Common Forms Of Dementia
There are many different forms of dementia. Alzheimer’s disease is the most common form and may contribute to 60-70% of cases. Other major forms include vascular dementia, dementia with Lewy bodies , and a group of diseases that contribute to frontotemporal dementia . Dementia may also develop after a stroke or in the context of certain infections such as HIV, harmful use of alcohol, repetitive physical injuries to the brain or nutritional deficiencies. The boundaries between different forms of dementia are indistinct and mixed forms often co-exist.
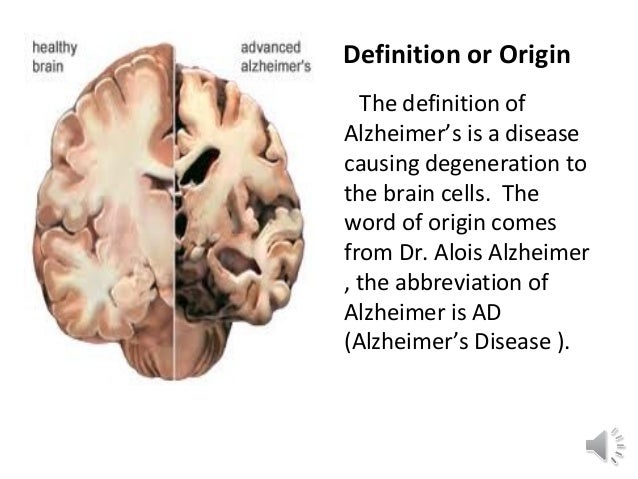
What Are The Stages Of Alzheimers
Alzheimers disease slowly gets worse over time. People with this disease progress at different rates and in several stages. Symptoms may get worse and then improve, but until an effective treatment for the disease itself is found, the persons ability will continue to decline over the course of the disease.
Early-stage Alzheimers is when a person begins to experience memory loss and other cognitive difficulties, though the symptoms appear gradual to the person and their family. Alzheimers disease is often diagnosed at this stage.
During middle-stage Alzheimers, damage occurs in areas of the brain that control language, reasoning, sensory processing, and conscious thought. People at this stage may have more confusion and trouble recognizing family and friends.
In late-stage Alzheimers, a person cannot communicate, is completely dependent on others for care, and may be in bed most or all the time as the body shuts down.
How long a person can live with Alzheimers disease varies. A person may live as few as three or four years if he or she is older than 80 when diagnosed, to as long as 10 or more years if the person is younger. Older adults with Alzheimers disease need to know their end-of-life care options and express their wishes to caregivers as early as possible after a diagnosis, before their thinking and speaking abilities fail.
How Long Can A Person Live With Alzheimers Disease
The time from diagnosis to death varies as little as three or four years if the person is older than 80 when diagnosed, to as long as 10 or more years if the person is younger.
Alzheimers disease is currently ranked as the sixth leading cause of death in the United States, but recent estimates indicate that the disorder may rank third, just behind heart disease and cancer, as a cause of death for older people.
Currently, there is no cure for Alzheimers disease, though there has been significant progress in recent years in developing and testing new treatments. Several medicines have been approved by the U.S. Food and Drug Administration to treat people with Alzheimers.
Read Also: Bob Knight Health Condition
Medications To Treat The Underlying Alzheimer’s Disease Process
Aducanumab is the first disease-modifying therapy approved by the FDA to treat Alzheimers disease. The medication helps to reduce amyloid deposits in the brain and may help slow the progression of Alzheimers, although it has not yet been shown to affect clinical outcomes such as progression of cognitive decline or dementia. A doctor or specialist will likely perform tests, such as a PET scan or analysis of cerebrospinal fluid, to look for evidence of amyloid plaques and help decide if the treatment is right for the patient.
Aducanumab was approved through the FDAs Accelerated Approval Program. This process requires an additional study after approval to confirm the anticipated clinical benefit. If the follow-up trial fails to verify clinical benefit, the FDA may withdraw approval of the drug. Results of the phase 4 clinical trial for aducanumab are expected to be available by early 2030.
Several other disease-modifying medications are being tested in people with mild cognitive impairment or early Alzheimers as potential treatments.
Vascular Dementia And Vascular Cognitive Impairment
Vascular dementia occurring with AD is common, but pure vascular dementia appears to be uncommon . A full review of the management of dementia with a cerebrovascular component was developed in Canada in the Third CCCD and was presented by Bocti, Black, and Frank . There are both conceptual and pragmatic difficulties in trying to portray vascular dementia as a distinct entity. Of the criteria now in use, the National Institute of Neurological Disorders and Stroke-Association Internationale pour la Recherché et l’Enseignement en Neurosciences criteria and the Alzheimer’s Disease Diagnostic and Treatment Centers criteria have been especially influential but each set has limitations. In practice, most criteria are insensitive and different sets of criteria give differing estimates of who has vascular dementia . Vascular lesions are found in many dementia patients, including those with otherwise classical AD, where they are often detected only by routine neuroimaging. On the contrary, patients with only vascular pathology as the cause of their dementia have been uncommon in many series . Most patients have mixed pathology, so that patients with vascular lesions commonly have evidence of other neuro degenerative disorders . One should also note that many patients with positive imaging do not have a stroke history, implying a high occurrence of silent strokes.
Also Check: Does Bob Knight Have Alzheimer’s
How Alzheimer’s Disease Is Treated
There’s currently no cure for Alzheimer’s disease, but medicines are available that can help relieve some of the symptoms.
Various other types of support are also available to help people with Alzheimer’s live as independently as possible, such as making changes to your home environment so it’s easier to move around and remember daily tasks.
Psychological treatments such as cognitive stimulation therapy may also be offered to help support your memory, problem solving skills and language ability.
Read more about treating Alzheimer’s disease.
What Is Known About Alzheimers Disease
Scientists do not yet fully understand what causes Alzheimers disease. There likely is not a single cause but rather several factors that can affect each person differently.
- Age is the best known risk factor for Alzheimers disease.
- Family historyresearchers believe that genetics may play a role in developing Alzheimers disease. However, genes do not equal destiny. A healthy lifestyle may help reduce your risk of developing Alzheimers disease. Two large, long term studies indicate that adequate physical activity, a nutritious diet, limited alcohol consumption, and not smoking may help people. To learn more about the study, you can listen to a short podcast.
- Changes in the brain can begin years before the first symptoms appear.
- Researchers are studying whether education, diet, and environment play a role in developing Alzheimers disease.
- There is growing scientific evidence that healthy behaviors, which have been shown to prevent cancer, diabetes, and heart disease, may also reduce risk for subjective cognitive decline. Heres 8 ways.
You May Like: What’s The Difference Between Parkinson’s And Alzheimer’s
Alzheimers Disease Vs Other Types Of Dementia
Dementia is an umbrella term for a range of conditions that involve a loss of cognitive functioning.
Alzheimers disease is the most common type of dementia. It involves plaques and tangles forming in the brain. Symptoms start gradually and are most likely to include a decline in cognitive function and language ability.
To receive a diagnosis of Alzheimers, a person will be experiencing memory loss, cognitive decline, or behavioral changes that are affecting their ability to function in their daily life.
Friends and family may notice the symptoms of dementia before the person themselves.
There is no single test for Alzheimers disease. If a doctor suspects the presence of the condition, they will ask the person and sometimes their family or caregivers about their symptoms, experiences, and medical history.
The doctor may also carry out the following tests:
- cognitive and memory tests, to assess the persons ability to think and remember
- neurological function tests, to test their balance, senses, and reflexes
- blood or urine tests
- a CT scan or MRI scan of the brain
- genetic testing
A number of assessment tools are available to assess cognitive function.
In some cases, genetic testing may be appropriate, as the symptoms of dementia can be related to an inherited condition such as Huntingtons disease.
Some forms of the APOE e4 gene are associated with a higher chance of developing Alzheimers disease.
Is There Treatment Available
At present there is no cure for Alzheimer’s disease. However, one group of drugs called cholinergeric drugs appears to be providing some temporary improvement in cognitive functioning for some people with mild to moderate Alzheimer’s disease.
Drugs can also be prescribed for secondary symptoms such as restlessness or depression or to help the person with dementia sleep better.
Community support is available for the person with Alzheimer’s disease, their families and carers. This support can make a positive difference to managing dementia. Dementia Australia provides support, information and counselling for people affected by dementia. Dementia Australia also aims to provide up-to-date information about drug treatments.
Further help
For more information contact the National Dementia Helpline on 1800 100 500.
For a range of books and videos contact our Library.
For advice, common sense approaches and practical strategies on the issues most commonly raised about dementia, read our Help Sheets.
Recommended Reading: Aphasia Alzheimer’s Disease
Epigenetic Age Analysis Of Different Brain Regions
The is the youngest brain region in centenarians according to an epigenetic biomarker of tissue age known as : it is about 15 years younger than expected in a centenarian. By contrast, all brain regions and brain cells appear to have roughly the same epigenetic age in subjects who are younger than 80. These findings suggest that the cerebellum is protected from aging effects, which in turn could explain why the cerebellum exhibits fewer neuropathological hallmarks of age related dementias compared to other brain regions.
Emotion And Behavior Treatments
The emotional and behavioral changes linked with Alzheimers disease can be challenging to manage. People may increasingly experience irritability, anxiety, depression, restlessness, sleep problems, and other difficulties.
Treating the underlying causes of these changes can be helpful. Some may be side effects of medications, discomfort from other medical conditions, or problems with hearing or vision.
Identifying what triggered these behaviors and avoiding or changing these things can help people deal with the changes. Triggers may include changing environments, new caregivers, or being asked to bathe or change clothes.
It is often possible to change the environment to resolve obstacles and boost the persons comfort, security, and peace of mind.
The Alzheimers Association offer a list of helpful coping tips for caregivers.
In some cases, a doctor may recommend medications for these symptoms, such as:
- antidepressants, for low mood
develops due to the death of brain cells. It is a neurodegenerative condition, which means that the brain cell death happens over time.
In a person with Alzheimers, the brain tissue has fewer and fewer nerve cells and connections, and tiny deposits, known as plaques and tangles, build up on the nerve tissue.
Plaques develop between the dying brain cells. They are made from a protein known as beta-amyloid. The tangles, meanwhile, occur within the nerve cells. They are made from another protein, called tau.
- aging
Also Check: Color For Dementia Awareness
Isnt Dementia Part Of Normal Aging
No, many older adults live their entire lives without developing dementia. Normal aging may include weakening muscles and bones, stiffening of arteries and vessels, and some age-related memory changes that may show as:
- Occasionally misplacing car keys
- Struggling to find a word but remembering it later
- Forgetting the name of an acquaintance
- Forgetting the most recent events
Normally, knowledge and experiences built over years, old memories, and language would stay intact.
Onset Of Ad A Stage Of Insecurity And Emerging Losses
AD is often diagnosed in the mild dementia stage since memory functioning and daily activities are apparently and observably impaired. The diagnosis of AD is considered here to mark the onset of the disease although the indicators of a weakened performance in the cognitive and functional domain certainly are registered, before this official marker, during the predementia stage. The concerned person, the partner, as well as friends and family members may register behavioral changes mostly indicated by weak memory performance and mood- and motivation-related phenomena linked to depression . Comparable to other diseases and as has been argued elsewhere , one may characterize this stage as weakly scripted, which signifies in the terminology of cognitive psychology that the concerned persons have no scripts and, related to this, are lacking the specific behavioral routines to deal with the situation at hand. Moreover, whereas other negative life experiences are embedded into culturally shaped ways of responding and routines that often facilitate the coping process, the initial diagnosis of AD clearly lacks this external facilitation there is no ritual or normed response to this.
Alfred W. Kaszniak, in, 2002
Also Check: Alzheimer’s Disease Ribbon Color
Cholinergic Neurotransmission And Alzheimer Disease
The cholinergic system is involved in memory function, and cholinergic deficiency has been implicated in the cognitive decline and behavioral changes of AD. Activity of the synthetic enzyme choline acetyltransferase and the catabolic enzyme acetylcholinesterase are significantly reduced in the cerebral cortex, hippocampus, and amygdala in patients with AD.
The nucleus basalis of Meynert and diagonal band of Broca provide the main cholinergic input to the hippocampus, amygdala, and neocortex, which are lost in patients with AD. Loss of cortical CAT and decline in acetylcholine synthesis in biopsy specimens have been found to correlate with cognitive impairment and reaction-time performance. Because cholinergic dysfunction may contribute to the symptoms of patients with AD, enhancing cholinergic neurotransmission constitutes a rational basis for symptomatic treatment.
How Is Alzheimers Disease Diagnosed
Doctors use several methods and tools to help determine whether a person who is having memory problems has Alzheimers disease.
To diagnose Alzheimers, doctors may:
- Ask the person and a family member or friend questions about overall health, use of prescription and over-the-counter medicines, diet, past medical problems, ability to carry out daily activities, and changes in behavior and personality.
- Conduct tests of memory, problem solving, attention, counting, and language.
- Carry out standard medical tests, such as blood and urine tests, to identify other possible causes of the problem.
- Perform brain scans, such as computed tomography , magnetic resonance imaging , or positron emission tomography , to support an Alzheimers diagnosis or to rule out other possible causes for symptoms.
These tests may be repeated to give doctors information about how the persons memory and other cognitive functions are changing over time.
People with memory and thinking concerns should talk to their doctor to find out whether their symptoms are due to Alzheimers or another cause, such as stroke, tumor, Parkinsons disease, sleep disturbances, side effects of medication, an infection, or another type of dementia. Some of these conditions may be treatable and possibly reversible.
In addition, an early diagnosis provides people with more opportunities to participate in clinical trials or other research studies testing possible new treatments for Alzheimers.
You May Like: Alzheimer’s Disease Color Ribbon
Ps1 And Ps2 Mutations
Approximately 50-70% of early-onset autosomal-dominant AD cases appear to be associated with a locus mapped by genetic linkage to the long arm of chromosome 14 . Numerous missense mutations have been identified on a strong candidate gene, called PS1.
At the same time, another autosomal dominant locus responsible for early-onset AD was localized to chromosome 1. Two mutations were identified on the candidate gene, designated PS2. The physiological role of presenilins and the pathogenic effects of their mutations are not yet well understood.
Health Environmental And Lifestyle Factors
Research suggests that a host of factors beyond genetics may play a role in the development and course of Alzheimers. There is a great deal of interest, for example, in the relationship between cognitive decline and vascular conditions such as heart disease, stroke, and high blood pressure, as well as conditions such as diabetes and obesity. Ongoing research will help us understand whether and how reducing risk factors for these conditions may also reduce the risk of Alzheimers.
A nutritious diet, physical activity, social engagement, and mentally stimulating pursuits have all been associated with helping people stay healthy as they age. These factors might also help reduce the risk of cognitive decline and Alzheimers. Researchers are testing some of these possibilities in clinical trials.
Don’t Miss: Alzheimer’s Awareness Ribbon
Impact On Families And Carers
In 2019, informal carers spent on average 5 hours per day providing care for people living with dementia. This can be overwhelming . Physical, emotional and financial pressures can cause great stress to families and carers, and support is required from the health, social, financial and legal systems. Fifty percent of the global cost of dementia is attributed to informal care.
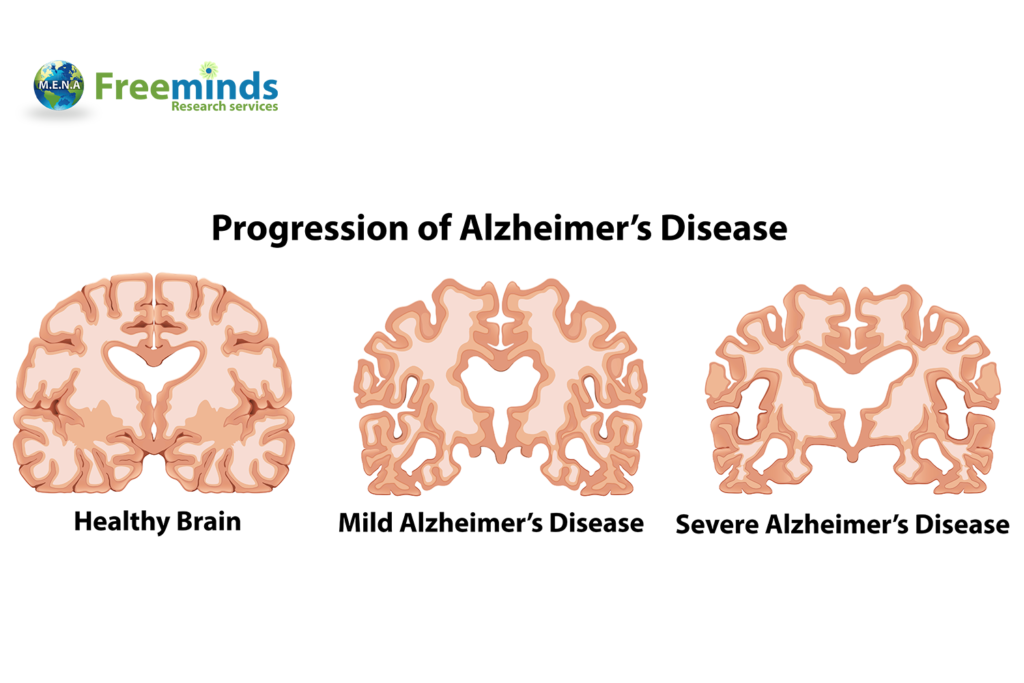
Stages Of The Disease
There are three recognized stages of Alzheimer disease: preclinical, mild cognitive impairment , and Alzheimer dementia. For clinical diagnosis the two most relevant stages are MCI and dementia. Recognition of the preclinical stage acknowledges that the Alzheimer disease process begins before symptoms are apparent and anticipates advances in diagnostic testing that may eventually enable diagnosis at the preclinical stage.
MCI often is subdivided into different types, namely amnestic and nonamnestic. One of the first symptoms marking the transition from normal aging to Alzheimer disease is forgetfulness. This transitional stage represents amnestic MCI and is characterized by noticeable dysfunction in memory with retention of normal cognitive ability in judgment, reasoning, and perception. In nonamnestic MCI, impairments in cognitive functions related to attention, perception, and language predominate over deficits in memory. However, as MCI progresses to Alzheimer disease, memory loss becomes more severe, and language, perceptual, and motor skills deteriorate. Mood becomes unstable, and the individual tends to become irritable and more sensitive to stress and may become intermittently angry, anxious, or depressed. Those changes mark the transition to Alzheimer dementia, which in its advanced stages is characterized by unresponsiveness and loss of mobility and control of body functions death ensues after a disease course lasting from 2 to 20 years.
Read Also: Alz Ribbon