How Mri Is Used To Detect Alzheimer’s Disease
One way to test for Alzheimer’s disease is to assess the brain’s functioning. There are several frequently used cognitive screenings that can be used to evaluate someone’s memory, executive functioning, communication skills, and general cognitive functioning. These tests are commonly done in your healthcare provider’s office widely used is Mini Mental Status Exam or Montreal Cognitive Assessment . These can be very helpful in identifying if a problem exists, or if there’s just a normal lapse in memory.
These can be very helpful in identifying if a problem exists, or if there’s just a normal lapse in memory due to aging. There are, however, several different types of dementia, as well as other conditions that can cause symptoms of dementia but are reversible. There are ways you can tell.
Alternatives To A Head Ct Scan
Head CT scans may be the most effective way to diagnose Alzheimers disease. But if you prefer another method, magnetic resonance imaging of the head shows your doctor if you have mild cognitive impairment or brain shrinkage. Cognitive tests are available online to download, print and bring to a doctors office for a score. One option is the SAGE test from the Ohio State University Wexner Medical Center.
To get the most accurate diagnosis, your doctor may recommend combining tests and scans. For example, you can have a head MRI along with an assessment by your primary care doctor.
Facing the idea that you or a loved one might have Alzheimers disease is difficult. Its important though to not delay important imaging scans. Learn more about how CT scans help you and how to prepare for an upcoming appointment.
Current Practice In Diagnosing Dementia
The remainder of this information will provide an overview of the diagnosis process and a guide to what happens after diagnosis.
It is important to remember that there is no definitive test for diagnosing Alzheimers disease or any of the other common causes of dementia. Findings from a variety of sources and tests must be pooled before a diagnosis can be made, and the process can be complex and time consuming. Even then, uncertainty may still remain, and the diagnosis is often conveyed as possible or probable. Despite this uncertainty, a diagnosis is accurate around 90% of the time.
People with significant memory loss without other symptoms of dementia, such as behaviour or personality changes, may be classified as having a Mild Cognitive Impairment . MCI is a relatively new concept and more research is needed to understand the relation between MCI and later development of dementia. However, MCI does not necessarily lead to dementia and regular monitoring of memory and thinking skills is recommended in individuals with this diagnosis.
You May Like: Where To Buy Jelly Drops For Dementia Patients
Early Signs Of Alzheimers Disease
The early signs of Alzheimers disease are of the utmost importance. If you or a loved one has early Alzheimers symptoms, and you get an early diagnosis, this increases your chance of prevention and maintaining a high quality of life.
These are some of the early signs your doctor may look for during a diagnosis:
- Memory loss, starting with short-term memory
- Social withdrawal
- Inability to find the right words
- Confusion about time
- Changes in mood and personality
- Trouble planning or problem-solving
- Lack of sense of direction
- Repetition in behavior
Changes in the brain that lead to a loss in cognitive function can begin in your 40s, long before youll have noticeable symptoms. The sooner you notice early warning signs of Alzheimers, the sooner you can start preventing Alzheimers disease.
About 5% of Alzheimers cases occur before the age of 65. This is called early-onset Alzheimers, or younger Alzheimers disease.
How is early-onset Alzheimers diagnosed? Early-onset Alzheimers is usually diagnosed by a doctor who specializes in Alzheimers disease since most doctors wont look for warning signs of Alzheimers in individuals younger than 65. This specialist doctor will likely administer a comprehensive medical exam, symptom checklist, cognitive tests, and brain imaging for diagnosis.
The Limitations Of Amyloid Pet In Ad
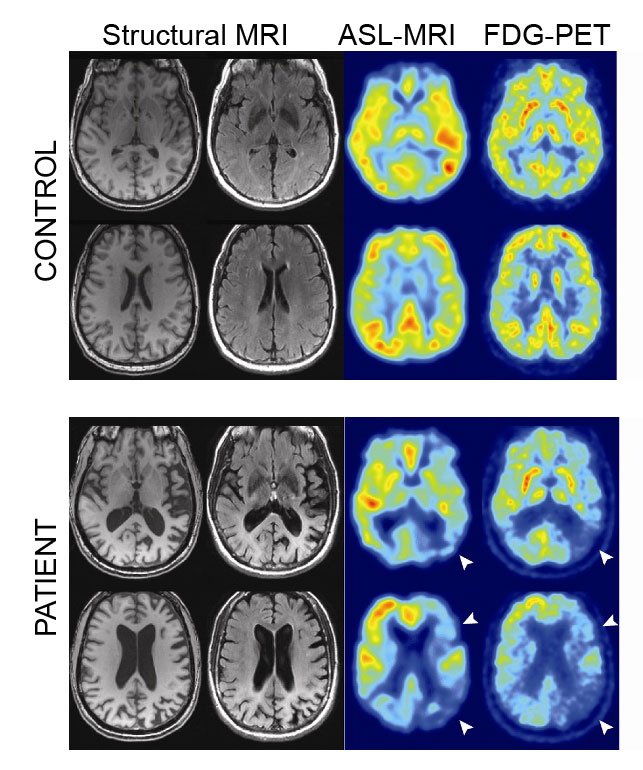
Major deterrents to the widespread use of amyloid PET remain cost and availability. Availability has been improved by the development of F-18-labeled agents that can be distributed to PET scanners not associated with a cyclotron. Cost remains an issue, especially where CSF measurement of A42 can provide very similar information when the question is simply the presence or absence of brain A deposition. Being an early event in the pathogenesis of AD, amyloid PET is not a good surrogate marker of progression during the clinical stage of the disease . This role is filled much better by structural MRI and FDG PET . Similarly, amyloid imaging gives much more of a binary diagnostic readout than techniques such as MRI and FDG PET. That is, amyloid imaging has a certain specificity for the pathology of AD, but when that pathology is absent, a negative amyloid PET scan will be identical regardless of the non-AD etiology of the dementia. In contrast, MRI and FDG PET may give an indication of a frontotemporal or vascular pathology when an amyloid PET scan would be ambiguously negative in both cases. The threshold of sensitivity of amyloid PET has yet to be precisely determined, but it is clear that some level of amyloid deposition is histologically detectable prior to the in vivo signal becoming positive .
Read Also: What Causes Senile Dementia
Limitations Of Fmri In Ad
There are multiple challenges in performing longitudinal fMRI studies in patients with neurodegenerative dementias. It is likely that fMRI will remain quite problematic in examining patients with more severe cognitive impairment, as these techniques are very sensitive to head motion. If the patients are not able to adequately perform the cognitive task, one of the major advantages of task fMRI activation studies is lost. Resting state fMRI may be more feasible in more severely impaired patients.
It is critical to complete further validation experiments. BOLD fMRI response is known to be variable across subjects, and very few studies examining the reproducibility of fMRI activation in older and cognitively impaired subjects have been published to date . Longitudinal functional imaging studies are needed to track the evolution of alterations in the fMRI activation pattern over the course of the cognitive continuum from preclinical to prodromal to clinical AD. It is also important to evaluate the contribution of structural atrophy to changes observed with functional imaging techniques in neurodegenerative diseases. Finally, longitudinal multimodality studies, including structural MRI, fMRI, and FDG-PET and PET amyloid imaging techniques, are needed to understand the relationship between these markers, and the relative value of these techniques in tracking change along the clinical continuum of AD .
Can Alzheimers Be Seen On An Mri
Alzheimers disease is an incurable, progressive form of dementia that results in widespread damage to nerve cell connections within the brain and loss of brain mass over time. The symptoms of Alzheimers are memory loss, difficulty with daily tasks, losing things, changes in mood or personality, social withdrawal, poor judgment like impulsive or out-of-character money decisions, poor hygiene, and psychological or behavioral problems.
Doctors typically begin assessing Alzheimers with a thorough physical examination and screening tests that measure general cognitive functioning. This usually takes place in the doctors office. These tests may help determine if a problem exists or if the changes are experienced from the aging process. There are multiple causes of dementia, and while Alzheimers is responsible for most dementia cases, your doctor will work to rule out other potential explanations.
MRI or magnetic resonance imaging is used to help diagnose in some cases. MRI can rule out other causes of Alzheimers symptoms like stroke or brain tumor. MRI is also useful in measuring the volume of the brain. The hippocampus, a portion of the brain that helps us access memories, is affected by Alzheimers. Memory changes are one of the more common and earliest symptoms, so an MRI that examines this area of the brain can help aid in diagnosis. Because Alzheimers can cause shrinkage in the brain’s hippocampus, changes in volume observed in MRI can indicate Alzheimers.
You May Like: Does Medicare Cover Respite Care For Dementia
What Is The Future Of Biomarkers
Advances in biomarkers during the past decade have led to exciting new findings. Researchers can now see Alzheimer’s-related changes in the brain while people are alive, track the disease’s onset and progression, and test the effectiveness of promising drugs and other potential treatments.
Researchers are continuing to study and develop biomarkers to improve dementia detection, diagnosis, and treatment. These may one day be used more widely in doctors’ offices and other clinical settings. Learn more about biomarker advancements and biomarkers for dementia detection and research.
Do I Need A Brain Scan To Diagnose Alzheimers Disease
Question: Do I need a brain scan to diagnose Alzheimers disease?
Answer: Yes, No, Maybe..
Alzheimers disease and dementia are diagnosed by physicians by taking a careful medical history from the patient and a family member, doing a number of brief memory and cognitive tests, and performing a physical exam. Whether your doctor will also order a brain scan might depend on where you live!
In the U.S., it is recommended that everyone being investigated for dementia have a CT scan or MRI . In Canada, we suggest that brain scans are only essential in cases where the history and physical exam suggest that the dementia is caused by something other than Alzheimers disease . Even in Canada, however, if you are seen by a dementia specialist, you will likely have a brain scan ordered, because of the extra information the scans can provide. Besides helping with the diagnosis for rarer forms of dementia, they can also help determine the presence of cerebrovascular disease. Cerebrovascular disease can be a primary cause of dementia, but can also frequently be mixed with other pathology like Alzheimers disease.
Don’t Miss: Does Ben Carson Have Dementia
Promoting Early Diagnosis Of Dementia
The early symptoms of dementia can include memory problems, difficulties in word finding and thinking processes, changes in personality or behaviour, a lack of initiative or changes in day to day function at home, at work or in taking care of oneself. This information does not include details about all of these warning signs, so it is recommended that you seek other sources of information. If you notice signs in yourself or in a family member or friend, it is important to seek medical help to determine the cause and significance of these symptoms.
Obtaining a diagnosis of dementia can be a difficult, lengthy and intensive process. While circumstances differ from person to person, Dementia Australia believes that everyone has the right to:
- A thorough and prompt assessment by medical professionals,
- Sensitive communication of a diagnosis with appropriate explanation of symptoms and prognosis,
- Sufficient information to make choices about the future,
- Maximal involvement in the decision making process,
- Ongoing maintenance and management, and
- Access to support and services.
Basics Of Fdg Pet As Applied To Ad
Brain FDG PET primarily indicates synaptic activity. Because the brain relies almost exclusively on glucose as its source of energy, the glucose analog FDG is a suitable indicator of brain metabolism and, when labeled with Fluorine-18 is conveniently detected with PET. The brains energy budget is overwhelmingly devoted to the maintenance of intrinsic, resting activity, which in cortex is largely maintained by glutamaturgic synaptic signaling . FDG uptake strongly correlates at autopsy with levels of the synaptic vesicle protein synaptophysin . Hence, FDG PET is widely accepted to be a valid biomarker of overall brain metabolism to which ionic gradient maintenance for synaptic activity is the principal contributor . In this context, a single, specific AD-related alteration in FDG metabolism has not been identified and therefore the FDG-PET abnormalities described below are assumed to be the net result of some combination of processes putatively involved in the pathogenesis of AD including, but not limited to, expression of specific genes, mitochondrial dysfunction, oxidative stress, deranged plasticity, excitotoxicity, glial activation and inflammation, synapse loss, and cell death.
Read Also: Alzheimer’s And Dementia Ribbon
Utility Of Fdg Pet In The Study Of Ad
The Pattern of FDG Hypometabolism Is an Endophenotype of AD
A substantial body of work over many years has identified a FDG-PET endophenotype of AD that is, a characteristic or signature ensemble of limbic and association regions that are typically hypometabolic in clinically established AD patients . The anatomy of the AD signature includes posterior midline cortices of the parietal and posterior cingulate gyri, the inferior parietal lobule, posterolateral portions of the temporal lobe, as well as the hippocampus and medial temporal cortices. Metabolic deficits in AD gradually worsen throughout the course of the disease. Bilateral asymmetry is common at early stages, more advanced disease usually involves prefrontal association areas, and in due course even primary cortices may be affected. Interestingly, the regions initially hypometabolic in AD are anatomically and functionally interconnected and form part of the large-scale distributed brain network known as the default mode network . We now know in addition that these regions are highly vulnerable to amyloid- deposition .
FDG Hypometabolism Is Related to Other AD Biomarkers and to Genes
FDG PET Is a Valid AD Biomarker
How Biomarkers Help Diagnose Dementia
On this page:
Biomarkers are measurable indicators of whats happening in the body. These can be found in blood, other body fluids, organs, and tissues. Some can even be measured digitally. Biomarkers can help doctors and researchers track healthy processes, diagnose diseases and other health conditions, monitor responses to medication, and identify health risks in a person. For example, an increased level of cholesterol in the blood is a biomarker for heart attack risk.
Before the early 2000s, the only sure way to know whether a person had Alzheimers disease or another form of dementia was after death through autopsy. But thanks to advances in research, tests are now available to help doctors and researchers see biomarkers associated with dementia in a living person.
The different types of biomarkers for dementia detection and diagnosis are outlined below. When combined with other tests, these biomarkers can help doctors determine whether a person might have or be at risk of developing Alzheimers or a related dementia. However, no single test can alone diagnosis these conditions. Biomarkers are only part of a complete assessment. Read more about diagnosing dementia.
Recommended Reading: What Happens In The Later Stages Of Vascular Dementia
Utility Of Amyloid Pet In The Study Of Ad
The obvious strength of amyloid imaging is that it has allowed the determination of brain A content to be moved from the pathology laboratory into the clinic. Amyloid imaging can detect cerebral -amyloidosis and appears specific for this type of amyloid pathology, giving negative signals in pathologically confirmed cases of prion amyloid , pathologically confirmed pure -synucleinopathy , as well as in apparently pure cases of tauopathy in semantic dementia .
PiB PET Images of normal control, MCI, and AD subjects showing a range of amyloid- deposition. Most controls show no evidence of amyloid- deposition , but a substantial portion do . Most patients with MCI show moderate or severe amyloid- deposition , but as many as 40%50% show no evidence of amyloid- pathology . The vast majority of clinically diagnosed AD patients show heavy amyloid- deposition .
In the setting of MCI, combined data from nine amyloid PET studies show that 161 of 272 MCI patients were amyloid positive . Five of these studies included longitudinal clinical follow-up for 13 years on 155 MCI patients and showed that 57 of these 155 progressed to clinical AD and 53 of these 57 were amyloid positive at baseline only four of 54 amyloid-negative MCI patients progressed to clinical AD in these studies .
Early Warning Signs And Diagnosis
Alzheimers Disease can be caught in the early stageswhen the best treatments are availableby watching for telltale warning signs. If you recognize the warning signs in yourself or a loved one, make an appointment to see your physician right away. Brain imaging technology can diagnose Alzheimers early, improving the opportunities for symptom management.
Read Also: 7th Stage Of Dementia
Imaging In The Diagnosis And Prognosis Of Ad
The uncertainty inherent in a clinical diagnosis of AD has driven a search for diagnostic imaging markers. A definitive diagnosis still requires histopathological confirmation and the inaccessibility of the brain means imaging has a key role as a window on the brain. Historically, imagingfirst computed tomography and then MRIwas used only to exclude potentially surgically treatable causes of cognitive decline. Now its position in diagnosis also includes providing positive support for a clinical diagnosis of AD in symptomatic individuals by identifying characteristic patterns of structural and functional cerebral alterations. We can now also visualize the specific molecular pathology of the diseaseamyloid depositswith amyloid imaging. Alongside this increasing specificity for AD, imaging also contributes to differential diagnosis in practice by identifying alternative and/or contributory pathologies. Imaging is central to identifying vascular and non-AD degenerative pathologies and has helped in the recognition of the prevalence of mixed pathology in dementia.
Ct Scans: How They Help Detect Alzheimers Disease
Early diagnosis of Alzheimers disease allows you to treat it sooner and stay healthy and independent for longer. Head CT scans are one the most effective tools to detect the condition. Learn how a head CT scan can help you or your loved one with memory loss determine if an advanced condition like Alzheimers disease is the root of the symptoms.
Read Also: Dementia Color Ribbon
Rate Of Change Of Brain Atrophy
Changes in the rate of atrophy progression can be useful in diagnosing Alzheimer disease. Longitudinal changes in brain size are associated with longitudinal progression of cognitive loss, and enlargement of the third and lateral ventricles is greater in patients with Alzheimer disease than in control subjects.
CT scan indices of hippocampal atrophy are highly associated with Alzheimer disease, but the specificity is not well established. Use of a nonquantitative rating scale showed a sensitivity of 81% and a specificity of 67% in differentiating 21 patients with Alzheimer disease with moderate dementia from 21 age-matched control subjects. Hippocampal volumes in a sample of similar size permitted correct classification of 85% of control subjects.