How Is Magnesium An Atrial Fibrillation Cause
Magnesium is an extremely well-researched mineral, and it is vital for the electrical activity in the body- especially for the heart and the brain. Every cell in the body and every single electrical pathway in the body is regulated by magnesium and when this electrical activity gets altered, you can have problems that range from simple irritability to atrial fibrillation to Sudden Death from Heart Failure. When you take a look at the Signs of Magnesium Deficiency, you will see that all of the symptoms have to do with the inability to relax- whether it is muscles, neurons or YOU that cant relax.
What IS atrial fibrillation anyway? It is the inability of the atrial portion of the heart and its electrical activity to relax. The effects of the atria are somewhat like a Muscle Cramp or a seizure of the heart. And muscle cramps and seizures are both related to magnesium deficiency as well!
There are many, many studies showing that the Causes of Muscle Cramps, spasms, tightness, seizures, Heart Palpitations etc. are improved or relieved entirely simply by the administration of magnesium. And atrial fibrillation is no different.
Do Sleep Medications Impact Women And Men Differently
The Cache County Study on Memory and Aging looked at whether taking sleep medications led to an increased Alzheimers risk and if men and women are impacted differently.
In an observational study of 3,656 adults over age 65, researchers found that men who used sleep medications had a 3.6 times increased risk of getting Alzheimers than those who didnt. In contrast, women who used sleep medications but did not suffer from sleep disturbances had a four times greater risk of getting Alzheimers, compared to women who had sleep disturbances and used sleep medications. These women had a 35.2% reduced risk of developing Alzheimers.
More research is needed to determine and understand the mechanisms underlying the differences between men and women, and the cognitive impact of using sleep medications, said Elizabeth Vernon, MS, Utah State University, who presented the data at AAIC 2019.
Clinical Use Of Melatonin In Pd
Approximately 3/4 of the dopaminergic cells in the SNpc need to be lost to uncover motor symptomatology in PD. However, non-motor symptoms like hyposmia, depression, or RBD precede the onset of PD for years and are index of worse prognosis . Indeed, up to 65% of patients showing RBD developed PD 1013 years later .
Table 5 summarizes the clinical studies reporting melatonin use in PD. Daily administration of 312 mg of melatonin at bedtime is effective in the treatment of RBD . Polysomnography in RBD patients treated with melatonin showed significant decreases in number of R epochs without atonia and in movement time during REM sleep, contrasting with the persistence of muscle tone in R sleep seen with patients treated with clonazepam. Based on these data, a clinical consensus recommended melatonin use in RBD at Level B .
Table 5. Studies including treatment of PD and RBD patients with melatonin.
An association between motor fluctuations in PD and diurnal variation in circulating melatonin levels was postulated via possible interactions of melatonin with monoamines in the striatal complex . Nearly half of the patients with PD showed L-DOPA-related motor complications after 5 years of treatment. In view of the results obtained in experimental parkinsonism discussed above, the use of melatonin as an adjuvant to decrease the therapeutic dosage of L-DOPA in PD deserves to be considered .
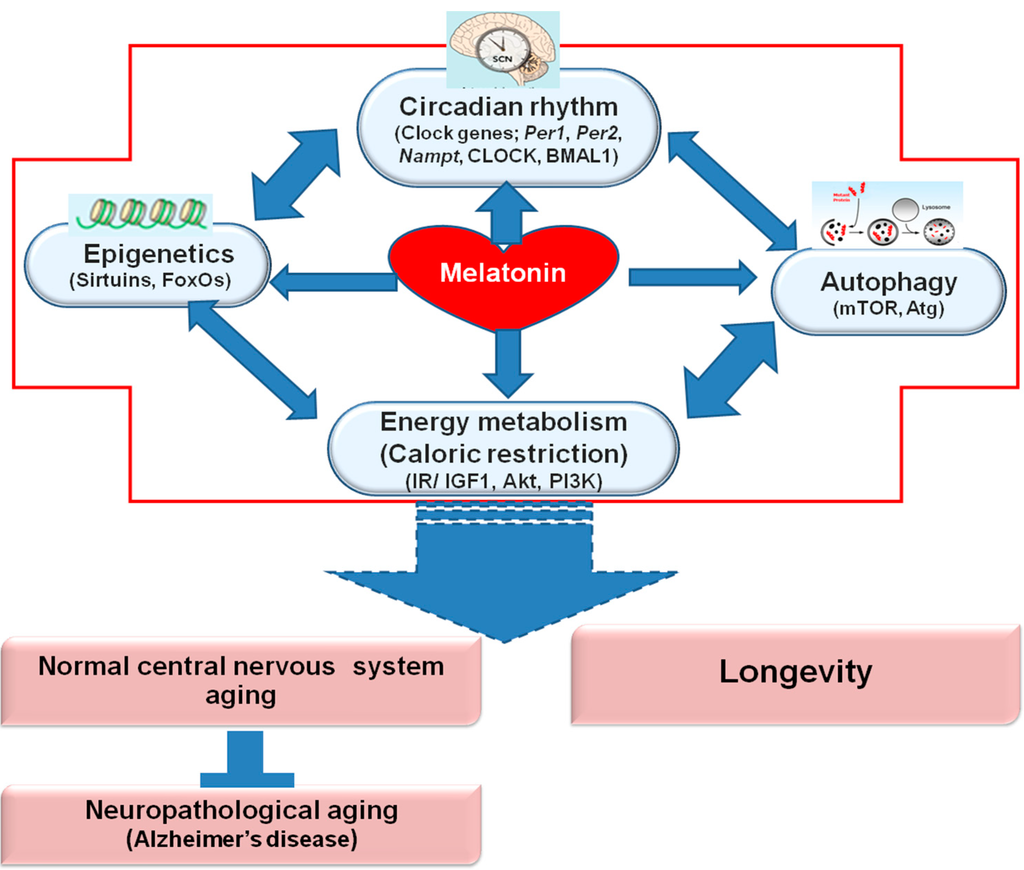
Figure 1. The different mechanisms through which melatonin may halt AD and PD progression.
Also Check: Alzheimer Awareness Ribbon
Why Do Alzheimers Patients Struggle With Sleep
Changes in sleep quality and duration in older age are common. However, the sleep concerns seen in people with Alzheimers are often more severe and complex. There may be a reciprocal relationship between sleep issues and the other symptoms of Alzheimers. This means that sleep loss can worsen other symptoms, such as delusions, restlessness, and wandering, which can, in turn, make sleeping more difficult.
Getting enough sleep and spending sufficient time in deep sleep and rapid eye movement sleep are necessary in order for preservation of memories to occur. Memory loss is the primary symptom in people living with Alzheimers, and compared to older adults without the disease, Alzheimers patients spend progressively less time in deep sleep and REM sleep.
People with Alzheimers experience dramatic changes to their sleep-wake cycle. The sleep-wake cyclealso called circadian rhythmis the internal clock in our body that initiates physical processes related to wake and sleep. When this cycle is disturbed in Alzheimers patients, the result is not sleeping at night and sleeping too much during the day. Researchers attribute circadian rhythm disruption in Alzheimers patients, at least in part, to cellular changes in the brain caused by the disease. Dysregulated production of the sleep hormone, melatonin, in patients with Alzheimers may play a role. Other possible factors include decreased physical activity and less natural light exposure.
Is Melatonin Safe For Senior Citizens

Since the deterioration of sleep quality with age occurs by itself due to lower melatonin production, melatonin supplements seem to be the simplest way to fill the need for this hormone. But are they safe for the elderly?
A study conducted in 2007 concluded that prolonged-release melatonin supplements showed good results in improving the quality of sleep in patients aged 55 years and older. The results were good for patients with dementia as well as for those whose cognitive functions were not significantly impaired. Therefore, taking melatonin is not only safe but also effective.
But its important to remember that the elderly, along with insomnia, often have age-related and chronic diseases such as hypertension, diabetes, or cardiovascular diseases and melatonin can interfere with the effectiveness of the drugs aimed at treating these conditions. Thats why, before you start taking melatonin supplements, an appointment with a healthcare professional is highly advised.
Also Check: Where To Buy Jelly Drops For Dementia Patients
How Much Should I Take
Because of its ability to promote sleep, melatonin should be taken before bedtime. Doctoroz.com recommends taking 0.3 to 1 milligram of melatonin an hour and a half before bedtime. The website warns that taking too much melatonin more than 1 milligram may have an adverse effect and end up disrupting your sleep cycle. Lack of sleep may in turn raise your blood pressure according to the American Heart Association.
Also Check: Can I Give My Cat Melatonin
Is It Safe For Alzheimers Patients Yo Take Sleep Aidswhat Should I Do If I Experience Side Effects
The routine use of medications to treat sleep issues in patients with Alzheimers disease is not supported by current scientific evidence. Sleep aids carry extra risks for people with Alzheimers they can cause falls and injury, increase memory loss and confusion, and may have an overly sedative effect. Sleep aids are typically reserved for cases where all other options have been exhausted and should only be given under guidance of a physician.
Melatonin supplements have been studied as a possible option for improving sleep quality in Alzheimers patients. However, research examining the effectiveness of melatonin supplements in people with dementia has produced conflicting results. Some studies demonstrated a small benefit, increasing nighttime sleep by around 30 minutes, while other studies showed no benefit. There is also evidence to suggest that melatonin supplements may increase social withdrawal and depression in patients with dementia.
You May Like: Margaret Thatcher Dementia
Studies Regarding Melatonin And Dementia
Researchers from the Netherlands Institute for Neuroscience reviewed the perks of melatonin and the effect of environmental light on seniors with dementia.
The study that was published in the Journal of the American Medical Association reported that melatonin was useful with sleep issues.
However, it also increased withdrawn dementia-related behavior. The results were enhanced when combined with a bright light environment. The study involved 189 elderly persons.
Most of the participants had dementia. All the participants were living in assisted care facilities.
The seniors were assigned to different groups randomly.
The groups received different treatments and these included:
- Melatonin and dim light exposure
- Melatonin and bright light exposure
- Placebo and dim light
- Placebo and bright light
The researchers discovered that melatonin helped to enhance the onset of sleep as well as sleep duration by 27 minutes.
Side Effects
However, it was also the cause of unwanted side effects of increased depressive and withdrawn behaviour in participants.
Bright light therapy was also linked to improvements in depressive and cognitive deterioration symptoms as well as improved functional abilities and daily living activities.
The experts concluded that a combination of the two therapies produced the best results. This resulted in a decrease in agitation, night-time restlessness, and aggression.
It seemed that a bright light environment countered the negative melatonin effects.
Why Dementia Patients Don’t Sleep Well
Depending on the stage of dementia the sleep pattern can change from sleeping too little to sleeping too much. As dementia progresses it is not unusual for the pattern to deteriorate. What makes things a little trickier is that dementia can make it harder for someone to communicate what is wrong. For example, they might not be able to tell you that theyre in pain. This is why it becomes even more important to pay close attention to other types of communication such as facial expression and body language. Below, we have outlined some issues which can cause dementia patients to not sleep well.
Recommended Reading: Does Coke Cause Alzheimer’s
Sleeplessness & High Blood Pressure
If you are experiencing occasional sleeplessness and have high blood pressure or are taking medication to help manage high blood pressure, you may be wondering which over-the-counter nighttime sleep aid options may be right for you. TYLENOL® PM and SIMPLY SLEEP® both contain the active ingredient diphenhydramine. Read more about diphenhydramine and high blood pressure below. to buy a TYLENOL® PM product.
What Does Melatonin Do For Dementia Patients
Melatonin can help naturally regulate a persons sleep cycles when their brain begins to fail.A number of studies have found that melatonin can ease insomnia and reduce sundowning behaviors. However, a 2006 Cochrane review suggests that, in some people with dementia, melatonin supplements may increase mood issues. So people with depression or severe dementia-related behavior problems should not take melatonin.
Most studies have looked at melatonin at a dosage of 2.5 to 5mg. Many have also assessed the effectiveness of melatonin along with dementia medications, and have not found any serious drug interactions. But if you or a loved one are taking any other drugs, talk to a doctor before trying melatonin.
While there is promising emerging data, the research supporting melatonins use in people with advanced or end-stage dementia is mixed. Moreover, most research has looked at people with Alzheimers or mild cognitive impairmentnot other types of dementia. So researchers dont know as much about how well melatonin works in atypical dementias like Lewey body dementia or frontotemporal dementia.
Dementia is an unpredictable disease, and what works well for one family can be catastrophic for another. Keep a log of symptoms and medications so you can track progress over time. And if a person with dementia doesnt want to take medication, do not force it. Ultimately, there is no cure for dementia, so forcing medication only increases conflict and stress.
Don’t Miss: Can Prevagen Help Dementia
Melatonin And For Early Cognitive Decline
Cognitive impairment inevitably increases with ageing. But when does age-related cognitive decline begin? In healthy educated adults even in their 20s and 30s, certain limited aspects of such decline had already started. Hypertension predisposes to early cognitive decline. The deterioration in mild cognitive declined could be countered by fast-release melatonin 39 mg given at bedtime for up to 3 years. Those treated with melatonin added to their prior medication, often donepezil, performed better in the Mini-Mental State Examination and in the Alzheimers disease Assessment Scale. Furthermore, depression scores decreased in melatonin-treated patients, while the quality of sleep and wakefulness also improved. But when does age-related cognitive decline begin? Controversially, the decline in healthy educated adults could start even when they were only in their 20s and 30s. When could melatonin be started to counter this age-related adverse effect? Sensitive testing with a complex video game , using a dataset of 3305 players, showed that age-related slowing began early and not late in life.
Drugs Sunlight And Low Melatonin
In Dr. Reiters view, the top threats to adequate melatonin production are our level of exposure to bright lights after darkness, and our habit of sleeping only 56 hours a night. The aging process also has an impact , as does the use of drugs like beta blockers and tranquilizers . Together, these things suggest that its a good idea to supplement with melatonin as we get older.
The point about beta blockers is an interesting one given that theyre widely prescribed to lower blood pressure yet it would seem that their effect on melatonin production may actually cause an increase in blood pressure. Ive always considered beta blockers to be among the safest cardiovascular medications available, and an essential therapy for patients whove had a heart attack. But their impact on melatonin production is a wise reminder that even good drugs have side effects. Beta blockers can also cause nightmares and insomnia!
If youre taking a beta blocker for any reason, you need to take a melatonin supplement. Moreover, take your medication in the morning, not before bed as many doctors recommend, when it is most likely to interfere with your natural tendency to produce melatonin.
Dont Miss: Does Blue Cross Blue Shield Cover Testosterone Therapy
Read Also: What Is Senility
The Use Of Melatonin Sleep
Melatonin is an all-natural sleep aid, but it has not been evaluated by the FDA for safety, effectiveness or purity or been approved for medicinal use. Potential risks or advantages of melatonin are unknown, and there are no regulated manufacturing standards in place for these supplements.
Though some success has been shown in using melatonin for a sleep aid, the issue is that the FDA classifies it as a dietary supplement, and that allows companies to sell melatonin in varying dosages.
Researchers have concluded that the correct dosage is between .3 and 1 mg, but since the dosages vary so much on bottles of the supplement, it can be risky not knowing the actual dosage you are taking.
According to MIT neuroscientist Dr. Richard Wurtman, who introduced melatonin 20 years ago, an overdose of melatonin can upset the bodys natural processes and rhythms and produce opposite effects of the intention, meaning, it can actually cause next-day drowsiness. More research needs to be done on the side effects of melatonin to ease sleep and sundowning problems in those with Alzheimers or dementia. When used correctly with the right dosage, the supplement can encourage sleep. However, prolonged use of melatonin actually increases insomnia, and changes how the individual reacts to it.
Melatonin Affects Cellular Receptors
Ventricular tachycardia and ventricular fibrillation are two types of dangerous, irregular electric activity in the heart that may cause a heart attack. It turned out the melatonin-treated rats had a lower rate of both types of arrhythmia . Also, a particular marker of antioxidant activity was elevated in the rats that got melatonin. However, no link was observed between the presence of oxidative stress and irregular electric activity in the heart.In a previous study, researchers observed that by blocking melatonin-specific receptors in the cells one can disable melatonins anti-arrhythmic effect. In other words, melatonin loses its effects in the cells if there are no receptors to which melatonin can attach. This fact combined with the recent rat study leads the scientists to believe that melatonin has a direct effect on cells, which is positive for the heart rhythm, and that the effect has nothing to do with melatonins role as an antioxidant.
Don’t Miss: Alzheimer’s Aphasia
What Are Light Sleep Disorders
Light sleep disorders are often called rapid eye movement sleep behaviour disorder , and cause people to act out their dreams through moving or talking in their sleep.
Dementia with Lewy bodies and Parkinson’s disease seem to be particularly associated with light sleep disorders and some studies have suggested that light sleep disorders are a very early indicator of these conditions, particularly in older men.
Some researchers believe that the part of the brain that is damaged with dementia with Lewy bodies or Parkinson’s disease also plays a role in light sleep, explaining why people with these conditions are particularly affected by light sleep disorders.
Tissue Collection For Oxygen Consumption Assay And Transcript Analysis
All mice were euthanized by sterile intraperitoneal overdose injection of ketamine and xylazine , followed by transcardial 0.9 % sterile saline perfusion. Brains were quickly removed and placed on an ice-cold plate for dissection. The brain was initially bisected along the sagittal plane and the left hemisphere was dissected for hippocampus, striatum, and frontal cortex. The dissected samples were then flash frozen for subsequent analysis. The right hemisphere was similarly dissected and preserved in QIAGEN RNAlater® RNA stabilization reagent for later mRNA analysis by qPCR.
Don’t Miss: 7th Stage Of Alzheimer’s
Get The Lighting Right
To aid a more restful nights sleep the bedroom should be as comfortable as possible. Using blackout curtains are a good idea during night-time to eliminate outside disturbances. Research suggests that light therapy can reduce restlessness and confusion for people with dementia. Should you wish to consider light therapy, it has been proven that violet coloured light promotes drowsiness and a full-spectrum fluorescent light used for the first two hours of the day can be settling. Light therapy that follows a regular pattern can also help with disturbed body clocks.
Safety – if night wandering is a problem, or frequent visits to the loo, you will need to consider some sort of low light to prevent your parent falling in the dark. You may want to invest in a motion sensor night light. A motion sensor light automatically turns on when motion is detected within three metres. It then turns off after 30 seconds of no activity. This means that people with dementia can use the bathroom in the night or get out of bed with less risk of falling. The light is gentle and warm in order to not interrupt sleep.
- Hard to stay awake during the day and taking frequent naps
- Sundowning, sometimes referred to as late-day confusion.
Sundowning is a dementia-related disorder where a person becomes increasingly anxious and unsettled in the late afternoons and evenings. Sundowning is more often experienced with mid-stage to advanced dementia.