What Are The Treatments For Chorea
Some people may not be aware of their chorea others may view their mild symptoms simply as a nuisance or perhaps as a social embarrassment. However, if your chorea is severe or disabling or interferes with the quality of your life, you should see your doctor for treatment.
The type of treatment depends on what is causing the movement disorder.
Inability To Block Out Distractions
Eating a meal while watching television or listening to music can be very difficult for a person with Huntington’s disease, because they cant concentrate on both things at once. Thats why it is recommended that meals should be eaten in a quiet environment.
Suggestions for family members, friends and carers include:
- Encourage the habit of doing one thing at a time.
- Remember that activities we take for granted, such as walking, can require concentration for the person with HD. They may not be able to carry on a conversation at the same time.
How Common Is Chorea
No one knows for sure how many people experience chorea. Chorea is usually a symptom of another disorder. About 30,000 people in the United States have Huntingtons disease . Doctors estimate another 200,000 people have a risk of developing Huntingtons disease because their parents have the genetic condition. Chorea is the most common symptom of Huntingtons disease.
In the United States, about 4,000 kids a year develop Sydenham chorea after having rheumatic fever. Rheumatic fever is a serious complication of untreated strep throat. Girls are more likely than boys to get rheumatic fever. It usually occurs between 5 and 15 years of age.
Recommended Reading: Alzheimer’s Color Ribbon
Who Is Affected By Chorea
Chorea can occur in people of all ages. However, certain groups of people have an increased risk, including:
- People with a family history of Huntingtons disease: If you have a parent with Huntingtons disease, there is a 50% chance youll inherit the disease. Usually, people develop symptoms of Huntingtons disease between ages 40 and 50. Huntingtons disease is the most common inherited type of chorea.
- Children who have had rheumatic fever: Kids and adolescents can develop Sydenham chorea after rheumatic fever, which is a complication of untreated strep throat.
- People with other medical conditions: Autoimmune diseases and hormonal disorders like hyperthyroidism and metabolic disorders such as hypoglycemia can cause chorea. There is a long list of other disorders that can cause chorea.
Predominant Movement Disorder Presentation
Progressive Supranuclear Palsy
Table 1. Chameleons of PSP and CBS.
Corticobasal Syndrome
Because of the overlapping phenotypes, whether PSP and CBD are two different disorders or are part of a spectrum, is a matter of debate . Phenotypically, PSP and CBD pathology both can present as speech/language dysfunction , frontal cognitive/behavioral presentation , Richardson’s syndrome, and corticobasal syndrome . Interestingly, if a patient presents with VSGP or slowing of vertical saccade, axial or symmetric limb rigidity or akinesia, limb apraxia, and postural instability, the patient can be classified as PSP-CBS or CBD-PSP. To get rid of this conundrum, Movement Disorder Society criteria for PSP have introduced the novel diagnostic category probable 4R-tauopathy for joint clinical recognition of the patients with PSP and CBD pathology and to facilitate the research on 4R-tau targeted therapeutic strategies . Probable 4R-tauopathy includes possible PSP with SL and possible PSP with CBS apart from all probable PSP.
On top of this, vertical gaze palsy can be seen in a lot of other disorders apart from PSP-RS and asymmetric dystonic stiff limb presentation can be seen in other disorders besides CBS. Thus, clinicians should always be aware of these look-alikes of PSP and CBS .
Table 2. Mimics of PSP and CBS.
Don’t Miss: Alz Ribbon
What Are The Complications Associated With Chorea
Depending on the cause of chorea, complications can be severe. Huntingtons disease is an ongoing disease that gets worse over time and has no cure. Although there is no cure for lupus, doctors can help you manage the disease with medications. Children who develop Sydenham chorea after rheumatic fever usually recover without long-term medical problems.
What Are Risk Factors For Chorea
People with a history of rheumatic fever are more likely to experience chorea. Other risk factors are related to risks for a specific disease.
For example, Huntingtons disease is a hereditary disorder that may cause chorea. A person with a parent who has Huntingtons disease has a 50 percent chance of inheriting the disease, according to the Mayo Clinic.
Because many conditions cause chorea, your doctor must request a thorough medical history to determine potential causes. To diagnose chorea, your doctor may ask:
- When did the symptoms begin?
- What makes the symptoms better or worse? Do your chorea symptoms tend to worsen when youre stressed?
- Do you have a family history of Huntingtons disease?
- What medications are you taking?
Some laboratory tests can indicate chorea. For example, abnormal copper levels in your body can indicate Wilsons disease, a genetic disorder that causes chorea.
Tests for spiky erythrocytes or red blood cells can indicate chorea-acanthocytosis. Blood tests for parathyroid hormones or thyroid hormones can indicate metabolic or endocrine-related chorea.
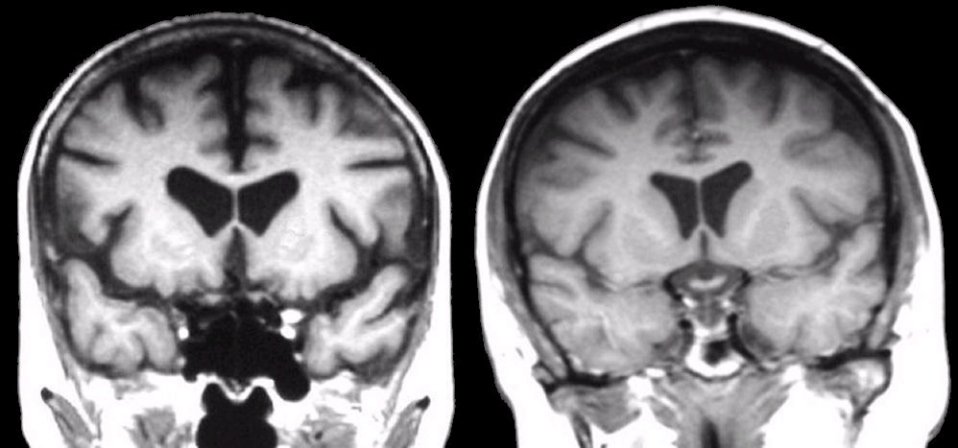
For Huntingtons disease, imaging studies, such as MRI scans, can show brain activity thats an indicator of the disease.
Recommended Reading: How To Get A Person With Dementia To Shower
How Is Chorea Diagnosed
Because so many conditions and disorders can cause chorea, your doctor will ask a range of questions about your family history, the medications you take, and any symptoms youre having besides uncontrollable movements. Your doctor will also conduct a physical exam and ask how often and how long your uncontrolled muscle movements have been happening and whether they get worse during times of stress.
To determine the cause of chorea, your doctor may order:
- Blood tests to check for infections, lupus, thyroid levels or other endocrine or metabolic abnormalities.
- Imaging studies such as magnetic resonance imaging scan or a computed tomography scan to look for changes in your brain.
- Genetic testing to see if you have the gene for Huntingtons disease.
Predominant Cognitive Or Mixed Presentation
Three other primary tauopathies namely globular glial tauopathy , argyrophilic grain disease and Pick’s disease present as cognitive or mixed . Clinical, radiological, and pathological features of these entities have been described in Table 3.
Table 3. Clinical, radiological, and pathological clues for GGT, AGD, and PiD.
Don’t Miss: Dementia Ribbon Tattoo
What Is Mitochondrial Disease
Mitochondrial Disease – Dementia and Chorea is a rare disease. There are currently no additional known synonyms for this rare genetic disease.
The clinical picture is that of a mid-life progressive dementia, with chorea, ataxia, and a peripheral neuropathy. The patient was deaf but had no primary muscle weakness . There were, however, ragged red fibres. A mutation was found in a highly conserved position in tRNA tryptophan.There has been another family reported with a tRNA tryptophan mutation .The clinical picture was very variable. An infant had a progressive encephalopathy, whereas a 16 month old child was normal except for optic disc pallor and basal ganglia hyperdensities. Previous generation maternal line relatives had depression and even psychosis. A child with early onset deterioration, optic atrophy and hypertonia had the single T insertion nt5537 in the tRNATrp gene . COX was deficient and the radiology was that of Leigh disease.
* This information is courtesy of the L M D. If you find a mistake or would like to contribute additional information, please email us at:
*This computer-generated image is for illustration purposes only
Huntingtons Disease And Behavioural Challenges
Behavioural challenges associated with Huntington’s disease are thought to be caused by a combination of events, including damage to the brain as the disease progresses, and the frustration and depression that people feel when challenged by chronic illness.
Not all people with Huntington’s disease will experience the same behavioural problems, since the disease affects people differently. The severity of behavioural changes can range from mild and barely noticeable to enormously disruptive. It is important for family, friends and carers to appreciate that the persons behavioural changes are often part of the disease and are not under their conscious control.
Also, people with Huntingtons disease may be trying to express their needs or wants but due to their limited ability to articulate themselves or do things independently, this expression comes out in a way that can be seen as a behavioural issue.
Read Also: Alzheimers Ribbon Color
What Are The Signs Of Chorea
Chorea symptoms usually depend upon the condition causing it. A common symptom is milkmaids grip. People with this condition dont have coordinated hand muscles and will squeeze and release their hand, as if milking. Another symptom is involuntarily sticking out the tongue.
Chorea movements can be fast or slow. A person may appear to be writhing in pain and have no bodily control. These movements have also been called dance-like or similar to piano playing.
Conditions associated with chorea and its symptoms include:
How Do People Get Chorea
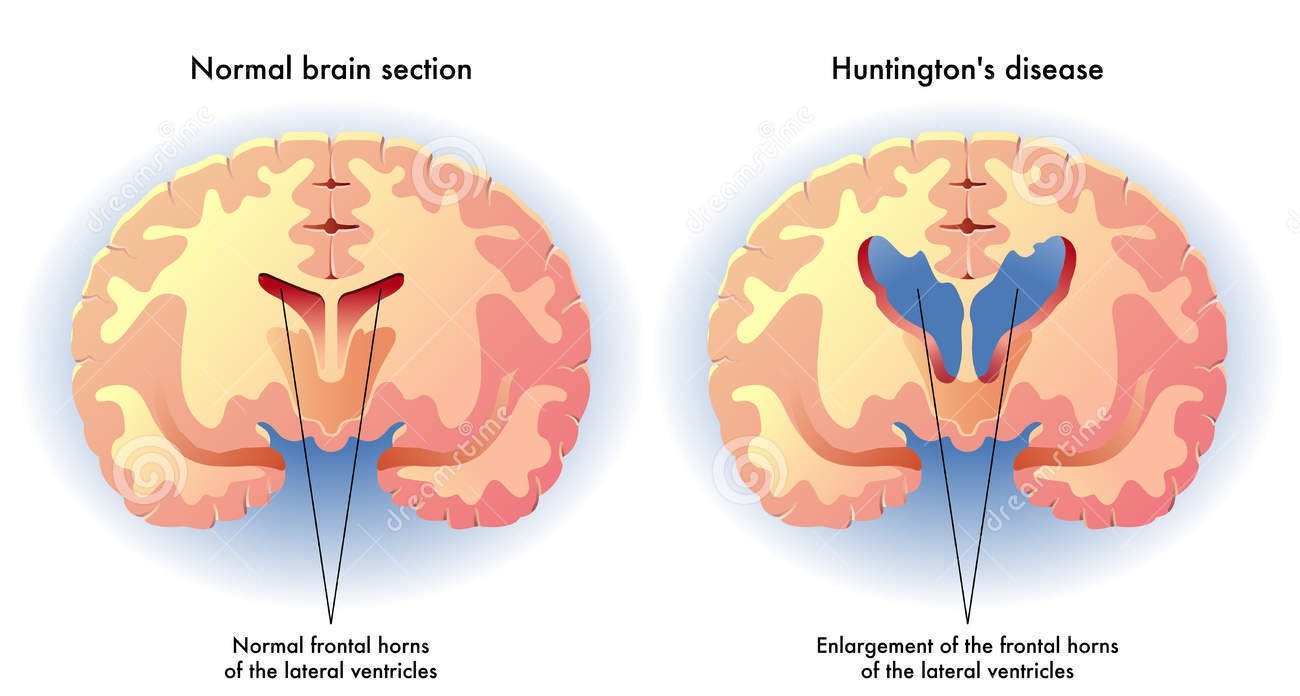
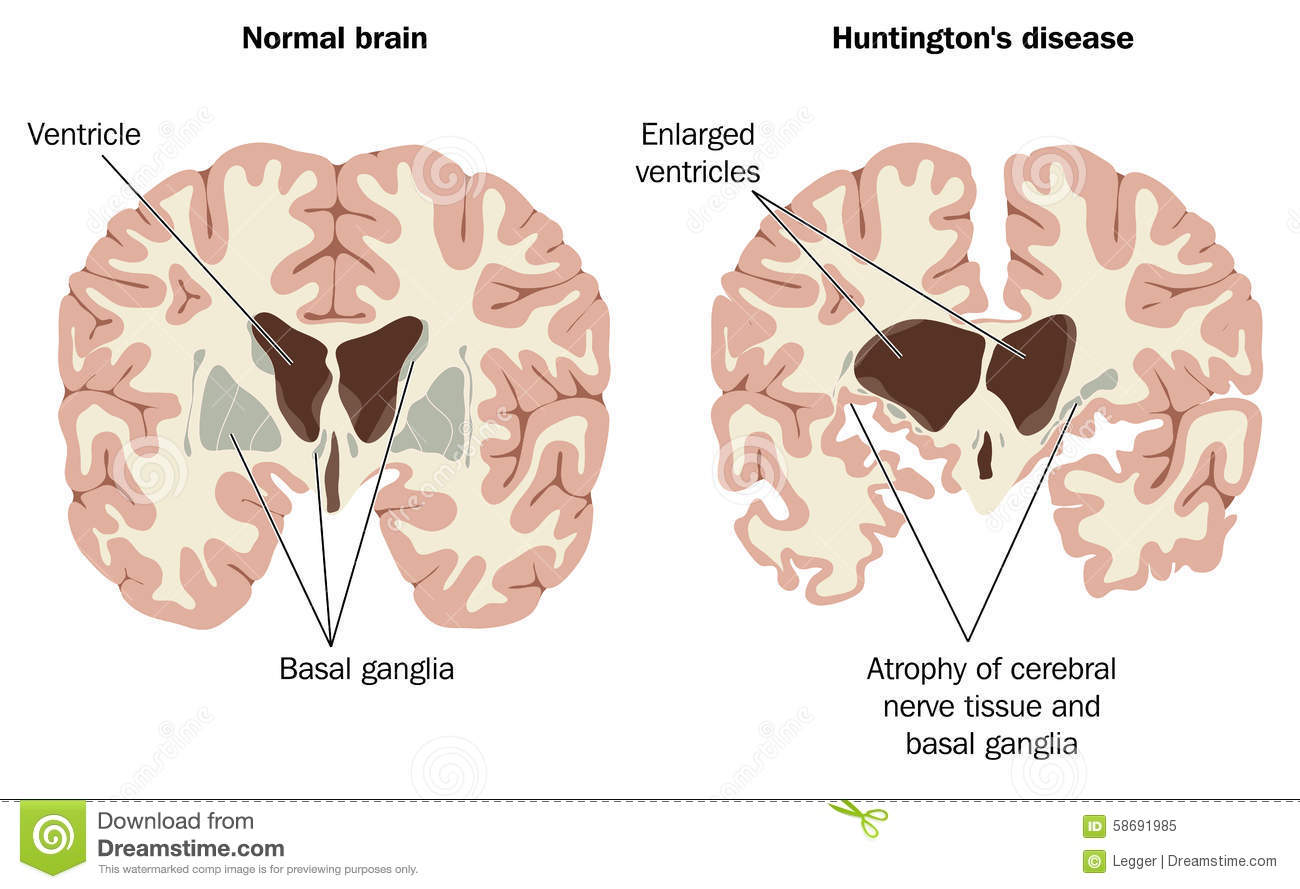
Chorea is a neurological symptom that originates in an area of the brain called basal ganglia, which are collections of nerve cells deep inside the brain that control movement. Dozens of genetic conditions, autoimmune diseases, metabolic disorders, infections and medications can affect basal ganglia and lead to the onset of chorea.
The most common causes of chorea are:
You May Like: How Long Do You Live After Being Diagnosed With Alzheimer
Box : Clinical Features Of Neuroacanthocytosis
-
A multisystem degenerative disorder of unknown aetiology.
-
Variable mode of inheritance.
-
Age of onset: approximately 30 years.
-
Chorea as well as orofacial-lingual dystonia are prominent.
-
Axonal neuropathy in 50% of cases.
-
Presence of acanthocytes on peripheral blood smears.
-
No curative treatment available treatment is largely supportive.
-
Relentlessly progressive .
How Is Chorea Treated
Treatment of chorea depends on the type of chorea you have. It aims to treat the underlying condition, which will help with chorea symptoms.
For example, Sydenhams chorea may be treatable with antibiotics. Huntingtons disease chorea can be treated with antipsychotic drugs, as well as other medications.
Chorea due to Parkinsons disease has no cure, but symptoms can be managed.
Read Also: Etiology Of Alzheimer’s
Other Causes Of Chorea
Metabolic alterations including hyperglycaemia and hypoglycaemia, hypernatraemia and hyponatraemia, hypomagnesaemia, hypocalcaemia, and hepatic or renal failure have been implicated in the development of various movement disorders including chorea. Correction of the metabolic abnormality leads to the resolution of the movement disorders. Postoperative encephalopathy with choreoathetosis or postpump choreoathetosis is a recognised complication of childhood cardiac surgery.
Exposure to various toxins including alcohol, amphetamines, heroin, glue sniffing, thallium, and mercury can cause choreiform movements. The movements can be transient or permanent. Intoxication with carbon monoxide, methanol, cyanide, or manganese produces bilateral necrosis of the pallidum, causing unconsciousness or parkinsonism. Involuntary movements can be a delayed sequel to acute high level exposure and disappear after a few months.Chorea can also occur in the setting of paraneoplastic syndrome associated with small cell lung carcinoma, renal cell carcinoma, and lymphoma.
Diseases Of The Nervous Systemtype 2 Excludes
- Altered behavior in huntington’s dementia
- Dementia due to huntington chorea
- Dementia due to huntington chorea with altered behavior
- Dementia due to huntingtons disease
- Dementia due to huntingtons disease w behavioral disturbance
- Dementia from huntingtons chorea
- Huntingtons chorea
- 056 Degenerative nervous system disorders with mcc
- 057 Degenerative nervous system disorders without mcc
- : New code
- 2017
Also Check: What Color Is For Alzheimer’s
Genetics Of Huntingtons Disease
Huntington’s disease is caused by an altered gene. This gene is passed on from parent to child, but the condition isnt obvious at birth or during childhood except in rare cases, which is known as Juvenile Huntingtons Disease. The symptoms usually, but not always, first appear when the person is approaching middle age. Huntington’s disease is a slow, progressive condition that affects people differently.
A person with Huntington’s disease may live for 15 to 25 years after developing the first symptoms. Diagnosis is based on a family history of Huntington’s disease , genetic testing, plus assessment of physical, neurological and emotional symptoms. There is currently no cure for Huntington’s disease.
A Practical Clinical Approach To Tauopathies And Movement Disorders
Considering tauopathies from a movement disorder perspective, interlacing clinical phenotypes and pathological, genetic heterogeneity often make it difficult to diagnose them clinically. Some clinical pointers like VSGP, frontal disinhibited behavior, amyotrophy, prominent language involvement, chorea, and cerebellar ataxia can be helpful clues for the clinician on this regard .
Figure 2. Clinical pointers for diagnosing tauopathies. *Novel tauopathies, +DDPAC, disinhibitiondementiaparkinsonismamyotrophy complex related to MAPT mutation .
Read Also: Does Diet Coke Cause Dementia
What Is The Outlook For Patients Who Have Chorea
The outlook depends on whats causing the involuntary muscle movements. People with Huntingtons disease can live 15 to 25 years after they develop symptoms. The condition slowly gets worse over time and makes it very difficult to do everyday activities like dressing, bathing and eating.
Children who develop Sydenham chorea after rheumatic fever usually recover within 2 years. Some children may have lingering behavioral or emotional issues, such as obsessive compulsive disorder . These issues can last a lifetime.
Chorea itself usually can be managed with currently available treatments.
Predominant Language Dysfunction Presentation
Progressive Nonfluent Aphasia or Agrammatic Variant of Primary Progressive Aphasia
PNFA/PPA-G can clinically present with . AOS manifests as slow, labored, effortful, hesitant speech with inconsistent speech sound error and aprosody. Groping after the target sound is characteristic. Patients have difficulty to utter polysyllabic words and sequences of syllables . Phonemic speech sound errors are more common . Errors in grammar mainly affects syntax, function words, use of conjunction and verb . Clinically, PPA-G must be differentiated from the semantic variant PPA-S and logopenic variant PPA-L . Orofacial apraxia is a common association with PPA-G. Signs of PSP or CBS may arise as the disease evolves . Predominately left peri-sylvian atrophy involving left posterior fronto-insular region is seen in MRI brain . Around 30% of the cases are genetic and association with MAPT, PGRN and C9orf72 have been reported . PSP pathology is common in AOS variant with more dysarthric presentation and CBD pathology with more sentence comprehension deficit . Sometimes PiD pathology, TDP43-A pathology if there is associated ALS or AD pathology is also seen .
Don’t Miss: Does Prevagen Help With Dementia
Stage : Age Associated Memory Impairment
This stage features occasional lapses of memory most frequently seen in:
- Forgetting where one has placed an object
- Forgetting names that were once very familiar
Oftentimes, this mild decline in memory is merely normal age-related cognitive decline, but it can also be one of the earliest signs of degenerative dementia. At this stage, signs are still virtually undetectable through clinical testing. Concern for early onset of dementia should arise with respect to other symptoms.
What Gene Changes Cause Mitochondrial Disease
The syndrome is inherited in the following inheritance pattern/s:
Mitochondrial – Mitochondrial inheritance is passed solely through theMother. It involves the genes found in our mitochondrialDNA. Mitochondria are passed through the egg cells.
In some cases, a genetic syndrome may be the result of a de-novo mutation and the first case in a family. In this case, this is a new gene mutation that occurs during the reproductive process. The syndrome can be caused by mutations in the following gene/s location/s: N/A
*This computer-generated image is for illustration purposes only
Read Also: Does Diet Coke Cause Alzheimer’s
My Doctor Mentioned Athetosis Is Athetosis The Same Thing As Chorea What Is Choreoathetosis
Athetosis is a form of chorea that is slow and writhing in quality. Most movement disorders neurologists consider it a form of chorea, and often athetosis can change over time into chorea and vice versa. When both chorea and athetosis occur at the same time, it is sometimes referred to as choreoathetosis. Athetosis and choreoathetosis can sometimes be mistaken for another involuntary movement called dystonia.
Do Patients With Parkinsons Disease Get Chorea
In patients who take medications to treat the symptoms of Parkinsons disease, the medications can cause choreic movements that are more commonly referred to as dyskinesias. These movements occur secondary to the anti-parkinsonian medications and are not caused by Parkinsons disease directly. Medications that are used to treat Parkinsons disease can sometimes cause other abnormal movements as well, such as dystonia.
Also Check: What Causes Senile Dementia
Classification Of Tauopathiescurrent Status And Pitfalls
Tauopathies have been conventionally classified from a pathological perspective into two groups Primary tauopathies where tau is the predominant pathology including three repeat and four repeat tauopathies, Secondary tauopathies where additional etiologies are involved for tau deposition . However, some tauopathies are geographically isolated like Guadeloupean parkinsonism , Western pacific amyotrophic lateral sclerosis and parkinsonism-dementia complex , and Nodding syndrome of northern Uganda . While exact etiopathogenesis of these geographically isolated tauopathies are still unknown, environmental impact has been highlighted in many studies. Thus, whether to include them in the group of secondary tauopathies or not, is still a matter of debate.
Figure 1. Classification of tauopathies.
Recently, Hõglinger et al. have highlighted syndromic classification of tauopathy based on the predominant domain affected :
1. Cognitive syndromes: Behavioral variant of frontotemporal dementia , non-fluent agrammatic variant of primary progressive aphasia , semantic variant of primary-progressive aphasia , and amnestic syndrome of hippocampal type .
2. Motor syndromes: Richardson syndrome , Parkinson syndrome , corticobasal syndrome , primary gait freezing , cerebellar syndrome , and primary lateral sclerosis .
Clinical Summary Of Cases
Demographic data
The clinical features of the three patients with chorea and the other FTLD-FUS cases are summarized in Table . More detailed clinical descriptions are provided in Japanese for cases 1 , 2 , and 3 . The three patients with chorea had no family history of dementia. Mean age at symptom onset for these patients was significantly younger than for other FTLD patients obtained from a consecutive clinical cohort in our archives.
Table 2 Clinical features of FTLD-FUS
Psychiatric, behavioral, cognitive, and language disturbance characteristics
The most frequent initial symptoms in the patients with chorea were apathy and behavioral abnormalities, such as criminal behavior and loss of manners, followed by polyphagia, disinhibition, and memory impairment. All three patients presented with a behavioral abnormality as the prominent feature during the disease course, and were finally diagnosed with bvFTD. Apathy, disinhibition, stereotypy, altered dietary habits, perseveration and memory impairment were the most prominent clinical features in this group. Wandering, hypersexuality, and an oral tendency were observed in two cases. Regarding language disturbances, echolalia and reduced speech output were observed in all three patients, and verbal stereotypies in two. No dysarthria or semantic errors were recognized in this group.
Neurological signs
BIBD compared with all FTLD cases
Table 3 The demographic data and major clinical features of all FTLD cases
Don’t Miss: Alzheimer’s Disease Color Ribbon