Nhs Support For Dementia
NHS help for dementia includes the treatment you receive from your GP and hospital. It can also include other types of healthcare, such as:
- speech and language therapy
- support from the Older People’s Mental Health team
In some parts of the country, the NHS provides Admiral Nurses in partnership with the charity Dementia UK.
Admiral Nurses are NHS specialist dementia nurses who will visit you to give practical guidance on accessing services as well as offering emotional support. Find out more about Admiral nurses and how they can help.
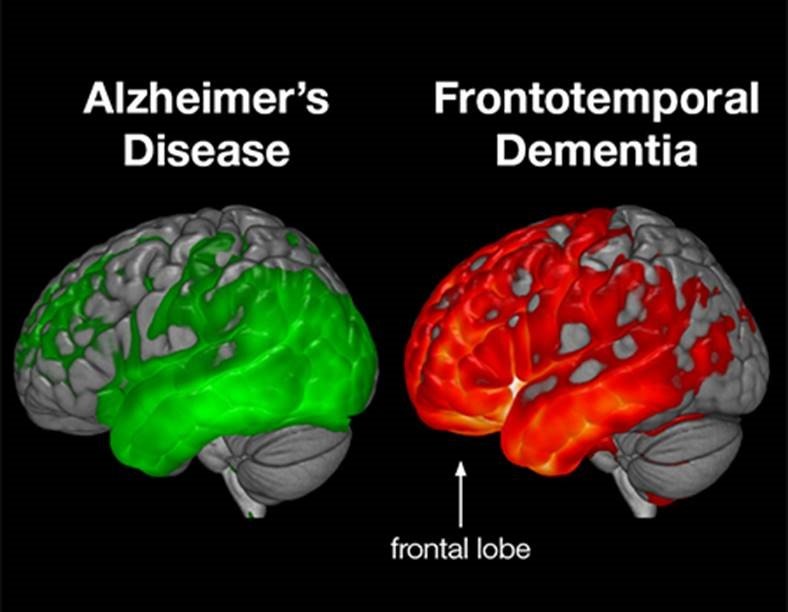
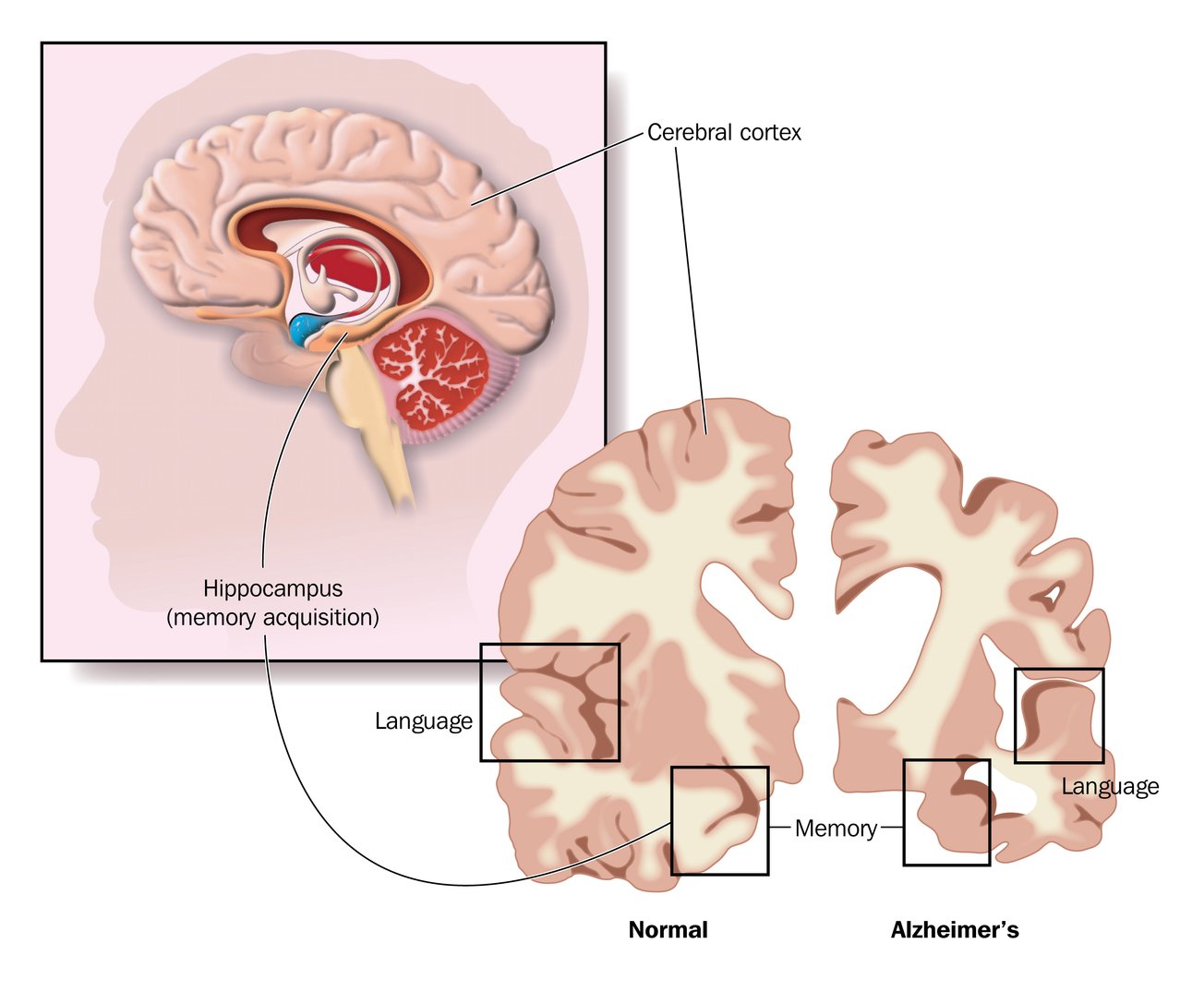
What Part Of The Brain Causes Dementia
It’s caused by an abnormal clumping of proteins, including tau, in the frontal and temporal lobes at the front and sides of the brain. The clumping of these proteins damages nerve cells in the frontal and temporal lobes, causing brain cells to die. This leads to shrinking of these areas of the brain.
Once The Lpa Is Registered
The attorney must follow the Mental Capacity Act when making decisions on behalf of the person with dementia. This means that they:
- must act in the persons best interests
- must consider the persons past and present wishes
- cannot take advantage of the person to benefit themselves
- must keep all of the persons money separate from their own
If an attorney fails to follow these rules, the LPA could be cancelled. The Office of the Public Guardian will investigate if an attorney is suspected of taking advantage of the person with dementia and if so, the attorney could be prosecuted.
It is possible for health professionals to override the views of the attorney in the case of the Health and Welfare LPA, if they believe the persons best interests are not being met. In this instance, the attorneys and the persons friends and family have the right to object to the health professionals decisions. If a person with dementia is detained under the Mental Health Act 1983, this will override the authority of the persons attorney.
Anyone planning to act as an attorney for someone else must read the Mental Capacity Code of Practice, a Government publication explaining the responsibilities ofan attorney. The Code of Practice can be accessed at
Also Check: Dementia Neurotransmitter
When People With Dementia Refuse Help
When a person with dementia is unwilling to do something that we want them to do, this may be described as refusal or resistance.
As with other areas of a persons behaviour that we may find challenging or distressing, we need to try to find out what the person is telling us through their refusal in other words, the reason why they are refusing. And rather than expecting the person with dementia to follow our wishes, we should be focusing on how we can co-operate with their wishes.
Being forced into things makes us upset or aggressive, even fearful.
Christine Bryden
How To Get The Nhs To Pay For Care
Many people find this book a cost-effective starting point, It takes you step-by-step through the whole NHS Continuing Healthcare process, right from the start, including how to approach the NHS, what should happen, the pitfalls to avoid, what to do and say before, during and after an assessment, whats right and whats not, how to challenge decisions, how to pull apart the NHSs assessment notes, etc.
It gives you a firm understanding of the process and lots of useful and practical information.
Also Check: Difference Between Senility And Dementia
When An Involuntary Admission Can Happen
You must not be willing to go into hospital.
You must have one of the following:
- A mental illness.
- Severe dementia.
You can only be admitted if one or all of the following apply to you:
- You pose a serious risk that they may cause immediate and serious harm to yourself or others.
- Your judgement must be so impaired that you need treatment that you can only get in a hospital.
- Your condition could get worse if you don’t get the treatment that could help your mental health.
An involuntary admission can’t happen if you:
- have a sole diagnosis of a personality disorder or social deviance
- are addicted to drugs or alcohol
Individual Preferences And Routines
Each one of us tends to live our life according to a set of routines. Some are imposed by necessity, but many reflect preferences and choices when we go to bed, when we get up, whether we get dressed before we have breakfast or vice versa, and so on.
A person with dementia may refuse to fit in with a routine that does not match their own. This is a positive sign! It shows us that the person still has a sense of their own identity and autonomy. Care services need to be flexible enough to fit in with the individuals routines. For example, if someone has always worked nights, it might be most natural for them to be up and about at night and this should not be seen as a problem. In this situation, the main challenge will be to find ways of engaging the person and providing company when there arent many other people around. In accepting a care service or moving into a care home a person hasnt given up their right to live according to their own standards and routines.
Recommended Reading: Does Neil Diamond Have Alzheimer’s
What Are The Goals Of The Sdcp
The program aims to:
- provide best-practice care, without restraints, in a dementia-friendly environment
- reduce or stabilise a persons behavioural and psychological symptoms within 12 months, on average
- support the persons move into less intensive care settings when they no longer need SDCP care
- work alongside state and territory government services, the Dementia Behaviour Management Advisory Service, and Severe Behaviour Response Teams
- improve quality of life for people living with very severe dementia
Living environments can have a big impact on quality of life for people living with dementia. SDCP units will be designed to:
- be tailored to people living with very severe dementia
- promote familiarity, stimulation and independence
- reduce risks
The SDCP works with key stakeholders to:
- assess and refine the SDCP model
- make sure the model provides the best possible care for people who have very severe dementia symptoms
- form relationships with local health networks, acute mental health services and allied health services
- draw on these relationships for expertise for clinical guidance and support when needed
Consent To Treatment Under The Mental Health Act
Part 4 of the Mental Health Act 2001 defines consent in relation to a patient under the Act as meaning consent obtained freely without threats or inducements where the consultant psychiatrist responsible for the care and treatment of the patient is satisfied that the patient is capable of understanding the nature purpose and likely effects of the proposed treatment and has given the patient adequate information in a form and language that the patient can understand on the nature purpose and likely effects .
Consent of the patient is not required for treatment when in the opinion of the consultant psychiatrist responsible for their care, the treatment is necessary to safeguard the life of the patient, to restore their health, alleviate their condition, or relieve their suffering and by reason of their mental disorder the patient is incapable of giving such consent. In all other circumstances consent is required. .
There are further safeguards in relation to certain highly invasive treatments. Psycho-surgery, even with the written consent of the patient, must be authorised by a Tribunal. Electroconvulsive therapy requires either the written consent of the patient or the approval of the consultant psychiatrist responsible for the patient and a second consultant psychiatrist and must be administered in accordance with the rules published by the Mental Health Commission .
You May Like: Does Prevagen Work For Dementia
Getting Our Approach Right
People may refuse help from some care staff but not others. This is likely to be to do with the quality of relationships and the type of approach. Refusing personal care from a particular staff member may be the persons way of saying I dont know who you are, I dont trust you, Im embarrassed or Youre going too fast. All of these messages can be addressed for example, we can:
- give clear explanations and repeat ourselves as necessary
- not ask for too much at one time
- work at building a closer relationship with the individual, showing that they are valued as a person and not just seen as a focus for a care task
- ensure that we are going at a pace with which the person feels comfortable and safe, not hurried or rushed
- ensure we are respecting their dignity and modesty as much as possible.
Refusing help is how some people communicate their need to believe that they are still independent. It is very important that we respect this and ensure that we help people to do everything that they can still do for themselves. It is often easier for a person to accept help with aspects of a task that they find difficult if they have a sense of achievement gained through completing some parts of the task on their own. For more on these ideas, look at the section on Communicating well.
Help For The People Who Care For You
Any family members or friends who regularly care for you should also get the help they need. If a person who cares for you appears to need support they should be offered an assessment. Help that the person might get could be:
- respite care to give them some rest
- financial support, such as Carers Allowance
Your local council, a doctor or your care coordinator can put your carer in touch with the right local organisation to help them find out more.
Read Also: Did Margaret Thatcher Have Dementia
Refusing Help With Personal Care
Personal care is an intimate activity and most people will experience difficult feelings if they need help with this. Trying to force a person with dementia to accept personal care constitutes abuse. It is a fundamental human right to say no. However, neglecting someones personal care needs can also be abusive, as the persons health may be put at risk. Therefore, it is essential to understand the persons reason for refusing and to address this.
We may need to find an alternative way of providing the personal care the person needs, for example, offering a bath rather than a shower. It will be important to find out as much as possible about the persons previous lifestyle and preferences concerning their hygiene. Perhaps the person always had a bath on Sunday mornings and had stand-up washes for the rest of the week. Then we need to adapt to this routine. Through finding out this background information, observing and listening to the person with dementia, we can gradually build up a picture of the personal care routines and preferences of each individual.
S Of The Mental Health Act You Should Know About
Section 2If your loved one is behaving in a way that possess a danger to their own health, or to the health of others, they can be detained in hospital for an assessment by doctors under this section of the Mental Health act.
But if they agree to go into hospital of their own free will the Mental Health Act does not need to be used, so its always best to try persuading them.
Two doctors need to agree that the section is necessary, one of them must be a dementia specialist, the other is often a GP who knows the person well.
Once the section is in place your loved one will not be allowed to leave the hospital without close supervision, though you can of course visit and advise staff on the best ways to help them stay calm.
The maximum amount of time this sort of section can last is 28 days.
Section 3 This is similar to a section 2 but can last for six months and should only be used if a person needs treatment and refuses to accept it voluntarily. Treatment can mean anything from specialist nursing to medication or psychological therapies.
Section 117 Section 117 requires councils to provide free care home funding, or care at home which is not means tested for patients who are sectioned under Section 3 . Its important to be aware of Section 117 because it might save your loved one quite a lot of money.
Take legal advice if your local council does not offer this funding or decides to withdraw it when youre loved one still needs it.
You May Like: Does Smelling Farts Help Prevent Dementia
Sundowning And Care At Home
Alzheimers and dementia can be difficult conditions to live with, not just for your loved one but also for the extended family. Thats why more and more people are turning to live-in carers to help with loved ones who are in the late stages of dementia. Employing a highly experienced and compassionate caregiver can be a relief to families who are struggling to cope with the demands of the disease, and the peace and calm that a skilled carer can bring to a household are beneficial for everyone.
Live-in carers can provide a range of dementia care services, from simple companion care to the specific demands of dementia. They remain calm under pressure and can cope with emergency situations, making them a great option for families who are concerned about residential care for their loved ones.
They can provide genuine support throughout the day and night, which can make a significant difference for families who are finding things challenging. The cost of live-in care in the UK with Elder starts at £1095 per week.
Even if you think that you are coping well with your loved one, a period of live-in respite care can be helpful for anyone dealing with the particular demands of sundowning, allowing you to return from a short break or holiday refreshed and ready to face the challenges ahead.
Getting funding from your local authority
How Can I Plan Ahead
Loss of mental capacity can happen unexpectedly, so its sensible to make plans in case youre unable to make your own decisions. You can:
- use a Lasting Power of Attorney to appoint someone to make decisions on your behalf. This includes decisions about property and financial affairs as well as your health and personal welfare
- make an advance decision to refuse treatment. This sets out the situations where you would want to refuse medical treatment if you lacked the capacity to make or communicate that in future. Advance decisions are legally binding. However, you cant generally use one to refuse treatment you might be given if youre detained under the Mental Health Act
- make an advance statement. This sets out your wishes, beliefs, feelings and values about your care and treatment in case youre unable to communicate them in future. It isnt legally binding but can help family, friends and medical professionals make decisions on your behalf.
Mind and Compassion in Dying have produced a factsheet about how advance decisions and advance statements work.
Read Also: What Is The Color For Dementia
Consent To Clinical Trials
Clinical trials in Ireland are governed by the European Communities Regulations, 2004, SI No 190 of 2004. The Regulations transposed into Irish law the provisions of Council Directive 2001/20/EC. The regulations supersede the Control of Clinical Trials Acts 1987 1990 for clinical trials using medicinal products.
There are safeguards in place governing the participation of incapacitated persons in clinical trials. In addition, the Clinical Trials Regulation No 536/2014), which is due to come into force in 2016, also contains extensive provisions relating to protection of those participating in clinical trials, including incapacitated persons.
Anyone who is a patient with a mental disorder in an approved centre under the Mental Health Act 2001 cannot take part in a clinical trial .
How An Involuntary Admission Happens
There are 3 stages.
Also Check: What’s The Difference Between Dementia And Alzheimer’s And Senility
Three Facts Worth Knowing
A section should only ever happen as a last resort when all other alternatives have been explored. If you dont think this has happened you can challenge it . A section is designed to protect, not punish, the person with dementia and keep them safe from harm. In 2012/3 nearly 9000 people over 65 were sectioned under the Mental Health Act, at least half of these were estimated to be sectioned as a result of severe dementia.
What Can Cause A Lack Of Mental Capacity
Lack of mental capacity can be caused by many things. It can be:
- permanent, where someones ability to make decisions is always affected. This could be because of a stroke or brain injury, severe dementia or learning disability
- temporary, where someone has capacity at some times but not others. This could be because of a mental health problem, substance or alcohol misuse, or confusion, drowsiness or unconsciousness because of an illness or treatment.
Don’t Miss: What Is The Color For Dementia