Research: The Road Ahead
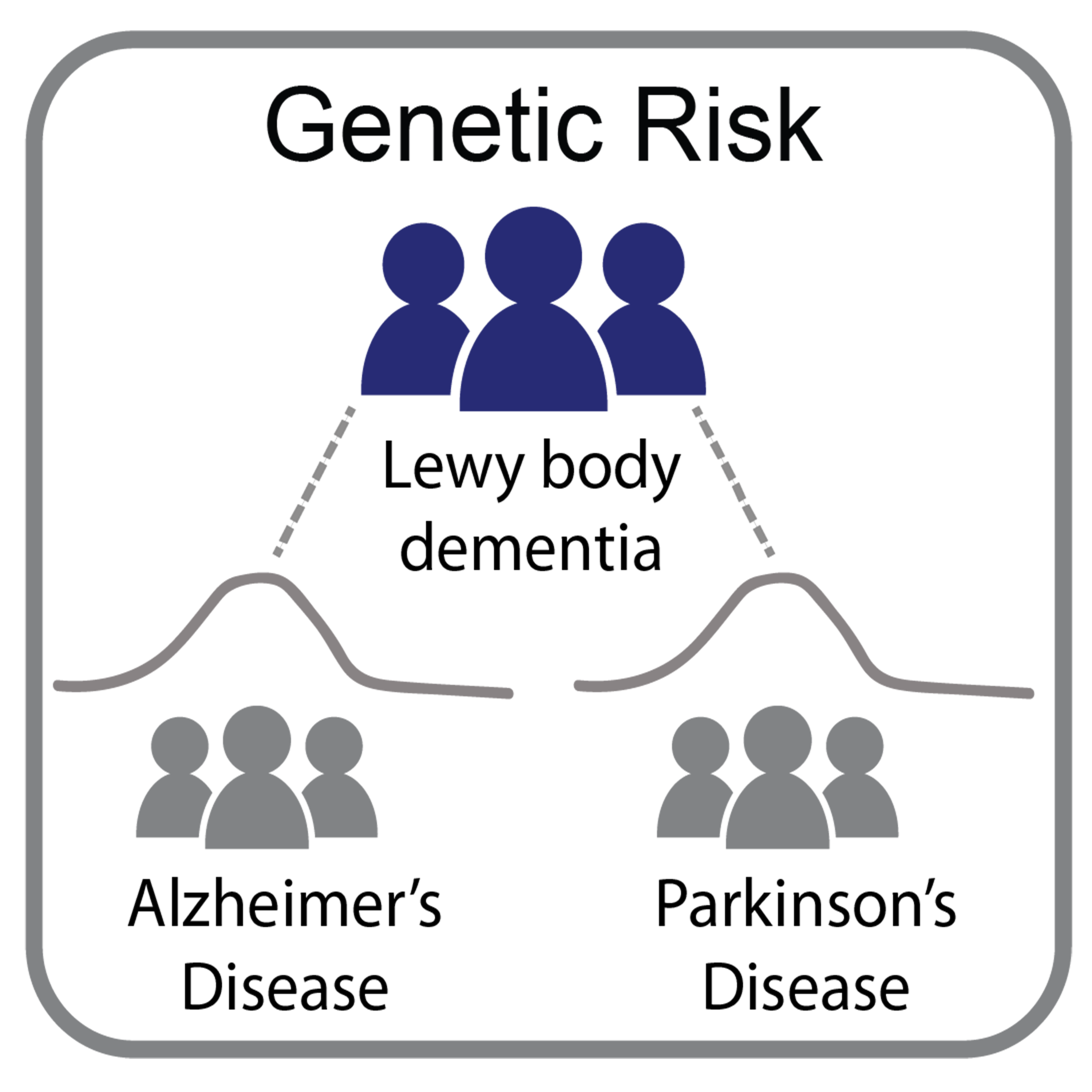
There is a great deal to learn about LBD. At a basic level, why does alphasynuclein accumulate into Lewy bodies, and how do Lewy bodies cause the symptoms of LBD? It is also of increasing interest to the Alzheimers and Parkinsons disease research communities. LBD represents an important link between these other brain disorders, and research into one disease often contributes to better understanding of the others.
Many avenues of research focus on improving our understanding of LBD. Some researchers are working to identify the specific differences in the brain between dementia with Lewy bodies and Parkinsons disease dementia. Others are looking at the diseases underlying biology, genetics, and environmental risk factors. Still other scientists are trying to identify biomarkers , improve screening tests to aid diagnosis, and research new treatments.
Scientists hope that new knowledge about LBD will one day lead to more effective treatments and even ways to cure and prevent the disorder. Until then, researchers need volunteers with and without LBD for clinical studies.
To find out more about clinical trials, talk with a doctor or visit the National Institutes of Health Web site at www.clinicaltrials.gov.
Where Can I Get More Information
For more information on neurological disorders or research programs funded by the National Institute of Neurological Disorders and Stroke, contact the Institute’s Brain Resources and Information Network at:
Office of Communications and Public LiaisonNational Institute of Neurological Disorders and StrokeNational Institutes of HealthBethesda, MD 20892
NINDS health-related material is provided for information purposes only and does not necessarily represent endorsement by or an official position of the National Institute of Neurological Disorders and Stroke or any other Federal agency. Advice on the treatment or care of an individual patient should be obtained through consultation with a physician who has examined that patient or is familiar with that patient’s medical history.
All NINDS-prepared information is in the public domain and may be freely copied. Credit to the NINDS or the NIH is appreciated.
What Causes Lewy Body Dementia
LBD happens when Lewy bodies build up in parts of the brain that control memory, thinking, and movement. Lewy bodies are abnormal deposits of a protein called alpha-synuclein. Researchers don’t know exactly why these deposits form. But they do know that other diseases, such as Parkinson’s disease, also involve a build-up of that protein.
Read Also: How To Deal With Inappropriate Sexual Behaviour In Dementia
Improving Diagnosis With Composite Scores
A diagnostic challenge, particularly outside of expert centers, there are long delays in diagnosing LBD leading to significant burden. Although consensus criteria have excellent specificity, there is no standardized way to assess symptoms, reducing sensitivity. We developed the LB Composite Risk Score 21 from autopsy-verified cases to improve the ability to detect LBD in clinic and research populations .
Figure. Diagnostic Tools for Dementia With Lewy Bodies. The Lewy Body Composite Risk Score is a 10-item questionnaire to capture signs and symptoms associated with Lewy body pathology. A score of 3 or greater represents a high probability that Lewy bodies are contributing to cognitive decline . Comparison of MRI in Alzheimers disease and dementia with Lewy bodies demonstrates less cortical and hippocampal atrophy in DLB . Comparison of dopamine transporter single photon emission tomography in AD and DLB shows decreased dopamine uptake in the basal ganglia in DLB vs normal uptake in AD.
Rcoe Articles For Community Education

All articles have been drafted and edited by members of the Community Education and Support Working Group, as well as edited and approved by Angela Taylor, LBDA, and Brad Boeve, MD, Mayo Clinic.
LBDA Research Center of ExcellenceUniversity of MichiganMichigan Alzheimers Disease Center
Lewy body dementia is the second most common form of progressive dementia. An estimated 1.4 million Americans in the United States have LBD. The symptoms of LBD overlap with other more well-known diseases, like Alzheimers and Parkinsons disease. This leads to misdiagnoses, with only 30-50% of LBD cases being accurately diagnosed. Read on to learn more about what makes LBD unique and the importance of receiving an early and correct diagnosis.
Imagine dementia as a fruit bowl
Whats the difference between Alzheimers disease and dementia? This is one of the most common questions we receive. Its an important question because the terms are often used in place of each other. However, they mean different things.
In brief dementia is a broad umbrella term. It means cognitive symptoms interfere with a persons normal daily functioning. Dementia can affect behavior, decision-making, memory, language, visual or spatial perception, and attention. Typically, more than one of these abilities is impaired. However, one category may be most obviously affected.
Consider the following visual image:
What makes LBD different?
Accurate diagnosis of LBD is critical.
Don’t Miss: What Is Vascular Dementia Without Behavioral Disturbance
Building A Lewy Body Dementia Care Team
After receiving a diagnosis, a person with LBD may benefit from seeing a neurologist who specializes in dementia and/or movement disorders. Your primary doctor can work with other professionals to follow your treatment plan. Depending on an individual’s particular symptoms, physical, speech, and occupational therapists, as well as mental health and palliative care specialists, can be helpful.
Support groups are another valuable resource for people with LBD and their caregivers. Sharing experiences and tips with others in the same situation can help people find practical solutions to day-to-day challenges and get emotional and social support.
Treatment And Care For Lewy Body Dementia
While LBD currently cannot be prevented or cured, some symptoms may respond to treatment for a period of time. An LBD treatment plan may involve medications, physical and other types of therapy, and counseling. A plan to make any home safety updates and identify any equipment can make everyday tasks easier.
A skilled care team often can suggest ways to improve quality of life for both people with LBD and their caregivers.
Read Also: How Does Alzheimer’s Disease Progress
Lewy Body Dementia Treatment Market Research Report Business Growth Segments Future Trends And Forecast 2028
Research and analysis about the key developments in the Healthcare industry and key competitors along with their strategies has been covered here. To achieve striking business growth and highest return on investment , choosing the finest market research report like Lewy body dementia treatment is truly favourable. It becomes simple to illustrate the commerce strategies for the businesses of small, medium as well as large size with the help of this business report. These parameters can be listed as latest trends, market segmentation, new market entry, industry forecasting, target market analysis, future directions, opportunity identification, strategic analysis, insights and innovation. The credible Lewy body dementia treatment report is bestowed with full allegiance to provide the best service and recommendations.
Global lewy body dementia treatment market is expected to gain market growth in the forecast period of 2021 to 2028. Data Bridge Market Research analyses the market is growing at a healthy CAGR of 4.90% in the above-mentioned research forecast period.
Get Sample Copy of the Report @
Inquiry before Buying the Report @
Global Lewy Body Dementia Treatment Market Scope and Market Size
About Data Bridge Market Research:
Contact:
US: +1 888 387 2818
New Drug For Lewy Body Dementia Shows Promise
Drug shows encouraging signs for patients of less common type of dementia. Pacific Neuroscience Institute located at Providence Saint Johns Health Center among sites for clinical trial.
SANTA MONICA, Calif., Oct. 30, 2020 An investigational drug for the treatment of Alzheimers disease shows significant improvement for patients with Lewy body dementia in a clinical trial that includes participants at the Pacific Neuroscience Institute located at Providence Saint Johns Health Center.
Recommended Reading: Why Do Dementia Patients Get So Angry
Melissa Armstrong Md Msc Faan
Dr. Melissa Armstrong is the Director of the Mangurian Clinical-Research Headquarters for Lewy Body Dementia at the University of Florida and she leads the Lewy Body Dementia Association Research Center of Excellence at UF. She is an Associate Professor in the Department of Neurology and has an affiliate appointment in the Department of Health Outcomes and Policy. Her clinical work and research focus on improving care for persons with Lewy body dementia and their families, including increasing Lewy body dementia awareness, identifying priorities for care, and improving end-of-life experience.
Assistant Professor, Department of Neurology
Targeting Lewy Body Specific Pathology Using Biomarkers
This study, supported by the National Institutes of Health, is designed to allow us to better diagnose Lewy Body disorders.
- Who can participate?
- An individual may be able to take part in the study if they:
- Have been diagnosed with Dementia with Lewy Bodies OR
- Have been diagnosed with Parkinsons Disease with cognitive changes AND
- They speak English or Spanish.
Also Check: How To Keep Alzheimer’s Patients Calm
Causes And Risk Factors
The precise cause of LBD is unknown, but scientists are learning more about its biology and genetics. For example, they know that an accumulation of Lewy bodies is associated with a loss of certain neurons in the brain that produce two important neurotransmitters, chemicals that act as messengers between brain cells. One of these messengers, acetylcholine, is important for memory and learning. The other, dopamine, plays an important role in behavior, cognition, movement, motivation, sleep, and mood.
Scientists are also learning about risk factors for LBD. Age is considered the greatest risk factor. Most people who develop the disorder are over age 50.
Other known risk factors for LBD include the following:
Is There A Cure How Is Lewy Body Dementia Treated
Unfortunately, there is currently no known cure. Treatment for Lewy body dementia is currently focused on treating symptoms only.
The first step in treating an individual with LBD is to identify medications the person is taking that could contribute to symptoms or are best avoided in adults with dementia. This includes benzodiazepines, anticholinergic medications , antipsychotic drugs and tricyclic antidepressants. Antipsychotic use is of particular concern in the treatment of dementia with Lewy bodies, given the risk of hypersensitive reactions. Anticholinergic medications used to treat tremors are associated with worsened cognition and psychosis.
Research suggests that cholinesterase inhibitor drugs used to treat Alzheimers Disease such as Aricept or Exelon could be helpful. Evidence suggests that these medications could improve behavioural such as psychosis, depression, anxiety and apathy for some people. Exelon is the only cholinesterase inhibitor approved by the FDA for use in Parkinsons Disease Dementia. Drugs used to treat Parkinsons disease could be useful to control rigidity and spasticity but may aggravate confusion and hallucinations. Physiotherapy and mobility exercises may be tried.
PDF: http://www.alzheimers.org.uk/site/scripts/download_info.php?fileID=1757
Recommended Reading: Will Mri Show Alzheimer’s Disease
Research News: Lewy Body Composite Risk Score
Diagnosing dementia with Lewy bodies is challenging both for specialists and primary care physicians. A new composite risk score may aid in differentiating DLB from other forms of dementia.
The Lewy Body Composite Risk Score was recently published in a scientific update paper on DLB by Dr. James E. Galvin, of New York University Langone Medical Center. Previous research of autopsy-confirmed cases of DLB identified clinical features that predict the presence of Lewy body disease in the brain . These features were used to develop a composite risk score that would aid in determining whether underlying Lewy body pathology is contributing to dementia symptoms and improve the ability of the clinician to make a confident diagnosis of DLB.
The Composite Risk Score was applied to 69 well-characterized individuals, including 25 healthy controls, 24 with Alzheimers disease and 20 with DLB. Subjects had detailed clinical and cognitive assessments and there were no differences in age or education between the groups. Global dementia ratings revealed no differences in dementia severity between the Alzheimers and DLB groups. Individuals with DLB performed significantly worse in visual/spatial tests, while both groups performed similarly in global and working memory tests.
Table 1. Lewy Body Composite Risk Score
CitationKarantzoulis, S., & Galvin, J. . Update on dementia with Lewy bodies. Current Translational Geriatrics and Experimental Gerontology Reports, 2, 196-204.
Connect With Us
Lewy Body Dementia Treatment: Why Choose Johns Hopkins
- Johns Hopkins is poised to advance LBD treatment and is proud to be recognized by the Lewy Body Dementia Association as a Research Center of Excellence.
- The large number of LBD patients we see gives our team rare expertise in assessing and treating this form of dementia.
- Our multidisciplinary approach aims to make the most of each persons function, independence and quality of life.
- Monthly multidisciplinary clinics focused on LBD and other atypical Parkinsonian disorders ensure our clinicians are sharing valuable clinical and research insights with each other and other members of your care team.
Recommended Reading: Is Alzheimer’s Hereditary Or Genetic
Lbd Research Center Of Excellence At Stanford University
The Research Center of Excellence is located in the Stanford University Department of Neurology & Neurological Sciences, as part of the Division of Memory Disorders and the Division of Movement Disorders, which have rapidly grown into world-leading programs that are highly integrated and uniquely collaborative. Our Center includes both Memory disorders and Movement disorders Physicians, Neuropsychologists, a Psychiatrist, Nurse coordinators, Social Worker, Genetics counselor, and Physical/Occupational/Speech Therapists.
Highlights of our integrated Center include:
The Stanford Alzheimers disease Research Center started at Stanford in 2015. Our ADRC is the only national Center with a dual focus on cognitive impairments due to Alzheimers and Lewy body pathologies. We are actively recruiting patients with Lewy Body Dementia , Alzheimers disease , Parkinsons disease , and healthy adults.
The Pacific Udall Center moved to Stanford in 2016. The PUC focuses on the underlying genetic and mechanistic causes for cognitive impairments in PD. We are actively recruiting people with Parkinsons disease, both with and without cognitive and memory problems.
Lewy Body Clinical Trials
The expansive Stanford Neuroscience Clinical Trials Program, under the direction of Dr. Sharon Sha who serves as Medical Director, includes clinical trials related to Neurology, Neurosurgery, and Neuroradiology. All of these clinical and research activities are on site at our new state-of-the-art Stanford Neuroscience Health Center where participants can obtain brain imaging , treatment infusions, lab tests, cognitive testing, and neurological evaluations. Our clinical trials are expanding and have approximately 100-200 clinical trials ongoing at any given time.
Also Check: Can You See Dementia On A Ct Scan
Finding Specific Treatments For Dementia With Lewy Bodies
Focusing on the early symptoms will help us give the appropriate treatment and support. This is important because some of the anti-psychotic drugs given to people with Alzheimers disease could be harmful to people with dementia with Lewy bodies.
There are currently no treatments that specifically work for people with dementia with Lewy bodies, although some doctors might prescribe treatments for Alzheimers such as donepezil and rivastigmine ‘off-label’ to help with certain symptoms.
Understanding early symptoms and improving diagnosis will also help with clinical trials. People can enrol in appropriate clinical trials that are developing specific treatments for people with the condition.
Read our dementia with Lewy bodies guide
Read our dementia with Lewy bodies factsheet for more information, including diagnosis, symptoms and treatments.
Coping With Cognitive Changes
Some medications used to treat Alzheimer’s disease also may be used to treat the cognitive symptoms of LBD. These drugs, called cholinesterase inhibitors, act on a chemical in the brain that is important for memory and thinking. They may also improve hallucinations, apathy, and delusions. The U.S. Food and Drug Administration has approved one Alzheimer’s drug, rivastigmine, to treat cognitive symptoms in Parkinson’s disease dementia. Several other drugs are being tested as possible treatments for LBD symptoms or to disrupt the underlying disease process.
Don’t Miss: How To Convince Alzheimer’s Patients
Types Of Lewy Body Dementia And Diagnosis
LBD refers to either of two related diagnoses dementia with Lewy bodies and Parkinson’s disease dementia. Both diagnoses have the same underlying changes in the brain and, over time, people with either diagnosis develop similar symptoms. The difference lies largely in the timing of cognitive and movement symptoms.
In DLB, cognitive symptoms develop within a year of movement symptoms. People with DLB have a decline in thinking ability that may look somewhat like Alzheimer’s disease. But over time, they also develop movement and other distinctive symptoms of LBD.
In Parkinson’s disease dementia, cognitive symptoms develop more than a year after the onset of movement symptoms . Parkinson’s disease dementia starts as a movement disorder, with symptoms such as slowed movement, muscle stiffness, tremor, and a shuffling walk. These symptoms are consistent with a diagnosis of Parkinson’s disease. Later on, cognitive symptoms of dementia and changes in mood and behavior may arise.
Not all people with Parkinson’s disease develop dementia, and it is difficult to predict who will. Many older people with Parkinson’s develop some degree of dementia.
Caregivers may be reluctant to talk about a person’s symptoms when that person is present. Ask to speak with the doctor privately if necessary. The more information a doctor has, the more accurate a diagnosis can be.
Theme : Fear Of The Now Worry For The Future

Fear and anxiety featured strongly in the quantitative questionnaires and people with Lewy body dementia and carer narratives . In the web-based surveys, the most frequent burden items reported by Lewy body dementia caregivers were fear or âconcernsâ for the future for their loved ones , with feelings of fear and uncertainty frequently highlighted around the ability to provide care and caregiver performance . The qualitative research of Parkinson’s disease dementia spouses spoke of negative feelings such as guilt, distress and fear of the progression of the disease, in addition to worrying about the future if they were unable to provide care for their partners . People with Lewy body dementia perspectives, although limited, highlighted a range of emotional responses to living with Lewy body â fear of hallucinations, fear of falls and frightening nightmares as a result of REM sleep disorder and being scared of the effects of tiredness, and fatigue . The symptoms of fluctuations, depression, delirium and violence were also expressed as âfrighteningâ .
Also Check: When Does Dementia Most Often Occur