How Do Physicians Ensure That The Person Has The Correct Diagnosis
Diagnosing both schizophrenia and dementia can be challenging. The challenges increase when a person already has one of the two conditions.
There is no single definitive test for dementia. While tests can show that a person has declined in cognitive function, these tests cannot conclusively prove that dementia is the cause, or determine which type of dementia a person has. That said, the testing can help to determine which diagnosis is more or less likely.
Instead, doctors use a combination of tests , such as bloodwork and brain scans, to look for dementia markers, including signs of plaques in the brain. However, not all people with dementia develop brain signs of the disease, and some people with plaques or other symptoms do not have dementia.
Similarly, no single test can prove that a person has schizophrenia, and doctors do not use brain scans or blood tests to diagnose this condition. Rather, such as delusions, hallucinations, socially unacceptable behavior, and a disconnection from reality.
Some of these symptoms are similar to dementia.
Certain types of dementia, especially frontotemporal dementia, are easy to confuse with schizophrenia. Frontotemporal dementia affects behavior and mental health, potentially causing aggression, impulse control, and hallucinations. It also tends to appear earlier in life than Alzheimers, making it even easier to mistake for schizophrenia.
The Risk Of Dementia In Late
Late-onset schizophrenia is usually defined as onset after 40 years of age, and very-late-onset as after 60 years of age. Studies of schizophrenia of late and very late onset are few and inconsistent in their results.
Reference Palmer, Bondi and TwamleyPalmer et al compared changes in cognition over 1 and 2 years for out-patients with late-onset schizophrenia-spectrum disorders, earlier-onset schizophrenia-spectrum disorders, Alzheimers disease with psychosis, or Alzheimers disease with baseline MMSE scores > 25, and healthy comparison participants. Cognitive changes among participants in the two schizophrenia-spectrum disorder groups were similar to those in the healthy controls, whereas both Alzheimers disease groups showed greater declines in cognition. The authors concluded that late-onset schizophrenia is a neurodegenerative disorder and, in agreement with earlier studies, a static encephalopathy.
This Danish study suggests that, although people with late-onset and very-late-onset schizophrenia have an increased risk of developing dementia, it does not seem to be due to an increased risk of developing Alzheimers disease, thus pointing to the possibility that they are developing a different type of dementia.
Box 1 summarises the evidence from international studies.
BOX 1 Cognitive impairment in schizophrenia
Cognitive impairment is a feature of schizophrenia
Over 25% of older people with schizophrenia have moderate to severe cognitive impairment
The Difference Between Sociopath And Schizophrenia
is that “sociopath” is a person with an antisocial personality disorder, exhibiting antisocial behavior that usually is the result of social and environmental factors in the persons early life and “schizophrenia” is a psychiatric diagnosis denoting a persistent, often chronic, mental illness characterised by abnormal perception, thinking, behavior and emotion, often marked by delusions.
Also Check: Senile Vs Dementia
Main Outcome Measure And Definition
Diagnoses of dementia were obtained from the DPCR and the DNPR . Diagnoses of the main outcome Alzheimer’s dementia were obtained . The date of dementia onset was defined as the first day of hospital contact with a diagnosis of dementia in either the DPCR or the DNPR . All analyses were also performed for vascular dementia and unspecified dementia .
Schizophrenia Risk Of Dementia

Dementia occurs around age 65 or later. The destruction of brain cells by the disease causes progressive problems with memory and other cognitive functions, such as spatial orientation, reasoning, language and abstract thinking. People with dementia experience many physical and psychological difficulties and often become anxious, agitated, aggressive and sometimes psychotic. Psychiatric challenges caused by dementia can be treated and medications can slow down the disease process, but only for months rather than years. This lifelong disease cannot be cured, but it can be controlled with proper treatment.
New research shows that every disease affects the same area of the brain, even though dementia and schizophrenia are completely different diseases. People with schizophrenia are at increased risk for several medical conditions, including obesity, diabetes, hyperlipidemia, and cardiovascular disease. All of these medical conditions are associated with an increased risk of dementia.
Common symptoms of dementia include:
- Memory lapses
- A diminishing attention span
- Difficulty communicating
Also Check: Alzheimers Ribbon Color
Increased Risk Of Dementia In Individuals With Schizophrenia
The finding of no familial coaggregation between schizophrenia and Alzheimer’s dementia is conflicting with the growing body of literature emerging of an intriguing relationship between schizophrenia in the individual and the development of dementia . However, whereas most of the studies investigating coaggregation used Alzheimer’s dementia as the main outcome measure, the studies investigating schizophrenia in the individuals themselves used all-cause dementia .
How Does Someone With Schizophrenia Feel
The symptoms of schizophrenia are usually classified into: positive symptoms any change in behaviour or thoughts, such as hallucinations or delusions. negative symptoms where people appear to withdraw from the world around then, take no interest in everyday social interactions, and often appear emotionless and flat.
Recommended Reading: Pathophysiology Of Dementia Disease
Assessment Of Cognitive Function
Many studies have shown that the MMSE is not adequate to pick up cognitive deficits in complex disorders such as schizophrenia. There is evidence that the MMSE scores of people with schizophrenia remain relatively stable over time . It will therefore take a long time for changes in cognitive function to become apparent using this measure.
The MATRICS Consensus Cognitive Battery assesses seven putatively separable domains of cognitive dysfunction in schizophrenia . In an ideal world, this tool could be used with every patient. However, practical and economic constraints facing many clinics and treatment settings make this unfeasible. Studies have shown that impairments on digitsymbol substitution tasks have the largest effect sizes among many different measures for characterising cognitive impairment in schizophrenia.
Another consideration is whether it is necessary to carry out a formal assessment of cognition, given that many clinicians will not have any experience in administering such measures. Scales such as the Schizophrenia Cognition Rating Scale may be easier for clinicians to administer as they are similar in format to a traditional diagnostic assessment.
A study involving a sample of elderly patients with schizophrenia concluded that the ADAS-L Cog reliably and validly assesses cognition in the presence of severe cognitive impairment. The authors felt that the CERAD battery was not adequate in a particularly low-functioning population.
BOX 4 Cognitive testing
Behavior Disorders Of Dementia: Recognition And Treatment
ABI V. RAYNER, M.D., M.P.H., JAMES G. OBRIEN, M.D., and BEN SCHOENBACHLER, M.D., University of Louisville School of Medicine, Louisville, Kentucky
Am Fam Physician. 2006 Feb 15 73:647-652.
Patient information: See related handout on dementia, written by the authors of this article.
Virtually all patients with dementia will develop changes in behavior and personality as the disease progresses.1 The nature and frequency of symptoms vary over the course of the illness, and psychotic features tend to present later, particularly when the patient becomes more dependent. Psychotic manifestations and other behavior problems may be more troubling and challenging than cognitive losses these features result in an increased burden for caregivers, earlier institutionalization, and an acceleration in cognitive decline.2
Psychotic features of dementia include hallucinations , delusions, and delusional misidentifications. Hallucinations are false sensory perceptions that are not simply distortions or misinterpretations. They usually are not frightening and therefore may not require treatment. Delusions are unshakable beliefs that are out of context with a persons social and cultural background. Delusional misidentification may result from a combined decline in visual function and cognition.2 For example, patients may suspect that their family members are impostors , believe that strangers are living in their home, or fail to recognize their own reflection in a mirror.
Also Check: How To Change Diaper Of Dementia Patient
In What Stage Of Dementia Are Hallucinations And Delusions Most Likely To Occur
The type of dementia most associated with hallucinations is Lewy body dementia, which affects about 1.4 million people in the U.S. and is the third-most-common type of dementia . People with Lewy body dementia will often see colorful people or animals that arent actually present, often for a few minutes at a time. This is actually more likely to occur in the early stages of the disease than later. People with Lewy body dementia, in fact, often have hallucinations early and then, as they enter the middle stages, the hallucinations will go away completely as other symptoms, like problems walking, get worse.
People with Alzheimers disease have been shown to sometimes have hallucinations, as have people with Parkinsons disease with dementia. This is rarer, however, and delusions are much more common with these illnesses. Both hallucinations and delusions in people with Alzheimers often occur in the late-middle to later stages of the disease.
The Innovation Gap And Translational Applications To The Prevention And Treatment Of Ad And Schizophrenia
Progress in conquering AD, schizophrenia, and related disorders is hampered by the so-called Innovation Gap , which is a collection of challenges that includes: the fact that the number of approved treatments has not increased despite substantial increments in the investment toward the discovery and testing for this purpose over decades, the frequent lack of predictive power for the efficacy in humans of the outcomes of testing in so-called models of the disorder, and in the case of AD, the failure of all trials published to date based on the overwhelmingly dominant amyloid hypothesis of AD pathogenesis . If the 4EC hypothesis is correct, it would open an essentially unexplored avenue for research and treatment development that could have a powerful effect in overcoming the IG. Similar challenges apply to schizophrenia, given the shared lack of an understood etiology and pathophysiology, and despite the larger number of therapeutic agents available since these like in AD palliate but do not cure the disorder.
Read Also: Neil Diamond Alzheimer’s
Schizophrenia And Dementia Incidence
The multivariable adjusted RRs of dementia incidence in respect of schizophrenia from a single study and the combined RR are presented in . In , all studies reported data on both men and women. The meta-analysis demonstrated that patients with schizophrenia, compared with non-schizophrenia subjects, had a significantly higher risk of developing dementia, based on the six studies . Heterogeneity was significantly observed . The forest plots of multivariable RRs and 95% CIs for dementia incidence and schizophrenia are shown in .
Meta-analysis of the association between schizophrenia and dementia incidence. The random-effects model was used. There was a highly significant difference between the two groups .
Note: Weights are from random effects analysis.
Abbreviation: RR, relative risk.
Relationship Dementia And Schizophrenia
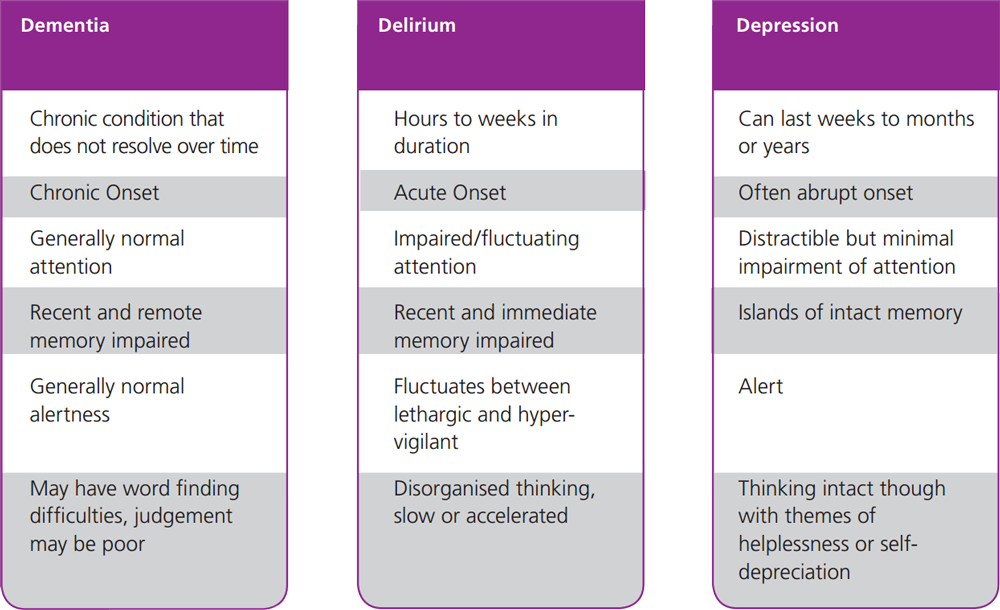
There are many similarities between the two, as well as some key differences. Mental illness can exhibit the same symptoms as dementia and vice versa. It is common for mental illnesses, particularly depression, to occur in the early stages of dementia illness. But accurate diagnosis and treatment are known to improve cognitive function. It is quite challenging to live with dementia but the symptoms are exacerbated in conjunction with other mental disorders such as anxiety, depression and psychotic conditions. Depression is often mixed with the belief that it is simply the reaction of an older adult and awareness of progressive decline. Anxiety can include anything from general nervousness and fear of leaving the house to agitation from routine changes and feelings of suspicion or paranoia. Stress can also be psychologically and physically related to dementia.
The research found that the brain regions that developed last were also the first to deteriorate with advancing age. These areas seem to be more susceptible to schizophrenia and dementia than other parts of the brain, although the two diseases have different origins and appear at almost opposite and completely different moments in life. Now, most research confirms that the same brain regions are affected in dementias disease and schizophrenia.
Also Check: Does Diet Coke Cause Dementia
More Than A Quarter Had A Dementia Diagnosis By Age 66
byKara Grant, Enterprise & Investigative Writer, MedPage Today March 10, 2021
Prevalence of dementia by the time of Medicare eligibility was significantly elevated among individuals with schizophrenia, a retrospective cohort study found.
Using data from a national sample of Medicare recipients, the prevalence of diagnosed dementia by age 66 was 25 times greater for patients with schizophrenia, at 27.9% versus 1.3% in individuals without a history of serious mental illness , reported T. Scott Stroup, MD, MPH, of Columbia University in New York City, and colleagues.
By age 80, prevalence in these groups increased to 70.2% and 11.3%, respectively, according to the findings in JAMA Psychiatry.
In those without a prior history of dementia, the annual incidence of dementia diagnoses at age 66 was 52.5 per 1,000 person-years among the schizophrenia group, but only 4.5 per 1,000 person-years among those without a past SMI. By 80, incidence of dementia diagnosis increased to 216.2 per 1,000 person-years for those with schizophrenia and to 32.3 per 1,000 person-years for the comparator group.
“When aging and other risk factors for dementia start accumulating, might cross a threshold for dementia diagnosis much sooner,” Stroup told MedPage Today.
Stroup’s group acknowledged that the study’s most significant limitation was that clinical diagnoses could not be individually confirmed or validated.
Disclosures
Primary Source
JAMA Psychiatry
How Is Psychosis Treated
Treatment is most effective when psychosis is identified and treated early. The treatment of psychosis typically includes a combination of the following:
- Medications. Antipsychotic medications can help to reduce the symptoms of psychosis. These medications can be given as either a pill or an injection.
- Therapy. Therapy for psychosis often consists of cognitive behavioral therapy provided by a mental health professional. It may be provided in an individual or group setting. CBT in this case is specifically tailored to symptoms of psychosis or schizophrenia.
- Family support. Family members are also key in treating psychosis. Its important for them to learn more about psychosis and how to interact effectively and empathetically with their loved one.
- Social support. Someone experiencing psychosis may benefit from social skills training or help with returning to work or school.
Additionally, since a variety of other underlying conditions can also cause psychosis, working to manage those conditions can also help to ease symptoms.
Recommended Reading: Is Senility The Same As Dementia
Schizophrenia Prs Is Associated With Ad Psychosis Status
After clumping, 76,213 independent variants were available for computing PRS. Random effects meta-analysis across the 11 cohorts showed the largest OR for the schizophrenia PRS at PT=0.01 and this was significantly associated with symptom status across the psychosis wide, psychosis narrow and delusions narrow phenotypes despite the progressively smaller sample size in each of these groups . PRS was also significantly associated with both the psychosis narrow and delusions narrow phenotypes at every PT> 0.01. The largest effect size was observed in the delusions narrow group. Overall, there was no evidence of significant heterogeneity I2 statistics were close to 0% for PT=0.01 across the three phenotypes.
Fig. 1: Odds ratios from random effects meta-analysis of AD psychosis wide, narrow and delusions narrow association with schizophrenia PRS.
Each bar represents PRS composed of markers at ten different schizophrenia GWAS P value thresholds . P values shown above each bar
How Is Schizophrenia Treated
Schizophrenia is a chronic condition for which theres no cure. As such, treatment focuses on managing symptoms and building coping skills for daily life and functioning. It can include a combination of the following treatments:
- Medications. Antipsychotic medications can help with the psychotic symptoms of schizophrenia. These include medications to treat acute psychosis, followed by maintenance medications to help prevent symptoms from returning.
- Therapy. Therapy, which can include CBT, is an important part of treatment. A mental health professional can also help a person with schizophrenia develop coping strategies and teach them how how to recognize signs of a recurrence.
- Family support. Its important that family members learn about schizophrenia and how to support their loved one. Making sure the loved one is taking medication and noting signs of recurrence are also vital.
- Social support. Similar to psychosis, people with schizophrenia can benefit from social support services. These services can help with returning to school or work, improving social skills, and coping with stress and everyday challenges.
Schizophrenia is also associated with several comorbid conditions. These are conditions that can occur along with schizophrenia and can include:
- depression
Read Also: Dementia Vs Senility
How Can You Tell The Difference Between Depression And Alzheimer’s
People with Alzheimer’s may experience depression differently from that of people without Alzheimer’s. For example, individuals diagnosed with Alzheimer’s disease: May have symptoms of depression that are less severe. May experience episodes of depression that don’t last as long or come back as frequently.
Where To Go What To Eat
And, unlike Alzheimers disease, there are medications to treat Schizophrenia and significantly reduce the symptoms.
Though Alzheimers disease and schizophrenia are radically different disorders, new research suggests that each disorder affects the same areas of the brain.
When investigators at Oxford University examined subjects and performed MRI scans, they found that the regions of the brain that developed last were also the first to deteriorate with advanced age. These areas seem to be more vulnerable than the rest of the brain to both schizophrenia and Alzheimers, even though the two diseases have different origins and appear at almost opposite and very different times of life. Schizophrenia was once labeled premature dementia, and some researchers considered that the two conditions were linked. The Oxford study now confirms that the same regions of the brain are affected in Alzheimers disease and schizophrenia.
Questions about Alzheimers disease or a related dementia disorder? Contact Dana Territo, the Memory Whisperer, Director of Services at Alzheimers Services of the Capital Area, 334-7494, , or visit the organization at 3772 North Blvd., Baton Rouge.
Don’t Miss: What’s The Difference Between Dementia And Alzheimer’s And Senility