How Is Alzheimers Disease Diagnosed And Evaluated
No single test can determine whether a person has Alzheimers disease. A diagnosis is made by determining the presence of certain symptoms and ruling out other causes of dementia. This involves a careful medical evaluation, including a thorough medical history, mental status testing, a physical and neurological exam, blood tests and brain imaging exams, including:
Also Check: Neil Diamond Alzheimers
Strategic Infarcts And Small Vessel Disease
Cognitive dysfunction in VaD can be the result of :
- Large vessel infarctions:
- Bilateral in the anterior cerebral artery territory.
- Parietotemporal- and temporo-occipital association areas of the dominant hemisphere
- oPosterior cerebral artery territory infarction of the paramedian thalamic region and inferior medial temporal lobe of the dominant hemisphere
- Multiple lacunar infactions in frontal white matter and basal ganglia
- WMLs
- Bilateral thalamic lesions
MTA in a patient with VaD
There is an increasing awareness for the importance of small vessel disease as a predictor of cognitive decline and dementia. Moreover, it seems to amplify the effects of pathologic changes of Alzheimer’s disease.On the left we see a patient who was diagnosed as having VaD.White matter disease is seen as severe WMH in the periventricular regions.In addition to these vascular changes, there is also MTA.Presumably this patient has both VaD and AD, a finding seen in many elderly patients. These findings should be described separately as it may have therapeutic consequences.
Bilateral medial strategic thalamus infarctions
The medial nuclei of the thalamus play an important role in memory and learning. A large unilateral infarction or bilateral infarctions in this region can cause dementia.You have to pay special attention to these areas to find these small infarctions.
FLAIR misses thalamus infarctionsCerebral Amyloid Angiopathy
Signs You May Need A Scan
If you have a family history of Alzheimers or dementia, you may want to get tested proactively so that you can determine if you have this condition. In other situations, you may want to get tested if you have any of the following symptoms:
- Memory loss
- Issues with depth perception
- Delusions or hallucinations
Many people believe that some memory loss is inevitable with aging, but this is simply not true. If you or your loved one is experiencing chronic or progressive memory loss or memory loss combined with the above symptoms, it may be a sign of Alzheimers.
Don’t Miss: What Color Ribbon Is For Alzheimer Disease
Diagnosing Dementia With An Alzheimer Mri
An MRI scan refers to the process of using magnetic resonance imaging, or MRI, technology to diagnose or assess the progress of any number of conditions, including Alzheimers disease. When looking at images from an Alzheimer MRI, your doctor assesses brain volume changes in key locations. Research in NeuroImage: Clinical shows a diagnostic accuracy of up to 87% when confirming the early presence of Alzheimers disease up to seven years before the onset of symptoms.
If you believe that you or a loved one may be in the early stages of Alzheimers disease, you should contact your primary care provider as soon as possible. No single test can determine with 100% certainty whether you or a loved one has Alzheimers disease, but through a combination of physical, mental and neurological exams, careful medical evaluation, blood tests, and an MRI, you can find an answer.
Measure Volume In The Brain
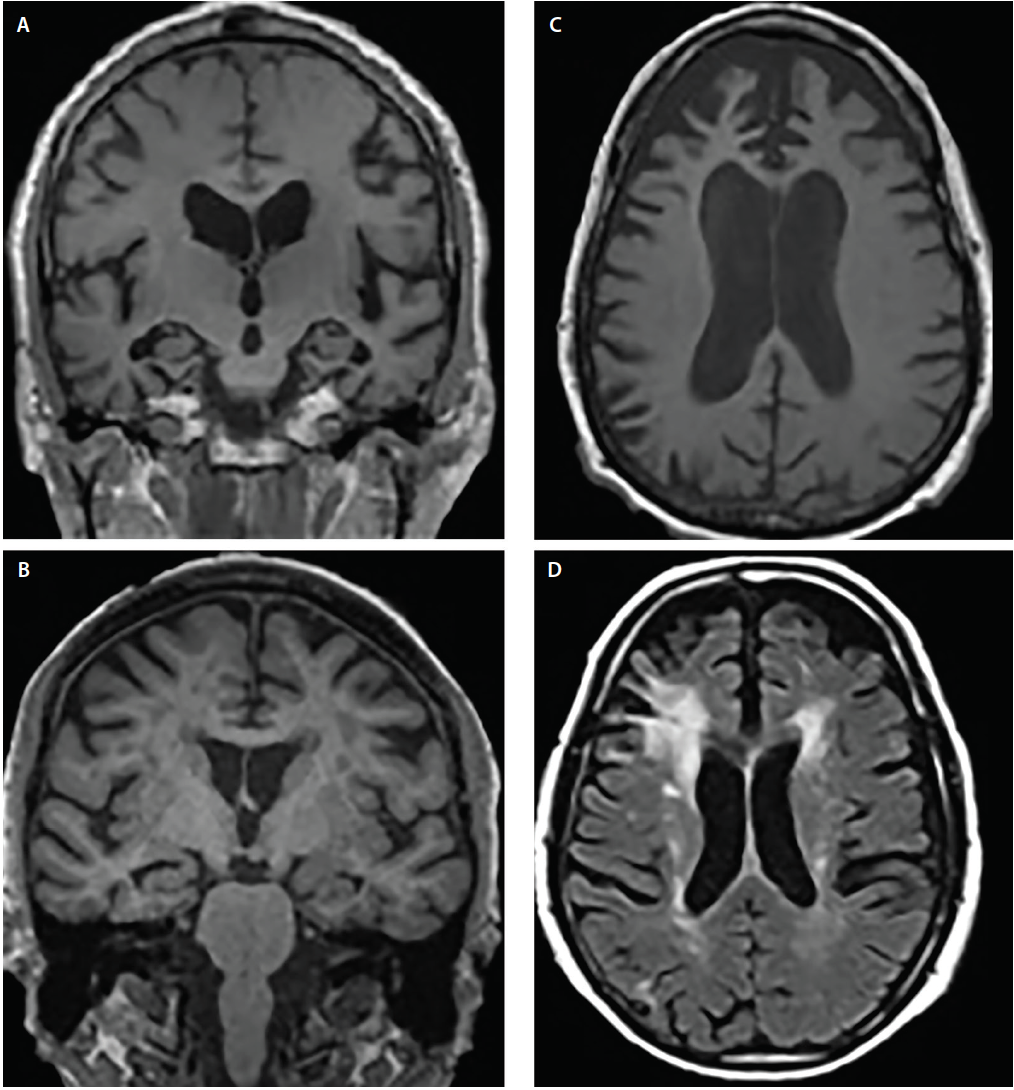
An MRI can provide the ability to view the brain with 3D imaging. It can measure the size and amount of cells in the hippocampus, an area of the brain that typically shows atrophy during the course of Alzheimer’s disease. The hippocampus is responsible for accessing memory which is often one of the first functions to noticeably decline in Alzheimer’s.
An MRI of someone with Alzheimer’s disease may also show parietal atrophy. The parietal lobe of the brain is located in the upper back portion of the brain and is responsible for several different functions including visual perception, ordering and calculation, and the sense of our body’s location.
Don’t Miss: What Stage Of Alzheimer’s Is Aphasia
Training To Spot Dementia
To improve dementia diagnosis rates and ensure referrals are appropriate in the UK, the RCGP is currently teaching GP trainees to better spot the signs of dementia.GPs have had more and more thrust on them over the years they dont have the specialist knowledge of dementia, so better support is needed, says Dr Hayo.New models of care are also introducing more help for patients and healthcare professionals.NHS High Weald Lewes Havens Clinical Commissioning Group and Buxted Medical Centre in East Sussex have joined up with the local council and several charities to deliver more joined-up care for dementia patients.Their golden ticket service gives patients a single point of contact for their care. They meet with a dementia guide within two days of a diagnosis, and can access personalised advanced care planning. Early evaluations show that it is already reducing GP visits and emergency admissions to hospital.Meanwhile, a scheme commissioned by NHS South Norfolk CCG links specialist dementia nurses with GP practices to give dementia patients direct support.7 A similar scheme in Norfolk saved £440,000 over 10 months, reducing contact time with GPs by 60% and with nurses by 16%.More help for GPs to diagnose and refer patients appropriately better access to diagnostic scans clear pathways for patients to access support. Together, these should help to reduce diagnosis delays and improve patient care.Then, perhaps the wait for a diagnosis might not be so long.
Utility Of Structural Mri In The Study Of Ad
Atrophy in AD
Progressive cerebral atrophy is a characteristic feature of neurodegeneration that can be visualized in life with MRI . The major contributors to atrophy are thought to be dendritic and neuronal losses. Studies of regional MRI volumes have shown these are closely related to neuronal counts at autopsy . The pattern of loss differs between diseases reflecting selective neuronal vulnerability and/or regional disease expression. AD is characterized by an insidious onset and inexorable progression of atrophy that is first manifest in the medial temporal lobe . The entorhinal cortex is typically the earliest site of atrophy, closely followed by the hippocampus, amygdala, and parahippocampus . Other structures within the limbic lobe such as the posterior cingulate are also affected early on. These losses then spread to involve the temporal neocortex and then all neocortical association areas usually in a symmetrical fashion. This sequence of progression of atrophy on MRI most closely fits histopathological studies that have derived stages for the spread of neurofibrillary tangles . Nonetheless, a significant minority of AD cases have atypical presentations and in these cases the pattern of atrophy accords with clinical phenotype: with language presentations particularly having left temporal atrophy and visual variants having posterior cortical atrophy.
Measuring Progression in AD with Structural MRI
Availability and Utility of Structural MRI
Also Check: What Causes Low Blood Pressure In Dementia Patients
What Is Vascular Dementia
BMJ Best Practice defines vascular dementia as:Vascular dementia is a chronic progressive disease of the brain bringing about cognitive impairment. The executive functions of the brain such as planning are more prominently affected than memory. Motor and mood changes are often seen early.The underlying damage occurs to both grey matter and white matter from predominantly vascular causes: that is, infarction, ischaemia, haemorrhage, and small-vessel changes.Alzheimer’s disease can also be a comorbidity, and a mixed dementia diagnosis is becoming more common.
Dr Clare Taylor, a GP in Birmingham and Academic Clinical Lecturer for the National Institute for Health Research, agrees: Dementia can be hard to spot. People often feel its just a little bit of forgetfulness or a normal part of getting older. Its often the family that notice a change.Dr Hayo says that some patients may not realise there is treatment and support available. They think theres no cure, no treatment no hope, she says. Theres a bit of fear, denial, and in some cases a lack of insight.Yet its vital that patients are aware of the symptoms of vascular dementia, Dr Taylor believes: Dementia isnt a normal part of ageing and its important to raise awareness of the signs.
Current Practice In Diagnosing Dementia
The remainder of this information will provide an overview of the diagnosis process and a guide to what happens after diagnosis.
It is important to remember that there is no definitive test for diagnosing Alzheimers disease or any of the other common causes of dementia. Findings from a variety of sources and tests must be pooled before a diagnosis can be made, and the process can be complex and time consuming. Even then, uncertainty may still remain, and the diagnosis is often conveyed as possible or probable. Despite this uncertainty, a diagnosis is accurate around 90% of the time.
People with significant memory loss without other symptoms of dementia, such as behaviour or personality changes, may be classified as having a Mild Cognitive Impairment . MCI is a relatively new concept and more research is needed to understand the relation between MCI and later development of dementia. However, MCI does not necessarily lead to dementia and regular monitoring of memory and thinking skills is recommended in individuals with this diagnosis.
Recommended Reading: Dementia Awareness Ribbon
Neuroimaging: Visualising The Brain
Neuroimaging describes a range of tools which are used to visualise the living brain, including computerised tomography scans, magnetic resonance imaging , single photon emission computerised tomography and positron emission tomography .
Researchers are working on new ways of using neuroimaging tools to diagnose Alzheimer’s disease and other types of dementia.
Positron Emission Tomography
In 2004, researchers successfully viewed beta-amyloid plaque deposits in the living human brain. The study used Pittsburgh Compound-B , a substance which binds to amyloid and can be visualised with PET scanning. The results demonstrated that people with Alzheimer’s disease displayed more amyloid deposits in certain brain areas compared to people without the condition. More recent research has shown that PiB-PET can also detect the early brain changes of Alzheimer’s disease before symptoms become apparent.
While PiB has proved quite effective, its widespread clinical use may be limited by the need for specialised equipment to produce PiB at the site of the PET scanner. Researchers are currently developing and testing other compounds that bind to beta-amyloid and may overcome the limitations of PiB.
Magnetic Resonance Imaging
MRI is able to image the structure of the brain, which changes in dementia, to a very high resolution.
The Seven Stages Of Dementia
One of the most difficult things to hear about dementia is that, in most cases, dementia is irreversible and incurable. However, with an early diagnosis and proper care, the progression of some forms of dementia can be managed and slowed down. The cognitive decline that accompanies dementia conditions does not happen all at once – the progression of dementia can be divided into seven distinct, identifiable stages.
Learning about the stages of dementia can help with identifying signs and symptoms early on, as well as assisting sufferers and caretakers in knowing what to expect in further stages. The earlier dementia is diagnosed, the sooner treatment can start.
Recommended Reading: Familial Dementia
How A Head Ct Scan Can Detect Alzheimers Disease
A head CT scan looks at the structure of your brain. This scan can detect issues such as tumors, hemorrhages, and strokes, which can all mimic the symptoms of Alzheimers, but in addition to helping you rule out those conditions, a CT scan can also detect the loss of brain mass thats associated with Alzheimers disease.
Does An Mri Or Ct Scan Show Dementia
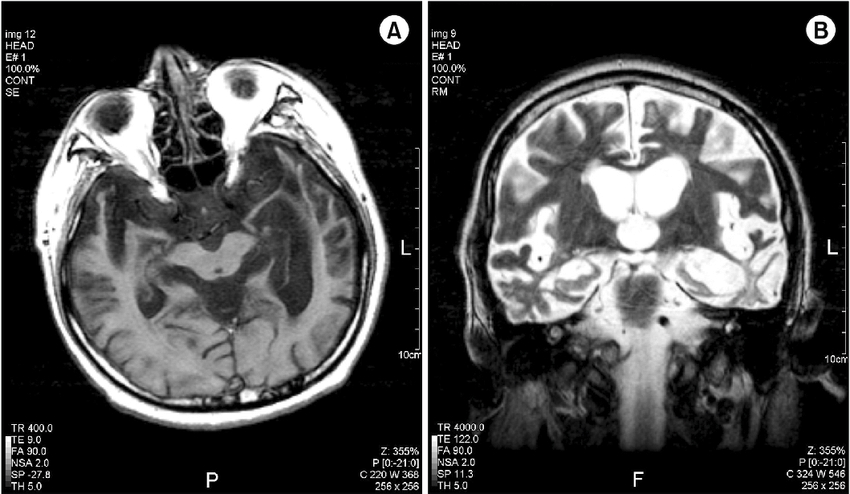
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Don’t Miss: Color For Dementia Awareness
Promoting Early Diagnosis Of Dementia
The early symptoms of dementia can include memory problems, difficulties in word finding and thinking processes, changes in personality or behaviour, a lack of initiative or changes in day to day function at home, at work or in taking care of oneself. This information does not include details about all of these warning signs, so it is recommended that you seek other sources of information. If you notice signs in yourself or in a family member or friend, it is important to seek medical help to determine the cause and significance of these symptoms.
Obtaining a diagnosis of dementia can be a difficult, lengthy and intensive process. While circumstances differ from person to person, Dementia Australia believes that everyone has the right to:
- A thorough and prompt assessment by medical professionals,
- Sensitive communication of a diagnosis with appropriate explanation of symptoms and prognosis,
- Sufficient information to make choices about the future,
- Maximal involvement in the decision making process,
- Ongoing maintenance and management, and
- Access to support and services.
Stage : Moderately Severe Dementia
When the patient begins to forget the names of their children, spouse, or primary caregivers, they are most likely entering stage 6 of dementia and will need full time care. In the sixth stage, patients are generally unaware of their surroundings, cannot recall recent events, and have skewed memories of their personal past. Caregivers and loved ones should watch for:
- Delusional behavior
Also Check: Can Aricept Make Memory Worse
White Matter And Basal Ganglia Hyperintensities
The results for WMHs and basal ganglia lesions are presented in table . Photographs of MRI demonstrating white matter changes in subjects from each group are shown in the figure.
White matter and basal ganglia hyperintensities
Total deep hyperintensity scores were significantly higher in all dementia groups compared with controls . Comparing the dementia groups, patients with vascular dementia had higher total lesion scores than those with Alzheimers disease and dementia with Lewy bodies . Overall, basal ganglia lesions were specifically associated with vascular dementia compared with all other groups .
A link between regional changes in white matter and specific non-cognitive symptoms in dementia patients was seen. The presence of frontal WMHs was associated with higher depression scores . The presence of delusions and visual hallucinations was associated with the absence of occipital WMHs. No patient with delusions had WMHs, and only one patient with visual hallucinations had occipital WMHs. Auditory hallucinations showed a similar trend . White matter hyperintensity scores did not correlate with age or cognitive impairment.
Other Imaging Options That Can Diagnose Dementia
Several other brain imaging procedures exist. Each can help detect dementia in different ways.
EEGs
EEGs are sometimes used on people who have suspected seizures, which accompany some types of dementia.
The procedure involves placing several electrodes at different points on the scalp to check for abnormalities in the brain through the recorded patterns of electrical activity.
The electrical activity shows instances of cognitive dysfunction that plague parts of the brain or the entire organ.
People with MODERATE to SEVERE cases of dementia present abnormal EEGs.
The procedure can also identify seizures, which 10% of people with Alzheimers are reported to experience.
Functional Brain Imaging
Functional brain imaging procedures are not often used as diagnostic tools. But they help researchers in the process of studying people with dementia.
They include functional single-photon emission computed tomography , MRI , magnetoencephalography , and positron emission tomography scans.
Nowadays, they have a hand in the EARLY DETECTION of dementia.
fMRI measures metabolic changes happening within the brain using strong magnetic fields.
SPECT scans reveal blood distribution within the brain. This aspect is responsible for discovering increased brain activity.
PET scans pick up on blood flow, glucose, and oxygen metabolism, and if amyloid proteins are present within the brain.
MEG scans record the electromagnetic fields that the brain produces through neuronal activities.
Also Check: What Causes Senile Dementia
Why Early Detection Can Be Difficult
Alzheimers disease usually is not diagnosed in the early stages, even in people who visit their primary care doctors with memory complaints.
- People and their families generally underreport the symptoms.
- They may confuse them with normal signs of aging.
- The symptoms may emerge so gradually that the person affected doesnt recognize them.
- The person may be aware of some symptoms but go to great lengths to conceal them.
Recognizing symptoms early is crucial because medication to control symptoms is most effective in the early stages of the disease and early diagnosis allows the individual and his or her family members to plan for the future. If you or a loved one is experiencing any of the following symptoms, contact a physician.
What Is Magnetic Resonance Imaging
A magnetic resonance imaging scan is usually called an MRI. An MRI does not use radiation and is a noninvasive medical test or examination. The MRI machine uses a large magnet and a computer to take pictures of the inside of your body. Each picture or “slice” shows only a few layers of body tissue at a time. The pictures can then be examined on a computer monitor.
Pictures taken this way may help caregivers find and see problems in your body more easily. The scan usually takes between 15 to 90 minutes. Including the scan, the total examination time usually takes between 1.5 to 3 hours.
A substance called gadolinium is injected into a vein to help the physicians see the image more clearly. The gadolinium collects around cancer cells so they show up brighter in the picture. Sometimes a procedure called magnetic resonance spectroscopy is done during the MRI scan. An MRS is used to diagnose tumors based on their chemical make-up.
How does MRI work?
The MRI machine is a large, cylindrical machine that creates a strong magnetic field around the patient. This magnetic field, along with a radiofrequency, alters the hydrogen atoms’ natural alignment in the body.
A magnetic field is created and pulses of radio waves are sent from a scanner. The radio waves knock the nuclei of the atoms in the body out of their normal position as the nuclei realign back into proper position, they send out radio signals.
Other related procedures that are used to assess the heart may include:
Also Check: Neurotransmitter Alzheimers