Trensomnia And How Trenbolone Can Potentially Cause Alzheimer’s Disease
As Matthew outlined in the clip above, the area of the brain that beta amyloid plaque builds up in is the same area of the brain responsible for getting into the stage of deep sleep required for cleaning beta amyloid out of your brain.
What I found most interesting about this is the fact that in humans, one of the main side effects of Tren most commonly reported that is unique to that compound is something called Trensomnia.
Trensomnia is the insomnia and poor quality sleep that many get when using Trenbolone.
Trenbolone is notorious for ruining sleep quality, and that is just one of the attributes of Trenbolone that make it unique from other steroids.
I think that in itself makes it pretty clear what mechanism is likely occurring with Trenbolone use not just in rodents, but in humans as well.
Trenbolone use inhibits deep sleep severely, which in turn results in impaired beta amyloid clean up via the glymphatic system, consequently increasing the amount of beta amyloid plaque accumulation in the brain, which ultimately results in neurodegeneration.
The more beta amyloid that builds up, the worse the quality of sleep becomes, and the worse the quality of sleep becomes, the more beta amyloid plaque will accumulate.
This is the vicious circle Trenbolone can have on the brain, at least in theory.
Is Trenbolone going to cause Alzheimer’s disease?
I don’t know.
Imagine what Trenbolone is doing to the brains of men using it year round.
Aducanumab: Right Treatment Wrong Time
As with treatments for many other human diseases, it might be that treatments such as aducanumab might only be effective if they are given early enough, before the disease has caused irreversible changes. A better understanding of the environmental and genetic factors behind Alzheimers disease combined with ever more sensitive brain imaging techniques will help doctors identify warning signs even earlier, before even minor memory loss occurs.
While screening and diagnosing people before symptoms have set in for an as-yet incurable disease, raises many ethical dilemmas, it might present a fresh window of opportunity to retest beta-amyloid drugs, such as aducanumab. Ultimately, we need to focus our research on understanding the early stages of the disease so that we can prevent Alzheimers disease before dementia takes hold.
Modeling States Of A And Ad
Alzheimers disease is a human specific disorder. Even our most closely related primate relatives do not develop pathology, much less the clinical outcome that can be considered to be actual AD. Still, much of our understanding of how amyloid pathology develops has been driven by studies in a variety of animal models. Although there is no animal model that accurately reflects every facet of AD, there are many models of A deposition. In a very broad sense, these can be subdivided into models where amyloid pathology develops naturally with age, and genetically modified mice that express mutant forms of APP. Animals in which amyloid deposition occurs naturally is attractive in that the researcher is not burdened with the numerous caveats that accompany genetically modified mice, such as separating the contributions of over expression and introduced mutations to the model phenotype. However, animals in which amyloid deposition occurs as a consequence of normal aging have a substantial longer lifespan than rodents , and their use can be difficult to justify based purely on their associated cost.
Recommended Reading: Diet Coke And Dementia
Alzheimers Mystery Solved: How Amyloid Beta Forms In Brain Nerve Cells
Amyloid protein forms clumps among neurons . Amyloid in the brain is one of the proteins associated with Alzheimers disease.
In a major breakthrough, researchers at Massachusetts General Hospital have discovered how amyloid beta the neurotoxin believed to be at the root of Alzheimers disease forms in axons and related structures that connect neurons in the brain, where it causes the most damage. Their findings, published in Cell Reports, could serve as a guidepost for developing new therapies to prevent the onset of this devastating neurological disease.
The new investigation revealed that palAPP is stabilized and prepared for cleavage by beta secretase in special lipid rafts within the neuron known as mitochondria-associated endoplasmic reticulum membranes . We showed for the first time not only that the MAM is where palAPP is processed by beta secretase to make Abeta, but that this happens exclusively in axons and neuronal processes where Abeta does most of its damage, says Bhattacharyya, lead author of the Cell Reports paper. This role for MAMs was previously unknown, though earlier research indicated that they are increased in number and activity in the brains of people with Alzheimers disease.
Cascade Hypothesis Versus Dysfunction Hypothesis
The BAD hypothesis is able to explain findings that are left unexplained by the Cascade hypothesis. Table 2 summarizes key major items that follow the rules of the BAD hypothesis but not the Cascade hypothesis.
Table 2. BAD vs. cascade hypothesis: key differences.
The plausibility for a physiological role of a highly expressed and high-turnover pre-amyloidogenic protein like the A peptide is already given through analogy with other CNS proteins like synuclein and tau, which are known to have a structural isoform associated with a benign physiological function . According to the Cascade hypothesis, the A formation is regarded as a superfluous relic left by evolution. But A homeostasis in brains is an extremely well-regulated and energy-consuming process in normal human brains. Eliminating the generation of this central protein in AD therapy therefore seems to lack plausibility.
Don’t Miss: Is Senility The Same As Dementia
What Causes Alzheimers Disease
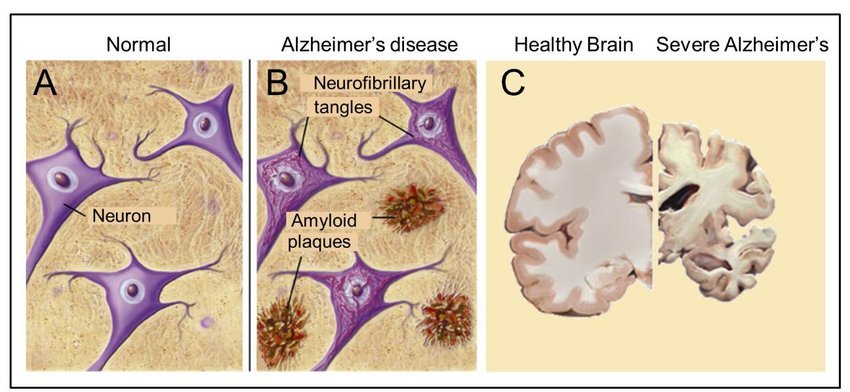
Scientists dont fully know what causes Alzheimers disease but recognize that certain changes in the brain cause the progressive loss of neurons and their connections. This is due in large part to the formation of lesions, called plaques, and twisted protein fibers, called tangles, in the brain. These changes may be due to aging-related changes in the brain combined with genetic, environmental, and lifestyle factors the contribute to the onset of the disease.
Cerebral Vascular Disease And Alzheimers Disease
There is increasing evidence that cerebral microvascular dysfunction plays an important role in the development of AD. Indeed, the interaction between cerebral vascular disease and AD is a topic of considerable current interest . However, it remains to be determined whether CVD in AD patients is secondary to the accumulation of A, or if it serves as an initiating factor in the development of this neurodegenerative disease. Hypertension, diabetes, and hyperlipidemia, along with aging, are the primary risk factors for AD. They all are the leading risk factors for cerebral vascular disease, endothelial dysfunction and stroke. Almost all elderly patients with severe CVD exhibit substantial A accumulation . Conversely, infarcts and small vessel disease, which are the hallmarks of vascular dementia , are found in > 50% of brains collected from AD patients . Based on this evidence, several investigators have suggested that AD may be a primary vascular disorder rather than secondary to A deposition induced neurodegeneration .
You May Like: Can Aricept Make Memory Worse
The Concept Of A Pools
A look through a microscope at a silver-stained section of AD brain tissue immediately shows the heterogeneity of the pathology. The use of silver impregnation techniques to evaluate brain pathology is an old approach, and the ones in use today differ little from those used by Alois Alzheimer when he initially described the disease. Over more than a century, a classification system has evolved to make sense of the progression of the disease, a tour-de-force effort of countless clinicians and pathologists. However, in the process a certain amount of information was averaged out and lost. In the past, simplification was necessary to improve understanding and provide a basis for testing hypotheses of the disease mechanism. Modern advances in technology, as well as new ways of studying the relationship of the pathology to brain biology and our improved understanding of the biochemical basis of the disease, require a re-evaluation of the lumping procedure used to discriminate among subpopulations of disease cases and different subtypes of plaques and tangles. If these misfolded protein structures are indeed polymorphic like prions, specific subpopulations will be strongly correlated with the clinical progression of the disease. Imaging agents based on analogs of histological dyes which are more discriminating among conformational states could then be used antemortem to evaluate the pathological components of the disease stage.
Post Mortem Or In Tissue Biopsies
Amyloid beta can be measured semiquantitatively with immunostaining, which also allows one to determine location. Amyloid beta may be primarily vascular, as in cerebral amyloid angiopathy, or in amyloid plaques in white matter.
One sensitive method is ELISA which is an immunosorbent assay which utilizes a pair of antibodies that recognize amyloid beta.
Atomic force microscopy, which can visualize nanoscale molecular surfaces, can be used to determine the aggregation state of amyloid beta in vitro.
Vibrational microspectroscopy is a label-free method that measures the vibration of molecules in tissue samples. Amyloid proteins like A can be detected with this technique because of their high content of -sheet structures. Recently, the formation of A fibrils was resolved in different plaque-types in Alzheimer’s disease, indicating that plaques transit different stages in their development.
Dual polarisation interferometry is an optical technique which can measure early stages of aggregation by measuring the molecular size and densities as the fibrils elongate. These aggregate processes can also be studied on lipid bilayer constructs.
Read Also: Can I Buy Jelly Drops For Dementia
Cerebral Autoregulation And Alzheimers Disease
Auto regulation of cerebral blood flow is a vital homeostatic mechanism that maintains adequate blood flow to the brain despite fluctuations in pressure . It protects the brain from increases in capillary pressure, which is associated with BBB leakage, cerebral edema and neurological damage . Recent studies have revealed that auto regulation of CBF is impaired in elderly hypertensive, diabetic and AD animal models. Impaired cerebral autoregulation increases transmission of pressure to small vessels which contributes to BBB disruption, inflammation, glial activation, capillary loss, microhemorrhage, localized ischemia and neurodegeneration, which accelerate the cognitive defecits in both VaD and AD patients .
App Cleavage And A Generation
Three main proteases-, – and -secretasesare involved in APP processing through the amyloidogenic pathway promoting A production through sequential cleavage by – and -secretases, and the non-amyloidogenic pathway in which APP is cleaved in the middle, either generating soluble APP directly by -secretase or generating shorter A species such as A1-15 and A1-16 by the sequential cleavage by -secretase and -secretase. The two pathways lead to different by-products with different intrinsic functional properties, putative physiological roles, and pathophysiological implications . Besides secretase activity, APP trafficking due to the secretory pathway is another essential factor in APP metabolism. APP is first matured in the endoplasmic reticulum and the Golgi apparatus, then translocated to the cell surface. Alternatively, APP can enter the lysosomal pathway and undergo proteolytic degradation .
Fig. 3: Amyloidogenic vs non-amyloidogenic pathway.
Recommended Reading: Does Ben Carson Have Dementia
A And The Immune System
In response to A-induced neurotoxicity in AD, both humoral and cellular immunity are activated. Aging is commonly accompanied by a progressive dysregulation of the immune response, mainly due to alterations of cellular immunity. In comparison to these changes in cellular immunity, many features of innate immunity are relatively well maintained with age .
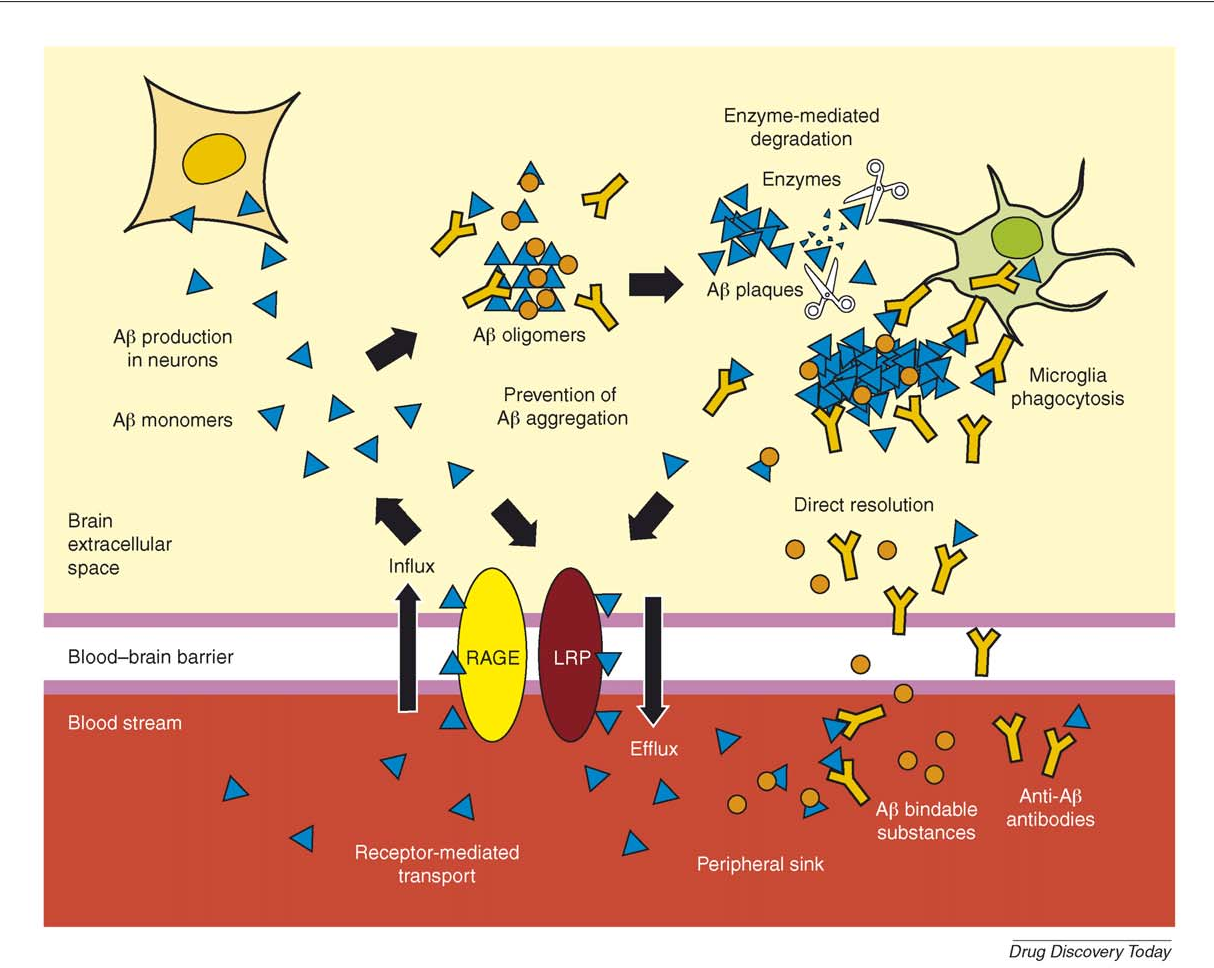
A number of publications have reported the presence of anti-A antibodies in the blood and CSF of patients with AD and healthy subjects . Also, some drugs have recently been designed based on fully human anti-A monoclonal antibodies for the clearance of A .
A deposition is responsible for microglia activation. A contributes to the enhancement of the inflammatory response by NF-B stimulation, a nuclear factor that is implicated in cytokine production and also regulates the ERK and MAPK pathways that lead to cytokine and chemokine production . Toll-like receptors are important for regulating microglial responses to A and fibrillar A triggers microglia inflammatory cytokine production via TLR4-TLR6 heterodimers, whose assembly is regulated by CD36. Modification of the inflammatory state of microglia/macrophages may have an axial role in AD-related pathology .
A Pathophysiology And The Neurochemical Systems In Ad: The Glutamatergic System
Glutamate excitotoxicity is considered one of the core molecular mechanisms of neurodegeneration in AD . The interaction between A aggregates and glutamatergic neurotransmission is a possible critical event for the A-induced disruption of excitatory synaptic transmission and plasticity associated with cognitive deficits . A species can promote the dysregulation of N-methyl-D-aspartate and, to a lesser extent ionotropic glutamate receptors in the brain .
Electrophysiological recordings on mouse hippocampal slices showed the ability of soluble A oligomers to enhance the activation of NR2B/2A subunits of NMDARs while inhibiting glutamate uptake and recycling at the synapse . Consequently, a partial block of NMDA receptors coupled with a shift of the activation of NMDAR-dependent signaling cascades can take place, thus inducing LTD and downstream synaptic loss. The hippocampal overstimulation of A oligomers is associated with decreased cell surface expression of NMDARs and alterations of dendritic spine density .
Recommended Reading: What Color Represents Alzheimer’s
Does Amyloidosis Cause Dementia
Amyloidosis can interfere with the function of organs throughout the body, resulting in symptoms such as swelling, fatigue, shortness of breath, and diarrhea. The condition does not, however, cause dementia characterized by impairment of brain functions. Nevertheless, there is a connection between amyloidosis and dementia.
Amyloidosis is caused by an abnormal buildup of particular proteins, called amyloids, in different organs. The buildup may lead to organ damage, and in severe cases, organ failure.
Dementia results from damage to brain cells and scientists have found that people with Alzheimers disease have amyloid deposits in the brain. Some doctors believe that these deposits are responsible for the brain damage that leads to dementia. However, research has not yet proven that to be the case.
In short, amyloidosis and dementia share a trait in that they are both linked to abnormal amyloid protein deposits. However, not all scientists are confident there is a direct causal relationship between them.
To better understand the relationship, lets take a closer look at amyloidosis, dementia, and other connections between the two.
Trenbolone Causes Beta Amyloid Plaque Accumulation
The male rats given Trenbolone injections had amyloid-beta-42 accumulate in their brains.
Alzheimer’s disease is believed to be caused by the accumulation of the beta amyloid peptide.
While there has been no human trial to assess if this occurs in humans, and there probably is never going to be, I think it is best to assume the worst when we see data like this.
As I already touched on, I do not think it is a coincidence that guys get very strange mental side effects from Tren that they don’t get with other compounds.
Beta amyloid plaque build up doesn’t just occur with Trenbolone use obviously, and our body does have internal mechanisms in place to clean the brain of it each day.
Healthy individuals clear beta amyloid out of the brain during deep sleep via glymphatic drainage.
Basically, beta amyloid builds up and then the brain cleans it up during deep sleep.
If sleep quality and/or duration is impaired, expectedly, drainage via the glymphatic system is impaired too, and beta amyloid plaque then starts to accumulate over time, which can eventually cause Alzheimer’s disease and a myriad of other neurodegenerative outcomes.
This is why so many neurodegenerative diseases have been linked to poor sleep quality.
If you don’t have enough brain cleaning occurring each night because of poor sleep, you will eventually pay the toll in some way with impaired cognitive function.
You May Like: What Color Is For Alzheimer’s
How Does Amyloid Plaques Cause Dementia
Do PlaquesCause Dementiaplaquescauses
. Also know, how do amyloid plaques cause Alzheimer’s?
Amyloid PlaquesIt is formed from the breakdown of a larger protein, called amyloid precursor protein. In the Alzheimer’s brain, abnormal levels of this naturally occurring protein clump together to form plaques that collect between neurons and disrupt cell function.
what causes amyloid plaques? Plaques form when protein pieces called beta-amyloid clump together. Beta-amyloid comes from a larger protein found in the fatty membrane surrounding nerve cells. Beta-amyloid is chemically “sticky” and gradually builds up into plaques.
Likewise, how are amyloid plaques related to dementia?
Amyloid plaques are clumps of beta-amyloids, which destroy connections between nerve cells. They are found in the brains of patients with Alzheimer’s disease, an incurable dementia that impacts thinking, memory, and behavior.
Where do amyloid plaques accumulate?
Unlike NFTs, amyloid plaques accumulate mainly in the isocortex.
A Biochemical Properties From Monomers Through Higher Aggregation States Including Plaques
After being generated as soluble monomers, A is found in several different intermediate aggregation states, including dimers and trimers, soluble oligomers, and protofibrils, until it forms fibrils that accumulate in plaques, typically viewed as an AD neuropathological hallmark . Understanding the biology and interlinked dynamics of these intermediate assemblies and their bio-activity, in either physiological and pathophysiological conditions, is essential from a diagnostic and therapeutic perspective.
Fig. 4: Amyloid- aggregation species and evidence of reversible states: the amyloid- cycle.
Aggregation species of A can exist as monomers, dimers, oligomers, protofibril, fibril and amyloid plaques. These species exist in steady state where one form can convert to another in a bidirectional manner. The species are characterized by aggregate size, conformation state and solubility, with fibril and amyloid plaque being insoluble. Adapted with permission from ref. .
Read Also: Smelling Farts Dementia
An Imbalance Between Production And Clearance
Research has shown that when amyloid beta is no longer properly cleared from the brain, it accumulates and may lead to neurodegeneration long before the first symptoms of AD become visible.1-6
This understanding of AD highlights the importance of early detection and diagnosis as a central component of future patient care.