and their families
How Is It Treated And Is There A Cure
FTD is not curable, and there’s no way to treat it directly. Its also impossible to slow the progress of the disease. Healthcare providers may recommend treating some of the symptoms, but this can vary from case to case. Your healthcare provider is the best person to tell you what treatments if any they recommend.
Also Check: How Do You Know If You Have Alzheimer’s Disease
Subtypes And Related Disorders
The main subtypes of frontotemporal dementia are behavioral variant FTD, semantic dementia, progressive nonfluent aphasia, and FTD associated with amyotrophic lateral sclerosis . Two distinct rare subtypes are neuronal intermediate filament inclusion disease, and basophilic inclusion body disease. Related disorders are corticobasal syndrome, and progressive supranuclear palsy.
What Is The Life Expectancy Of Ftd
The average life expectancy after a diagnosis of FTD is 7.5 years. But the condition can progress faster or slower. Your healthcare provider is the best person to tell you more about the progress of the disease and the likely timeline. They can also update you throughout the course of the disease if it progresses faster or slower than expected.
Also Check: Can Tinnitus Lead To Alzheimer’s
How Is Frontal Lobe Dementia Diagnosed
Diagnosing this group of disorders can be difficult because the behavior and language changes can mimic psychiatric disorders and the movement impairments can mimic other degenerative neurologic conditions. Unless an individual has an inherited form of the disease and can be tested for one of the known mutations, the diagnosis is made by taking a detailed personal and medical history , performing a thorough physical exam, obtaining laboratory testing to rule out metabolic causes of dementia, and using imaging studies to identify abnormalities in the frontal or temporal lobes.
Magnetic resonance imaging can reveal structural abnormalities and positron emission tomography or single photon emission computed tomography can evaluate activity, including glucose and oxygen usage, in these areas of the brain.
What Is The Outlook For Frontotemporal Dementia
In the early stages, the symptoms and signs of frontotemporal dementia can be cared for and treated with good results. Late-stage frontotemporal dementia can take years to develop. As the disease progresses, 24-hour care may become necessary.
Frontotemporal dementia shortens a persons life span. The condition will eventually cause a person to have difficulty with bodily functions such as:
- swallowing
Also Check: Does Vascular Dementia Come And Go
Clinical And Neurochemical Testing
All patients underwent detailed neuropsychological examination. Disease severity was assessed using the FTLDspecific Clinical Dementia Rating score . CSF was collected to determine Tau, phosphorylated Tau , Amyloid-beta , as well as CSF PGRN, phosphorylated neurofilament heavy chain , and NfL levels. Data on these biomarkers was available in 226, 180, 224, 173, 187, and 166 individuals, respectively. In addition, blood samples were collected to measure serum NfL and serum PGRN as previously described . Data on these biomarkers was available in 201 and 75 subjects, respectively.
Family history was assessed using the query, Are there any neuropsychiatric disorders in your family up to the grand-parental generation?. Neuropsychiatric disorders included dementia, amyotrophic lateral sclerosis , Parkinson syndromes, psychosis, depression, and suicide. Information on the family history was available for a total of 385 cases.