Support For Families And Alzheimers Disease Caregivers
Caring for a person with Alzheimers can have significant physical, emotional, and financial costs. The demands of day-to-day care, changes in family roles, and decisions about placement in a care facility can be difficult. NIA supports efforts to evaluate programs, strategies, approaches, and other research to improve the quality of care and life for those living with dementia and their caregivers.
Becoming well-informed about the disease is one important long-term strategy. Programs that teach families about the various stages of Alzheimers and about ways to deal with difficult behaviors and other caregiving challenges can help.
Good coping skills, a strong support network, and respite care are other things that may help caregivers handle the stress of caring for a loved one with Alzheimers. For example, staying physically active provides physical and emotional benefits.
Some caregivers have found that joining a support group is a critical lifeline. These support groups enable caregivers to find respite, express concerns, share experiences, get tips, and receive emotional comfort. Many organizations sponsor in-person and online support groups, including groups for people with early-stage Alzheimers and their families.
Read about this topic in Spanish. Lea sobre este tema en español.
What Is The Cost Of Dementia Care
- The total cost of care for people with dementia in the UK is £34.7billion.
- This is set to rise sharply over the next two decades, to £94.1billion in 2040.
- These costs are made up of healthcare costs , social care costs , and costs of unpaid care .
- The largest proportion of this cost, 45%, is social care, which totals £15.7billion.
- Social care costs are set to nearly triple over the next two decades, to £45.4billion by 2040.
Treatment Of Alzheimer’s Dementia
2.5.1 Pharmacologic treatment
None of the pharmacologic treatments available today for Alzheimer’s dementia slow or stop the damage and destruction of neurons that cause Alzheimer’s symptoms and make the disease fatal. The U.S. Food and Drug Administration has approved five drugs for the treatment of Alzheimer’s â rivastigmine, galantamine, donepezil, memantine, and memantine combined with donepezil. With the exception of memantine, these drugs temporarily improve cognitive symptoms by increasing the amount of chemicals called neurotransmitters in the brain. Memantine blocks certain receptors in the brain from excess stimulation that can damage nerve cells. The effectiveness of these drugs varies from person to person and is limited in duration.
Many factors contribute to the difficulty of developing effective treatments for Alzheimer’s. These factors include the slow pace of recruiting sufficient numbers of participants and sufficiently diverse participants to clinical studies, gaps in knowledge about the precise molecular changes and biological processes in the brain that cause Alzheimer’s disease, and the relatively long time needed to observe whether an investigational treatment affects disease progression.
2.5.2 Non-pharmacologic therapy
Read Also: Does Diet Coke Cause Dementia
Projected Growth Of Dementia
If current trends continue and no action is taken, the number of people with dementia in the UK is forecast to increase to 1,000,000 by 2025 and 1,590,000 by 2040.
Many people talk about a dementia time bomb that the state cannot cope with. This is misleading. A steady, rather than dramatic, growth is expected over the next 25 years.
Dont Miss: Difference Between Senility And Dementia
Greater Risks Of Alzheimers And Dementia For Blacks And Latinos
-
18.6% of Blacks and 14% of Hispanics age 65 and older have Alzheimers compared with 10% of White older adults .
- Other prevalence studies also indicate that older Blacks are about twiceas likely to have Alzheimers or other dementias as older Whites.
Also Check: How Fast Can Alzheimer’s Progress
What Are The Costs Of Dementia Care In The Uk
There are currently around 900,000 people living with dementia in the UK. Read projected figures until the year 2040, and find out what rising numbers will mean for the cost of dementia care.
A new report commissioned by Alzheimers Society from the Care Policy and Evaluation Centre at the London School of Economics and Political Science sets out new estimates for the number of people with dementia and the cost of dementia care in the UK, in 2019, with projections to 2040.
It shows the scale and impact of dementia, and the urgent need for action to be taken to meet current and future care needs and the associated costs.
Read the key findings of the report below, or .
Why Are Dementias Including Alzheimers Disease Important
In 2014, Alzheimers disease was the 6th leading cause of death among adults aged 18 years and older based on death certificate data.1 Estimates vary, but analysis of data from the Chicago Health and Aging Project and 2010 U.S. Census data suggests that the prevalence of dementia among adults aged 65 years and older in the U.S. in 2016 is 11%, or 5.2 million people.2,3 The estimated total cost for health care, long-term care, and hospice for persons with Alzheimers disease and other dementias is estimated to be $236 billion for 2016.2
Dementia affects an individuals health, quality of life, and ability to live independently. It can also diminish a persons ability to effectively:
- Manage medications and medical conditions
- Make financial decisions
There are important steps to take to improve the care and support for people with dementia and their caregivers. These include:
- Increasing the availability of existing effective diagnostic tools
- Reducing the severity of cognitive and behavioral symptoms through medical management
- Supporting family caregivers with social, behavioral, and legal resources
- Encouraging healthy behaviors to reduce the risk of co-occurring conditions
Don’t Miss: Dementia Color Ribbon
Diagnosis Of Dementia Due To Alzheimer’s Disease
- Obtaining a medical and family history from the individual, including psychiatric history and history of cognitive and behavioral changes.
- Asking a family member to provide input about changes in thinking skills and behavior.
- Conducting problem-solving, memory and other cognitive tests, as well as physical and neurologic examinations.
- Having the individual undergo blood tests and brain imaging to rule out other potential causes of dementia symptoms, such as a tumor or certain vitamin deficiencies.
- In some circumstances, using PET imaging of the brain to find out if the individual has high levels of beta-amyloid, a hallmark of Alzheimer’s normal levels would suggest Alzheimer’s is not the cause of dementia.
- In some circumstances, using lumbar puncture to determine the levels of beta-amyloid and certain types of tau in CSF normal levels would suggest Alzheimer’s is not the cause of dementia.
What To Do If A Loved One Is Suspicious Of Having Dementia
- Discuss with loved one. Talk about seeing a medical provider about the observed changes soon. Talk about the issue of driving and always carrying an ID.
- Medical assessment. Be with a provider that you are comfortable with. Ask about the Medicare Annual Wellness exam.
- Family Meeting. Start planning, and gather documents like the Health Care Directive, Durable Power of Attorney for Health Care, Estate Plan.
Read Also: Alzheimer’s Disease Color Ribbon
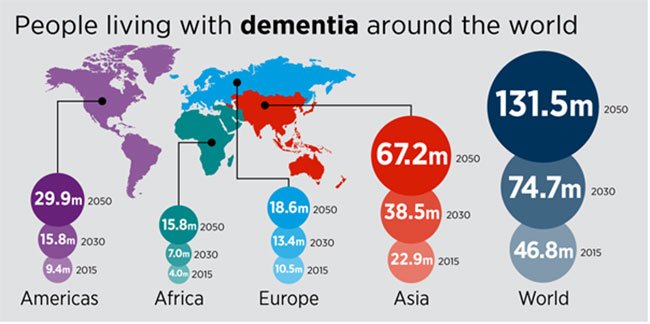
How Many People Have Alzheimers Disease Worldwide
Recent statistics show that about 50 million people around the world have Alzheimers disease or another type of dementia.
Facts from the World Health Organization reveal that about 60 percent of people living with dementia worldwide are from a low- or middle-income country.
The total number of people with dementia is projected to reach 82 million in 2030 and 152 million in 2050, WHO said. To put that in perspective, the current population of the U.S. is 329 million.
In fact, dementia is now the leading cause of death in the United Kingdom, pushing heart disease into second place. This finding comes from the Northern Ireland Statistics and Research Agency and the Office for National Statistics.
Risk Factors For Alzheimer’s Dementia
The vast majority of people who develop Alzheimer’s dementia are age 65 or older. This is called late-onset Alzheimer’s. Experts believe that Alzheimer’s, like other common chronic diseases, develops as a result of multiple factors rather than a single cause. Exceptions are cases of Alzheimer’s related to uncommon genetic changes that increase risk.
2.7.1 Age, genetics and family history
The greatest risk factors for late-onset Alzheimer’s are older age,, genetics, and having a family history of Alzheimer’s.-
Age
Age is the greatest of these three risk factors. As noted in the Prevalence section, the percentage of people with Alzheimer’s dementia increases dramatically with age: 3% of people age 65-74, 17% of people age 75-84 and 32% of people age 85 or older have Alzheimer’s dementia. It is important to note that Alzheimer’s dementia is not a normal part of aging, and older age alone is not sufficient to cause Alzheimer’s dementia.
Genetics
| APOE Pair |
|---|
- One in 10 people age 65 and older has Alzheimer’s dementia.,,
- The percentage of people with Alzheimer’s dementia increases with age: 3% of people age 65-74, 17% of people age 75-84, and 32% of people age 85 and older have Alzheimer’s dementia. People younger than 65 can also develop Alzheimer’s dementia, but it is much less common and prevalence is uncertain.
3.1.1 Underdiagnosis of Alzheimer’s and other dementias in the primary care setting
3.1.2 Prevalence of subjective cognitive decline
Read Also: Diet Soda And Alzheimer’s
Stage : Age Associated Memory Impairment
This stage features occasional lapses of memory most frequently seen in:
- Forgetting where one has placed an object
- Forgetting names that were once very familiar
Oftentimes, this mild decline in memory is merely normal age-related cognitive decline, but it can also be one of the earliest signs of degenerative dementia. At this stage, signs are still virtually undetectable through clinical testing. Concern for early onset of dementia should arise with respect to other symptoms.
Alzheimers Is The Only Top
- 1 in 3 seniors dies with Alzheimers or another dementia, killing more than breast and prostate cancer combined.
- Alzheimers disease is listed as the sixth leading cause of death in the U.S. States, but it may cause more deaths than is recognized by official sources.
- The COVID-19 pandemic caused Alzheimers deaths to increase by approximately 16% more than expected.
- Deaths due to Alzheimers between 2000 and 2019 have more than doubled, increasing 145%. During the same time period, deaths from heart disease increased 7.3%.
Also Check: Does Diet Coke Cause Memory Loss
Public Health Impact Of Deaths From Alzheimer’s Disease
Although deaths from other major causes have significantly or remained approximately the same, official records indicate that deaths from Alzheimer’s disease have increased significantly. Between 2000 and 2019, the number of deaths from Alzheimer’s disease as recorded on death certificates more than doubled, increasing 145.2%, while deaths from the number one cause of death decreased 7.3% ., The increase in the number of death certificates listing Alzheimer’s as the underlying cause of death probably reflects both a real increase in the actual number of deaths from Alzheimer’s due in large part to Alzheimer’s becoming a more common cause of death as the population ages, as well as increased reporting of Alzheimer’s deaths on death certificates over time by physicians, coroners and others who assign causes of death.
FIGURE 7
Deaths From Alzheimer’s Disease
It is difficult to determine how many deaths are caused by Alzheimer’s disease each year because of the way causes of death are recorded. According to data from the CDC, 121,499 people died from Alzheimer’s disease in 2019, the latest year for which data are available. The CDC considers a person to have died from Alzheimer’s if the death certificate lists Alzheimer’s as the underlying cause of death, defined as the disease or injury which initiated the chain of events leading directly to death.
In the United States, Alzheimer’s disease is counted as a cause of death that can be ranked against other leading causes of death such as cancer and heart disease, but deaths due to other types of dementia are not ranked in this manner. The number of deaths from dementia of any type is much higher than the number of reported Alzheimer’s deaths. In 2019, some form of dementia was the officially recorded underlying cause of death for 271,872 individuals ., Therefore, the number of deaths from all causes of dementia, even as listed on death certificates, is more than twice as high as the number of reported Alzheimer’s deaths alone.
Irrespective of the cause of death, among people age 70, 61% of those with Alzheimer’s dementia are expected to die before age 80 compared with 30% of people without Alzheimer’s dementia.
You May Like: What Causes Low Blood Pressure In Dementia Patients
Stage : Mild Dementia
At this stage, individuals may start to become socially withdrawn and show changes in personality and mood. Denial of symptoms as a defense mechanism is commonly seen in stage 4. Behaviors to look for include:
- Difficulty remembering things about one’s personal history
- Disorientation
- Difficulty recognizing faces and people
In stage 4 dementia, individuals have no trouble recognizing familiar faces or traveling to familiar locations. However, patients in this stage will often avoid challenging situations in order to hide symptoms or prevent stress or anxiety.
Disparities Still Impacting Health And Health Care
Reducing or eliminating disparity has been part of the national conversation as a key goal of the U.S. Department of Health and Human Services Healthy People initiative for more than 20 years., Yet disparity is still evident in health and health care.
While health disparities and health care disparities are often used interchangeably, there are important distinctions between the two terms. A health disparity exists when there is a higher burden of illness, injury, disability, or mortality in one group relative to another, whereas a health care disparity is used to describe differences between groups in health insurance coverage, access to and use of health care, and quality of health care. For both these disparities, the differences are not explained by variations in health needs, patient preferences, or treatment recommendations and are closely linked with social, economic, and/or environmental disadvantage.
The existence and adverse effects of health disparities are well documented. For example, Blacks and Native Americans are more likely than Whites to report a range of health conditions, including asthma and diabetes. Native Americans also have higher rates of heart disease compared with Whites.
Health care system factors that contribute to disparity should also be acknowledged. These include implicit bias on the part of health care providers, as well as cultural and language barriers that impede patient-provider relationships.
Also Check: Does Ben Carson Have Dementia
Risk Factors And Prevention
Although age is the strongest known risk factor for dementia, it is not an inevitable consequence of ageing. Further, dementia does not exclusively affect older people young onset dementia accounts for up to 9% of cases. Studies show that people can reduce their risk of dementia by getting regular exercise, not smoking, avoiding harmful use of alcohol, controlling their weight, eating a healthy diet, and maintaining healthy blood pressure, cholesterol and blood sugar levels. Additional risk factors include depression, low educational attainment, social isolation, and cognitive inactivity.
Total Cost Of Health Care And Long
Table reports the average annual per-person payments for health care and long-term care services for Medicare beneficiaries age 65 and older with and without Alzheimers or other dementias. Total per-person health care and long-term care payments in 2019 from all sources for Medicare beneficiaries with Alzheimers or other dementias were over three times as great as payments for other Medicare beneficiaries in the same age group .,
| Payment Source | ||
|---|---|---|
| 2,395 | ||
| TOTAL* Payments from sources do not equal total payments exactly due to the effects of population weighting. Payments for all beneficiaries with Alzheimers or other dementias include payments for community-dwelling and facility-dwelling beneficiaries. | 50,201 | 14,326 |
- * Payments from sources do not equal total payments exactly due to the effects of population weighting. Payments for all beneficiaries with Alzheimers or other dementias include payments for community-dwelling and facility-dwelling beneficiaries.
Recommended Reading: What Color Ribbon For Dementia
How Many Canadians Live With Dementia Including Alzheimer’s Disease And How Many Are Newly Diagnosed Each Year
According to the most recent data available , more than 402,000 seniors are living with dementia in Canada . This represents a prevalence of 7.1%. About two-thirds of Canadian seniors living with dementia are women. Annually, there are approximately 76,000 new cases of dementia diagnosed in Canada. This represents an incidence of 14.3 new cases per 1,000 in the senior population . The incidence is higher among women than men. The prevalence and the incidence increase with age, as does the differential in prevalence and incidence estimates between men and women .
Table 1:
| Age | |
|---|---|
| 15.8 | 14.3 |
Notes: Data do not include Saskatchewan’s data. The 95% confidence interval shows an estimated range of values which is likely to include the true value 19 times out of 20.
Data source: Public Health Agency of Canada, using Canadian Chronic Disease Surveillance System data files contributed by provinces and territories, April 2017.
Over a ten-year period , the age-standardized prevalence of dementia increased by 21.2%. During the same period, fluctuations in incidence have been observed. Drug data, one of the criteria used for case identification , became available in Alberta and Prince Edward Island in 20092010, which contributed to the temporary peak in incidence that year. Since then, incidence data suggest a decline .
| Sex | |
|---|---|
| 6.1 | 14.3 |
What Is The Average Life Expectancy Of Someone Living With Alzheimers Disease
Life expectancy varies depending on the person or when someone developed the disease. The Mayo Clinic reports that in general, most people live for three to 11 years after they are diagnosed, though some people may live for over 20 years after a diagnosis.
Learn about the final stage of Alzheimers and how you die from Alzheimers.
Read Also: Alzheimer’s Disease Neurotransmitters